Necrobiosis lipoidica
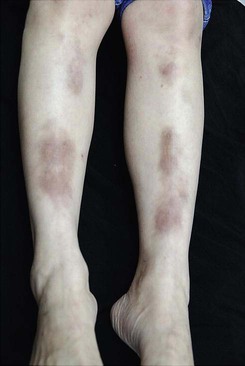
(From Pei-Shan Yen, Kuo-Hsien Wang, Wei-Yu Chen, Ya-Wen Yang, Wen-Tsao Ho, 2011. The many faces of necrobiosis lipoidica: a report of three cases with histologic variations. Dermatologica Sinica 29 (2), 67–71.)
First-line therapies
Second-line therapies
Third-line therapies






 Stop smoking and optimize diabetic control
Stop smoking and optimize diabetic control Intralesional or topical corticosteroids under occlusion
Intralesional or topical corticosteroids under occlusion Systemic corticosteroids
Systemic corticosteroids Aspirin and dipyridamole
Aspirin and dipyridamole Ticlopidine
Ticlopidine Nicotinamide
Nicotinamide Clofazimine
Clofazimine Topical PUVA
Topical PUVA Topical tacrolimus
Topical tacrolimus Topical retinoids
Topical retinoids Cyclosporine
Cyclosporine Heparin
Heparin Chloroquine
Chloroquine Mycophenolate mofetil
Mycophenolate mofetil Infliximab
Infliximab Etanercept
Etanercept Fumaric acid esters
Fumaric acid esters Promogran for ulceration
Promogran for ulceration GM-CSF for ulceration
GM-CSF for ulceration Becaplermin for ulceration
Becaplermin for ulceration Pentoxifylline
Pentoxifylline Photodynamic therapy
Photodynamic therapy Pulsed dye laser for telangiectasia
Pulsed dye laser for telangiectasia Surgery for ulceration
Surgery for ulceration Thalidomide
Thalidomide Intravenous immunoglobulins and methylprednisolone
Intravenous immunoglobulins and methylprednisolone Ultraviolet A1 phototherapy
Ultraviolet A1 phototherapy
