Walk into any medical facility and your brain starts making judgments before you have even signed in.
Is the reception area calm or chaotic? Does the layout make sense? Are the staff moving with purpose or scrambling to keep up?
These are not trivial observations. The environment around you is quietly reflecting the standard of care you are about to receive.
Understanding that connection can genuinely shift how you think about your own health decisions, and those of the people you care for.
This is not a conversation about aesthetics. It is about recognising that great healthcare outcomes begin long before a patient sits on an examination table. They begin in the planning, the policies, and the financial systems that either open or close the door to proper treatment.
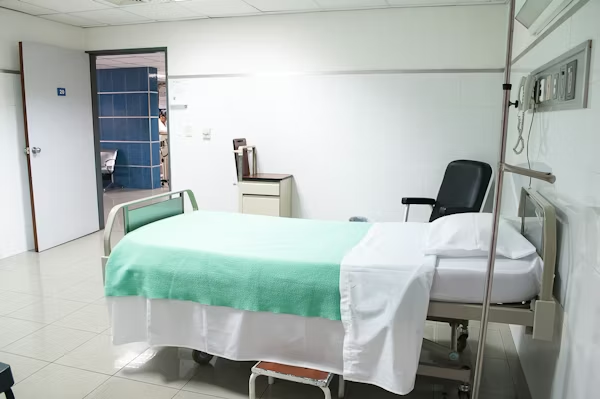
The Room You Walk Into Is Already Part of Your Treatment
Most people underestimate how much a clinical environment affects them physically and mentally.
A cluttered, poorly planned space triggers a low-grade stress response. That tension, even when it goes unnoticed, affects how clearly patients describe their symptoms. It affects how willing they are to ask questions. It even affects how well they follow through on treatment afterward.
A well-designed facility does the opposite. It signals competence before a single word is exchanged.
There are real functional consequences too. Thoughtful layouts reduce clinical errors. They improve staff efficiency. They create clear pathways for infection control that protect everyone inside the building.
None of that happens by chance.
When a practice invests in a quality medical clinic fitout, the benefits ripple outward in every direction. Staff morale lifts because the working environment is functional and dignified. Patient flow improves because the layout eliminates bottlenecks. Equipment is stored correctly and accessed quickly.
Consultation rooms provide the acoustic privacy they should. Waiting areas feel considered rather than cobbled together.
Every one of those details contributes to a clinical experience that patients trust and return to.
It is also worth remembering that a fitout is not a one-time decision made at the point of opening. As services expand, patient volumes grow, and clinical technologies evolve, the physical space must evolve alongside them.
A periodic reassessment of how a space is functioning is simply good practice management.
And then there is compliance. Healthcare environments must meet specific requirements around infection control, disability access, and clinical safety. Getting this right from the outset, rather than retrofitting it as an afterthought, saves significant time and money down the track.
A poorly planned space does not just inconvenience staff. It creates genuine risk.

Workplace Health Is a Clinical Issue, Not Just a Corporate Policy
Now shift the perspective slightly. The conversation about healthcare environments does not stop at clinic walls. It extends directly into the workplace itself.
Organisations across almost every industry are coming to terms with something that should have been obvious long ago: employee health is a core operational concern, not a human resources formality.
When workers operate heavy machinery, drive vehicles, manage medications, or make decisions affecting public safety, impairment is not a personal matter. It is a shared risk.
Substance testing has historically been handled inconsistently. Older methods were often seen as invasive, logistically difficult, and easy to resist on dignity grounds. That has changed significantly.
Oral fluid testing, in particular, has become the preferred approach for many organisations. It is non-invasive and quick to administer. It is well-suited to detecting recent impairment, which is the risk that matters most in safety-critical environments.
Organisations that rely on reliable mouth saliva drug test services are able to meet their legal and ethical obligations without making employees feel like they are under suspicion. The process is straightforward, the results are clinically relevant, and the disruption to daily operations is minimal.
An employee who tests positive for a substance that impairs judgment or reaction time is a safety concern at that moment. Responding to that promptly and consistently is not punitive. It is protective, for the individual and for everyone around them.
Workplaces that apply these standards consistently tend to attract people who genuinely value a safety culture. And that culture pays dividends well beyond incident prevention.
Organisations that engage with employee wellbeing in a structured and transparent way identify problems earlier. They intervene more effectively. They reduce the downstream costs of absenteeism, injury, and turnover that quietly drain resources year after year.
There is also a meaningful link to mental health here. When people feel that their workplace takes their wellbeing seriously, trust builds. And that trust directly affects how openly employees engage with health support programs when they need them.
Workplace health and clinical health have always been the same conversation. The organisations performing best understand that.

The Financial Barrier Nobody Talks About Enough
Here is something that does not get enough honest attention. The gap between the care people need and the care they can actually afford is one of the most persistent and quietly damaging problems in public health.
When people delay treatment because of cost, conditions worsen.
Complications develop. The eventual bill, to both the individual and to the broader healthcare system, ends up far higher than it would have been with timely intervention.
Dental health sits in a particularly uncomfortable position within this problem. It is routinely treated as a separate category from general medical care, with different funding models and significantly higher out-of-pocket costs.
The result is predictable. A large number of people are walking around with untreated dental conditions that have real consequences for their overall health.
The clinical links between oral health and cardiovascular disease, diabetes, and respiratory conditions are well-documented. You can explore the supporting research in more detail through the clinical resources available on this site. Yet the financial barrier to accessing good dental care remains stubbornly high for too many people.
There is, however, an option that a surprising number of people are completely unaware of.
Superannuation, the funds that most working adults accumulate over their careers, can in certain circumstances be accessed early to cover significant medical costs. Dental treatment is one of those qualifying circumstances.
If you have been putting off necessary dental work purely because of what it costs, it is worth taking the time to discover using your super for dental treatments as a legitimate funding pathway. The application process involves demonstrating that the treatment is medically necessary. For complex or expensive procedures, approval can remove a barrier that felt immovable.
This is not a workaround or a loophole. It is a provision that exists within the superannuation framework specifically for situations where genuine health needs arise.
Many dental providers are now familiar with this process and can support patients through the application without it feeling overwhelming.
Knowing this option exists is simply part of being an informed patient. And informed patients consistently get better outcomes.

When You See the Full Picture, Everything Connects
Pull all of these threads together and a clear pattern emerges.
The quality of care people receive is shaped by far more than what happens in the consultation room. It is shaped by the physical environment of the clinic. By the health culture of the workplace. By the financial systems that determine whether treatment is actually accessible.
A patient who comes from a workplace with a genuine safety culture, who receives care in a well-designed and functional clinic, and who has the means to access the full scope of treatment they need, is a patient positioned for good outcomes.
Close the gap in any one of those areas and it makes a measurable difference.
For practitioners, this means thinking about the patient experience more broadly. Pointing patients toward financial access options, advocating for workplace health initiatives, and investing in the quality of the clinical environment are all part of delivering genuinely good care.
For patients, it means getting curious.
Ask about your options. Look into the funding pathways that exist for treatment you have been putting off. Look at the physical environment of the practice you attend and ask whether it reflects the standards you deserve.
The system has more flexibility in it than most people realise.
For employers, it means accepting something straightforward. The health of your workforce is not a consideration separate from the success of your organisation. It has never been.
A Final Word
The best healthcare systems are not always the most expensive ones.
They are the most thoughtful. The most accessible. The most willing to address the gaps that leave people without care they genuinely need.
The physical space matters. The workplace culture matters. The financial pathways matter.
And recognising that all three are connected is exactly where meaningful change begins.

