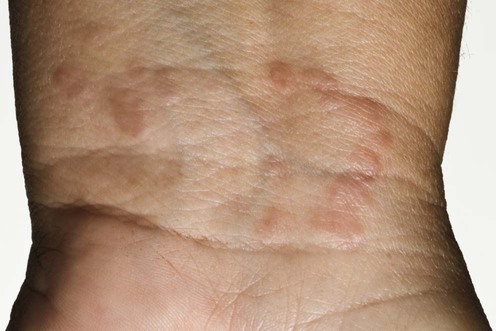
Granuloma annulare
Specific investigations
Localized granuloma annulare
First-line therapies
Second-line therapies
Generalized granuloma annulare
First-line therapies
Resolution of disseminated granuloma annulare with isotretinoin.
Schleicher SM, Milstein HJ, Lim SJ, Stanton CD. Int J Dermatol 1992; 31: 371–2.
Six women treated with isotretinoin 0.5 mg/kg/day showed complete or almost complete resolution.
There is a report in which etretinate was used successfully in this condition.


 Intralesional steroids
Intralesional steroids Cryotherapy
Cryotherapy Topical steroids
Topical steroids Laser
Laser Photodynamic therapy
Photodynamic therapy Imiquimod
Imiquimod UVA1
UVA1 Interferon
Interferon Scarification
Scarification Surgery
Surgery Rifampin, ofloxacin, minocycline combination
Rifampin, ofloxacin, minocycline combination UVA1
UVA1 Isotretinoin
Isotretinoin Dapsone
Dapsone Tacrolimus
Tacrolimus Photodynamic therapy
Photodynamic therapy PUVA
PUVA Fumaric acid esters
Fumaric acid esters Hydroxychloroquine
Hydroxychloroquine Topical steroids
Topical steroids Systemic steroids
Systemic steroids Chlorambucil
Chlorambucil Cyclosporine
Cyclosporine Hydroxyurea
Hydroxyurea Doxycycline
Doxycycline Laser (Nd : YAG)
Laser (Nd : YAG) Pimecrolimus
Pimecrolimus Adalimumab
Adalimumab Infliximab
Infliximab Allopurinol
Allopurinol Nicotinamide
Nicotinamide Pentoxifylline
Pentoxifylline Defibrotide
Defibrotide Vitamin E topically
Vitamin E topically Anthralin
Anthralin
