44 Thermal Applications
Physiologic Effects of Local Application of Heat
Heat energy applied to a localized area of the body produces changes not only at the site of application, but also in surrounding tissues and in distant regions. The resultant changes counter the threat to thermal equilibrium and assist the local structures to avoid tissue damage. The local effects are caused by the elevated temperature response of cellular function by direct and reflex action. The rise in temperature is accompanied by an increase in blood flow. Dilatation of the capillaries on exposure to local heat leads to an elevation of hydrostatic pressure and an increase in capillary permeability. The increase in permeability leads to an increase in leukocytic and antibody infiltration in the area, which is an important factor in controlling inflammation and promoting early healing. However, an increase in hydrostatic pressure may cause edema of the desired region. This effect would contraindicate the use of heat in conditions where swelling or edema is to be avoided.1
Superficial heat remodels connective tissue by three mechanisms. First, heat creates several physiologic changes through subsequent vascular changes, causing vasodilation. This dilation gives an analgesic effect, which increases the patient’s pain threshold and results in greater tolerance of connective tissue stretching. Second, physiologic effect of heat is an alteration of the viscous flow properties of collagen, which results in the relief of joint stiffness. Third, there is an increase in the extensibility of collagen tissue, a major component of connective tissue, through changes in its viscoelastic properties following the application of heat.2
In general, the transfer of heat (whether the purpose is heating or cooling) often is classified into four general types of heat transfer: conduction (hot pack, paraffin bath), convection (fluidotherapy, hydrotherapy), conversion (radiant heat), and radiation. The most commonly used in clinical application is conduction, through the agency of water.1 The level of the tissue temperature (usually 40 to 45° C), duration of the tissue temperature increase, rate of increase in the tissue temperature, and the size of the area being treated determine the extent of the physiologic response to heat.
Commonly Used Heat Modalities in Present Clinical Setting
Hot Packs or Hydrocollator Packs
To prevent burning, adequate layer(s) of towel should be added during the duration of treatment and the patient should never lie on the packs because the patient’s body weight could squeeze hot water out of the pack into the towel and potentially cause a burn. It is highly recommended to check the patient every 5 minutes. Indications for the application of hot packs may include painful muscle spasms, abdominal muscle cramping, menstrual cramps, and superficial thrombophlebitis.3
Contraindications may include peripheral vascular diseases, skin eruptions at the site of application, desensitized skin, new skin, and obtunded sensorium of the patient.4
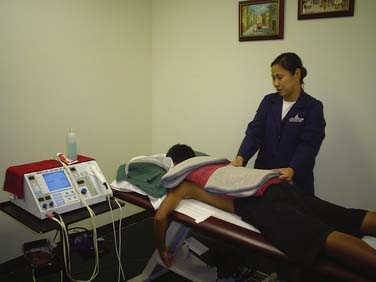
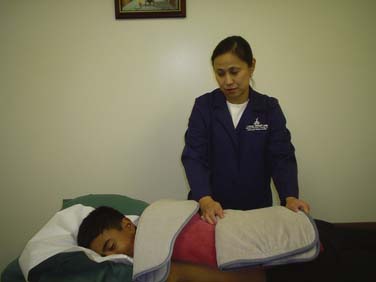
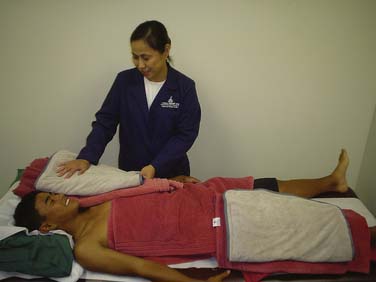
Determine the wrapping procedure to be used. Apply the hot pack to the area to be treated. Cover it with a dry towel. Check the patient every 5 minutes (Figs. 44-1 to 44-3).
Ultrasound/Ultrasonic Therapy
Ultrasonographic energy is generated by the piezo-electric effect. Electrical energy is applied to a crystal causing the crystal to vibrate at a high frequency and thereby to produce ultrasound waves. Ultrasound is delivered by continuous or pulsed high-frequency sound waves and provides a high heating intensity.3 The sound waves vibrate tissues deep inside the injured area. This creates heat that draws more blood into the tissues, which institutes the reparative process.
Ultrasound is the optimal form of heat treatment for soft tissue injuries. It is used to treat joint and muscle sprains, bursitis, and tendonitis. Ultrasound can produce many effects other than just the potential heating effect. It has been shown to cause increases in tissue relaxation, local blood flow, and scar tissue breakdown. The effect of the increase in local blood flow can be used to help reduce local swelling and chronic inflammation, and, according to some studies, promote bone fracture healing. The intensity or power density of the ultrasound can be adjusted depending on the desired effect.5 Knight and associates6 studied the effects of superficial heat and deep heat including ultrasound on the extensibility of plantar flexors. The results indicated that among the modalities tested, the use of ultrasound for 7 minutes prior to stretching may be the most effective for increasing ankle dorsiflexion range of motion (ROM).
A typical ultrasound treatment will take from 3 to 5 minutes depending on the size of the area being treated. For underwater treatment, time is progressive, beginning at 5 minutes and increasing to a maximum of 8 to 10 minutes per treatment. The dosage depends on the intensity and time, and the product of these factors is usually expressed in watt-minutes. The intensity of sound energy available from the ultrasound head is usually expressed as watts per square centimeter. Therapeutic intensities of 0.5 to 2.0 watts per square centimeter have been determined to be useful.7
Ultrasound treatment series is considered to be 6 to 12 applications, applied daily according to some authorities. Others say, every other day. It is also important to remember that when using this modality in acute conditions, low intensity treatment is required. Chronic conditions will require a higher intensity. Ultrasound treatment, just like any other deep heating modality is used to (1) relieve pain and inflammation, (2) speed healing, (3) reduce muscle spasms, and (4) increase ROM. This treatment modality is commonly used for joint contractures, joint adhesions, calcific bursitis, hematoma resolution, and neuromas. Other conditions that may benefit from ultrasound treatment include fibrosis, phantom limb pain, myofascial pain, reflex vasodilatation, and ulcer débridement. However, the therapeutic benefit maybe limited in these later conditions. Warden and associates8 have shown that conventional therapeutic ultrasound as traditionally used by physical therapists may be used to accelerate fracture healing.
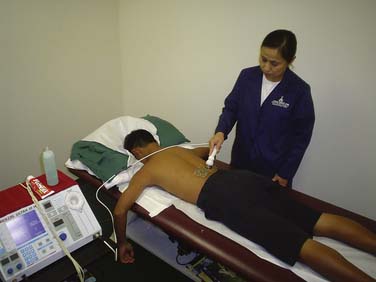
Ultrasound treatment is contraindicated in the pregnant uterus, laminectomy sites, and ischemic areas. Application of ultrasound over surgically implanted hardware remains controversial and when performed in these areas it should be done with caution (Figs. 44-4 and 44-5).3
Paraffin Bath
A paraffin bath is another form of conductive heating. Paraffin baths are particularly useful for contractures due to rheumatoid arthritis, burns, and progressive systemic sclerosis (scleroderma).3 Paraffin is usually applied to the hands, arms, and feet. Higher temperature (55° C) is tolerable without danger of burning the tissue when using paraffin as compared to water, (42° C to 45° C) because the specific heat is one-half that of water and solid paraffin forms a protective and insulating coat over the skin. For therapeutic purposes, the paraffin bath is maintained at the melting point of 51.7° C to 54.4° C in an insulated, thermostatically controlled container.
Ayling and associates9 studied the efficacy of paraffin baths for rheumatoid arthritic hands. The results indicated that of the four randomized trials identified concerning the outcome of paraffin wax applications to rheumatoid arthritic hands, one yielded equivocal results, whereas three reported that after 3 to 4 weeks, paraffin wax applications were accompanied by significant improvements in rheumatoid arthritic hand function when followed by exercise. This modality also relieves pain and stiffness immediately after its application with no documented detrimental effects on the disease process, even though paraffin wax temporarily raises joint temperature.
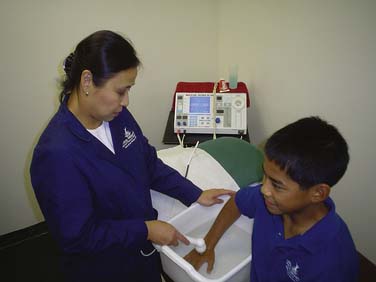
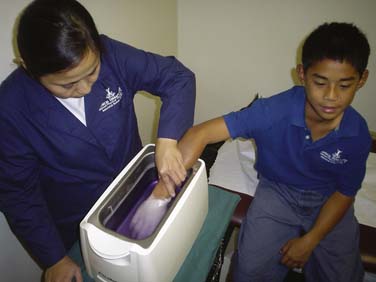
When performing the dipping method, the hand or foot is placed in the liquid paraffin bath and is withdrawn when a thin layer of warm, solid paraffin forms, becomes adherent, and covers the skin. This procedure is repeated 8 to 10 times until a thick paraffin glove is formed. By wrapping the body part with plastic wrap and towels for 20 to 30 minutes, the heat can be retained. A masking tape can be used to hold the towel in place. To remove the paraffin, slip finger under the upper edge and peel it off. Return the paraffin to the bath. The paraffin can be re-used. When performing the immersion method, initially perform the dipping method to form a protective covering of paraffin. Then immerse extremity for the prescribed time or until the paraffin is melted. Make sure the patient is rested in a relaxed position. Putting a padding on the edge of the tank will make the patient more comfortable during the treatment process (Figs. 44-6 to 44-9).
Heat Treatment for Home Use
Warm compresses or moist warm towels can be used at home. Preparation includes the following: (1) fold the hand towel lengthwise and then crosswise; (2) wet the towel and place it in a plastic bag; (3) put the bag in the microwave oven for 4 minutes; (4) wrap the bag in a dry towel and apply to affected area; (5) apply the warm compress for 10 minutes and repeat the same process twice to complete the 20-minute treatment (Fig. 44-10).
1. Reyes T. Introduction to Physical Therapy and Patient Care, Hydrotherapy, Traction, and Massage, 2nd ed. Manila, Philippines: UST Press; 1985. 121
2. DiFrancesco B: Heat application in physiotherapy. Website. http://www.activebodyclinic.com/core_Physio_heat.html. Accessed August 23, 2009.
3. Klein M: Superficial heat and cold. Website: http://emedicine.medscape.com/article/324974-overview. Accessed August 23, 2009.
4. Reyes T. Introduction to Physical Therapy and Patient Care, Hyrotherapy, Traction, and Massage, 2nd ed. Manila, Philippines: UST Press; 1985. 143
5. Ultrasound in physical therapy. Website: http://www.automailer.com/tws/ultrasound.html#ixzz0QeK81VD9. Accessed August 28, 2009.
6. Knight C., Rutledge C., Cox M., et al. Effect of superficial heat, deep heat, and active exercise warm-up on the extensibility of the plantar flexors. Phys Ther. 2001;81:1206-1214.
7. Shestack R. Handbook of Physical Therapy, 3rd ed. New York: Springer Publishing; 1977. 47
8. Warden S.J., Fuchs R.K., Kessler C.K., et al. Ultrasound produced by a conventional therapeutic ultrasound unit accelerates fracture repair. Phys Ther. 2006;86:1118-1127.
9. Ayling J., Marks R. Efficacy of paraffin wax baths for rheumatoid arthritic hands. Physiotherapy. 2000;86:190-201.