26 Transition from the operating room to the PACU
Documentation of Handoff: Includes information about the patient’s status, assessment notes, plan of care, nursing interventions, and a continuous evaluation of nursing care and patient responses.
Patient Handoff: Transfer of information about the patient so that the next health care provider can take responsibility for the patient’s safety and care while ensuring that continuity of care is preserved.
Perianesthesia Care: Includes care of a patient undergoing a surgical procedure, intervention, or treatment that requires anesthesia or sedation during the perianesthesia continuum: before (preanesthesia), after (postanesthesia phase 1, postanesthesia phase 2, extended care).
Perioperative Care: Includes care of a patient before (preoperative), during (intraoperative), and after (postoperative) surgery.
Verbal Report: Used for a “snapshot” or abbreviated synopsis of the patient status and care delivered.
Written Report: Provides a basis for verbal reports and is usually in the form of standardized operative or anesthesia records.
Perioperative nursing
According to the Association of periOperative Registered Nurses (AORN), the goal of perioperative nursing practice is “to assist patients and their designated support person(s) with achieving a level of wellness equal to or greater than that which they had before their operative or other invasive procedures.”1 At the core of the Perioperative Patient Focused Model is the patient surrounded by the four domains of “patient safety, physiological responses, behavioral responses of the patient and support person(s), and the health system in which the perioperative care is delivered.” 1 Perioperative care is delivered by a nurse during the preoperative, intraoperative, and postoperative phases of the patient’s surgical experience in a variety of environments, including hospital surgical suites, outpatient centers, catheterization suites, endoscopy units, radiation departments, clinics, physician offices, and other sites. The model for competency for perioperative nurses is evidenced through perioperative assessment, diagnosis, outcome identification, planning, implementation, and evaluation. “Standards, knowledge, judgment, and skills based on scientific principles”1 serve as the solid foundation for perioperative practice. The perioperative nurse, therefore, has the requisite skills and knowledge to use the nursing process to design, coordinate, and deliver care to patients to meet their specific needs when their protective reflexes or self-care abilities are potentially compromised because of an operative or invasive procedure.1 The care of the surgical patient continues through the transportation to the PACU, where this care is transferred to the perianesthesia nurse.
Perianesthesia nursing
According to the American Society of PeriAnesthesia Nurses position statement on perianesthesia safety, characteristics of the culture of safety are identified by activities representing communication, advocacy, competency, efficiency, timeliness, and teamwork.2 When a patient’s care is safely transferred to another provider, these six characteristics are also present. Appropriate communication requires “ensuring a complete and systematic approach to hand-off processes and transfer of care and developing and using effective listening skills.”2 Advocacy mandates protecting the patient from injury and implementing best practices. This requires a complete understanding of the patient’s condition and status by actively participating in the hand-off process. Competency involves clinical judgment and critical thinking as the care of the surgical patient is transferred to the perianesthesia nurse postoperatively. Patient hand-offs must be timely so that efficiently of care is encouraged. Finally, teamwork is vital so that the promise of safety can be guaranteed to the recovering patient.
Implications for practice
Although handovers from an anesthesia provider to a postanesthesia care nurse are often standardized and formal, the informal elements and cultural factors must not be overlooked. For example, a PACU nurse usually sets the boundaries of when the responsibility of the patient’s care can actually be safely shifted from the physician to the nurse. If the nurse is unsure of the patient’s condition or believes that the anesthesia provider cannot safely leave the patient’s side, then the PACU nurse intervenes and freely voices these concerns.
Source: Smith AF, et al: Interpersonal handover and patient safety in anaesthesia: observational study of handovers in the recovery room, Br J Anaesth 101:332–337, 2008.
According to the American Society of PeriAnesthesia Nurses, the scope of perianesthesia nursing practice involves “age-specific assessment, diagnosis, intervention, and evaluation of individuals within the perianesthesia continuum. Those individuals have had or will have sedation/analgesia and/or anesthesia for surgical, diagnostic, or therapeutic procedures.” The practice “is systematic, integrative, and holistic and involves critical thinking, clinical decision making, and inquiry. The specialty of perianesthesia nursing encompasses the care of the patient and family/significant other along the perianesthesia continuum of care – Preanesthesia, Postanesthesia Phase I, Phase II, and Extended Care.”3
“Professional behaviors inherent in perianesthesia practice are the acquisition and application of a specialized body of knowledge and skills, accountability, and responsibility, communication, autonomy, and collaborative relationships with others.”3
The perianesthesia nurse has a responsibility to the patient to provide quality care and safety. The American Society of PeriAnesthesia Nurses (ASPAN) Perianesthesia Standards for Ethical Practice state that the perianesthesia nurse “communicates pertinent information as the patient progresses through the continuum of perianesthesia care.”3 The nurse also has the professional responsibility to collaborate “with appropriate healthcare providers as needed to ensure optimum care.” 3
According to the ASPAN Practice Recommendation 2, “components of initial, ongoing, and discharge assessment and management” provides recommendations for the different phases of perianesthesia patient care. For example, when the patient’s care is transferred from the perioperative nurse to the perianesthesia nurse in phase 1, the integration of the information about the patient should include3:
• Relevant preoperative status
• Anesthesia or sedation technique and agents
• Length of time anesthesia or sedation was administered; time reversal agents given
• Pain and comfort management interventions and plan
• Estimated fluid and blood loss and replacement
• Complications that occurred during anesthesia course; treatment initiated; response
• Emotional status on arrival to the operating or procedure room
Communication between perioperative and perianesthesia nurses
AORN recommended practices for transfer of patient care information
AORN has published a recommended practice that specifically addresses the transfer of patient care information. This recommended practice provides guidance for perioperative nurses who are responsible for accurately transferring patient information to succeeding healthcare professionals, including perianesthesia nurses. AORN has also created a hand-off tool kit available to all AORN members that provides a companion resource to the recommended practices that are described as follows.1
• Recommended practice I: “A transfer of patient information process should be developed, standardized, and based upon the best available and most current evidence.” 1 Reliability and accuracy of information is improved when standardization is enforced to prevent communication breakdowns. Everyone on the multidisciplinary team (perioperative nurses, perianesthesia nurses, anesthesia providers, surgeons, and others) should be involved with creating a format and process upon which a standardized transfer policy can be created. Written and verbal formats are both included in a successful patient transfer. When nurses use both verbal (like face-to-face interaction) and a standardized written form, data loss is minimal.4 Actual transfers should be made in an environment that has minimal interruptions and extraneous sounds.
• Recommended practice II: “Patients, families, and significant others should have an active role in transfer of patient information processes whenever possible.” 1 When families or support persons are kept informed about an impending patient transfer from surgery to PACU, anxiety is reduced and realistic expectations are promoted.
• Recommended practice III: “Personnel should receive education, training, and competency validation on effective communication skills and processes for the transfer of patient information.” 1 Because communication problems are often the cause of sentinel events, effective communication techniques and skills are mandatory.
• Recommended practice IV: “The perioperative registered nurse should document the process for the transfer of patient information using a standardized documentation format, and the document should be recorded and retained in a manner consistent with the health care organization’s policies and procedures.” 1 A standardized documentation tool promotes timely and accurate patient information and continuity of care.
• Recommended practice V: “Policies and procedures for standardized transfer of patient information processes should be developed, reviewed periodically, readily available in the practice setting, and reflect the rules and recommendations from regulatory and accreditation bodies.” 1 Policies and procedures guide practices within a health care facility, should emanate from evidence-based practices, and may often be used as the basis to validate competencies of practice.
• Recommended practice VI: “A quality management program should be implemented to evaluate and monitor the processes for the transfer of patient information. Components should include patient, process, and structural (e.g., format) outcome indicators. A fundamental precept of AORN is that it is the responsibility of professional perioperative registered nurses to provide safe, high-quality nursing care to patients undergoing operative and invasive procedures.” 1 Quality review activities help to identify communication problems, practice issues, and practices that may need improvement. Evaluation efforts of transfer activities should be ongoing to ensure patient safety and compliance with evidence-based practices.
Hand-off communication
Patient hand-offs today are extremely variable and often lack purpose and structure.5 In the past, The Joint Commission’s National Patient Safety Goals included implementation of a standardized approach to hand-off communication. The 2011 National Patient Safety Goals note that communication errors can occur when patient care is transferred from one provider to another.6 A standardized approach to patient hand-off must include a reconciled list of medications and this communication must also be documented.6 Accurately communicating the patient’s reconciled list of medications to the next provider “reduces the risk of transition-related adverse drug events.”6 The interface between the preoperative nurse to the operating room (OR) nurse and the OR nurse to the PACU nurse are crucial to continuity of care and safety for the patient. Standardizing a process in which all information about patient care is communicated in a consistent manner assures that the information about the patient will be accurate and pertinent.
During a comprehensive literature search, approximately 400 articles were reviewed that identified seven primary functions for patient hand-offs. These include7:
1. Information processing (transfer of patient data)
2. Highlighting deviations from stereotypical narratives (e.g., the patient is allergic to the preferred antibiotic that would be used to treat his or her condition)
3. Identification of erroneous assumptions and actions (e.g., a nurse questioning a surgeon or anesthesia provider about a specific patient order)
4. Accountability (e.g., transfer of responsibility and authority over the patient’s care)
5. Social interactions (in support of interdisciplinary team communication and actions)
6. Distributed cognition (promoting the ease of transfer of up-to-date information to all professionals involved in the patient’s care)
7. Cultural norms (negotiating and educating about hand-off procedures)
Hand-off information needs to be standardized and communicated in a logical and meaningful manner. Current literature notes that hand-off quality measures lack consensus regarding the primary purpose of the hand-off.7 Basic principles of hand-off practices include written and verbal communication along with the essentials of documentation.
Different standardized documentation formats have been developed that have gained popularity in the United States. These formats are easy to remember as the letters represent the name of the step within the process of handing off a patient from one provider to another. The goal of these standardized formats is to reduce communication breakdowns. Some of these formats include1:
• SBAR: situation, background, assessment, recommendation
• I PASS the BATON: introduction, patient, assessment, situation, safety concerns, (the) background, actions, timing, ownership
• SURPASS: surgical patient safety system
• SHARED: situation, history, assessment, request, evaluate, document
The SBAR is one of the most popular and accepted standardized documentation formats today. This format can be used for patient hand-offs during the perioperative experience as shown in Box 26-1.
BOX 26-1 Sample of SBAR Format Used for Perioperative Patient Transfers
Modified from Sandlin D: Improving patient safety by implementing a standardized and consistent approach to hand-off communication, J Perianesth Nurs 22:289–292, 2007.
Written and verbal communication
Researchers have documented that approximately 20% to 30% of the information relayed during a patient hand-off is not documented in the medical record.7 Written documentation provides a basis for verbal reports and is usually in the form of standardized operative or anesthesia records. AORN’s recommended practice for Documentation of Perioperative Nursing Care notes that the “patient’s record should reflect the perioperative patient’s plan of care, including assessment, diagnosis, outcome identification, planning, implementation, and evaluation.”1 Documentation should include information about the patient’s status, assessment notes, plan of care, nursing interventions, and a continuous evaluation of nursing care and patient responses. The written patient operative record facilitates communication and provides continuity of care and also serves as a legal record of the care provided.
• Why? Verbal reports highlight written documentation on the patient record. A written report records the details of the patient care, whereas a verbal report is a quick description or overview used when the patient’s care is transferred to another nurse. This communication and documentation is vital so that continuity and safe patient care can be maintained.
• When? A formal written report begins with the admission of the patient for the surgical procedure and extends through discharge from the surgical arena. Written reports that document patient information before admission or after discharge may be added to the patient’s chart. A verbal report from the perioperative nurse to the perianesthesia nurse begins with the call to the PACU to announce the completion of the surgical procedure and the request to transfer the patient to the PACU. At this time, any special needs must be communicated (i.e., ventilator needed). The verbal report continues when the patient is actually admitted to the PACU.
• Where? Ideally the written patient record is kept with the patient during transfer from the operating room into the PACU. The verbal report is given when the patient’s care is transferred from the perioperative nurse to the perianesthesia nurse in the PACU. Sometimes with a recovering patient from the obstetric unit, the postanesthesia care can be delivered in an area outside the normal postanesthesia care unit. Wherever the postanesthesia care is given, the standards of care (including communication) are no different than those used for nonobstetric surgical patients.8
• Who? Written patient reports are completed by the perioperative nurse, anesthesia provider, and surgeon (or a designee). Usually the verbal report is given by the anesthesia provider and the perioperative registered nurse. In a few surgical environments, the perioperative nurse may phone the perianesthesia nurse to give a report while the anesthesia provider and an orderly (patient care assistant) transfer the patient to the PACU. Ideally the perioperative nurse and anesthesia provider should both accompany the patient to the PACU. Sometimes the surgeon or the surgical assistant may also participate in the patient transportation and verbal report.
• How? The written patient record is documented on a health care facility–approved standardized form. The verbal report is usually given in person from one professional to another, but verbal reports have also been given via telephone or computer, depending on the patient acuity and facility protocols.
• What? The reporting of specific and appropriate information about the patient’s surgical experience is critical. The perianesthesia nurse must receive the full details of the patient’s condition, interventions, and plan of care so that continuity and safety can be maintained.
Care of certain patients, such as the patient recovering from cesarean section, can pose unique challenges. Documentation and verbal reports should alert the perianesthesia nurse to watch for signs and symptoms of adverse anesthetic effects, pulmonary problems, hemorrhage, infection, and other specific potential complications.8 The care of a pregnant patient who is transferred from the operating room presents distinctive challenges because the status of the fetus must also be assessed, documented, and reported verbally.
• Type of surgery, length of surgery, complications encountered
• Vital signs and airway patency (e.g., oxygen saturation)
• Muscular strength (e.g., mobility limitations)
• Condition of operative site and dressing
• Location and patency of tubes or drains
• Medications given and response to those medications (e.g., anesthetic agents and technique, reversal agents)
• Intake and output (e.g., intravenous, estimated blood loss)
• Tests ordered, with pertinent results, if available
• Psychosocial status (e.g., substance abuse, physical or mental impairments, prostheses)
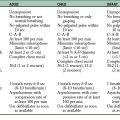
Surgical team members, including the anesthesia provider, perioperative nurse, and surgeon (or designee including fellow, resident, or intern) participate in giving the report during transfer of the patient’s care to the PACU nurse. Box 26-2 includes suggestions on what each professional should report.9
BOX 26-2 Suggestions on Topics for Report from Each Professional
Anesthesia provider may report
Perioperative nurse may report
Modified from Sullivan EE: Handoff communication, J Perianesth Nurs 22:275–279, 2007.
Documentation and reporting of patient positioning
Documentation and reporting of positioning used during a surgical procedure may seem trivial and insignificant and often may be overlooked by the surgical team members. However, patient injuries from prolonged or improper positioning during the surgical procedure have been assessed and documented by astute PACU nurses. Practices recommended by AORN note that perioperative documentation should include “patient positioning and/or repositioning devices and supports, including immobilization devices used during the surgical procedure.”1
Cardiovascular
Cardiac output can indicate intraoperative positioning injuries and can easily be assessed with measurement of the patient’s blood pressure. The following list provides some examples of how positioning in surgery can affect the patient’s cardiovascular status after surgery:
• Hypotension or hypertension can be caused by the type of anesthesia administered, but can be intensified by specific positioning during a surgical procedure.
• Regional or general anesthesia may cause peripheral blood vessels to dilate (from the relaxation of the muscle lining of the blood vessels) and may lead to venous pooling, a decrease in circulating blood volume, and a fall in blood pressure if the extremities are in a dependent position.
• Reverse Trendelenburg, lithotomy, or jack-knife positions can contribute to venous pooling because of the dependent position of the lower extremities.
• Pooling of the blood in the trunk may be caused from unusual pressure on the abdomen from the thighs during the lithotomy position, which compresses the external iliac artery that distributes blood to the abdominal wall, external genitalia, and lower limbs.
• Lowered blood pressure may be the result of unusual pressure or tension on the major blood vessels, such as the inferior vena cava, from improper positioning or through the inappropriate positioning of deep retractors.
• Hyperabduction of the arm (greater than 90 degrees) can cause axillary and subclavian vessels to be stretched and compressed between the first rib and the clavicle, which can cause the radial pulse to be undetectable and could result in arterial thrombosis.
Skin
Pressure
If the patient’s skin is thin, tissue can be easily compromised. With prolonged pressure, blood vessels may constrict and occlude and thus lead to possible ischemia, which is the first step in pressure ulcer formation. In a classic study, researchers showed that pressures of more than 32 mm Hg cause arterioles to constrict and occlude, thus leading to decreased nourishment and oxygenation of the capillary beds. Ischemia and microscopic necrosis can then result and cause pressure ulcerations.10 Injuries from prolonged pressure may not be evident for hours or even days and may even be missed by the perianesthesia nurse. Because a pressure ulcer starts at a bony prominence and extends to the skin, manifestation at the skin level takes time; therefore a pressure ulcer may not be readily identified. Researchers have noted that one in every 12 patients who undergoes surgery for more than 3 hours can have at least one pressure ulcer develop within 4 days of surgery.11
Maceration
Maceration injuries are caused by prolonged contact of the patient’s skin with fluids (e.g., pooling of preparation solutions, incontinence, sweat, or irrigants) during a surgical procedure. This contact with fluids causes the skin to weaken and become more vulnerable to pressure, shearing, or friction injuries. The perianesthesia nurse should consider maceration injuries if the skin integrity has been compromised.
Nervous system
The most frequently injured nerves from positioning problems are the following:
• The ulnar nerve extends from the upper arm to the lower arm. When the compression of the ulnar nerve is near the elbow, a clawing effect of the fingers may be present.
• Lower extremity nerves in the legs can be injured by improper stirrup use or by improper use of positioning devices.
• The brachial plexus consists of a network of nerves from the clavicle down the upper arm. When the arm is overextended, a numbness or palsy of the hand, arm, or wrist can result.
• Lumbosacral nerves are located in the lower back region. When a patient is placed in the lithotomy position for a long procedure, the lumbosacral nerves can be stretched, thus leading to weakness of the quadriceps muscle or a sensory deficit in the anterior thigh area.
Summary
Florence Nightingale wrote in Notes on Nursing in 1860, “In dwelling upon the vital importance of sound observation, it must never be lost sight of what observation is for. It is not for the sake of piling up miscellaneous information or curious facts, but for the sake of saving life and increasing health and comfort.”12
1. Association of periOperative Registered Nurses: Perioperative standards and recommended practices. Denver: AORN; 2011.
2. American Society of PeriAnesthesia Nurses: Position statement on perianesthesia safety. available at: https://www.aspan.org/ClinicalPractice/PositionStatements/PerianesthesiaSafety/tabid/3282/Default.aspx, March 27, 2011. Accessed
3. American Society of PeriAnesthesia Nurses: Perianesthesia nursing standards and practice recommendations, 2010-2012. Cherry Hill, NJ: ASPAN; 2010.
4. Pothier D, et al. Pilot study to show the loss of important data in nursing handover. Br J Nurs. 2005;14(20):1090–1093.
5. Van Eaton E. Handoff improvement: We need to understand what we are trying to fix. The Joint Commission Journal on Quality and Patient Safety.2010;36(2):51.
6. The Joint Commission: Accreditation program: hospital national patient safety goals, 2011. available at: http://www.jointcommission.org/assets/1/6/2011_NPSGs_HAP.pdf, March 27, 2011. Accessed
7. Patterson E, Wears M. Patient handoffs: Standardized and reliable measurement tools remain elusive. The Joint Commission Journal on Quality and Patient Safety.2010;36(2):52–61.
8. Torgersen K. Communication to facilitate care of the obstetric surgical patient in a postanesthesia care setting. J Perianesth Nurs. 2005;20((3):177–184.
9. Sullivan EE. Handoff communication. J Perianesth Nurs. 2007;22:275–279.
10. Kosiak M. Etiology and pathology of ischemic ulcers. Physiol Med Rehabil. 1959;40:60–69.
11. American Health Consultants: Are you overlooking your OR in the battle against pressure ulcers. Wound Care.1998;3(6):61–63.
12. Nightingale F. Notes on nursing (an unabridged republication of the first American edition published by D. Appleton and Company in 1860). Toronto: Dover Publications; 1969.