Integrating ultrasound in emergency prehospital settings
A prospective evaluation in a hospital environment, determined that handheld focused assessment sonography in trauma (HHFAST) examination was equivalent to the FAST examination, using more conventional equipment. HHFAST had a sensitivity of 78%, specificity of 100%, positive predictive value (PPV) of 100%, and negative predictive value (NPV) of 97%.1,2 HHFAST can detect intraperitoneal fluid with high degrees of accuracy. It will miss some injuries, but the majority of injuries missed do not require therapy.3 In addition, field US, using the HHFAST, can also be performed by nonphysician providers. With close supervision, paramedics can adequately obtain and interpret FAST and abdominal aortic US images under protocol.4
Remote location imaging
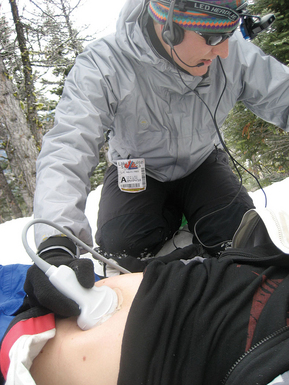
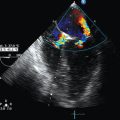
Popov et al5 set out to demonstrate both the simplicity and robustness of existing US technologies in a remote location. They evaluated telementored resuscitative extended FAST (e-FAST) US examination. An expert interpreter guided a first responder located midmountain at a commercial ski resort. The test subject was a healthy volunteer. US images were obtained on a first-generation SonoSite 180 machine and were converted to digital video using a readily available video converter. A head-mounted camera provided a macroscopic view of the examination, allowing the remote examiner to view both the patient and examiner’s hands, while simultaneously viewing the US results (Figures 48-1 and 48-2).6–8
Remote US has also been evaluated and tested aboard Aquarius, an underwater habitat off the Florida Keys, as part of the NASA Extreme Environment Mission Operations (NEEMO). The life sciences mission NEEMO 7 investigated the role of US examination of the abdominal organs and structures. US-trained and untrained aquanaut crew members conducted a series of diagnostic and interventional procedures with remote guidance from experts more than 3000 km away. Researchers demonstrated that mean efficiencies were slightly higher with telementoring than with the use of a procedure manual.9
Disaster and prehospital medicine
The role of US in disaster medicine has not been well established and is generally limited to case reports and case series. A report by the Disaster Medical Assistance Team (DMAT), responding to the aftermath of a cyclone in Western Australia, demonstrated that US-competent physicians were able to use portable US on casualties to exclude intraabdominal hemorrhage, pericardial fluid, pneumothoraces, and hemothoraces. The US machine had a weight of 3.7 kg (MicroMaxx, SonoSite, Bothell, WA). It was powered by using a self-contained, rechargeable battery. A 60-mm, 5-2-MHz curvilinear probe and a 38-mm, 10-5-MHz linear probe were selected as most appropriate for the likely requirements. Information obtained using US made initial patient management and subsequent decisions regarding triage for transport safer and based on more detailed clinical information.10,11
Sarkisian et al12 reported from the Armenian earthquake of 1988, in which US was performed as a primary screening procedure in 400 of 750 mass casualty patients with trauma who were admitted to a large hospital within the first 72 hours after the earthquake. Two real-time sector scanners were used in the reception area of the hospital, and the average time spent on one patient was 4 minutes. More than 130 follow-up ultrasonographic examinations were required. Impressively, trauma-associated pathology of the abdomen and retroperitoneal space was detected in 12.8% of the patients, with 1% false negatives and no false positives.
In the Marmara earthquake, which occurred on August 17, 1999, 639 people had renal complications and 477 needed hemodialysis treatment because of acute renal failure caused by crush injury. This led Keven et al13 to undertake a study using renal US, in which resistive indexes were measured, and it was demonstrated that in crush injury, measurement of renal resistive indexes can be useful for the prognosis of recovery from acute renal failure.
Thoracic imaging
In addition to the potential role as FAST, field medics are using US to detect abnormalities in other anatomic regions. Studies have demonstrated that US scanning, in the right hands, is extremely accurate in determining the presence of pneumothoraces.14,15 In a normal individual, there is visible sliding of the pleura on ultrasonography16 and comet tails.17 However, the presence of a pneumothorax will eliminate the presence of both. Use of M-mode ultrasonography also allows the detection of pneumothoraces. This can be of great advantage in the field environment or disaster relief situations because chest radiographs are not readily available.
US has also shown promise in detecting medical problems in austere settings. It has been successfully used in demonstrating adequate endotracheal tube positioning (which is especially useful if there is suspicion that the tube is malpositioned and radiography is not available),18 diagnosis of cerebrovascular accidents,19 differentiating between pulmonary edema and chronic obstructive pulmonary disease,20 and the diagnosis and treatment of myocardial infarction with wall hypokinesis.21
Airway imaging
Currently, the role of US in anesthesia-related airway assessment and procedural interventions is encouraging, although it is still ill defined. US can visualize anatomic structures in the supraglottic, glottic, and subglottic regions. The floor of the mouth can be visualized by both transcutaneous views of the neck and also by transoral or sublingual views. However, imaging the epiglottis can be challenging because it is suspended in air. US may detect signs suggestive of difficult intubation, but the data are limited. Other possible applications in airway management include confirmation of correct endotracheal tube placement, prediction of postextubation stridor, assessment of subglottic diameter for determination of pediatric endotracheal tube size, and percutaneous dilational tracheostomy.22,23
Transtracheal or transcricothyroid placement of a cannula is a practice used in a number of aspects of airway management in anesthesia and intensive care. If a difficult intubation scenario occurs in a patient with unidentifiable anterior neck airway anatomy, at a location where an US machine is immediately available, it is recommended that consideration be given to the use of US-guided cannula tracheotomy as the first-line rescue technique.24
Cardiovascular imaging
Experimental studies have shown that some US contrast agents actually enhance the effectiveness of thrombolytic agents in the presence of US in vitro and in vivo. Recent “sonolysis” studies have been undertaken to study this effect in patients with ST-elevation myocardial infarction, based on proximal lesions of the infarct-related artery,25–27 which theoretically could be initiated in the field.
There are case series that suggest that abdominal aortic aneurysm and e-FAST emergency US examinations can be performed in the stationary or moving land/air ambulance environment to a standard consistent with those performed in the hospital emergency department.28, 29
Other regions
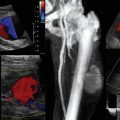
A recent study30 demonstrated that US-trained personnel can correctly detect, with a high degree of sensitivity and specificity, the presence or absence of simulated long bone fractures.
Pearls and highlights
• There are several extremely portable US scanners that afford imaging in remote locations. Imaging can be performed by nonphysicians, with images downloaded to more experienced providers. This has been successfully accomplished in space and at high altitude. The absence of gravity in space makes traditional FAST imaging challenging.
• Portable US has been used successfully in disaster mass casualty situations to prioritize care of the injured patients. In addition to trauma applications, portable US can be used to image the airway and to assess cardiac and pulmonary function in the face of hypotension and hypoxia.
References
1. Kirkpatrick, AW, Simons, RK, Brown, R, et al, The hand-held FAST: experience with hand-held trauma sonography in a level-I urban trauma center. Injury. 2002;33(4):303–308.
2. Khan, M, Lovegrove, RE, Diagnostic peritoneal lavage versus hand-held FAST: the future for diagnosis of injury in the military environment. J R Nav Med Ser. 2008; 94:19–21.
3. Kirkpatrick, AW, Sirois, M, Laupland, KB, et al. Prospective evaluation of hand-held focused abdominal sonography for trauma (FAST) in blunt abdominal trauma. Can J Surg. 2005; 48(6):453–460.
4. Heegaard, W, Hildebrandt, D, Spear, D, et al, Prehospital ultrasound by paramedics: results of field trial. Acad Emerg Med. 2010;17(6):624–630.
5. Popov, V, Popov, D, Kacar, I, Harris, RD, The feasibility of real-time transmission of sonographic images from a remote location over low-bandwidth Internet links: a pilot study. AJR Am J Roentgenol. 2007;188(3):W219–W222.
6. McBeth, PB, Hamilton, T, Kirkpatrick, AW. Cost-effective remote iPhone-teathered telementored trauma telesonography. J Trauma. 2010; 69(6):1597–1599.
7. Crawford, I, Tiruta, C, Kirkpatrick, AW, et al, Big brother could actually help quite easily: telementored “just-in-time” telesonography of the FAST over a smartphone. Ann Emerg Med. 2011;58(3):312–314.
8. Dyer, D, Cusden, J, Turner, C, et al. The clinical and technical evaluation of a remote telementored telesonography system during the acute resuscitation and transfer of the injured patient. J Trauma. 2008; 65(6):1209–1216.
9. Doarn, CR, Anvari, M, Low, T, Broderick, TJ. Evaluation of teleoperated surgical robots in an enclosed undersea environment. Telemed J E Health. 2009; 15(4):325–335.
10. Mazur, SM, Rippey, J, Transport and use of point-of-care ultrasound by a disaster medical assistance team. Prehosp Disaster Med. 2009;24(2):140–144.
11. Walcher, F, Weinlich, M, Conrad, G, et al. Prehospital ultrasound imaging improves management of abdominal trauma. Br J Surg. 2006; 93(2):238–242.
12. Sarkisian, AE, Khondkarian, RA, Amirbekian, NM, et al. Sonographic screening of mass casualties for abdominal and renal injuries following the 1988. Armenian earthquake. J Trauma. 1991; 31(2):247–250.
13. Keven, K, Ates, K, Yagmurlu, B, et al. Renal Doppler ultrasonographic findings in earthquake victims with crush injury. J Ultrasound Med. 2001; 20(6):675–679.
14. Kirkpatrick, AW, Brown, DR, Crickmer, S, et al. Hand-held portable sonography for the on-mountain exclusion of a pneumothorax. Wilderness Environ Med. 2001; 12(4):270–272.
15. Lyon, M, Walton, P, Bhalla, V, Shiver, SA. Ultrasound detection of the sliding lung sign by prehospital critical care providers. Am J Emerg Med. 2012; 30(3):485–488.
16. Blaivas, M, Inadequate needle thoracostomy rate in the prehospital setting for presumed pneumothorax: an ultrasound study. J Ultrasound Med. 2010;29(9):1285–1289.
17. Noble, VE, Lamhaut, L, Capp, R, et al. Evaluation of a thoracic ultrasound training module for the detection of pneumothorax and pulmonary edema by prehospital physician care providers. BMC Med Educ. 2009; 9:3.
18. Brun, PM, Bessereau, J, Cazes, N, et al. Lung ultrasound associated to capnography to verify correct endotracheal tube positioning in prehospital. Am J Emerg Med. 2012; 30(9):e5–e6. [2080].
19. Holscher, T, Schlachetzki, F, Zimmermann, M, et al. Transcranial ultrasound from diagnosis to early stroke treatment. 1. Feasibility of prehospital cerebrovascular assessment. Cerebrovasc Dis. 2008; 26(6):659–663.
20. Zechner, PM, Aichinger, G, Rigaud, M, et al. Prehospital lung ultrasound in the distinction between pulmonary edema and exacerbation of chronic obstructive pulmonary disease. Am J Emerg Med. 2010; 28(3):e1–e2. [389].
21. Slikkerveer, J, Dijkmans, PA, Sieswerda, GT, et al, Ultrasound enhanced prehospital thrombolysis using microbubbles infusion in patients with acute ST elevation myocardial infarction: rationale and design of the Sonolysis study. Trial. 2008; 9:72.
22. Kundra, P, Mishra, SK, Ramesh, A. Ultrasound of the airway. Indian J Anaesth. 2011; 55(5):456–462.
23. Prasad, A, Singh, M, Chan, VW. Ultrasound imaging of the airway. Can J Anaesth 2009. 2009; 56(11):868–869. [author reply 869-780].
24. Dinsmore, J, Heard, AM, Green, RJ. The use of ultrasound to guide time-critical cannula tracheotomy when anterior neck airway anatomy is unidentifiable. Eur J Anaesthesiol. 2011; 28(7):506–510.
25. Slikkerveer, J, Veen, G, Appelman, Y, et al, Therapeutic application of ultrasound: contrast-enhanced thrombolysis in acute ST-elevation myocardial infarction; the Sonolysis study. Neth Heart J. 2011;19(4):200–205.
26. Xie, F, Slikkerveer, J, Gao, S, et al. Coronary and microvascular thrombolysis with guided diagnostic ultrasound and microbubbles in acute ST segment elevation myocardial infarction. J Am Soc Echocardiogr. 2011; 24(12):1400–1408.
27. Slikkerveer, J, Kleijn, SA, Appelman, Y, et al, Ultrasound enhanced prehospital thrombolysis using microbubbles infusion in patients with acute ST elevation myocardial infarction: pilot of the Sonolysis study. Ultrasound Med Biol. 2012;38(2):247–252.
28. Snaith, B, Hardy, M, Walker, A, Emergency ultrasound in the prehospital setting: the impact of environment on examination outcomes. Emerg Med J. 2011;28(12):1063–1065.
29. Walcher, F, Kortüm, S, Kirschning, T, et al. [Optimized management of polytraumatized patients by prehospital ultrasound]. Der Unfallchirurg. 2002; 105(11):986–994.
30. Heiner, JD, McArthur, TJ. The ultrasound identification of simulated long bone fractures by prehospital providers. Wilderness Environ Med. 2010; 21(2):137–140.
31. Gerson, J, Perera, P, Ultrasound in austere settings: a case report from a field hospital in Haiti. Crit Ultrasound . 2011; 3:97–99.
32. Shah, P, Price, DD, Manual of ultrasound for resource-limited settings. Partners in Health, Boston, 2011.