8.2 Autoimmune disease71
8.3 Transplantation72
• A defective (insufficient) immune response will compromise the host defences against microorganisms and predispose to infection. In severe cases, there is also a predisposition to certain neoplasms.
• In hypersensitivity reactions, host tissue is secondarily destroyed during an immune response.
• If the immune system fails to distinguish between self and non-self antigens, the immune system will attack normal tissues. This is autoimmunity.
• Undesirable immune responses are also seen in patients in whom there is rejection of tissue transplants.
8.1. Hypersensitivity
Hypersensitivity is a process whereby the host’s tissue is injured during an immune response to a foreign antigen. When this process is inappropriate ‘hypersensitivity diseases’ occur. They are divided into four types; types I–III are mediated by antibodies (humoral immunity), whereas type IV is mediated by cellular immunity.
Type I hypersensitivity
Type I hypersensitivity is commonly called allergy. It is due to the interaction of antigen with IgE antibody previously bound to the surfaces of mast cells and basophils. In this context, the antigen is referred to as an allergen. Type I hypersensitivity is rapid (hence its alternative name, immediate hypersensitivity) and triggers mast cells and/or basophils to release substances that cause blood vessels to dilate and become leaky and cause smooth muscle contraction in bronchial walls and elsewhere. Later, eosinophils and other inflammatory cells infiltrate the tissue, causing further damage. The reaction can be localised or generalised.
Localised reactions
Common examples of localised type I hypersensitivity reactions are asthma, hay fever and urticaria. In susceptible, sensitised individuals, exposure to antigen (allergen) results in an immediate and acute immune response mediated by IgE. The reaction can be triggered by substances which are commonly found all around us. For example, asthma can be triggered by house dust or animal proteins, and hay fever can be caused by pollen.
Generalised reactions
Rarely, antigen enters the bloodstream of a sensitised individual and binds to IgE on circulating basophils. This can lead to a severe reaction known as anaphylaxis in which there is acute bronchospasm, shock (circulatory collapse as a result of peripheral vasodilatation), and even death. This may happen to people who are sensitised to penicillin or bee stings, for example.
Sequence of events
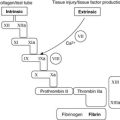
This is the same in both localised and generalised type I hypersensitivity reactions. In sensitised people, IgE is bound to the surface of tissue mast cells (and also their circulating counterparts, basophils), which have specific receptors for the Fc portion of the antibody, leaving the antigen-binding sites free to link with antigen. This binding has high affinity. After antigen and IgE have linked together, there follows an increase in membrane permeability to calcium with activation of a cascade of intracellular signals. This leads to degranulation of mast cells, which release histamine, a powerful vasodilator and constrictor of smooth muscle, and an eosinophil chemotactic factor (Table 13). Degranulation of mast cells can also be caused by substances other than IgE, e.g. drugs such as morphine, activated complement components C3a and C5a, and by physical stimuli such as heat, cold and trauma.
| Substances found in mast cell granules | Action |
|---|---|
| Eosinophil and neutrophil chemotactic factors | Chemotaxis |
| Histamine | Vasodilatation, increased permeability |
| Heparin | Late phase reactions |
| Trypsin | Late phase reactions |
| Substances made by mast cells during response | |
| Leukotrienes | Chemotaxis, smooth muscle contraction |
| Prostaglandins | Vasodilatation, smooth muscle contraction |
| Platelet-activating factor | Platelet aggregation, smooth muscle contraction, increased permeability |
Type II hypersensitivity
In type II hypersensitivity reactions, antibody binds directly to tissues: antibodies are directed against and bind with normal or altered components on the cell surface which they recognise as non-self. The presence of bound antibody induces damage by three main mechanisms:
• complement-mediated cytotoxicity: fixation of complement to the cell surface produces lysis via the membrane attack complex
• opsonisation: cells coated with antibody and complement C3b fragments are susceptible to phagocytosis
• antibody-dependent cell-mediated cytotoxicity: target cells are coated with IgG (or occasionally IgE); the cells are attacked by cells which have receptors for Fc that enable them to recognise and kill cells that have immunoglobulin bound to them. Such cells are the natural killer (NK) cells, neutrophils, macrophages, and (in the case of IgE) eosinophils. However, NK cells appear to be most important in this process.
Examples of such reactions are transfusion reactions, haemolytic disease of the newborn and Goodpasture’s syndrome.
Incompatible blood transfusion reaction
Antibodies against a blood group antigen, e.g. rhesus or ABO, bind directly to the surface of the blood cells, causing haemolysis. Thus, a patient who has antibodies to blood group B but is inadvertently given type B blood will experience massive intravascular haemolysis.
Haemolytic disease of the newborn
Rhesus (Rh) blood group antigens are present in about 85% of people (rhesus positive); the remainder of the population are rhesus negative. Rhesus antigen is inherited through a dominant gene (D) so that rhesus-positive individuals can be homozygous (DD) or heterozygous (Dd). Haemolytic disease of the newborn may arise if a rhesus-negative mother carries a rhesus-positive fetus. When fetal red cells enter the maternal circulation, usually at delivery, maternal antibodies against fetal rhesus antigen will be produced. The first rhesus-positive baby from a rhesus-negative mother is usually normal, but the mother will have become sensitised to the rhesus antigen during delivery of this pregnancy. The next time she carries a rhesus-positive fetus, she will be able to mount a secondary immune response to the rhesus antigen, causing haemolysis of the red cells in the developing fetus. Therefore, subsequent babies from a sensitised mother will tend to develop progressively more severe haemolysis. The disease can be prevented by injecting the mother with IgG rhesus antibody immediately after delivery to ‘mop up’ any fetal cells and prevent her producing natural antibody.
Goodpasture’s syndrome
Goodpasture’s syndrome is an autoimmune disease. Autoantibodies to type IV collagen develop and bind to the type IV collagen in the basement membrane of the glomeruli and the lungs. Consequently, complement is fixed and antibody-dependent cell-mediated cytotoxicity is activated, causing glomerulonephritis (see Ch. 23, Section 23.3) and inflammation of the lung.
Type III hypersensitivity
Type III hypersensitivity is caused by antigen–antibody complexes. When antibody reacts with antigen in certain proportions, complexes form that can be deposited either locally or at a distant site. The antigen–antibody (immune) complexes cause tissue damage where they are deposited, usually in blood vessel walls, where they induce an inflammatory reaction as a result of complement activation and infiltration by neutrophils.
Localised immune complex disease (Arthus reaction)
The Arthus reaction is an example of immune complex damage following injection of an antigen into the skin of an individual with high levels of preformed antibody. Within 2–8 hours, a haemorrhagic oedematous reaction occurs. After 12–24 hours, skin necrosis occurs as a result of localised vasculitis (inflammation of vessels causing necrosis of the wall) from local immune complex deposition. Histologically there is an acute inflammatory reaction with numerous neutrophils.
Systemic immune complex disease
When an antigen first stimulates the formation of antibody, there is antigen excess. As levels of antibody rise, antigen/antibody equivalence occurs and as antigen is removed, there is a relative excess of antibody in the circulation. Small soluble immune complexes are formed when there is antigen excess. They are not easily phagocytosed and may be deposited in the walls of blood vessels in the kidney (glomerulus), heart, joints and skin. Here they activate complement and cause tissue damage. Large immune complexes are formed when there is antigen/antibody equivalence or antibody excess and these are readily cleared from the circulation by macrophage phagocytosis.
There are various clinical situations in which systemic immune complexes can form and cause disease:
• infection, e.g. post-streptococcal glomerulonephritis
• autoimmune disease, e.g. systemic lupus erythematosus (see Box 8).
Box 8
Definition. Chronic autoimmune illness with fluctuating activity. Multisystem involvement, especially skin, joints, kidneys and serosal surfaces.
Age/sex. Young to middle-aged females typically.
Cause. Most cases are spontaneous and probably mediated by polyclonal B cell hyperactivity with autoantibody production and immune complex formation. The autoantibodies are antinuclear (anti-double-stranded DNA antibodies); this is diagnostic of the disease. Some cases occur in patients on drugs (hydralazine). The tissue injury is caused by a type III hypersensitivity reaction.
Pathological processes. The main pathological changes and their resulting symptoms are:
• vasculitis (inflammation of vessels) with necrosis: rashes, muscle weakness
• glomerulonephritis: haematuria, proteinuria, renal failure
• synovitis: arthritis
• pleuritis, lung inflammation: chest pain, breathlessness
• pericarditis, endocarditis: chest pain, heart failure.
Clinical course. Very varied. A few patients die rapidly with heart/renal failure. Most have a chronic illness requiring repeated courses of immunosuppressive drugs.
Type IV hypersensitivity
Type IV hypersensitivity is a reaction mediated by sensitised T cells rather than antibodies. It characterises the host response to a variety of microorganisms, including viruses, fungi, protozoans and mycobacteria, but it is also seen in many other circumstances, e.g. transplanted organs, inflammatory drug reactions, and contact sensitivities (such as poison ivy reaction). It takes time for primed T cells to react and hence there is a delay of at least 12 hours before the reaction can be seen. For this reason, type IV hypersensitivity is sometimes called ‘delayed hypersensitivity’.
The prototype of this reaction is the tuberculin test. If a small amount of protein derived from tubercle bacilli is injected into the skin of a non-immune person, there will be no reaction. However, in people who have already had tuberculosis (TB) or been immunised with BCG (bacille Calmette–Guérin derived from TB) and therefore have primed T cells, an area of reddening develops in 12 hours. The reaction is maximal at 1week and histologically the tissue at the reaction site shows granulomas, which are accumulations of lymphocytes and macrophages. The macrophages are typically transformed into epithelioid cells, and some fuse together to form giant cells (see Ch. 9).
At the first encounter with the tubercle bacillus, CD4+ T cells recognise antigen when it is presented with class II MHC molecules on antigen-presenting cells. Memory T cells are then formed. On re-encountering the antigen, sensitised T cells react with antigen on the antigen-presenting cell surface, become stimulated to produce cytokines (e.g. interleukin-2) which in turn activate CD8+ T cells and recruit macrophages into the area. Interleukin-1 from macrophages increases T cell proliferation and promotes the release of acute phase reactants, which have a number of effects including fever production.
8.2. Autoimmune disease
Patients with autoimmune disease mount an immune response against their own tissues. They typically have antibodies directed against components of their own tissues (autoantibodies) in their blood; autoantibodies can be detected serologically and serve as a clinical test for autoimmune diseases. In many cases, a hypersensitivity reaction of type II, III or IV is responsible. In some diseases, however, there is antibody-mediated cellular dysfunction, in which antibodies against cell surface receptor molecules impair their function. For example, in Graves’ disease the autoantibodies bind to the receptor for thyroid-stimulating hormone and activate it, causing the thyroid cells to secrete excessive amounts of thyroxine. Autoimmune disease can affect one particular cell type, one organ system or many systems of the body (multisystem disease).
Normally, the immune system recognises the body’s own antigens as being ‘friendly’ and does not attack them, i.e. the immune system normally exhibits tolerance to self-antigens. In essence, autoimmunity is a failure of the mechanisms of self-tolerance. The processes by which the body’s immune system is triggered to attack itself are only partially understood. It is possible that cross-reaction of an antibody produced against a foreign antigen (e.g. bacterium) with a normal tissue antigen occurs (e.g. rheumatic heart disease), or that tissue antigens can be altered by drugs. Sometimes, marked changes in major histocompatibility complex (MHC) expression occur with both increased expression and de novo expression of class II in previously negative cell types (see Table 14). In addition, abnormalities in the regulation of T and B lymphocyte function have been implicated. Two classic examples of multisystem autoimmune diseases are systemic lupus erythematosus (Box 8) and rheumatoid disease (Box 9).
| Disease | Cells affected |
|---|---|
| Graves’ disease | Thyroid epithelium |
| Type 1 diabetes mellitus | Pancreatic β cells |
| Primary biliary cirrhosis | Bile duct epithelium |
| Sjögren’s syndrome | Salivary ducts |
Box 9
Age/sex. Young to middle-aged females. About 1–2% of the adult population are affected worldwide.
Cause. Unknown. However, most patients (∼80%) with rheumatoid disease (and particularly joint problems) have circulating rheumatoid factors, which are autoantibodies, usually IgM, against the Fc region of IgG. It is thought that the disease is initiated by an infectious agent, e.g. virus or bacterium. Rheumatoid disease can be complicated by amyloid deposition (see Ch. 13).
Clinicopathological features:
• joints – the synovium is initially targeted leading to destruction of cartilage and bone and damage to tendons and ligaments
• skin – firm ‘rheumatoid nodules’ are found in about a quarter of patients, especially on the elbows. These are seen down the microscope as large necrotic areas surrounded by macrophages
• blood vessels – vasculitis
• lungs, heart, kidney – non-specific inflammation and/or vasculitis.
Clinical course. Variable. There may be sudden onset of debilitating arthritis or slow, inexorable loss of joint movements. Rarely, patients die from systemic complications (e.g. vasculitis, amyloidosis). Often a variety of powerful anti-inflammatory drug therapies are required to slow disease progression.
8.3. Transplantation
Organ transplantation is an important part of medicine that over the years has become relatively commonplace. A working knowledge of basic immune mechanisms is needed to understand the phenomenon of rejection. The target antigens are called histocompatibility antigens; the human leucocyte antigen (HLA) (MHC) antigens are the target of the most destructive reactions, hence the importance of HLA typing in transplantation. Both the cell-mediated and humoral arms of the immune response are involved in rejection reactions, which can be classified according to:
• whether the response is cell and/or antibody mediated
• the speed of evolution of the response.
Hyperacute rejection
Hyperacute rejection is antibody mediated and occurs when a donated organ is placed in a patient who has preformed, circulating antibodies to donor antigens (e.g. multiparous women, patients undergoing multiple transfusions). The rejection occurs within minutes of the new organ having its blood supply established as antibodies target HLA on the vascular endothelium. Inflammation of vessels, thrombosis and necrosis occur.
Acute rejection
Acute rejection typically appears a week or two after transplantation. It is due to cellular immunity and is initiated by the generation of CD8+ (cytotoxic) T cells which, through various effector mechanisms, destroy the donor organ. An important component of some acute rejection reactions is vasculitis causing intimal proliferation and stenosis or obliteration of graft vessels. This process, called acute vascular rejection, causes necrosis and scarring.
Chronic rejection
Chronic rejection is due to cellular immunity and takes the form of a slow diminution in organ function over time. Characteristically, plasma cells, lymphocytes and eosinophils are seen within the tissue; intimal fibrosis is also prominent.
Rejection of grafts can now be prevented, or at least slowed, by a variety of drugs (see Box 10).
Box 10
• Reduce graft immunogenicity by:
• ensuring ABO compatibility
• ‘matching’ class I and class II MHC in donor and recipient.
• Immunosuppression of recipient. The drugs used and their actions include:
• corticosteroids: cytokine gene transcription blocker
• azathioprine: metabolic toxin
• cyclosporin A: interleukin-2 gene transcription blocker
• FK506: cytokine gene transcription blocker; less nephrotoxic than cyclosporin A.
Most drugs act by inhibiting T cell function.
8.4. Immunodeficiency
You should:
• describe the pathology of AIDS.
Immunodeficiency can be classified as congenital (primary) (see Box 11) and acquired (secondary) types. The human immunodeficiency virus (HIV) is responsible for the acquired immunodeficiency syndrome (AIDS) and worldwide is the most important cause of secondary immunodeficiency. Other infections can also adversely affect the immune system, although not to the same extent as encountered in AIDS. The use of drugs also gives rise to secondary immunodeficiencies. For example, cytotoxics damage or kill replicating cells (including replicating cells of the immune system), whereas corticosteroids and immunosuppressive drugs interfere with cytokine production. Patients who are malnourished or elderly also have diminished immune responses.
Box 11
• Bruton’s agammaglobulinaemia:
• X linked
• no mature B cells, T cells normal
• recurrent bacterial infections.
• DiGeorge syndrome:
• maldevelopment of thymus gland
• no cell-mediated response; reduced T cell levels, but normal antibody levels
• recurrent viral and fungal infections.
• Severe combined immunodeficiency disease (SCID):
• autosomal recessive and X linked forms
• defect is at the stem cell level; defective T and B cell responses; virtually absent lymphoid tissue
• early death from opportunistic infections.
Immunodeficiency can also be associated with the development of cancer. Presumably, the lack of normal immune reactions to abnormal cells (see Ch. 7) allows neoplastic cells to survive and multiply. For example, some high-grade B cell lymphomas arise in the setting of severely compromised T cell function, as seen in AIDS or in patients with transplants who are taking immunosuppressive medication.
AIDS
Aetiology
AIDS follows, after a varying time interval, infection with human immunodeficiency virus (HIV).
Pathogenesis
The CD4 molecule of CD4+ T cells acts as a receptor for HIV allowing it to enter the cell. The virus then uses reverse transcriptase to produce DNA from its own RNA. The viral DNA produced is inserted into the lymphocyte’s chromosomes. The DNA may be transcribed to form more HIV or lie dormant. Tissue macrophages (CD4+) can also be infected. By insertion of viral DNA into the host genome, irreversible and permanent infection of the cell occurs. Direct lysis of CD4+ T cells, the cytopathic effects of viral RNA, DNA and protein, and inhibition of CD4+ T cell maturation as well as autoimmune destruction all contribute to the immunodeficiency. Severe immunosuppression occurs in AIDS patients, leaving them susceptible to a variety of infections and tumours.
Clinical features
Opportunistic infections
The following organisms do not affect individuals with normal immunity, or cause only mild disease, but they can cause debilitating and fatal illness in patients with AIDS (or immunodeficiency from other causes):
• Pneumocystis carinii
• atypical mycobacteria e.g. Mycobacterium avium-intracellulare
• Epstein–Barr virus (EBV)
• herpes simplex virus (HSV)
• Cryptosporidiosis
• Cryptococcosis
• Toxoplasmosis
• cytomegalovirus (CMV).
Tumours
AIDS is associated with the development of Kaposi’s sarcoma, high-grade B cell lymphomas, primary brain lymphomas and cervical carcinoma.
Brain
This is a major site of HIV infection. Most patients develop some form of encephalitis or dementia.
At-risk populations
These include:
• homosexual/bisexual men
• intravenous substance users
• recipients of blood products prior to the introduction of screening blood donations for HIV
• heterosexual contacts of members of other high-risk groups.
Transmission
Transmission is via:
• sexual intercourse (vaginal or anal)
• direct inoculation of the virus through the bloodstream, e.g. needle stick injury
• placenta (mother-to-child).
Self-assessment: questions
One best answer questions
2. Which of the following generally produces the fastest response after exposure to an antigen?
a. type I hypersensitivity
b. type II hypersensitivity
c. type III hypersensitivity
d. type IV hypersensitivity
3. A 22-year-old woman complains of pain and swelling in several joints. She also says she has been lacking in energy recently. On examination she has a facial rash and a pleural effusion. Urinalysis shows haematuria and proteinuria. Which one of the following mechanisms is most likely to be responsible?
a. anaphylactic reaction
b. immune complex disease
c. neoplastic proliferation of B cells
d. primary immunodeficiency
e. steroid-induced immunodeficiency
True-false questions
1. The following statements are true:
a. asthma is primarily a T cell-mediated immune disease
b. skin prick tests are a useful way of predicting immediate hypersensitivity reactions
c. rheumatic fever is thought to be immune complex mediated
d. Goodpasture’s syndrome is due to immune complex deposition
e. the complement product C3a can cause non-IgE-mediated mast cell degranulation
2. Immune complexes:
a. are made up of antigen and antibody
b. contain antibody of the IgG class
c. are usually insoluble
d. combine with complement, which initiates an inflammatory reaction
e. are responsible for post-streptococcal glomerulonephritis
3. Type II (antibody-mediated) reactions:
a. may involve opsonisation
b. may involve complement-mediated cytotoxicity
c. are characterised histologically by large numbers of eosinophils
d. are responsible for transfusion reactions
e. are responsible for granuloma formation in tuberculosis
Case history questions
Case history 1
A 26-year-old rhesus-negative woman with a 20-week pregnancy was admitted to an obstetric observation unit. She had not felt the baby move for 3days. An ultrasound scan confirmed the fetus was dead and a stillbirth occurred the following day. At post-mortem examination, the fetus was swollen and had massive pleural effusions and ascites. A high level of anti-D antibodies was detected in the mother’s blood. The father had a blood test which showed him to be O rhesus-positive. The woman had had three previous pregnancies by the same man; the babies were completely normal.
1. What was the underlying immunological process which led to the death of the baby? Why were there no problems with the first baby?
2. Give two other examples of this type of hypersensitivity reaction.
Self-assessment: answers
One best answer
2. a. Type I hypersensitivity can cause clinical effects in minutes or hours, because IgE-mediated mast cell degranulation occurs very rapidly.
3. b. The woman has systemic lupus erythematosus, which is a type III hypersensitivity disease. Even if you did not know the diagnosis, the involvement of multiple organs suggests a systemic autoimmune disease caused by immune complex deposition: in particular, the renal glomeruli, blood vessel walls, synovial membranes of joints and the skin seem particularly prone to accumulate immune complexes. She does not have an immune deficiency; the disease is rather caused by over-activity of the immune system. A neoplastic proliferation of B cells is multiple myeloma. This condition can cause proteinuria due to excretion of excess light chains, but it does not commonly present with the other features of this case; furthermore, it tends to cause immunodeficiency as the patient’s B cells are gradually replaced with the monoclonal proliferation. Anaphylaxis is a systemic type I reaction.
True-false answers
1.
a. False. Asthma is a disease caused by an immediate (type I) hypersensitivity reaction, mediated by IgE. The intense bronchoconstriction which causes the breathlessness and wheezing results from the action of smooth muscle contractors released by mast cells.
b. True. If a small amount of allergen such as house dust or pollen is injected into the skin of a person already sensitised to the substance, i.e. who already has IgE antibodies against the substance, an immediate wheal and flare reaction will occur. This clinical test is a useful way of predicting hypersensitivity reactions and also for determining which antigens are likely to trigger them.
c. False. Rheumatic fever is an autoimmune disease due to cross-reactive antibodies produced during an infection with the group A streptococci. The disease often affects children and usually follows a few weeks after a group A streptococcal sore throat. During the course of the immune response to the streptococci, antibodies are produced which cross-react with the body’s own tissues. There is a breakdown in the principle of self-tolerance, and the antibodies attack tissues of the heart, joints and brain, causing an acute febrile illness. This is different from post-streptococcal glomerulonephritis, which is a type III reaction.
d. False. Goodpasture’s syndrome is an autoimmune disease mediated by type II hypersensitivity; immune complexes are not a significant component of the pathogenesis.
e. True. A variety of substances cause degranulation of mast cells independent of IgE. These include the complement components C3a and C5a (the anaphylatoxins, see Ch. 5) and drugs such as morphine and physical stimuli.
2.
a. True. Classical experiments in the 1960s and 1970s showed that if rabbits are injected with bovine serum albumin (BSA), they quickly produce anti-BSA antibodies, and immune complexes of BSA-anti-BSA form. These initially circulate in the bloodstream and are then deposited in tissues (e.g. glomerulus).
b. True. IgG is nearly always the antibody involved in complex formation.
c. False. Small soluble complexes are the ones which deposit in blood vessel walls and cause damage. Large insoluble complexes are easily phagocytosed and removed by tissue macrophages.
d. True. Tissue damage occurs following the classical pathway of complement activation (see Ch. 5).
e. True. Soluble immune complexes composed of IgG and streptococcal antigen deposit in the glomerular capillary loops and initiate a complement-mediated inflammatory reaction. Alternatively, if some streptococcal antigens are positively charged they may ‘stick’ in the negatively charged matrix of the glomerulus and in situ immune complex formation occurs. There is damage to the glomerular basement membrane via a type III hypersensitivity reaction and neutrophils and macrophages are recruited to the site. Immune complexes can be demonstrated in tissue sections of the glomerulus by immunofluorescent or immunohistochemical techniques.
3.
a. True. Opsonisation is the coating of a target structure by immunoglobulin, encouraging phagocytosis.
b. True. Complement is activated by immunoglobulin.
c. False. Eosinophils characterise type I reactions. Antibody is produced by plasma cells.
e. False. Granulomas are part of the type IV response.
Case history answers
Case history 1
1. The baby died of haemolytic disease of the newborn (HDN), in this case caused by rhesus incompatibility. If a fetus inherits paternal red cell rhesus antigens that are foreign to the mother’s immune system, reaction to these antigens may occur. In this case, the father is rhesus-positive so he must have at least one copy of the D allele to pass on to his offspring. At the time of birth, leakage of the baby’s red cells into the maternal circulation occurs. If these blood cells express the rhesus antigen, the mother will recognise it as foreign and become immunologically sensitised. Although there will be no effect on the first baby, who will be a week or two old by this time, subsequent rhesus-positive fetuses will be at risk. If fetal blood crosses into the mother’s circulation during a subsequent pregnancy, maternal IgG anti-D antibodies will be produced quickly. IgG antibodies can cross the placenta and fix to the antigen on fetal red cells, causing them to be rapidly destroyed (haemolysed). In severe cases, there is hypoxic injury to the heart and liver. Liver failure results in reduced production of albumin with consequent reduced oncotic pressure and thus oedema, ascites and pleural effusions, leading to the swollen appearance of the baby. The destruction of red cells produces high levels of circulating unconjugated bilirubin, which can deposit in and damage the brain, causing fits and death if untreated. As a reaction to the loss of red cells, a phenomenon known as extramedullary haemopoiesis (EMH) occurs. Bone marrow elements producing red cells, white cells and platelets are present in sites other than the medullary cavities of bones. In severe HDN, there are red cell precursors in the liver, spleen, skin and many other organs, in an attempt to maintain red cell numbers and circulating and tissue oxygen levels. Normally, EMH is only seen in the first and second trimester when the fetus cannot fully depend on bone marrow precursors for blood formation. Sites of EMH are mainly the liver, spleen and yolk sac. Some EMH is seen in full-term infants, but the bone marrow takes over soon after birth. Not all cases of HDN are caused by rhesus incompatibility. In fact, ABO incompatibility is more common but rarely causes clinical problems, partly because the antibodies are IgM and cannot cross the placenta. The routine administration of anti-D immunoglobulin to women soon after birth means that rhesus incompatibility is now an unusual clinical problem where this prophylaxis is available.
2. Rhesus incompatibility is an example of a type II hypersensitivity reaction. Other examples include incompatible blood transfusion reactions (blood group ABO antigens), Goodpasture’s syndrome, and some autoimmune haemolytic anaemias.