Issues in ambulatory anesthesia
Issues in the postanesthesia care unit
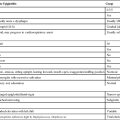
The main source for unexpected delayed discharge or hospital admission after ambulatory surgical procedures is PONV. Without prophylactic intervention, PONV occurs in 20% to 30% of the general surgical population, with higher rates in at-risk patients (Box 169-1). At this time, antiemetic medications used in anesthesia are relatively inexpensive and have minimal side effects (e.g., ondansetron), affording their routine use without significant concerns regarding overall cost or complications; the numbers required to treat to demonstrate an advantage of prophylactic antiemetic therapy is very low. Transdermal scopolamine appears to augment the effects of other antiemetics, particularly in patients with a history of motion sickness. Scopolamine should be used cautiously in men with symptoms of prostatic hypertrophy in whom urinary retention may become problematic. Although patients may initially feel well and recover from their anesthesia uneventfully, PONV may occur several hours postoperatively, suggesting a contribution from oral analgesic agents. More attention appears to be needed for improving oral analgesic-related nausea and vomiting.