Hypertension (Case 7)
Elie R. Chemaly MD, MSc and Michael Kim MD
Case: A 59-year-old African-American woman is referred by her primary physician. She has had a history of severe hypertension for 38 years. She complains of dizziness, occipital headaches with blurred vision, and palpitations correlated with high BP sometimes reaching 200 mm Hg systolic and 120 mm Hg diastolic. She also has claudication of the legs and thighs upon walking four street blocks. She has a history of thyroid disease and is presently hypothyroid. Her medications on presentation were valsartan/hydrochlorothiazide 320 mg/25 mg (one tablet daily in the morning), clonidine 0.3 mg (one tablet daily in the evening), verapamil SR 240 mg (one tablet twice a day), and levothyroxine 0.1 mg (one tablet daily). Although she takes her medications each day as directed, she confides to you that she is concerned that they are becoming increasingly difficult for her to afford on a limited budget. She has an extensive family history of hypertension, and her father died at the age of 57 years in his sleep. On examination she weighs 68 kg, her pulse is 60 bpm, and her BP is 148/88 mm Hg. Her examination is remarkable for bilateral femoral bruits.
Differential Diagnosis
|
Essential hypertension |
Obesity |
Sleep apnea |
|
Renovascular disease |
Primary aldosteronism |
Primary mineralocorticoid excess, other than primary aldosteronism |
|
Alcohol and substance abuse |
Pheochromocytoma |
Cushing syndrome (glucocorticoid excess) |
|
Iatrogenic hypertension |
Primary (parenchymal) renal disease |
Other endocrine disorders: hypothyroidism, hyperthyroidism, hyperparathyroidism, acromegaly |
Speaking Intelligently
The first assessment when approaching the hypertensive patient is to classify the patient based on the following:
1. The arterial BP measurements
2. The acuteness of the problem
3. The status of the patient in terms of antihypertensive therapy
PATIENT CARE
Clinical Thinking
• The definition of hypertension is an operational definition, which means that a BP is considered to be in the hypertensive range when it requires treatment to lower it, not just when it is above the number considered to be normal, and such treatment is required when the benefit of therapy outweighs the risk of therapy. This explains the changes in the definition of hypertension over the course of the years, motivated by treatment availability and data on treatment benefit and treatment targets.
• The seventh report of the Joint National Committee (JNC 7), published in 2003, has issued those definitions.1 Based upon the average of two or more BP readings at each of two or more visits after an initial screen, the following classification is used:
• Normal blood pressure: systolic less than 120 mm Hg and diastolic less than 80 mm Hg
• Prehypertension: systolic 120 to 139 mm Hg or diastolic 80 to 89 mm Hg
Stage 1: systolic 140 to 159 mm Hg or diastolic 90 to 99 mm Hg
Stage 2: systolic ≥160 mm Hg or diastolic ≥100 mm Hg
• If the patient is already receiving antihypertensive therapy, the diagnosis of hypertension is made. I need to assess the particular therapeutic goal for the BP of this patient, since BP treatment goals vary from patient to patient (see JNC 7 report1) and the appropriateness of the treatment.
History
The history should search for precipitating or aggravating factors as well as an identifiable cause (secondary hypertension), establish the course of the disease, assess the extent of target organ damage, and look for other risk factors for cardiovascular disease.
• Duration and course of the disease
• Medications, diet, and social history: Drugs that may aggravate or cause hypertension include sympathomimetics, steroids, NSAIDs, and estrogens; psychiatric medications causing a serotonin syndrome; cocaine and alcohol abuse. Withdrawal syndromes and rebound effects also need to be considered: alcohol, benzodiazepines, β-blockers, and clonidine.
• Symptoms of sleep apnea: early-morning headaches, daytime somnolence, snoring, erratic sleep.
Physical Examination
• Funduscopic examination to evaluate retinal complications.
• Vascular auscultation (carotid bruits, renal bruits, pulses): to assess atherosclerotic status and the presence of renal artery stenosis; the relationship between carotid artery disease, its treatment, and hypertension is not well understood.
• Abdominal examination, especially of the aorta and the kidneys.
• Neurologic examination, if applicable.
Tests for Consideration
| Clinical Entities | Medical Knowledge |
|
Essential Hypertension (90% of Patients) |
|
|
Pφ |
Essential hypertension accounts for 90% of the cases of hypertension. The pathogenesis of essential hypertension is poorly understood. In fact, it does not appear to be one disease so that, among the multiple processes involved in the development of hypertension, one particular process may dominate the pathophysiology in a particular patient or group of patients. Among the important factors involved in essential hypertension are increased activity of the sympathetic nervous system, increased activity of the renin-angiotensin-aldosterone system, increased sodium retention (concepts of low-renin hypertension and impaired pressure natriuresis), low nephron mass, increased stiffness of the aorta and central arteries (thought to explain isolated systolic hypertension in the elderly), genetic factors, diet (high sodium and probably also low potassium intake), and psychosocial factors (especially the white coat form of hypertension). |
|
TP |
Hypertension by itself is generally asymptomatic unless BP is markedly and acutely elevated (malignant hypertension). Patients may also present with symptoms related to end-organ damage from hypertension (see “complications” above). Symptoms in the acute setting include headache, epistaxis, visual disturbances and signs of encephalopathy, chest pain in cases of aortic dissection or myocardial ischemia, and dyspnea and signs of congestion in the setting of heart or kidney failure. Since an acute illness or intoxication can be the cause of acute severe hypertension, it is important to relate the elements in the particular context of the patient and draw cause-effect relationships. For example, a patient with marked hypertension and altered mental status may have a hypertensive encephalopathy or a primary neurologic disorder leading to the elevation of his or her BP. |
|
Dx |
BP elevation as described above without an evident secondary cause (see Secondary Hypertension discussion by etiology). More emphasis is placed today on ambulatory BP measurement, since it is more representative of the real BP load sustained by the body in the patient’s daily life than an office measurement. Ambulatory BP monitoring is necessary to diagnose “white coat hypertension” and “masked hypertension.” The diagnostic workup, besides establishing hypertension, includes the search for a secondary cause (other than essential hypertension), the search for end-organ damage, and the evaluation of cardiovascular risk. |
|
Tx |
BP must be properly measured and hypertension diagnosed by repeated measurements over several visits. • Drug monotherapy must be initiated at 140/90 mm Hg, and initial dual therapy may be needed above 160/100 mm Hg. |
|
Pφ |
Hypertension occurs in kidney disease, acute or chronic. It is usually seen in vascular or glomerular disease, but polycystic kidney disease also frequently results in hypertension. In acute glomerular disease, hypertension is related to sodium and water retention. In vascular disease, it is primarily the activation of the renin-angiotensin system in the ischemic kidney that causes hypertension. In chronic kidney disease, hypertension is highly prevalent, and several mechanisms are involved: sodium and water retention, activation of the renin-angiotensin system, high sympathetic tone, endothelial dysfunction, high levels of parathyroid hormone, and arterial stiffening. |
|
TP |
Elevation of the serum creatinine with a glomerular filtration rate below 60 mL/min and/or proteinuria. Edema is characteristic of acute glomerulonephritis. |
|
Dx |
Serum BUN and creatinine with urinalysis make the positive diagnosis. Etiologies are numerous and outside the scope of this chapter. Hypertension may itself cause kidney disease (nephroangiosclerosis, which can be acute, malignant or chronic). |
|
Tx |
Treatment depends on the cause. Fluid removal by diuretics and dialysis is important in acute glomerulonephritis, while inhibition of the renin-angiotensin system is important in vascular causes. Aggressive treatment of hypertension is important in chronic kidney disease to reduce disease progression and cardiovascular risk. Goal BP is 130/80 mm Hg. The treatment of proteinuria is also essential. ACE inhibitors and ARBs specifically reduce the progression of chronic kidney disease and are indicated to reduce proteinuria but can result in further decrease in glomerular filtration and hyperkalemia; thus, they need to be used carefully. Most ACE inhibitors are eliminated by the kidneys, but fosinopril is cleared by the liver. Keep in mind that a small (~30%) and limited elevation of the serum creatinine that stabilizes over 1–2 months when treating with ACE inhibitors or ARBs does not require treatment interruption but is a sign of treatment efficacy. Hyperkalemia can be managed with diuretics and/or kayexalate. Diuretics are needed to treat volume overload, and loop diuretics are needed if the glomerular filtration rate falls below 30 mL/min. See Cecil Essentials 13. |
|
Pφ |
A number of prescribed or over-the-counter medications can cause or aggravate hypertension through different mechanisms. • Licorice is discussed in the section on mineralocorticoid excess. • Glucocorticoids are discussed in the section on Cushing syndrome. • Cyclosporine causes renal vasoconstriction and sodium/water retention. • Sympathomimetics and stimulants (enhance sympathetic tone). |
|
TP |
As in essential hypertension. Malignant hypertension can occur with oral contraceptives. Edema, renal failure, and hyperkalemia can occur with NSAIDs. In the case of erythropoietin, hypertensive encephalopathy can occur with rapid rise of BP. |
|
Dx |
The association is not automatic; it may be established only when discontinuation of the medication lowers the BP. |
|
Tx |
Discontinuation or dose reduction of the responsible agent is usually effective. In terms of analgesics, acetaminophen may be better than NSAIDs (although acetaminophen was also associated with hypertension). In terms of oral contraceptives, hypertension is rare but may be severe. In the case of erythropoietin, slowly increasing the hematocrit along with fluid removal and antihypertensive therapy is helpful. Antiplatelet agents may reduce the risk of erythropoietin-induced hypertension. In the setting of cyclosporine-induced hypertension, calcium channel blockers are the drugs of choice; diltiazem can be used and reduces cyclosporine metabolism, but the benefit on cyclosporine nephrotoxicity is unproven. See Cecil Essentials 13. |
|
Hypertension Secondary to Alcoholism and Substance Abuse |
|
|
Pφ |
Alcohol: Reactive acute hypertension can occur during alcohol withdrawal, but chronic alcohol consumption, even if moderate, can lead to hypertension. The mechanism is not clear. Cocaine inhibits norepinephrine reuptake. |
|
Alcohol can lead to hypertension that may be treatment-resistant. Cocaine raises BP but usually presents with acute cardiovascular complications (myocardial infarction, arrhythmias, stroke, and also aortic dissection among other manifestations). |
|
|
Dx |
History, toxicology screen, other features of intoxication or abuse. |
|
Tx |
Abstinence and management of the (acute) complications of the intoxication. See Cecil Essentials 13, 135. |
|
Pheochromocytoma |
|
|
Pφ |
Excess production of norepinephrine, epinephrine, or dopamine by a tumor usually located in the adrenal medulla (90%), but also anywhere along the sympathetic chain. |
|
TP |
Half of the patients have paroxysmal hypertension and most of the rest have “what appears to be essential hypertension.” Some patients are normotensive. There is a triad of symptoms: headache, sweating, and palpitations. Many other presentations are possible. Secondary diabetes and a cardiomyopathy may occur. |
|
Dx |
Diagnosis is established by measurement of 24-hour urine metanephrines and catecholamines. Plasma free metanephrines can also be measured; some authors consider them the test of choice (they are sensitive but less specific). Urinary VMA (vanillylmandelic acid) is specific but less sensitive. CT scan or MRI of the abdomen should follow to locate the tumor (usually intra-adrenal; if not, can still be intra-abdominal). If using CT scan with contrast, keep in mind that iodine contrast agents can precipitate a hypertensive crisis in the setting of a pheochromocytoma. MIBG scintigraphy can locate tumors not seen on CT or MRI; MIBG scintigraphy is also useful to locate metastases of a malignant pheochromocytoma. 111In-pentetreotide scintigraphy (Octreoscan), or total-body MRI, and PET scanning are other imaging options to locate extra-adrenal or multiple tumors. A pheochromocytoma can occur in the setting of a multiple endocrine neoplasia (MEN) or a phacomatosis. Both types of syndromes bring associations of life-threatening diseases. Uncovering the association is a caveat when a pheochromocytoma is diagnosed. |
|
Tx |
Removal of the tumor after appropriate pre-operative medical preparation. Surgery is usually delayed until hypertension is controlled by a combination of α- and β-blockade; β-blockers should not be used until appropriate α-blockade is achieved. See Cecil Essentials 13, 67. |
|
Primary Aldosteronism and Other Mineralocorticoid Excess States |
|
|
Pφ |
Aldosterone can be produced in excess by a tumor or a hyperplasia of the adrenal cortex. Less commonly, disorders of the synthesis of the steroid hormones can lead to the inappropriate accumulation of steroids (aldosterone or other metabolites or precursors of cortisol) that have mineralocorticoid effect. One situation is of interest: The deficiency in 11β-hydroxysteroid dehydrogenase type 2 (11βHSD2) that converts cortisol to cortisone in the renal tubule and prevents cortisol from having mineralocorticoid action, since this enzyme can be inhibited by the ingestion of licorice and both situations lead to apparent hypermineralocorticism. |
|
TP |
Hypertension with hypokalemia and metabolic alkalosis (usually spontaneous hypokalemia). However, (severe) hypertension alone can lead to the diagnosis, and hypokalemia is thought to be a late manifestation and is often absent in patients with primary aldosteronism. |
|
Dx |
Hypertension, unexplained hypokalemia, and metabolic alkalosis. Some patients have a normal serum potassium concentration. The next step is to measure plasma renin activity and serum aldosterone levels. Typically, in primary aldosteronism, renin is suppressed and aldosterone elevated with an aldosterone-to-renin ratio above 20 and often above 50. Imaging of the adrenal glands follows to search for the adenoma, and adrenal vein sampling to demonstrate asymmetric secretion of aldosterone may be needed either if imaging is equivocal or if surgical removal of an adenoma is considered. If both renin and aldosterone are suppressed, then the hypermineralocorticism is not aldosterone-dependent. Glucocorticoid-remediable aldosteronism is one of the zebras in this category, and it requires genetic testing to demonstrate the hybrid gene in which aldosterone synthase is driven by adrenocorticotropic hormone (ACTH). |
|
Tx |
Removal of the tumor (especially if a carcinoma) and/or a mineralocorticoid receptor antagonist such as spironolactone or eplerenone. Dexamethasone suppression in the rare case of glucocorticoid-remediable aldosteronism. See Cecil Essentials 13, 67. |
|
Pφ |
Mechanisms of hypertension in obesity are complex and not fully elucidated but include impaired sodium excretion, increased sympathetic nervous system activity, and activation of the renin-angiotensin-aldosterone system. Obesity is associated with insulin resistance and hyperinsulinism, which also has complex cardiovascular consequences; obesity is also a common cause of sleep apnea (see below). |
|
TP |
Same as essential hypertension. Obesity is also a factor in resistant hypertension. |
|
Dx |
Body mass index is above 30 kg/m2. |
|
Tx |
Weight reduction, diet, and exercise. Bariatric surgery in selected cases. See Cecil Essentials 60. |
|
Sleep Apnea |
|
|
Pφ |
Increased sympathetic tone (reactive), lower nitric oxide availability. |
|
TP |
Hypertension in the setting of obesity, snoring, morning headaches, and daytime sleepiness. |
|
Dx |
Polysomnography can be ordered based on symptoms of sleep apnea. |
|
Tx |
Positive airway pressure or airway surgery. See Cecil Essentials 13, 20. |
|
Renovascular Disease |
|
|
Pφ |
Renal artery stenosis is typically caused by atherosclerosis of the renal arteries in older patients or fibromuscular dysplasia (young women). There are numerous, less common other causes. One of those that deserves attention is cholesterol embolus after an angiography, which can cause ischemic renal injury and initiate a pathophysiologic process similar to that of renal artery stenosis. A unilateral stenosis of a renal artery induces renin secretion downstream and activation of the renin-angiotensin system in the affected kidney. BP rises to restore perfusion of that kidney and the other kidney is subjected to higher perfusion pressure, which preserves overall sodium and water elimination. In the setting of bilateral renal artery stenosis, the pathophysiology is similar but hypervolemia can occur, since pressure natriuresis is impaired. |
|
Hypertension is usually severe. It can be early in onset. Refractory hypertension, worsening hypertension in the setting of preexisting essential hypertension, reduced or worsening renal function, especially if renal function worsening follows treatment with an ACE inhibitor or an ARB (the new renin inhibitor can theoretically also have that latter effect), abdominal bruit, asymmetric kidney size on imaging, and/or hypertension with flash pulmonary edema. |
|
|
Dx |
The diagnosis should be pursued only if correction of a possible stenosis is an option. Stenoses >70% are most likely to cause hypertension. The best test is arteriography, but it is invasive. Noninvasive alternatives are less sensitive. They include MR angiography, CT angiography, and Doppler ultrasound. MR angiography is less sensitive in patients with fibromuscular dysplasia and is best for proximal disease. It also has specificity issues, since it can exaggerate stenoses. The use of gadolinium is also problematic in the setting of renal dysfunction. CT angiography is also good for proximal disease but has the problem of nephrotoxic contrast. Doppler ultrasound is better at detecting bilateral disease but is time-consuming and operator-dependent. If suspicion is high and the patient is high risk, noninvasive testing is not sufficient to rule out the disease and angiography may have to be considered. The two main indications for testing are severe or progressive hypertension and ischemic renal failure. Angiography is a risky procedure (cholesterol emboli, contrast-induced renal injury). Even if a stenosis is found, its clinical significance remains to be established. A number of tests can be used to determine its hemodynamic significance (e.g., renal vein sampling for renin). In this situation the benefit of correcting the stenosis can be predicted. There is also a role for captopril renography. |
|
Tx |
Renal artery revascularization may improve hypertension and/or renal function, but the benefit of stenosis correction may be difficult to establish in the individual patient. In the setting of fibromuscular dysplasia, angioplasty is almost always effective if not curative. See Cecil Essentials 13, 31. |
|
Cushing Syndrome and Glucocorticoid Excess |
|
|
Pφ |
Primary mechanism involves overstimulation of the nonselective mineralocorticoid receptor by excess cortisol, but insulin resistance and sleep apnea are additional contributors. |
|
Cushingoid facies, central obesity, ecchymoses, and muscle weakness. Exogenous steroid administration is a key question to ask. |
|
|
Dx |
History of steroid ingestion is essential, since it is most often iatrogenic. Initial testing includes a 24-hour urine cortisol or dexamethasone suppression test. If positive, more advanced testing is needed to establish if the syndrome is adrenal (ACTH-independent) or ACTH-dependent (may be pituitary or ectopic ACTH or ectopic corticotropin-releasing factor [CRF]). |
|
Tx |
A mineralocorticoid receptor antagonist should be the best antihypertensive therapy. Otherwise, removal of the tumor producing ACTH or cortisol (or CRF) is the definitive treatment. See Cecil Essentials 13, 67. |
|
Other Endocrine Diseases |
|
|
Pφ |
|
|
TP |
Symptoms are variable but often subtle for all three entities that are detected on more or less routine laboratory testing. However, note that pulse pressure is narrow in the setting of hypothyroidism and wide in the setting of hyperthyroidism. |
|
Dx |
Hypothyroidism is diagnosed by a typically elevated TSH and low T4 if peripheral in origin, or low to normal TSH and low T4 if pituitary in origin. In hyperthyroidism it is almost always peripheral in origin, so a low TSH is characteristic (other situations are very rare). Hyperparathyroidism comes with hypercalcemia, hypophosphatemia, and high parathyroid hormone concentrations. Further workup is needed to determine the etiology. Individual situations are often complex in terms of thyroid and parathyroid disease, and their discussion is beyond the scope of this chapter. MEN should be looked for in the setting of hyperparathyroidism, since hypertension may be due to an associated adrenal or pituitary tumor. |
|
Tx |
Varies according to the entity. BP responds variably to the correction of the endocrine disorder. See Cecil Essentials 66, 74. |
Practice-Based Learning and Improvement: Evidence-Based Medicine
Title
Effect of lower targets for blood pressure and LDL cholesterol on atherosclerosis in diabetes: the SANDS (Stop Atherosclerosis in Native Diabetics) randomized trial
Authors
Howard BV, Roman MJ, Devereux RB, et al.
Institution
MedStar Research Institute, 6495 New Hampshire Avenue, Suite 201, Hyattsville, MD 20783, USA
Reference
JAMA 2008;299:1678–1689
Problem
Diabetes mellitus (DM) is associated with an increased cardiovascular risk and requires aggressive management of BP and low-density lipoprotein cholesterol (LDLc). Standard targets for these parameters as recommended by the guidelines in the DM population are SBP less than 130 mm Hg and LDLc less than 100 mg/dL.
Intervention
Participants were 499 American Indian men and women aged 40 years or older with type 2 DM and no prior cardiovascular disease (CVD) events. They were randomized to aggressive (n = 252) versus standard (n = 247) treatment groups with stepped treatment algorithms defined for both. Aggressive treatment targets were SBP less than 115 mm Hg and LDLc less than 70 mg/dL.
Outcome/effect
Primary end point was progression of atherosclerosis measured by common carotid artery intimal medial thickness (IMT). Secondary end points were other carotid and cardiac ultrasonographic measures and clinical events.
Results: Mean target LDLc and SBP levels for both groups were reached and maintained. Compared with baseline, IMT regressed in the aggressive group and progressed in the standard group; carotid arterial cross-sectional area also regressed, and there was greater decrease in LV mass index in the aggressive group. Rates of adverse events and serious adverse events related to BP medications were higher in the aggressive group. Clinical CVD events did not differ significantly between groups.
Historical significance/comments
The trial addresses a long-debated question about “the lower the better” in terms of therapeutic goals for hypertension. However, some gray zones remain: (a) The trial was randomized but open-label with blinded end points, but it would have been difficult to blind patients and providers to treatment in that case. (b) The outcome assessed is a surrogate (see Outcome/effect section) and there was no difference in the clinical event rate, though the trial duration was 3 years and the rate of cardiovascular events was low overall, making the starting sample a low-risk population. (c) The magnitude of change in the surrogate markers used as primary end point is statistically significant but may not be clinically significant. (d) There was a higher rate of adverse events related to the intervention. (e) The patient population is limited to Native Americans with type 2 DM, so applicability may be problematic. (f) As suggested by the authors in their comment, a longer follow-up is needed.
Interpersonal and Communication Skills
Determine the Likelihood of Compliance through Candid Dialogue
In the treatment of hypertension, education of the patient is paramount. The disease is usually asymptomatic and is almost always diagnosed in the outpatient setting. Its potentially devastating complications will require lifetime treatment with medications that have variable effectiveness and tolerance. It is through candid dialogue with your patient that you will sort out if the patient is likely to be compliant with your selected treatment regimen and with the monitoring and follow-up that may be required. A low-cost diuretic, for example, may be your treatment of choice. However, if you sense that the patient will not comply with the need to monitor electrolytes, use of a (more costly!) calcium channel blocker may be a more appropriate treatment regimen.
Control Personal Feelings That May Impede Effective Communication
Caring for patients with hypertension and heart disease involves, at times, multiple medications as well as lifestyle changes. It can be frustrating for physicians (and patients) when disease complications and hospital readmissions occur secondary to noncompliance with recommended treatments. There are multiple reasons why this occurs. Medications can be cost-prohibitive, confusing, or carry side effects intolerable to the patient. Lifestyle modifications are often very difficult to make. Patients may not follow instructions completely, no matter how good the advice, even if they fully understand the health consequences of their decisions. Anger and frustration can lead to difficult interactions between doctors and their patients. In the most extreme circumstances, a physician may be unable to care for a particular patient because of personality incompatibility, or the patient may ask to have a different doctor altogether. There is no such thing as walking away from difficult patients. In such cases, it is the responsibility of the physician to continue to care for the patient until a suitable accepting physician is identified.
Systems-Based Practice
Hypertension: Effective Treatment Is Cost-Effective for the Patient and the System
Hypertension is largely undertreated and is a risk factor for numerous complications that affect life expectancy and quality of life, such as heart attacks, strokes, and renal disease. The social and economic consequences of hypertension are enormous. There is overwhelming evidence demonstrating that aggressive treatment of hypertension is a highly cost-effective intervention. Unfortunately, multiple social and economic factors such as obesity and physical inactivity confound the appropriate care of the hypertensive patient. Efforts to prevent and control the disease are needed beyond the physician-patient relationship and involve complex social and even political factors.
Reference
1. Chobanian AV, Bakris GL, Black HR, et al. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The JNC 7 Report. JAMA 2003;289:2560–2572.
Suggested Readings
Calhoun DA, Jones D, Textor S, et al. Resistant hypertension: diagnosis, evaluation, and treatment. A scientific statement from the American Heart Association Professional Education Committee of the Council for High Blood Pressure Research. Hypertension 2008;51:1403–1419.
Kaplan NM, Lieberman E, Neal W. Kaplan’s clinical hypertension. 8th ed. Philadelphia: Lippincott Williams & Wilkins; 2002.
Morrison A, Vijayan A. Hypertension. The Washington manual of medical therapeutics. 32nd ed. Philadelphia: Lippincott Williams & Wilkins, 2007, Chapter 4, pp. 102–118.
Victor RG. Arterial hypertension. Cecil Medicine, 24th ed. Philadelphia: Saunders/Elsevier, 2012, pp. 373–389.
Thorough and continuously updated reviews on several subjects can be found on www.uptodate.com. These include an overview of hypertension in adults, hypertension in kidney disease, and the screening for renovascular hypertension.

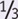 SBP +
SBP + 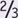 DBP but is best measured directly by integrating the BP waveform in the arterial line; automated BP cuff machines give mean BP directly).
DBP but is best measured directly by integrating the BP waveform in the arterial line; automated BP cuff machines give mean BP directly).
