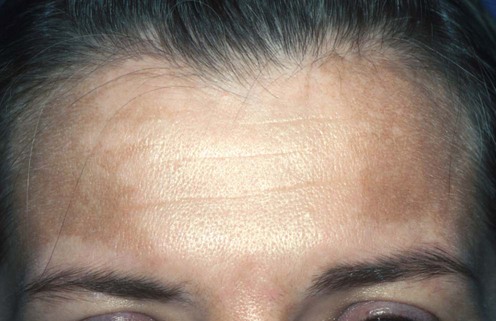
Melasma
First-line therapies
A randomized controlled trial of the efficacy and safety of a triple fixed combination (fluocinolone acetonide 0.01%, hydroquinone 4%, tretinoin 0.05%) compared with hydroquinone 4% cream in Asian patients with moderate to severe melasma.
Chan R, Park KC, Lee MH, Lee ES, Chang SE, Leow YH, et al. Br J Dermatol 2008; 159: 697–703.
Commonly reported adverse effects include mild erythema, burning, and peeling.
Second-line therapies
Third-line therapies
Sequential treatment with triple combination cream and intense pulsed light is more efficacious than sequential treatment with an inactive (control) cream and intense pulsed light in patients with moderate to severe melasma.
Goldman MP, Gold MH, Palm MD, Colon LE, Preston N, Johnson L, et al. Dermatol Surg 2011; 37: 224–33.


 Triple combination cream
Triple combination cream Hydroquinone
Hydroquinone Tretinoin
Tretinoin Adapalene
Adapalene Sunscreen
Sunscreen Azelaic acid
Azelaic acid Glycolic acid peel
Glycolic acid peel Rucinol
Rucinol Jessner’s solution
Jessner’s solution Salicylic acid peel
Salicylic acid peel Niacinamide
Niacinamide Kojic acid
Kojic acid Laser and intense pulsed light
Laser and intense pulsed light Liquiritin
Liquiritin Tranexamic acid
Tranexamic acid