Chapter 43 What Is the Best Treatment for Open Fractures?
A fracture is considered open if the bone or the fracture hematoma communicates with the outside environment. These injuries often occur in conjunction with high-energy trauma. It is imperative not be distracted by the potentially gross injury and initiate an Advanced Trauma Life Support protocol. Stabilization of the patient can prevent secondary injury from hypoxia, hypothermia, and reduced tissue perfusion. The treatment of open fractures is a multifactorial and longitudinal endeavor. As with most orthopaedic algorithms the evidence for each step of treatment has a differing level of supporting literature. An exhaustive discussion of each anatomic location and grade of open fracture is neither practical nor supported in the literature. Most studies group all open fractures together or concentrate on tibia fractures when assessing different treatment protocols. Tibias are among the most common location of open fractures, as well as the ones plagued with the highest rates of infection and nonunion. With this in mind most of the treatment recommendations for the tibia can be considered as worst-case scenario for other fractures regardless of their location. Preservation of blood supply is of paramount importance in the treatment of any fracture. This is what allows fracture healing and prevents infection.
OPTIONS
A careful neurological and vascular assessment should be completed and documented. A photograph of the open injury prior to dressing and splint application reduce repeated exposures of the open wound by multiple examiners leading to potential contamination, as a large number of infections are nosocomial.1 Rapid transportation to the nearest trauma center may reduce the overall rate of long term complications, especially in grade III B open fractures requiring specialty care from orthopaedic and plastic surgeons.2 Tetanus status must be established early in the course of treatment. Tetanus toxoid should be administered if the patient’s immune status is uncertain or the last booster was more than 10 years previous. The administration of human tetanus immune globulin will depend on the patient’s injury and immunization status.
EVIDENCE
Timing of Surgical Intervention
Open fractures have traditionally been considered orthopaedic emergencies, however, there is some evidence that operative treatment within six hours of injury versus treatment after six hours has no effect on ultimate infection rates.11 Definitive guidelines are not yet established for all open fractures. It is known that the location and grade of injury has a significant bearing on complication rates.12 As the severity of the fracture increases so does the infection rate. With the tibial location of the open fracture the complication rate is highest. Current evidence with regards to delayed initial treatment is Level II.
Type and Duration of Antibiotic Administration
Prophylactic antibiotics play a key role in the prevention of one of the most dreaded complications of open fractures; that of infection.3 It is well established that antibiotics reduce the risk of infection.4 Numerous studies have looked at antibiotic selection and duration. There is evidence that when infection does become established the organism is usually one that is resistant to the original antibiotic chosen.1,5
Protocols for antibiotic selection are based upon the grade of open fracture and the degree of contamination. Although the open fracture grading system has poor interobserver reliability it still provides guidelines for treatment.6 There are numerous randomized control trials studying different antibiotic protocols and their conclusions are all very similar. The use of a broad spectrum antibiotic, such as cefazolin, or the use of clindamycin or cloxacillin has been proven to reduce infection rates in grade I and grade II open fractures up to seven fold.7,8, 9 In grade III fractures, additional coverage is needed for gram-negative organisms with an aminoglycocide or fluoroquinolone.8 Gross contamination or “farm injuries” necessitate the addition of clostidial coverage and this usually means adding penicillin or metronidazole. Once daily high dose gentamicin (5-6 mg/kg) has been proven to be as effective as conventional divided dosing.10 In severe open wounds the use of an antibiotic bead pouch has been shown to reduce infection rates.20,21 Gentamicin beads are available commercially or tobramycin beads can be made by hand. Add 1.2 grams of powdered tobramycin to each package of cement. Round beads of 5 to fifteen millimeters are formed, strung on a wire, and placed in the open wound. The wound is sealed over with an adhesive, impermeable film such as Opsite or Ioban until the second debridement in 48 to 72 hours.
Irrigation Fluid during Debridement
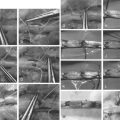
With the patient under anaesthetic the extremity is carefully exposed and a wound scrub is generally recommended to remove gross debris prior to preparation and draping of the fracture. Maintaining control of both sides of the fracture is imperative throughout the process. A tourniquet is applied but used only if absolutely necessary (level V). One of the most important steps in the optimization of outcomes is a meticulous layer-by-layer debridement of the open wound. An extensile exposure should be used taking care to minimize further soft tissue injury. Skin resection should be limited, knowing that questionable integument can be resected at the time of secondary debridement. Fat and fascia are generally expendable and poorly vascular. Muscle viability is evaluated along the lines of consistency, contractility, color, and capillary perfusion (4 C’s). Bone ends are delivered into the wound and cleaned and all non-viable bone is resected. Retained devascularized bone in the wound, even as a structural piece, can lead to a fifty percent increase in infection rates.13 Fasciotomies may be required in open fractures.
Throughout and following the surgical debridement six to twelve litres of warm isotonic irrigation should be run through the wound. The use of detergents such as castile soap as well as antibiotic solutions such as bacitracin has been studied. One large Level I prospective study concluded that neither fluid affected fracture healing or infection rates but the antibiotic solution cases had an increased rate of wound healing problems.14 Lavage fluid should be delivered by open gravity flow cystoscopy tubing or with low pressure pulsed lavage. High-pressure lavage has been shown to cause damage to bone.15 There is at least one well-designed in-vitro study showing increased effectiveness of 1% liquid soap in removing adherent bacteria from bone and preservation of osteoblast activity when applied with low-pressure lavage.16
Fracture Stabilization
Stabilization of the fracture is the next step. Depending on the grade and location of the injury different treatment methods are recommended. In general, unless a wound is highly contaminated and/or in the tibia, definitive fixation can occur after the irrigation and debridement is completed with the fixation method of choice. The use of both reamed and unreamed nails (level 1) has been proven safe in all grades of open tibia fractures.16,17, 18 Although considered quite safe and probably preferable in the upper extremity, plate fixation is generally not recommended in open tibia fractures.19 In some cases with extensive contamination and soft tissue injury an external fixator may be chosen for temporary or definitive stabilization.
Timing of Definitive Wound Closure
By convention most open wounds are dressed open or loosely closed with repeat debridements completed every 48 hours until the wound is clean. Antibiotics coverage should continue for 24 hours after definitive closure as greater than 24 hours imparts no greater protection from infection.22
A large prospective randomized study is currently underway to look at primary closure of open fracture wounds. It appears that simple, low energy grade one injuries in highly vascular areas may be safe to close primarily. At least one study has shown no difference in infection rates with wound closure at the initial debridement compared to delayed closure.5 This does not however eliminate the risk of infection with common organisms or a clostridial infection.
In the case of soft tissue loss or high-energy gunshot wounds, early emergency treatment is extremely important. In order to optimize patient outcomes rapid re-establishment of blood supply and limb stabilization is mandatory. Vascular reconstruction needs to take place in less than six hours if there is any hope of limb salvage. In some cases this means rapid transportation of a patient to an appropriate trauma center. Immediate coverage with flaps has been used with success in some centers having microvascular surgeons available. Soft tissue coverage with local tissue, wound vacuums, grafts, or flaps should be completed within 7 to 10 days to significantly reduce overall infection rates.23
Additional Techniques to Promote Bone Healing
Reconstruction of bony defects can take place as a planned bone grafting at 6 weeks post injury or using a bone transport system such as an Ilizarov fixator early on. Bone grafting prior to six weeks can lead to resorption of the graft in the inflammatory wound bed or an increased infection rate.24
At least 1 large, prospective, multi-centered trial has been completed to study the use of bone morphogenic protein in open fractures. A collagen sponge was soaked with rhBMP-2 and placed in the open fracture at the time of definitive closure. The conclusion of this randomized trial was that the technique was safe and that both wound and fracture healing were accelerated.25
Another technology that has been tested in open fractures is the use of Ultrasound to stimulate bone healing. This is controversial as one study in closed fractures revealed no difference in healing rates in tibias.26 A second study in open tibia fractures concluded accelerated fracture healing with the use of ultrasound.27
AREAS OF UNCERTAINTY
Type and Duration of Antibiotic Administration
Grade 1 and 2 fractures should be given a broad-spectrum antibiotic, such as cefazolin. An alternative is clindamycin, cloxacillin, or vancomyacin if allergies exist. In grade III fractures additional coverage is needed for gram-negative organisms with an aminoglycocide or fluoroquinolone.8 Gross contamination or “farm injuries” necessitate the addition of clostidial coverage and this usually means adding penicillin or metronidazole we administer antibiotics until 24 hours after definitive wound closure.
Timing of Closure
Ancillary techniques to obtain bone healing: Currently we do not employ any ancillary techniques such as ultrasound or bone-morphogenic proteins in the face of primary treatment of open fractures. On a rare occasion or with a particularly difficult case of non-union we may add 1 of the ancillary techniques to a standard approach (Table 43-1).
| RECOMMENDATION | LEVEL OF EVIDENCE/GRADE OF RECOMMENDATION |
|---|---|
1 Carsenti-Etesse H, Doyon F, Desplaces N, et al. Epidemiology of bacterial infection during management of open leg fractures. Eur J Clin Microbiol Infect Dis. 1999;18:315-323.
2 Naique SB, Pearse M, Nanchahal J. Management of severe open tibial fractures. The need for combined orthopaedic and plastic surgical treatment in specialist centres. J Bone Joint Surg Br. 2006;88:351-357.
3 Braun R, Enzler MA, Rittmann WW. A double-blind clinical trial of prophylactic cloxacillin in open fractures. J Orthop Trauma. 1987;1:12-17.
4 Gosselin RA, Roberts I, Gillespie WJ. Antibiotics for preventing infection in open limb fractures. Cochrane Database Syst Rev.; 1; 2004; CD003764.
5 Benson DR, Riggins RS, Lawrence RM, et al. Treatment of open fractures: A prospective study. J Trauma. 1983;23:25-30.
6 Brumback RJ, Jones AL. Interobserver agreement in classification of open fractures of the tibia. J Bone Joint Surg Am. 1994;76:1162-1166.
7 Patzakis MJ, Bains RS, Lee J, et al. Prospective, randomized, double-blind study comparing single-agent antibiotic therapy, ciprofloxacin, to combination antibiotic therapy in open fracture wounds. J Orthop Trauma. 2000;14:529-533.
8 Vasenius J, Tulikoura I, Vainionpaa S, Rokkanen P. Clindamycin versus cloxacillin in the treatment of 240 open fractures. A randomized prospective study. Ann Chir Gynaecol. 1998;87:224-228.
9 Patzakis MJ, Harvey JPJr, Ivler D. The role of antibiotics in the management of open fractures. J Bone Joint Surg Am. 1974;56:532-541.
10 Sorger JI, Kirk PG, Ruhnke CJ, et al. Once daily, high dose versus divided, low dose gentamicin for open fractures. Clin Orthop Relat Res. 1999;366:197-204.
11 Charalambous CP, Siddique I, Zenios M, et al. Early versus delayed surgical treatment of open tibial fractures: Effect on the rates of infection and need of secondary surgical procedures to promote bone union. J Injury. 2005;36:656-661.
12 Harley BJ, Beaupre LA, Jones CA. The effect of time to definitive treatment on the rate of non-union and infection in open fractures. J Orthop Trauma. 2002;16:484-490.
13 Edward CC, Simmons SC, Browner BD, et al. Severe open tibial fractures: Results treating 202 injuries with external fixation. Clin Orthop. 1988;230:98-115.
14 Anglen JO. Comparison of soap and antibiotic solutions for irrigation of lower-limb open fracture wounds. A prospective, randomized study. J Bone Joint Surg Am. 2005;87:1415-1422.
15 Bhandari M, Schemitsch EH, Adili A, et al. High and low pressure lavage of contaminated tibial fractures: An in vitro study of bacterial adherence and bone damage. J Orthop Trauma. 1999;13:526-533.
16 Bhandari M, Adili A, Schemitsch EH. The efficacy of low-pressure lavage with different irrigating solutions to remove adherent bacteria from bone. J Bone Joint Surg Am. 2001;83-A:412-419.
17 Dervin GF. Skeletal fixation of grade IIIB tibial fractures. The potential of metaanalysis. J Clin Orthop Relat Res. 1996;332:10-15.
18 Keating JF, O’Brien PJ, Blachut PA, et al. Locking intramedullary nailing with and without reaming for open fractures of the tibial shaft. A prospective, randomized study. J Bone Joint Surg Am. 1997;79:334-341.
19 Tornetta P, Bergman M, Watnik N, et al. Treatment of grade-IIIb open tibial fractures. A prospective randomised comparison of external fixation and non-reamed locked nailing. J Bone Joint Surg Br. 1994;76:13-19.
20 Bach AW, Hansen STJr. Plates versus external fixation in severe open tibial shaft fractures. A randomized trial. Clin Orthop Relat Res. 1989;241:89-94.
21 Ostermann PA, Seligson D, Henry SL. Local antibiotic therapy for severe open fractures: A review of 1085 consecutive cases. J Bone Joint Surg Br. 1995;77:93-97.
22 Moehring HD, Gravel C, Chapman MW, Olson SA. Comparison of antibiotic beads and intravenous antibiotics in open fractures. Clin Orthop Relat Res. 2000;372:254-261.
23 Dellinger EP, Caplan ES, Weaver LD, et al. Duration of preventive antibiotic administration for open extremity fractures. Arch Surg. 1988;123:333-339.
24 Godina M. Early microsurgical reconstruction of complex trauma of the extremities. Plast Reconst Surg. 1986;78:285-292.
25 Johnson KD, Bone LB, Scheinberg R. Severe open tibial fractures: A study protocol. J Orthop Trauma. 1988;2:175-180.
26 Govender S, Csimma C, Genant HK, et al. Evaluation in Surgery for Tibial Trauma Study: Recombinant human bone morphogenetic protein-2 for treatment of open tibial fractures: A prospective, controlled, randomized study of four hundred and fifty patients. J Bone Joint Surg Am. 2002;84-A:2123-2134.
27 Emami A, Petren-Mallmin M, Larsson S. No effect of low-intensity ultrasound on healing time of intramedullary fixed tibial fractures. J Orthop Trauma. 1999;13:252-257.
28 Heckman JD, Ryaby JP, McCabe J, et al. Acceleration of tibial fracture-healing by non-invasive, low-intensity pulsed ultrasound. J Bone Joint Surg Am. 1994;76:26-34.