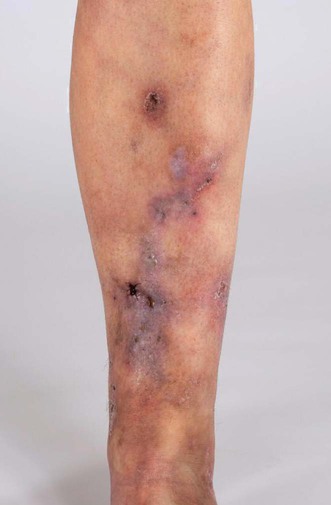
Observation (persistent aPL elevation but no thromboembolic events) Observation (persistent aPL elevation but no thromboembolic events) |
A |
 Long-term warfarin, target INR 2.0–3.0 Long-term warfarin, target INR 2.0–3.0 |
A |
 Correction of reversible prothrombotic factors Correction of reversible prothrombotic factors |
B |
 Long-term warfarin, target INR >3.0 (recurrent or arterial thrombosis) Long-term warfarin, target INR >3.0 (recurrent or arterial thrombosis) |
B |
 Low molecular weight heparin and low-dose aspirin (pregnancy) Low molecular weight heparin and low-dose aspirin (pregnancy) |
B |
 Heparin followed by warfarin (acute thrombosis) Heparin followed by warfarin (acute thrombosis) |
C |
 Thrombolytic therapy or percutaneous/surgical intervention (critical thrombosis) Thrombolytic therapy or percutaneous/surgical intervention (critical thrombosis) |
E |
 Reduction of prothrombotic risk factors, such as avoidance of prolonged immobilization Reduction of prothrombotic risk factors, such as avoidance of prolonged immobilization |
E |