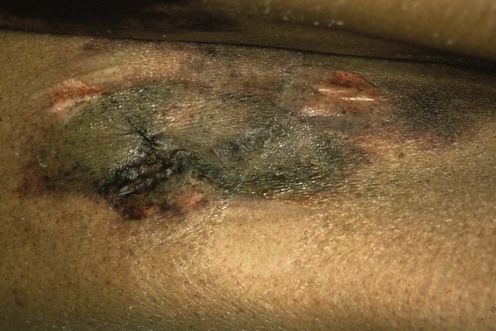
Calciphylaxis
First-line therapies
Second-line therapies
Successful treatment of severe calciphylaxis in a hemodialysis patient using low-calcium dialysate and medical parathyroidectomy: case report and literature review.
Wang HY, Yu CC, Huang CC. Ren Fail 2004; 26: 77–82.
This is one of several case reports of successful calciphylaxis treatment with low-calcium dialysis.






 Debridement of necrotic tissue and aggressive wound care
Debridement of necrotic tissue and aggressive wound care Discontinuation of calcium and vitamin D supplementation
Discontinuation of calcium and vitamin D supplementation Decrease of serum phosphorus
Decrease of serum phosphorus Treatment of low serum albumin
Treatment of low serum albumin Monitoring for infection
Monitoring for infection Intravenous sodium thiosulfate
Intravenous sodium thiosulfate Prednisone (for patients without ulcerations only)
Prednisone (for patients without ulcerations only) Pamidronate
Pamidronate Cinacalcet
Cinacalcet Parathyroidectomy (for patients with elevated parathyroid hormone)
Parathyroidectomy (for patients with elevated parathyroid hormone) Hyperbaric oxygen therapy
Hyperbaric oxygen therapy Low-calcium dialysate
Low-calcium dialysate Vitamin K supplementation in patients who are deficient
Vitamin K supplementation in patients who are deficient Tissue plasminogen activator
Tissue plasminogen activator Maggot therapy and pentoxyfillin
Maggot therapy and pentoxyfillin Ozon etherapy
Ozon etherapy Cryofiltration apheresis
Cryofiltration apheresis
