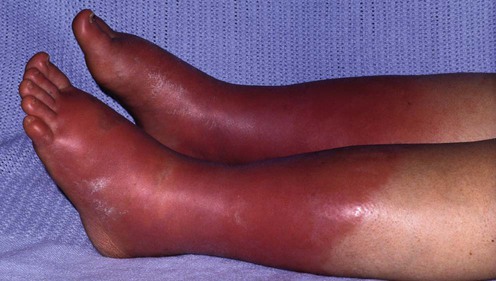
Erythromelalgia
Management strategy
Numerous treatment alternatives based on case reports have been presented in the literature. Anecdotally, nitroglycerin ointment, capsaicin cream, ketanserin, methysergide, pizotifen, β-blockers, cyproheptadine or other antihistamines, carbamazepine, clonazepam, corticosteroids or other immunosuppressants, pentoxifylline, phenoxybenzamine, opiates, prazosin have been presented as effective. Hyperbaric oxygen treatment, spinal cord stimulation, thalamic stimulation, epidural blocks have also been proposed. Sympathectomy has been beneficial in some patients and in other patients caused worsening of symptoms. Treatment modalities such as hypnosis, biofeedback and learning to avoid triggers can be beneficial for coping with pain. A survey of members of The Erythromelalgia Association (TEA, www.erythromelalgia.org) shows that more than 50 therapeutic regimes have been tried out. TEA is a non-profit organization that may be helpful in providing information, awareness and support.
Specific investigations
First-line therapies
Second-line therapies





 Treatment of underlying disease
Treatment of underlying disease Cooling
Cooling Aspirin
Aspirin Prostaglandins/prostacyclin or oral analogs
Prostaglandins/prostacyclin or oral analogs Sodium channel blockers (lidocaine, mexiletine, bupivacaine, XEN402)
Sodium channel blockers (lidocaine, mexiletine, bupivacaine, XEN402) Gabapentin
Gabapentin Antidepressants (venlafaxine, sertraline)
Antidepressants (venlafaxine, sertraline) Sodium nitroprusside
Sodium nitroprusside Vasodilators (calcium antagonists, magnesium)
Vasodilators (calcium antagonists, magnesium)