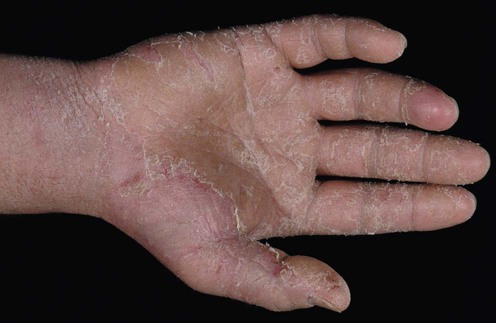
| Allergic contact dermatitis |
 Prevent contact with allergen Prevent contact with allergen |
C |
 Topical corticosteroids Topical corticosteroids |
B |
 Emollients and soap substitutes Emollients and soap substitutes |
C |
 Barrier creams Barrier creams |
B |
 Tacrolimus Tacrolimus |
B |
 Pimecrolimus Pimecrolimus |
B |
 Prednisolone Prednisolone |
D |
 Antibiotics – topical and systemic Antibiotics – topical and systemic |
D |
 Alitretinoin Alitretinoin |
A |
| Photoallergy/chronic actinic dermatitis |
 Reduction of ultraviolet light Reduction of ultraviolet light |
C |
 Sunscreens – physical agents Sunscreens – physical agents |
E |
 Tacrolimus Tacrolimus |
D |