Everyone knows that heavy drinking and drug use are bad for you.
That part is not new information.
What gets talked about far less is the specific, often permanent, physical damage that builds up quietly over time. The liver gets mentioned. The heart sometimes. But there is a whole list of consequences most people are completely unaware of until they are already dealing with them.
This article covers what long-term substance use actually does to the body, what proper withdrawal and detox involve, and some of the physical conditions that can develop as a direct result of prolonged use, including ones that require medical or surgical intervention to address.
More Than Just Addiction: What Chronic Use Does to the Body
Addiction gets framed as a mental health issue, which it is.
But the physical dimension is just as significant, and often harder to reverse.
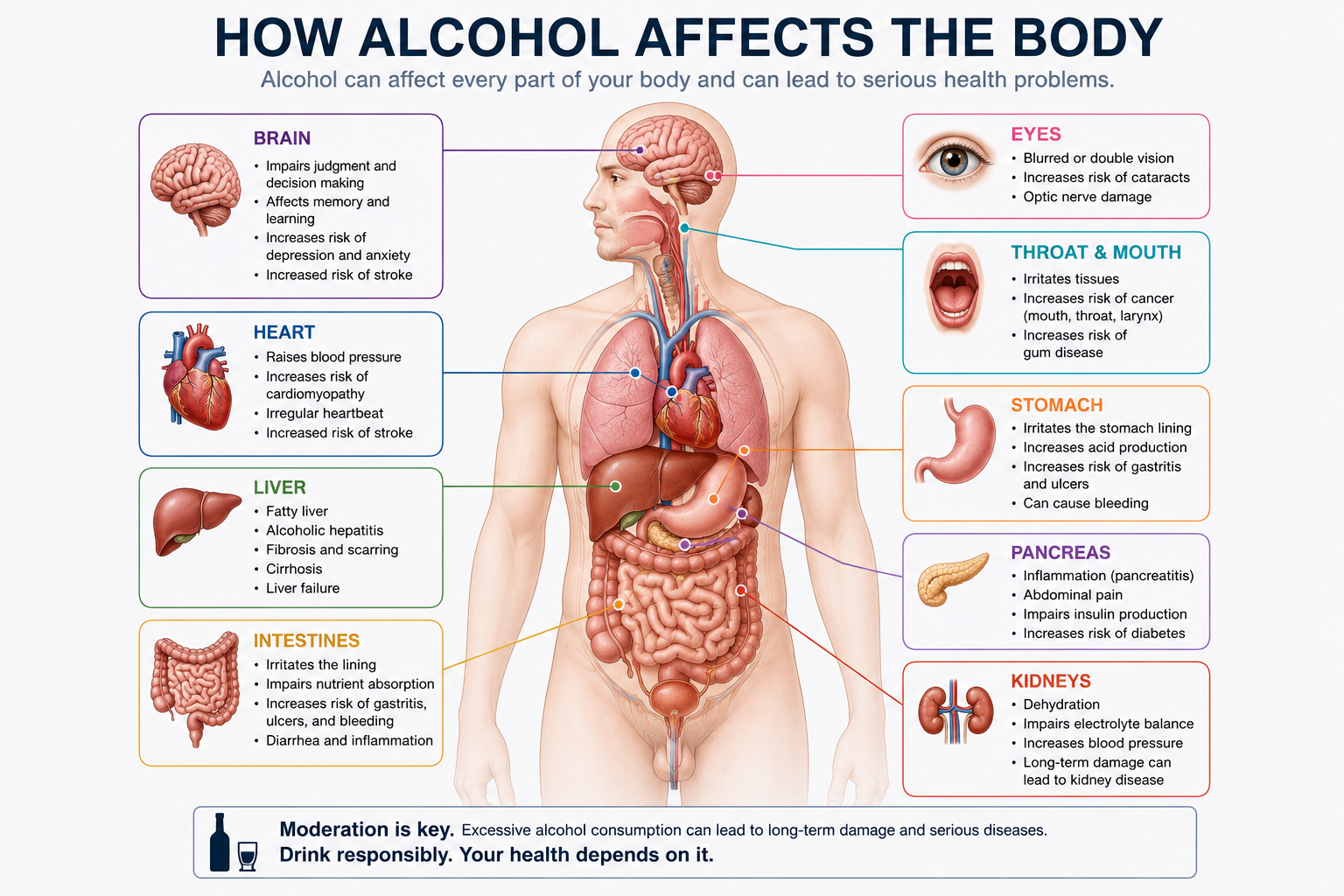
Long-term alcohol use affects almost every major organ system. The liver is the obvious one. But chronic drinking also damages the pancreas, disrupts cardiovascular function, weakens the immune system, and interferes with the body’s ability to absorb essential nutrients.
Drug use, depending on the substance, carries its own specific physical consequences.
Stimulants put sustained stress on the heart. Opioids suppress respiratory function and dysregulate the digestive system. Heavy, long-term cannabis use has been linked to lung issues and structural changes in the brain.
The common thread across all of them is inflammation.
Chronic substance use creates a state of ongoing physiological stress that the body was simply not designed to sustain.
What makes this particularly difficult is that many of these changes are subtle at first. They accumulate quietly. By the time someone notices something is genuinely wrong, the damage is often well established.
Why Stopping Is Not as Simple as Just Stopping
There is a widespread belief that choosing to stop using a substance is primarily a matter of willpower.
That belief causes enormous harm.
For many substances, particularly alcohol, benzodiazepines, and opioids, abrupt cessation triggers a withdrawal process that is not just uncomfortable. It can be medically dangerous.
Alcohol withdrawal is one of the few withdrawal syndromes that can be fatal without proper medical management.
Symptoms can include severe anxiety, tremors, elevated blood pressure, hallucinations, and in serious cases, seizures. The risk is highest in people who have been drinking heavily over an extended period.
This is why simply going cold turkey at home, without clinical oversight, is something healthcare professionals consistently advise against.
Proper detoxification involves medical monitoring, medication to manage withdrawal symptoms safely, nutritional support, and a structured plan for what comes after the physical process.
It is the foundation of recovery, not the whole building.
For anyone supporting someone through this process, or going through it themselves, connecting with professional detox services that are specifically equipped to manage medically complex withdrawal is often the safest and most effective starting point.
Getting the detox phase right matters.
A poorly managed withdrawal can not only be dangerous in the short term. It can also make sustained recovery significantly harder.

The Hormonal Consequences People Rarely Expect
Here is something that genuinely surprises a lot of people.
Long-term alcohol use significantly disrupts hormone production.
Chronic alcohol consumption suppresses testosterone levels in men while simultaneously increasing the conversion of androgens to oestrogen. Over time, this hormonal imbalance can produce physical changes that go well beyond fatigue and reduced libido.
One of the most visible of these changes is the development of gynaecomastia.
This is the enlargement of glandular breast tissue in men, caused by that shift in the oestrogen to testosterone ratio. It is not the same as excess chest fat. It is the actual growth of breast tissue, driven by hormonal disruption.
It is more common than most people realise.
Alcohol is one of several contributing factors. Anabolic steroid use is another well-documented cause. So is the use of certain medications, including some prescribed for heart conditions and psychiatric disorders.
For men who develop gynaecomastia, the experience often carries a significant psychological weight alongside the physical one.
Many feel self-conscious about their appearance, avoid situations that involve removing their shirt, and find the condition affects their confidence in ways that are hard to articulate.
The important thing to understand is that gynaecomastia caused by hormonal disruption does not simply reverse itself once the underlying cause is addressed.
Once glandular tissue has developed, it often does not regress on its own. That is where medical intervention becomes relevant.
When Lifestyle Changes Are Not Enough
Addressing the root cause of gynaecomastia always matters and should be the first step.
For alcohol-related cases, this means achieving sobriety and giving the body time to stabilise hormonally.
But for men who have had the condition for an extended period, lifestyle changes alone often do not produce the physical result they are looking for.
Surgical correction is a well-established option in these situations.
Gynaecomastia surgery involves the removal of excess glandular tissue, and in some cases excess skin, to restore a flatter chest contour. It is not a cosmetic shortcut. For many men, it is the resolution of a condition that has affected their quality of life for years.
If you are weighing up whether surgery is the right path, understanding the full range of gyno surgery options available is a sensible place to start.
A qualified surgeon can assess the composition and extent of the tissue, explain what the procedure involves, and set realistic expectations for recovery and results.
The decision is a personal one. But having accurate information takes the uncertainty out of it.
Recovery as a Physical Process, Not Just a Mental One
There is a tendency to frame recovery almost entirely in psychological terms.
The mental work is real and it matters. But the physical recovery process deserves equal attention.
The body takes time to recalibrate after sustained substance use.
Hormonal levels gradually normalise. The liver begins to repair itself, within limits depending on the extent of the damage. Sleep architecture, which chronic alcohol use severely disrupts, starts to restabilise. Nutritional deficiencies that have built up over months or years begin to be corrected.
This process is not quick. And it is not linear.
Many people in early recovery are surprised by how physically rough the first weeks and months can feel, even after the acute withdrawal phase has passed.
This is the body working hard to find its new normal. Understanding that this is expected, and temporary, makes a significant difference to how people experience it.
Recovery support needs to address the physical dimension properly.
Nutritional guidance, regular medical check-ins, and appropriate treatment for conditions that developed during the period of use are all part of genuine, comprehensive care.
The Bigger Picture
Long-term substance use leaves marks.
Some are invisible, showing up in blood work or in the way organs function. Others are physical and visible, in ways that affect how a person sees themselves and moves through the world.
None of these consequences are a reason to feel shame.
They are clinical realities that can be understood, addressed, and in many cases resolved with the right professional support.
What matters most is getting the right help at the right stage.
That means medically supervised detox when the withdrawal risk is significant. It means proper recovery support in the months that follow. And it means accessing specialist medical care for any physical conditions that have developed along the way.
The body has a remarkable capacity to recover. But it needs the right conditions to do so.

