Exercise Testing and Training
Secondary Cardiovascular and Pulmonary Dysfunction
This chapter extends the general principles of exercise testing and training presented in Chapter 19 and describes special considerations concerning exercise testing and training for individuals with secondary cardiovascular and pulmonary dysfunction. These special considerations are also important when managing an individual with primary cardiovascular and pulmonary dysfunction who, in addition, has cardiovascular and pulmonary dysfunction secondary to other conditions. In that case, management is modified based on the combination of comorbidities. Individuals with progressive degenerative conditions are often older and debilitated; thus the combination of problems is common. Exercise testing and training is one component of the comprehensive physical therapy management of individuals with chronic, secondary cardiovascular and pulmonary dysfunction, which is described in Chapter 32.
Secondary cardiovascular and pulmonary dysfunction refers to dysfunction of the cardiovascular and pulmonary system that is a consequence of pathology other than primary chronic heart and lung disease. Examples of such secondary conditions are described in Chapter 6. These conditions include dysfunction of the musculoskeletal, connective tissue, neurological, gastrointestinal, hepatic, renal, hematological, endocrine, and immunological systems, or some combination thereof. Nutritional disorders, specifically obesity and starvation (anorexia nervosa), also have cardiovascular and pulmonary manifestations. Conditions leading to secondary cardiovascular and pulmonary dysfunction affect one or more steps in the oxygen transport pathway in such a way that the capacity for oxygen delivery is reduced, oxygen consumption is increased, or both.1 Often oxygen delivery is further compromised by restricted mobility. Oxygen transport limitations resulting from secondary cardiovascular and pulmonary dysfunction can present subtly, yet have significant clinical implications. Exercise has a primary role in the management of these conditions, along with the elements of comprehensive multidisciplinary prevention and long-term rehabilitation programs.
Contemporary approaches to the rehabilitation of individuals with stroke serve as a prime example of conventional practice aligning with contemporary exercise physiology principles. Over the past 20 years, stroke rehabilitation has shifted from a focus on Bobath and Brunnstrom interventions to structured exercise training. Exercise training in the management of stroke has the potential for driving brain reorganization and exploiting the property of neuroplasticity to maximize functional capacity.2 Exercise can take advantage of the potential for neural reorganization, optimize functional capacity, and address deconditioning. A focus on endurance and strengthening exercise, task-specific training, and treadmill walking in the rehabilitation of individuals with stroke, in addition to the conventional focus on cognitive engagement, sensorimotor integration, skill acquisition, and social readjustment has been an exciting advance in the rehabilitation of people with strokes.
Another prime example of exercise testing and training being prescribed for noncardiovascular and pulmonary conditions is their inclusion as a component of prehabilitation in preparation for surgery for a range of conditions. Before orthopedic surgical procedures, for example, improvements in functional capacity have been advocated to reduce perioperative complications and speed recovery.3 Such programs include warm-up, aerobic training, resistance training, flexibility, and daily functional activities.
Assessment and Goals
Assessment
Goals: Prevention
Many individuals with systemic conditions (see Chapter 6), the focus of this chapter, have manifestations of oxygen transport limitations or one or more risk factors. The risk factors must be identified and considered in a preventive management plan that includes exercise prescription to exploit the preventive effects of activity described in Chapters 18 and 19. Preventive goals for individuals with chronic, secondary cardiovascular and pulmonary conditions include optimizing central and peripheral adaptations to exercise, reducing biomechanical stress and strain (hence minimizing oxygen cost of exercise at submaximal work rates), optimizing fluid dynamics and hemodynamics, and optimizing lung health (e.g., alveolar ventilation, flow rates, mucociliary transport, and lymphatic drainage).
Goals: Short Term
When oxygen transport limitations occur, a regimen of physical activity and exercise can be prescribed to elicit the acute effects of exercise (see Chapter 18). Prescription of exercise to elicit its acute effects has a primary role in the management of individuals during acute episodes of illness and setbacks.
Goals: Long Term
When an individual has recovered from an acute episode, or an individual requires subacute and long-term management, a regimen of physical activity and exercise can be prescribed to elicit the long-term effects of exercise described in Chapter 18. The capacity of each individual to respond to an exercise stimulus and the individual’s oxygen transport reserve capacity are both assessed in detail. Knowledge of the reserve capacity is essential for optimal exercise prescription.
Individuals with Musculoskeletal Conditions
Exercise is prescribed for a broad range of conditions affecting the musculoskeletal system, with favorable outcomes and no documented deleterious effects. With increased understanding of exercise pathophysiology, physical therapists can prescribe therapeutic exercise that has the greatest benefit in terms of improved activities of daily living and life satisfaction with the least risk. Individuals with mitochondrial myopathies and nonmetabolic myopathies experience typical aerobic responses to low intensity training (i.e., improved aerobic capacity and reduced submaximal heart rate and blood lactate).4 The extent of these training effects, however, is less in individuals with nonmetabolic myopathies compared with those who have mitochondrial myopathies. Improved aerobic capacity is associated with improved self-reported functional status and quality of life in both groups.
Osteoporosis
Exercise is central to the prevention and management of osteopenia and osteoporosis. In addition to weight-bearing exercise, relatively intense exercise promotes bone density as well as a high volume of activity.5 Muscle stress across joints appears to be a critical component for osteogenesis; thus torsion around joints such as in racket sports is favorable provided risk for falling is minimized. Practicing tai chi may reduce bone loss in postmenopausal women and may have some role in the management of osteoporosis.6
Osteoarthritis
Osteoarthritis has an indirect impact on cardiovascular and pulmonary conditioning because of its effect on mobility. Aerobic exercise can improve functional aerobic capacity in individuals with osteoarthritis, but this effect is less pronounced with hydrotherapy programs.7 In response to a fitness walking program for obese people with osteoarthritis of the knee, self-efficacy tended to improve commensurate with improved functional capacity.8 When prescribing an increase in physical activity and exercise, the physical therapist needs to consider the person’s weight (not only in terms of the general health benefits of weight loss, but also in relation to the specific need to reduce weight bearing in obese patients). Given the fact that the majority of patients undergoing lower extremity joint replacement are overweight or obese,9 weight loss in conjunction with exercise is fundamental in the perioperative course of these patients with the expectation that some patients may avoid the need for surgery entirely. Even small amounts of weight gain have profound effects on joints and joint mechanics (hence, increased pain with exercise). In addition, most patients do not lose weight after their joint replacement surgery, so lifestyle changes need to be approached aggressively before, as well as after, surgery.10
Scoliosis
Individuals with idiopathic scoliosis and associated restrictive ventilatory disorder can improve pulmonary function with exercise.11 Selected exercise can improve both vital capacity and chest wall expansion by almost 20%. The role of exercise for remediation of restrictive lung dysfunction associated with other spinal and chest wall deformities warrants further investigation. Correction of spinal defects in individuals with muscular dystrophy, for example, does not improve cardiac or pulmonary function and thus may not result in appreciably improved response to exercise.12
Individuals with Neuromuscular Conditions
Stroke
Because the pathoetiology of stroke involves atherosclerosis and hypertension, individuals with stroke need to be managed comparably to individuals with systemic atherosclerosis and circulatory dysfunction. Appropriate precautions must be taken when exercising these individuals or conducting other physical therapy interventions. Within weeks after a stroke, cardiorespiratory deconditioning complicates the clinical picture, along with muscle weakness, spasticity, incoordination, and abnormal gait.13 In the subacute stage of stroke, individuals who undergo aerobic training can improve aerobic and functional abilities;14 however, these benefits may not be reflected in the long-term by indexes such as the Frenchay Activities Index.15,16 Although research is necessary to refine exercise testing and training procedures for individuals with stroke,17 there is no reason to believe that these patients would not respond to aerobic conditioning to counter the deconditioning that occurs after stroke or that this intervention would not augment gait reeducation and sensorimotor integration. Evidence supports that the application of a modified treadmill training protocol, based on exercise physiology principles, can be superior to conventional approaches to the rehabilitation of people with strokes.18
Although individuals with physical impairment secondary to stroke present methodological challenges during exercise testing and training, submaximal oxygen consumption (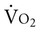 ) has good agreement with maximum
) has good agreement with maximum 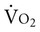 (
(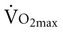 ) when the test is tightly standardized.19 The high degree of reliability of these tests supports their use as outcome measures in this population. Metabolic assessment during short, submaximal tests, such as a five-minute walk, can provide supplemental information for evaluating gait in individuals with stroke.20 Individuals with mild-to-moderate impairment from chronic stroke who require hand rail support on the treadmill also have been reported to have good reliability with respect to heart rate and oxygen pulse in peak-effort treadmill testing.21 However, hand rail support is an important variable that can increase or decrease work intensity and thus must be described and recorded to facilitate comparison of exercise results across tests. Hand rail support can be described on the data sheet with respect to side or front support, one or two hands, finger support or grasp support, and heavy or light support.
) when the test is tightly standardized.19 The high degree of reliability of these tests supports their use as outcome measures in this population. Metabolic assessment during short, submaximal tests, such as a five-minute walk, can provide supplemental information for evaluating gait in individuals with stroke.20 Individuals with mild-to-moderate impairment from chronic stroke who require hand rail support on the treadmill also have been reported to have good reliability with respect to heart rate and oxygen pulse in peak-effort treadmill testing.21 However, hand rail support is an important variable that can increase or decrease work intensity and thus must be described and recorded to facilitate comparison of exercise results across tests. Hand rail support can be described on the data sheet with respect to side or front support, one or two hands, finger support or grasp support, and heavy or light support.
Treadmill training has proven to be a useful means of improving fitness and offsetting deconditioning in individuals with stroke. Individuals with impaired gait can improve their oxygen transport reserve capacity with a regular program of treadmill walking.22 Peak 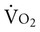 and walking workload are increased, and the energy cost associated with abnormal gait is reduced. For individuals with stroke, these changes may help to enhance functional capacity comparable to those achieved in individuals with other neurological deficits.
and walking workload are increased, and the energy cost associated with abnormal gait is reduced. For individuals with stroke, these changes may help to enhance functional capacity comparable to those achieved in individuals with other neurological deficits.
Treadmill training and weight support with a body harness for walking after stroke are showing promise in terms of conditioning strategy and gait reeducation.23 Patients with severe impairments after stroke who retrain their gait with a portion of their body weight (up to 40%) supported during exercise have better outcomes after training than those who carry their full weight.24 Older individuals and those with the most impairment show the greatest benefits. These individuals walk more symmetrically on a treadmill compared with ground walking, and they walk with less spasticity and improved movement economy.25 Furthermore, improvement in treadmill walking speed in these individuals generalizes to balance, trunk control, functional activities, and ground locomotion.24,26 Training at speeds comparable to an individual’s normal velocity over ground is more effective than training at speeds above or below that velocity.27 Also, when different treadmill walking protocols are compared, structured speed-dependent treadmill training, as performed in sports training, improves walking ability more than either modified progressive treadmill training or conventional gait training.18
Despite the compelling results of studies on partial body weight support in the rehabilitation of individuals with stroke, these and related studies often fail to address the principles of physical therapy for management of individuals with systemic atherosclerosis, which include hemodynamic monitoring and possibly electrocardiogram (ECG) screening. One exception was a study by Eng et al (2002)28 that recommended that actual exertion (defined as a physiology measure; specifically, rate pressure product or heart rate) be measured in conjunction with walking distance in functional walk tests when testing people with stroke. When performance on several functional walk tests was compared, performance was associated with level of impairment rather than perceived exertion or intensity as measured by rate pressure product or heart rate. Thus debility may limit aerobic training capacity.
Aerobic exercise may have a preventive effect for stroke mediated by endothelium-dependent vasodilation in the cerebral arterioles.29 Several risk factors are associated with impairment of this mechanism. Exercise stimulates the expression of endothelial nitric oxide synthase, which promotes vascular dilation and thereby exercise’s potential protective and preventive effect.
Community ambulation is a meaningful outcome for people with stroke.30 A discrepancy exists, however, between mobility outcomes on standardized measures of community-based individuals and the extent to which they actually get out in the community. Gait velocity is an important variable in determining community ambulation capacity.
Resistance muscle training has been of interest as a component of physical therapy management of individuals with stroke. Strength training augments the benefits of aerobic exercise with respect to functional strength31 without reinforcing abnormal movement patterns.32 One study, however, reported no difference between leg exercise training programs with and without resistance.33 Inadequate exercise prescription to explain the absence of an effect of resistance training cannot be ruled out.
Spinal Cord Injury
Spinal cord injury (SCI) can afflict anyone at any age and is certainly a risk in older adults because of the higher probability of falls. Most often, however, SCI results from trauma incurred in young adulthood, and it is more prevalent in men. Depending on the level of the injury, individuals with SCI have altered hemodynamic response to exercise and positional stress. Life expectancy has increased in recent decades for these individuals, which correspondingly has increased their incidence of cardiac risk factors and disease.34 An active lifestyle and regular exercise are imperative to ensure that these risk factors and related cardiac morbidity are reduced. Heart rate is highly correlated with respiratory minute volume, 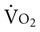 , and workload, which enables exercise to be prescribed in a predictable manner for this group. Exercise capacity is a function of the capacity of the patient to increase heart rate.35 Significant aerobic gains in peak
, and workload, which enables exercise to be prescribed in a predictable manner for this group. Exercise capacity is a function of the capacity of the patient to increase heart rate.35 Significant aerobic gains in peak 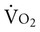 and work rate peak result from aerobic exercise in combination with functional electrical stimulation of the lower extremity muscles performed, on average, twice a week. Recovery times also improve with training.
and work rate peak result from aerobic exercise in combination with functional electrical stimulation of the lower extremity muscles performed, on average, twice a week. Recovery times also improve with training.
Individuals with SCI have a higher heart rate and lower stroke volume during exercise compared with individuals without SCI.36 Cardiac output is lower at rest. Peak exercise responses are greater for those without SCI with the exception of heart rate. Despite higher heart rates for a given workload, stroke volume and cardiac output are lower. An intact autonomic nervous system is necessary for a large increase in cardiac output and blood flow to working muscles. Thus, depending on the level of the lesion, the heart and peripheral circulation and their capacity to respond to increased work demand are affected.37 Assessment of autonomic nervous system status is key in exercise testing and training individuals with SCI.38
Arm ergometry can be used to test the aerobic capacity of individuals with SCI. Because of the small muscle mass of the arms compared with the legs, the pressure of contracting upper extremity muscles over blood vessels, and the need for postural stabilization, hemodynamic responses are disproportionately elevated compared with the same work intensity performed by the legs. With training, 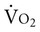 on-off kinetics, but not heart rate, is accelerated in individuals with SCI.39 Cardiac output during exercise also tends to be lower for these individuals. Thus
on-off kinetics, but not heart rate, is accelerated in individuals with SCI.39 Cardiac output during exercise also tends to be lower for these individuals. Thus 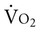 kinetics may be a prime limiter of exercise capacity in people with SCI, which could contribute to their lower anaerobic threshold with deconditioning.
kinetics may be a prime limiter of exercise capacity in people with SCI, which could contribute to their lower anaerobic threshold with deconditioning.
Wheelchair athletes with SCI show cardiovascular adaptation to exercise. Echocardiographic evidence shows an increase in left ventricular volume compared with individuals without SCI, but this adaptation is less than in healthy runners.40 Both long-term arm and leg exercise produce morphometric changes in cardiac mass and volume; however, these changes are less pronounced in wheelchair athletes compared with runners. Also, submaximal heart rates are greater for the wheelchair athletes than for runners.
Movement economy varies depending on how a specific activity is performed mechanically. Wheelchair propulsion is more mechanically and energetically efficient, using a pumping motion rather than the traditional semicircular motion.41 This has implications for energy conservation and minimization of upper extremity overload in individuals with SCI and for optimizing energy-efficient wheelchair design.
Movement economy (i.e., energy cost in relation to workload) is a concern in managing individuals with physical deformity related to musculoskeletal impairments because of the increased energy cost associated with physical activity of tasks and exercise in general. The degree to which spasticity contributes to increased energy cost is unclear. In individuals with acquired brain injury, for example, 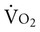 increases with exercise in a predictable, linear manner, although energy cost does not increase disproportionately with spasticity.42
increases with exercise in a predictable, linear manner, although energy cost does not increase disproportionately with spasticity.42
Finally, unlike able-bodied individuals, those with SCI do not show comparable cardiac adaptation. The typical left ventricular enlargement is not observed,43 suggesting that peripheral factors are responsible for conditioning with training in this cohort.
Chronic Effects of Poliomyelitis
The last poliomyelitis epidemic in the United States occurred in the 1950s. Individuals who had poliomyelitis as children at that time are now older adults. The delayed effects of having lived for years with poliomyelitis and its associating limitations may begin to manifest with or without postpolio syndrome (PPS). The chronic effects of poliomyelitis affect functional capacity, exercise tolerance, and cardiovascular and pulmonary risk. About 50% of individuals who had poliomyelitis develop PPS. The principles for prescribing exercise are distinct for those survivors of poliomyelitis, with or without PPS.44,45
PPS is hallmarked by new fatigue, muscle weakness, and pain.46 In addition, survivors of poliomyelitis with PPS may experience exercise intolerance, choking and swallowing dysfunction, temperature sensitivity, and psychological problems. Patients who did not have ventilatory involvement at onset, as well as those who had bulbar involvement at disease onset, may have impaired pulmonary function with PPS. During exercise, ventilatory involvement may be evidenced by impaired blood gases that are not apparent at rest.47 This has been proposed as a mechanism for delaying diaphragmatic fatigue. In addition to the chronic effects of poliomyelitis, survivors of poliomyelitis are also afflicted with the same health challenges faced by their peers who have no history of poliomyelitis. This clinical picture may be further superimposed with weight gain and reduced activity, hence, deconditioning, which is associated with aging in Western cultures.
Overuse abuse has been proposed as a mechanism of the delayed-onset effects of poliomyelitis.48 Injudicious prescription of strengthening or aerobic exercise can be deleterious to the patient because it contributes to the overuse abuse of affected, as well as unaffected, muscle.45 A reduced motor unit pool has less capacity to recover with prolonged demands, and this pool is further reduced with advancing years. With a prescribed program of rest and activity that augments muscle and endurance capacity without contributing to the patient’s symptoms, an individual can show improved tolerance to activities of daily living.44
Because of the overuse abuse phenomenon associated with PPS, an injudicious exercise program (aerobic or muscle strengthening) can lead to further overuse and progressive deterioration.49 Thus reserve capacity for exercise is assessed based on a detailed assessment so that overuse is not worsened.
An exercise test can be used to assess conditioning and movement economy, which are distinct entities.46 Modified aerobic training can be prescribed within the limits of subjective complaints of fatigue and discomfort/pain rather than with conventional indexes of exercise intensity (i.e., heart rate and blood pressure). Although conventional submaximal indexes of conditioning may not be apparent after several weeks of training, walking tolerance at subthreshold levels (measured by walking duration) may improve, along with movement economy.46 Thus some patients with a history of poliomyelitis can respond favorably to a modified walking program.
Individuals with postural malalignment experience biomechanical stress over joints during ambulation, which in turn can contribute to increased energy cost.50 An individual’s overall energy cost must be considered when prescribing exercise. Activities normally associated with low energy cost for an individual with normal posture and muscle strength can have significantly higher metabolic demand in an individual with postural deformity, limb length discrepancy, and strength asymmetry. Because fatigue and pain are symptoms associated with PPS, these subjective parameters must be monitored before, during, and between exercise sessions to monitor immediate and delayed effects and capacity to recover after exercise. In this way deleterious exercise workloads may be minimized. Overall, objective measures of walking performance are reported to be associated with subjective reports of functional capacity.51
New muscle weakness is a marker of PPS. Modified strengthening programs may benefit individuals whose muscles are weak from overuse whereas conventional muscle strengthening programs are indicated for muscles weakened by deconditioning.45 This distinction, that is, muscles that are weak and fatigued from overuse vs. muscles weak from deconditioning, is critical in the physical therapy management of this population. Stronger muscles may help improve peripheral extraction of oxygen at the peripheral level and thus contribute to an aerobic training effect and improved endurance.
Down Syndrome
Down syndrome is an example of a condition marked by mental as well as physical challenges. People with the syndrome vary widely with respect to the severity of the condition and their functional capacity, which ranges from living totally independently and being gainfully employed to being somewhat dependent in these domains. Many individuals with the syndrome benefit from physical therapy that includes a lifelong exercise program, usually commencing in childhood during growth and development. Longevity has improved as a result of improved detection and management of heart defects and prevention of respiratory complications. With greater life expectancy, individuals with the syndrome encounter many of the same acute and chronic conditions that individuals without the syndrome encounter over their lifetime, such as the diseases associated with higher civilization. Cardiac defects and sleep apnea are more common in persons with Down syndrome than in the general population.52 These conditions may affect exercise capacity; thus exercise and monitoring must be individualized to each person’s unique needs. Obesity and deconditioning can further complicate the clinical presentation. Communication style must be adapted with respect to the exercise prescription and health maintenance program. Optimal health is necessary to maximize function and long-term self-care. A caregiver may need to be involved to promote a sustained program of regular physical activity and exercise.
Individuals with Connective Tissue Conditions
Resting data are limited in predicting responses to activities of daily living and exercise. Thus exercise testing is a primary tool to assess pulmonary function dynamically and thereby unmask abnormalities that can compromise daily function.53 Women with systemic lupus erythematosus (SLE) have a several-fold increase in incidence of heart disease over other women, corresponding to an increased number of cardiac risk factors.54 In addition, hypertension and diabetes are also more prevalent in this group.
Individuals with Rheumatoid Conditions
Individuals with rheumatoid arthritis (RA) have a higher incidence of cardiovascular disease and related mortality. Despite normal left ventricular systolic function, left ventricular diastolic function is impaired without clinical evidence of cardiovascular disease, which may place this group at risk.55 At maximal exercise, heart rate, systolic blood pressure, and peak 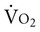 are comparable for individuals with RA and healthy people.
are comparable for individuals with RA and healthy people.
Contemporary approaches to the management of people with RA include exercise prescription for strength, endurance, and emotional well-being.56 Joint inflammation may be reduced with judiciously prescribed exercise.
Individuals with Gastrointestinal Conditions
Conditions such as irritable bowel syndrome and Crohn’s disease are characterized by disturbed homeostasis related to gut motility and function. Because these conditions are chronic and medical care is noncurative, physical deconditioning and debility are common. Few studies have examined the acute or chronic effects of exercise in this population, so specific guidelines for testing and training are lacking. One study examined the effects of moderately intense exercise (60% of 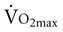 for 1 hour) on gastrointestinal function in individuals with Crohn’s disease who were in remission.57 The conventional measures of gastrointestinal function were unchanged. It may be necessary to observe caution because of oxygen metabolite production and potential zinc deficiency. Individuals with gastrointestinal conditions have nutritional deficits that must be considered when placing increased metabolic demands on energy substrate stores. The capacity of these individuals to respond to exercise appropriately will fluctuate with exacerbations and remissions of their conditions. It is hoped that with improved health and functional capacity, the duration between exacerbations will be increased, the severity of exacerbations will be reduced, and speed of recovery will be increased.
for 1 hour) on gastrointestinal function in individuals with Crohn’s disease who were in remission.57 The conventional measures of gastrointestinal function were unchanged. It may be necessary to observe caution because of oxygen metabolite production and potential zinc deficiency. Individuals with gastrointestinal conditions have nutritional deficits that must be considered when placing increased metabolic demands on energy substrate stores. The capacity of these individuals to respond to exercise appropriately will fluctuate with exacerbations and remissions of their conditions. It is hoped that with improved health and functional capacity, the duration between exacerbations will be increased, the severity of exacerbations will be reduced, and speed of recovery will be increased.
Individuals with Hepatic Conditions
The exercise responses of individuals with hepatopulmonary syndrome (HPS) are not well understood, which has hampered attempts to define guidelines for mobilization and exercise testing and training. One study, however, has shown that individuals with HPS have markedly reduced aerobic capacity and exercise-induced hypoxemia that exceeds the limitations of patients with liver disease but without the syndrome.58 Hypoxemia and increased ventilatory dead space at peak exercise support impairment in the pulmonary circulation.
Exercise capacity and maximum oxygen consumption are impaired by cirrhosis. This can be explained by an associated cirrhotic cardiomyopathy. Myocardial thickening and ventricular stiffness lead to decreased diastolic function and inotropic and chronotropic incompetence when the oxygen transport system is stressed during exercise.59
Individuals with Renal Conditions
Limitation of mitochondrial oxidative capacity has been ruled out as a limiter of exercise capacity in patients with chronic renal failure.60 Muscle oxygen conductance, however, is low.
Exercise has a role in the management of individuals undergoing hemodialysis. One study examined the role that normalizing hemoglobin has on exercise response of these individuals.61 Although both young and old subjects showed evidence of improved oxygen transport and exercise tolerance, exercise responses were not normalized completely. Further, impaired potassium regulation appeared related to hemoglobin concentration and was thought to contribute to exercise limitation.
Patients with end-stage renal disease can also benefit from exercise. Minimally, deconditioning may be prevented, but alternatively, functional status will be improved. An ideal exercise program should have both aerobic exercise and resistance muscle training components, and the prescription for both should be designed to minimize cardiovascular and musculoskeletal risks. Exercise is initiated at a low level to ensure the exercise responses are normal and the patient responds favorably before progression of the prescription. With respect to exercising patients who are severely ill, the consequences of not exercising must be considered.62 Regular physical activity, particularly when the patient is relatively stable and well, must be encouraged. This ensures that the patient is as well as possible when a change in his or her condition occurs, which in turn speeds recovery and minimizes associated challenges to aerobic and strength status.
Erythropoietin therapy in the management of patients with chronic renal failure fails to augment peak 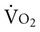 as much as might be predicted from a corresponding increase in hemoglobin.63 Lactate differences may explain abnormal muscle oxygen transport and reduced exercise tolerance in these patients. Erythropoietin-mediated increases in hemoglobin, however, reduce the respiratory exchange ratio at submaximal exercise (comparable to activities of daily living), reflecting a decrease in anaerobic metabolism and reduced exercise stress.64
as much as might be predicted from a corresponding increase in hemoglobin.63 Lactate differences may explain abnormal muscle oxygen transport and reduced exercise tolerance in these patients. Erythropoietin-mediated increases in hemoglobin, however, reduce the respiratory exchange ratio at submaximal exercise (comparable to activities of daily living), reflecting a decrease in anaerobic metabolism and reduced exercise stress.64
Chronic renal insufficiency is strongly associated with exercise-induced ischemia in individuals with atherosclerosis. The greater the severity of atherosclerosis in these individuals with chronic renal insufficiency, the greater their cardiovascular risk.65
Frequent exercise for patients with renal disease has been proposed as a means of maximizing effective use of their anemia-imposed reduced oxygen delivery capacity.66
Individuals with Hematological Conditions
Sickle cell anemia is a common hematological condition in the United States with a high prevalence in the African American population. Patients with sickle cell disease have reduced hemoglobin and oxygen transport capacity. On maximal exercise testing and endurance testing, they have lower exercise tolerance; however, their responses relative to deconditioned individuals without sickle cell anemia are generally comparable.67 Thus exercise performance of these individuals must be interpreted in this context.
Individuals with Endocrine Conditions
Special considerations include monitoring blood glucose before, during, and after exercise (immediate and delayed), at least initially when prescribing exercise for a person with diabetes. Exercise is postponed if blood glucose is extremely high and in the presence of ketone bodies. Daily regular exercise is recommended to maintain health and optimal blood glucose regulation. Intensity should be mild to moderate for a given individual.68 Exercise is judiciously timed with the intake of both foods of optimal glycemic index for the person’s needs and insulin or oral agents, as indicated. With improved glucose tolerance and insulin sensitivity and a long-term aerobic exercise program, the need for insulin or oral agents will be affected. The need for these will be eliminated, ideally, or at least reduced.
Individuals with Immunodeficiency Conditions
The pharmaceutical drugs that have been developed to improve the survival of individuals with human immunodeficiency virus (HIV) and acquired immune deficiency syndrome (AIDS) (e.g., highly active antiretroviral therapy [HAART]) can impair oxygen transport, hence reducing functional capacity. At peak exercise, heart rate has been reported to be lower and stroke volume higher in individuals with HIV taking HAART when compared with individuals with HIV not taking the drug.69 The a-vO2 difference was lower at peak exercise for those on the drug. HAART is a primary contributor to decreased muscle oxygen extraction-utilization in individuals infected with HIV. The physical therapist must be highly knowledgeable about the combined response of exercise and the potent medications used to control the disease in these individuals. This is important in order to build on an individual’s exercise reserve capacity when health is best, as well as to maintain health and social participation. It is hoped that with improved health and conditioning, morbidity and its severity are reduced.
Immunodeficiency has been implicated in chronic fatigue syndrome (CFS). This syndrome, currently of unknown etiology, appears to run its course over time. Guidelines for exercise testing, particularly maximal testing and training, have been uncertain. In one study individuals with CFS were exercise-tested to the maximal extent. Exercise responses were comparable to individuals with reduced conditioning without CFS, supporting the theory that the physiological responses of individuals with CFS were not abnormal and that exercise testing resulted in no harmful or deleterious effects.70
Individuals with Cancer
The physical capacity of cancer survivors and their capacity to respond to exercise conditioning vary depending on the primary type of cancer, the presence of metastases, chemotherapy and radiation therapy and their schedule of administration, and other morbidity.71 Mind-body considerations, including the psychological, cognitive, and physiological (immune) interface of the patient’s presentation and related outcomes, are emphasized. Given that cancer is a leading cause of morbidity and premature mortality and that many cancer survivors can expect to die with the condition rather than from it as a result of advances in cancer management, the role of exercise has been a focus of attention over the past decade or so. The goals have been to improve health and conditioning, potentially augment remission and reduce progression through immunity stimulation, and reduce the negative effects of the potent treatments that are often administered. Muscle weakness and fatigue are primary complaints of patients with cancer. These complaints are likely related to the body’s attempt to heal itself and in response to the potent treatments, as well as the overall deconditioning associated with illness.72,73
General guidelines for exercise testing and prescription include resistance training in conjunction with aerobic exercise.71 Exercise provides both psychological and physical benefits in enabling an individual to thrive when living with cancer. The parameters of the exercise program may vary depending on a patient’s response to potent radiation and chemotherapy (i.e., reducing the intensity and frequency or temporarily discontinuing the program). The role of exercise in improving the health and well-being of people with cancer and in attenuating the negative effects of potent treatments has been a hotbed of research in recent years. Significant advances can be expected in refining exercise testing and training parameters in the near future.
Individuals with Nutrition-Related Conditions
Obesity
In preparation for exercise prescription, the individual who is obese requires a comprehensive multisystem assessment to establish all factors that may limit exercise tolerance. These individuals require high volumes of physical activity and exercise (see the physical activity and exercise pyramid in Chapter 1) in conjunction with a nutritious dietary program. Introducing more exercise, however, must be done gradually so that it is as enjoyable as possible and also less likely to cause musculoskeletal strain and injury. Biomechanics change with weight loss, and exercise becomes biomechanically less stressful and better tolerated.
Prescriptive parameters for optimal weight loss remain a matter of debate with respect to prolonged, low-intensity aerobic exercise versus short, high-intensity exercise. Moderate intensities of effort, however, have been reported to be more effective at mobilizing fat, whereas heavy exercise promotes energy expenditure after exercise.2 The critical factor is the number of calories expended, and burning calories is best achieved with a regularly active lifestyle supplemented with additional formal exercise sessions. Lower-intensity exercise may be favored to avoid musculoskeletal strain or for psychological and motivational reasons. Aerobic training increases lipid oxidation during exercise in fasting conditions.74 Such a regimen maintains glucose homeostasis and facilitates fat oxidation. Additional benefits of endurance training for individuals who are obese include reduced cholesterol and insulin concentrations in the blood.
Some individuals may benefit from a structured program (see Chapter 32) and the social support of others in the program.
Anorexia Nervosa
The malnutrition and weight loss due to catabolism associated with anorexia nervosa predisposes individuals with the condition to deconditioning and impaired oxygen transport reserve capacity. Such capacity is vital to optimally respond and adapt to exercise and the physical demands of daily life in the short and the long term.75 Fluid and electrolyte imbalance can complicate the clinical picture and is the primary cause of death in extreme cases. Although quantitatively abnormal, responses to exercise may be appropriate in the absence of abnormal myocardial performance. Exercise is prescribed in conjunction with an optimal nutritional plan so that further catabolism is not precipitated.
Summary
This chapter extends the general exercise testing and training principles covered in Chapter 19 and describes special considerations for exercise testing and training individuals with cardiovascular and pulmonary dysfunction secondary to conditions other than primary chronic heart and lung disease. Exercise testing and training is one component of a comprehensive physical therapy management program that is described in Chapter 32.