!DOCTYPE html>
Anaesthesia for paediatric liver transplantation
32.8 Transfer to intensive care unit
The first paediatric liver transplant was performed in 1963 by Thomas E. Starzl in Denver, Colorado, on a baby with biliary atresia [1]. With the development of cyclosporine and other immunosuppressive agents [2] since that time, as well as the development of new surgical techniques, there are now more than 140 transplant centres in the United States alone. Several hundred transplants are now performed each year both in the United States and abroad, all with significantly reduced morbidity and mortality [3].
No one individual can take credit for a successful outcome when a child is undergoing liver transplantation, as it requires a multidisciplinary team. This consists of surgeons, anaesthesiologists, operating room nurses, scrub technicians, hepatology advanced practice nurses (APNs), fellows, attending faculty members, intensive care unit (ICU) fellows, ICU nurses and other ancillary personnel, among many others. All of these people are vitally important for ensuring good outcomes in these medically complex children. Anaesthesiologists play an integral part of this team. Developing an anaesthetic plan for these patients involves careful preoperative evaluation, close intraoperative monitoring and frequent communication with the surgeon and other specialties involved in the care of this child.
It is imperative that a careful preoperative assessment be performed when a child presents for liver transplantation. This begins with a thorough history and physical examination. The anaesthesiologist should focus on the extent of liver disease and any comorbidities, including but not limited to
• Cause of liver failure and reason for transplant
• Coagulation status (prothrombin time [PT]/partial thromboplastin time [PTT]/international normalised ratio [INR], fibrinogen, platelets)
• Sequelae of portal hypertension (oesophageal varices, significant ascites, etc.)
• Current liver and renal function
• Cardiopulmonary comorbidities
• Review of recent cardiology evaluation and any imaging studies (e.g. echocardiography)
• Acid/base status
• Electrolytes and blood glucose (especially any existing hyperkalaemia)
• Temperature irregularities
• Prior surgeries or procedures
• Any other existing comorbidities and their anaesthetic implications
In addition to the preoperative evaluation, the anaesthesiologist should discuss with the patient and family members the preoperative plan, as well as the risks and benefits of the anaesthesia associated with the procedure. Liver transplantation is a high-risk surgery. As with any other high-risk procedure, possible complications, including massive haemorrhage; risks of blood transfusion, death or major neurologic, cardiac or pulmonary complications; and the need for reoperation, should be discussed.
It is important to be aware of the patient–family unit’s ability to hear and understand the conversations that are taking place. The discussion can also be tailored to the developmental level of the patient. Unnecessary anxiety and fear can thus be avoided.
Liver transplants are commonly performed at all hours of the day or night. However, there is usually a 6- to 8-hour lead time between the notification of a transplant to the operating room staff and the actual transplant for deceased donor transplants, and living donor transplants are often scheduled weeks in advance. Ample time therefore exists for preanaesthetic planning, including establishing initial intravenous (IV) access or preoperative central access (e.g. peripherally inserted central catheters or PICC lines), preoperative laboratory evaluation and review of any and all of the patient’s history. Blood products are ordered by the surgical team and are included in the preoperative orders.
For preoperative lab evaluation, serum electrolytes (specifically Na/K+), renal function, complete blood count (CBC) and platelet count, coagulation status (PT/PTT/INR) and type and cross-match of blood products should be performed. In addition, it is common practice to notify the blood banking services of these cases, so that adequate personnel are available and blood products are in ample supply in the event of a massive transfusion requirement. This of upmost importance in patients with a very high risk of haemorrhage, including but not limited to redo liver transplants, patients with a history of prior abdominal surgery with adhesions, patients with significant coagulation abnormalities and patients receiving a reduced-size graft with a cut liver edge.
Upon arrival in the preoperative holding area, a final assessment should take place prior to proceeding to the operating room. This includes identification of any airway abnormalities, loose teeth or anything (facial hair, facial dysmorphism, etc.) that could potentially make mask ventilation and intubation difficult, as well as any underlying ascites or positional respiratory compromise. Fasting status should also be verified, as well as any other aspiration risk. The need for initial IV access should be noted. Perioperative anxiety is often present in these patients, since stranger anxiety has its onset at about 9 months of age. This can be treated with oral midazolam 0.25–1.0 mg/kg or IV/intramuscular (IM) midazolam 0.1–0.2 mg/kg. Preoperative anxiolysis is acceptable in these patients, despite significant liver dysfunction, as the clearance in these patients of a one-time dose of midazolam is only slightly impaired [4].
The standard preoperative check should be performed by the anaesthesia and nursing staff upon arrival to the operating room. Close attention when moving the patient on the operating room table will prevent dislodging of any IVs or indwelling catheters. Patients who are already intubated and coming from an ICU should be transported to the operating room with emergency drugs and airway supplies should the patient be inadvertently extubated or become acutely unstable on transport.
Once in the operating room, the standard monitors are attached with the assistance of the nursing staff so as to avoid the operative field. As there is a risk for life-threatening hyperkalaemia upon reperfusion, the application of defibrillation or pacing pads on the patient prior to incision is advisable.
The use of induction agent and technique should be individualised for each patient after careful consideration of underlying liver pathology, haemodynamic abnormalities, electrolyte abnormalities, presence of ascites, history of gastrointestinal bleeding from any gastric varices and so forth. Sevoflurane is commonly used for the induction of younger and healthy vigorous patients who lack IV access and who do not have severe ascites, vomiting or any other aspiration concerns. Propofol (2–3 mg/kg IV) is often well tolerated in haemodynamically stable patients, even in liver failure; however, etomidate (0.2–0.3 mg/kg IV) and ketamine (1–2 mg/kg IV) are suitable alternatives.
For rapid sequence induction in normokalaemic patients, succinylcholine (1–2 mg/kg IV) is acceptable. Otherwise, high-dose rocuronium (1.2 mg/kg IV) is preferable. For anaesthetic maintenance, isoflurane is often selected, as this has been shown to preserve splanchnic blood flow [5] and vasodilate hepatic vasculature for improved perfusion [6]. Also, we advocate low fresh gas flows for maintenance during the procedure to also help maintain normothermia. Additional intraoperative analgesia is provided by narcotics, often given by infusion. Fentanyl is most often chosen, as its metabolism is mostly unchanged in liver disease [7]. Cisatracurium is often then chosen via infusion as the mode of muscle relaxation, as it is metabolised independent of liver metabolism [8].
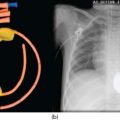
Orotracheal intubation with a cuffed tube is utilised for most patients, even small infants. If the patient is already intubated, a recent chest X-ray should be reviewed for ideal tube placement. In some cases, it may be prudent to replace the endotracheal tube (ETT) altogether if a cuffed ETT or different-sized ETT is desired.
The establishment of large-bore venous access is critical for liver transplantation, since sudden massive haemorrhage necessitating rapid blood product administration can occur. Invasive monitoring for real-time blood pressure and central venous pressure (CVP) monitoring is extremely useful and advisable.
Standard anaesthesia monitoring should be utilised in these cases, including electrocardiogram, pulse oximetry, fractional inspired O2, noninvasive blood pressure monitoring, end-tidal CO2, central temperature and urine output.
32.6.1 Peripheral intravenous lines
Typically, it is wise to establish two large-bore cannulas in large veins for volume resuscitation. It is important to place them in the upper extremities, recognising the fact that during the anhepatic phase, the inferior vena cava (IVC) is clamped, which significantly decreases venous return from the lower extremities. Also, it is common practice to have them on separate extremities, to avoid fluid overload of one extremity. In small children, however, they are placed where there are suitable vessels. Ultrasound (US) or infrared vein-finding tools are useful as well. Additional help from surgeons or interventional radiologists can also aid in the placement of proper IV access.
At our institution, once adequate large-bore venous access is obtained, it is attached to a rapid transfusion device or other blood product administration device and tested for patency and the maximum flow which can be delivered through the cannula.
To prevent the situation where boluses of banked blood with high potassium levels are given directly into the heart via central access, large-bore peripheral access is often preferred in younger neonates, infants and children, as this minimises the risk of life-threatening hyperkalaemia associated with massive transfusion [9].
32.6.2 Intra-arterial lines
Invasive arterial access is useful, as it provides real-time blood pressure measurement as well as arterial blood gas (ABG) sampling. The radial artery is preferable for most cases due to possible partial aortic clamping during the procedure. At our institution, for smaller (<20 kg) patients, a 22 g angiocatheter is used to access the radial artery, and for those >20 kg, a 20 g angiocatheter is used. If radial access is not possible, the dorsalis pedis or posterior tibial arteries are attempted; however, these may be difficult to access during the anhepatic phase. Although these lines can be unreliable, they do allow avoidance of femoral artery cannulation with its associated risk of limb ischaemia. If femoral artery cannulation is performed, we use a 2.5 Fr catheter if <10 kg and a 3 Fr (polyethylene) catheter in those who are >10 kg. Aids for arterial cannulation include US or an interventional radiologist’s assistance. The surgeons can also assist by placing a femoral arterial line. Once an arterial line is placed, a baseline ABG and point-of-care electrolytes and haemoglobin are often measured.
Some institutions, given the frequency of surgeons leaning on the cuff and often dampening of these lines during the 8- to 12-hour procedure, will place two arterial lines. Long surgical times, mechanical interference with line function and the ability to sample and monitor simultaneously make the utilisation of two arterial lines beneficial. However, this is dependent on the institution, patient and anaesthesiologist preference.
32.6.3 Central access
Central venous access is strongly recommended in these patients, as this allows the anaesthesiologist to measure CVP and deliver often needed vasoactive infusions. It also allows rapid delivery of medications directly into the central circulation. At our institution, the vast majority of these patients have at least a double-lumen PICC if >10 kg or a single 3–3.5 Fr lumen if <10 kg, placed by interventional radiology either the day before the scheduled transplant or in the operating room prior to surgical incision. If this is unavailable or not common practice, the internal jugular or subclavian veins are also suitable for cannulation, with the internal jugular vein being a more ideal choice, as this is more readily compressible in the event of haematoma formation. In older teenage patients and adult patients, the internal jugular vein can be accessed with two separate wires. This is so that a large-bore central venous catheter may be placed for blood product administration, as well as a second line for added central pressure monitoring.
32.6.4 Pulmonary artery catheter
There is controversy regarding the use of pulmonary artery (PA) catheterisation in paediatric patients. Although most studies do not suggest that the use of PA catheters in paediatric patients increases mortality [10], there are a few which have noted life-threatening complications, especially in high-risk populations [11,12]. We currently do not use these catheters routinely. However, when present, they can be utilised for temperature, continuous cardiac output, mixed venous oxygen saturations and PA pressures.
32.6.5 Other monitoring
32.6.5.1 TRANSCUTANEOUS HAEMOGLOBIN MONITOR
This is a noninvasive haemoglobin monitor incorporated into a pulse oximeter. It can be used as a surrogate monitor for blood loss. For its proper function, there must be no motion and no other light interference, as there can be inaccuracies in the measurements; as such, it should not solely be used to guide transfusion management [13]. At our institution, we utilise it as a trend monitor for blood loss, but not as a sole replacement for serum haemoglobin measurement.
32.6.5.2 TRANSOESOPHAGEAL ECHOCARDIOGRAPHY
Transoesophageal echocardiography can be placed preoperatively or emergently intraoperatively if the patient develops unstable haemodynamics not explained by intra-operative blood loss. However, given that most patients have a preoperative echocardiogram, its use is primarily for cardiac function and volume status monitor. However, at most paediatric institutions, cardiologists must be consulted and be present for probe placement and intraoperative interpretation.
32.7.1 Preanhepatic period
Once the patient is intubated, but prior to prepping and draping, all monitors and lines should be checked for patency and proper placement. It is often helpful to label lines and pulse oximeters if necessary to avoid confusion later in the case. Any antibiotics and steroids should be given as directed by the surgical team.
During the preanhepatic period, the native liver and the biliary tree are removed after ligating all the vascular and biliary connections. Patients with impaired synthetic liver function and patients with prior abdominal surgery can have a prolonged preanhepatic stage complicated by massive bleeding [14]. If a large volume of ascites is drained, one can expect severe hypotension as preload is decreased and rapid fluid shifts occur, necessitating volume replacement with colloid-containing solutions or vasopressors.
Regarding the use of blood products during this time, there is a wide range of clinical practice among institutions, surgeons and anaesthesiologists [15], and it is our practice to use our clinical judgement to guide our blood product administration.
Goals during the preanhepatic period are
• Maintenance of haemodynamic stability.
• Normothermia and normoglycaemia.
• Replacement of blood or volume losses.
• Avoidance of significant acidosis and hyperkalaemia. This can be difficult in patients who have any element of hepatorenal syndrome or renal dysfunction, or in the setting of blood administration.
32.7.2 Anhepatic period
The anhepatic phase begins with cross-clamping of the IVC, hepatic veins and portal vein. It ends with the unclamping of the vena cava and portal vein. It is typical for this phase to last 30–90 min, although it can last longer depending on individual patient and graft factors. During this period, the important goals are
• Maintenance of intravascular volume and haemo-dynamic stability without overtransfusion or volume overload, ensuring a low-normal CVP.
• Maintenance of normoglycaemia
• Maintenance of normothermia
• Maintenance of low-normal potassium levels
• Maintenance of acid–base balance
If hypotension occurs during this time, it is our practice to maintain blood pressure with judicious vasopressor use. Administration of large volumes of IV fluid and blood products can lead to congestion of the liver, so generally most practitioners will utilise a low-normal CVP technique (8–12 mmHg), with supplementation of vasopressors as needed to maintain perfusion. Hypotension may be due to loss of preload instead of bleeding, so this is important to keep in mind. This is present also with removal of the vascular clamps, as a large volume of blood will be diverted to the new liver.
32.7.3 Reperfusion
This occurs with unclamping of the portal vein and suprahepatic and infrahepatic vena cavae. This is often one of the potentially riskiest and haemodynamically unstable times during the procedure, as a massive bolus of cold fluid, potassium and other ischaemic factors, and possibly venous air emboli, are released into the recipient patient’s circulation from the donor liver, resulting in hypotension, arrhythmias and even cardiac arrest [16]. This is known as postreperfusion syndrome. The goal of this period is to maintain end-organ perfusion and haemodynamic stability and avoid or treat any life-threatening arrhythmias and hypotension.
Below is a checklist for reperfusion:
• Adequate heart rhythm and rate.
• Electrolytes: correct calcium and treat any acidosis and hyperkalaemia (goals are generally as low as possible, generally less than 3.5–4.0).
• Treatment of hyperkalaemia includes hyperventilation, calcium chloride boluses for cardiac protection, sodium bicarbonate, insulin or dextrose, inhaled albuterol and furosemide. In the event of renal failure or profound hyperkalaemia, intraoperative dialysis may be undertaken, but this involves considerable planning.
• Discuss and start vasoactive infusions as needed, generally dopamine or epinephrine to maintain blood pressure or perfusion.
• Patient temperature can be expected to drop over a degree or more centigrade; our temperature goal is to be at least 36° before reperfusion. During this time, the room temperature is often raised, and the forced air warmers are utilised.
• Right before reperfusion, it is common to administer calcium (10–20 mg/kg), lidocaine (1.5 mg/kg), sodium bicarbonate (1–2 mEq/kg) and IV epinephrine (0.5–1 μg/kg) with repeated boluses as necessary. One hundred percent O2 and transiently decreasing volatile anaesthetic agent are other measures used in order to mitigate any hypotension and hyperkalaemia which may occur with reperfusion.
• Vigilance and close communication among the peri-operative team are imperative during this period, as is the readiness and ability to treat any life-threatening arrhythmias which may ensue due to reperfusion. Rarely, there is need to use preoperatively placed defibrillator pads or surgeon-performed chest compressions.
32.7.4 Neohepatic period
Once the portal vein and vena cava are unclamped, the neohepatic phase begins, which usually starts with the hepatic artery anastomosis, followed finally by the biliary anastomoses. Either a choledochocholedocostomy or a Roux loop hepaticojejunostomy is done. Also at this time, general ‘drying up’ and correcting any surgical causes of bleeding is performed. Multiple lab values are often frequently checked during this time, including electrolytes, coagulation studies and platelet count or CBC. This period ends with the conclusion of the procedure.
This period can be marked by ongoing blood losses (especially from a reduced size graft with a cut surface), as well as any bleeding secondary to coagulopathy or from vascular anastomotic sites. If and when the graft begins to function, the acid–base status and electrolyte abnormalities will quickly begin to reverse, and oliguria due to hepatorenal syndrome will improve.
At our institution, the administration of fresh-frozen plasma-packed red blood cells or cell saver is directed primarily by the anaesthesiologist. However, a discussion with the surgeon regarding the use of platelets or cryoprecipitate usually takes place at our institution, as they are concerned about the risks of hepatic artery thrombosis (HAT) in smaller, younger paediatric patients.
32.8 TRANSFER TO INTENSIVE CARE UNIT
Haemodynamically stable patients whose surgical procedures were short and not complicated by intraoperative blood loss may be extubated in the operating room. Often, extubation in the operating room is transplant centre and anaesthesiologist dependent, and can also depend on a variety of patient, surgical and graft factors [12,13]. Below is a set of some of the extubation criteria [17,18] used by some centres with reported success. However, mostly patients remain intubated postoperatively.
• Low PELD or MELD score
• Excellent graft and renal function
• Relatively short operative time
• Absence of preoperative encephalopathy
• Absence of pressor need
• Limited blood transfusion during procedure and no evidence of ongoing coagulopathy
• Normothermia
• Normal acid–base balance
• Minimal ventilator pressure settings with adequate ventilation
• FiO2 < 0.4
Transfer to the ICU takes place following the procedure. In anticipation for transport to the ICU, emergency airway and resuscitation equipment and blood products, fluids and medications are prepared. Although surgery has ended, the patient is in critical condition, and may not tolerate the haemodynamic stress of transport, the restrictive effect on ventilation following closure of the abdomen and continued ongoing blood loss. Extreme vigilance is required during this period.
Upon arrival in the ICU, once the patient is stabilised, a complete report is given. Participants include the surgery team, anaesthesia team and PICU team and nursing staff. At our institution, this includes a brief patient history, discussion of anaesthetic induction and maintenance, preoperative lab abnormalities, physical exam findings, lines, intubation characteristics and important events that occurred during the case, including cold ischaemic cross-clamp time and reperfusion times. We transfer care to the ICU team postoperatively for further management, with our team following postoperatively in the event of the need to return to the operating room.
1. Starzl TE, Marchioro TL, Von Kaulla KN, et al. Homotransplantation of the liver in humans. Surgery, Gynecology & Obstetrics 1963; 117: 659–676.
2. Starzl TE, Todo S, Fung J, et al. FK 506 for liver, kidney, and pancreas transplantation. Lancet 1989; ii (8670): 1000–1004.
3. Steadman RH. Anesthesia for liver transplant surgery. Anesthesiology Clinics of North America 2004; 22: 687–711.
4. Amarapurkar DN, Deepak N. Prescribing medications in patients with decompensated liver cirrhosis. International Journal of Hepatology 2011; 2011: 519526. doi:10.4061/2011/519526.
5. O’Riordan J, O’Beirne HA, Young Y, Bellamy MC. Effects of desflurane and isoflurane on splanchnic microcirculation during major surgery. British Journal of Anaesthesia 1997; 78: 95–96.
6. Gatecel C, Losser MR, Payen D. The postoperative effects of halothane versus isoflurane on hepatic artery and portal vein blood flow in humans. Anesthesia & Analgesia 2003; 96: 740–745.
7. Tegeder I, Lotsch J, Geisslinger G. Pharmacokinetics of opioids in liver disease. Clinical Pharmacokinetics 1999; 37: 17–40.
8. De Wolf AM, Freeman JA, Scott VL, et al. Pharmacokinetics and pharmacodynamics of cisatracurium in patients with end-stage liver disease undergoing liver transplantation. British Journal of Anaesthesia 1996; 76: 624–628.
9. Lee AC, Reduque LL, Luban NLC, et al. Transfusion-associated hyperkalemic arrest in pediatric patients receiving massive transfusion. Transfusion 2014; 54: 244–254.
10. Perkin RM, Anas N. Pulmonary artery catheters. Pediatric Critical Care Medicine 2011; 12 (Suppl): S12–S20.
11. Carmosino MJ, Friesen RH, Doran A, et al. Perioperative complications in children with pulmonary hypertension undergoing non-cardiac surgery or cardiac catheterization. Anesthesia & Analgesia 2007; 204: 521–527.
12. Taylor CJ, Derrick G, McEwen A. Risk of cardiac catheterization under anesthesia in children with pulmonary hypertension. British Journal of Anaesthesia 2007; 98: 657–661.
13. Kost GJ. Tran NK. Continuous noninvasive hemoglobin monitoring: the standard of care and future impact. Critical Care Medicine 2011: 39: 2369–2371.
14. Bechstein WO, Neuhaus P. Bleeding problems in liver surgery and liver transplantation. Chirurgia 2000; 71: 363–368.
15. Ozier Y, Pessione F, Samain E, Courtois F. Institutional variability in transfusion practice for liver transplantation. Anesthesia & Analgesia 2003; 97: 671–679.
16. Bulkley GB. Reactive oxygen metabolites and reperfusion injury: aberrant triggering of reticuloendothelial function. Lancet 1994; 344 (8927): 934–936.
17. Kerkar N. ICU care for the transplant recipient. Post-graduate course. Presented at the International Pediatric Transplant Association 8th Congress on Pediatric Transplantation, San Francisco, March 28–31, 2015.
18. O’Meara ME, Whiteley SM. Immediate extubation of children following liver transplantation is safe and may be beneficial. Transplantation 2005; 80: 959–963.