Chapter 29 What Is the Best Treatment for Growth Plate Injuries?
A growth plate is a disc of cartilage that is organized into a physiologic pattern that, as it matures, is responsible for longitudinal growth of long bones. The cause of growth plate injuries may be acute or chronic. An injury is most commonly caused by trauma. Less frequent causes include infection, thermal injury, effects of metabolic abnormalities, tumors, or neuromuscular conditions, and there are iatrogenic causes such as exposure to irradiation or LASER.1
WHAT IS THE BEST TREATMENT OF A GROWTH PLATE INJURY CAUSED BY A FRACTURE?
Epidemiologic Studies
In a study of 2650 long-bone fractures in children younger than 16 years, 30% involved the growth plate.2 A population-based study was performed assessing 951 physeal fractures over a 10-year period in Minnesota.3 The following bones were involved in decreasing frequency: finger phalanges (37%), distal radius (18%), distal tibia (11%), distal fibula (7%), metacarpals, toe phalanges, distal humerus, distal ulna, proximal humerus, distal femur, metatarsals proximal tibia, and proximal radius fibula. In these and other studies, male individuals were affected twice as often as female individuals. Female individuals were most commonly injured at a younger age (11–12 years compared with 12–14 years in boys). When all types of growth plate fractures are considered, the rate of growth disturbance is approximately 30%. Some sites are more prone than others; however, only 2% of such fractures result in a significant functional disturbance.
How Should These Injuries Be Followed Up
For all of these fractures, it is generally agreed that they should be re-examined with radiographs in the short term to ensure reduction has been maintained, and in the longer term to ensure that growth arrest has not occurred. No evidence is available to indicate how long review should continue; most experts are of the opinion (Level V evidence) that a parallel Harris line4 at some distance from the growth plate at 6 to 12 months is a sign that normal growth has resumed.
Factors That Affect Treatment.
Pattern of the Fracture.
There have been many classification systems proposed based on the pattern of the fracture. These include the systems of Salter and Harris, Ogden, and Peterson. The most widely known is that of Salter and Harris.5 Evidence for the best treatment of each type of fracture is summarized in the following sections. In general, this evidence is not based on comparative studies but on received wisdom (Level V evidence) and case series (Level IV).
Best Treatment for a Salter–Harris Type I or II Growth Plate Fracture.
With a transverse fracture through the hypertrophic zone (Type I), the germinal layer usually is not primarily involved, although there may be some microfracture that extends into the germinal zone,6 and significant growth disturbance is uncommon, unless there is associated injury to the blood supply.5 In the more common, type II fracture, which runs through the growth plate with a triangular fragment of metaphysis (Thurston–Holland fragment), there is usually an intact periosteal hinge5 that can aid closed reduction.
In laboratory rats after a type I or II fracture, a brief growth arrest is noted. However, the growth plate appears normal after 25 days other than a thickened hypertrophic zone.7
Specific treatment depends on the site of the fractures. There are no high-level studies that compare open with closed treatment or use of fixation. The accepted wisdom is that reduction should be gentle to avoid scraping the growth plate on bone fragment or damaging the germinal layers during manipulation.1,5, 8 It is generally agreed that closed reduction and casting is successful; however, that it may be necessary to use internal fixation after open or closed reduction if it is unstable.8 In some circumstances, the periosteum may become interposed into the fracture and block satisfactory or anatomic reduction requiring exploration.9
Best Treatment for Salter–Harris Type III or IV Growth Plate Fractures.
No randomized studies have compared open with closed treatment or use of fixation. According to Bright,9 anatomic alignment of the growth plate and articular surface is important and requires anatomic reduction and internal fixation. There are case reports of nondisplaced fragments becoming displaced if fixation is not used.
No studies have compared methods of fixation. It is generally accepted that nonthreaded wires should be used in the epiphysis or metaphysis that run parallel to the growth plate.8 Alternatively, screw fixation parallel to the growth plate can be used. If stable anatomic fixation cannot be attained with transverse pins, it is also accepted that oblique nonthreaded wires across the growth plate may be used.8 There have been case-series reports (Level IV evidence) of the use of biodegradable rods, Polylactide-glycolide polymer,10 across the growth plates without disturbance of growth.
Best Treatment of Salter–Harris Type V and “VI” Fractures.
Compression or crush injuries to the growth plate (type V) are rarely diagnosed acutely. Some debate exists in the literature whether this mechanism exists. Although several reports have demonstrated that growth plate compression injuries occur, they usually result in a complete arrest (rather than partial growth arrest that is indicated in the Salter–Harris article).1 The average time until diagnosis of this type of injury is 17 months.
Although not included in the original Salter–Harris classification, a type “VI” fracture is included in Rang’s book.11 He reports that Kessel suggested an additional type of growth plate injury, that is, an injury to the periosteum or perichondrial ring resulting in a bony bridge. It is suggested that this may lead to angular deformity from a bone bridge. Few cases series have reported this injury type.
Site of Growth Plate Injury.
Acetabular Triradiate Cartilage Fractures.
Injury to the acetabular triradiate growth plate cartilage is rare, but it may be associated with progressive acetabular dysplasia and subluxation of the hip. Bucholz and colleagues12 found nine patients with triradiate growth plate injury (Level IV evidence). Shearing (SH type I or II) injury seems to have a favorable prognosis. However, a crushing SH type V growth plate injury has a poor prognosis, with premature closure. Prognosis is dependent on the age of the patient at the time of injury and on the extent of chondro-osseous disruption.
Approximately 50% of distal femur growth plate fractures are associated with growth disturbance, even the type I or II fractures (Level IV evidence, case series).13,14
Expert advice is that closed reduction should also be attempted for all minimally to moderately displaced Salter–Harris type I and II fractures.15 However, a study of 10 distal femoral physeal fractures found that 7 displaced, and the authors suggest that internal fixation should be used.16 Fractures with greater displacement, especially those with a hyperextension pattern, are associated with an increased risk for redisplacement; therefore, percutaneous fixation is recommended.17
Salter–Harris type II fractures can be stabilized by fixation across the Thurston Holland metaphyseal spike if it is large. Percutaneous screws are preferred for fixation if they can be inserted without crossing the physis. If metaphyseal stability cannot be obtained, Salter–Harris type I and II fractures can be fixed with one or two smooth Steinmann pins from the epiphysis to the metaphysis. If the pins are left outside of the skin, they can cause irritation and may even lead to infection septic arthritis.15 Salter–Harris type III and IV fractures can be fixed with intraepiphyseal screws.14
Proximal Tibia Fractures.
Fractures of the proximal tibia growth plate are among the most uncommon but have the greatest rate of serious complications. Displacement of the fracture can result in significant problems related to popliteal artery disruption in 5% to 7% of cases18,19 or common peroneal nerve injury, and these should be looked for. In these retrospective series (Level IV evidence), it is also noted that there may be a growth arrest that does not correlate well with fracture pattern, and close follow-up should be made to detect angular or leg-length deformity.
Expert advice is that fractures that can be reduced by closed methods can usually be held in alignment with a long leg cast. If the fracture is displaced, the cast should be bivalved and the patient should be observed overnight for vascular complications. The circulation should be carefully assessed, and an intraoperative arteriogram should be made when the vascular supply is compromised, and compartment syndrome should be ruled out clinically.15
Salter–Harris type III pattern of injury is rare in the proximal part of the tibia (except as a pattern of tibial tubercle avulsion), which has been attributed to the shape of the epiphysis. Unstable fractures of any pattern and all displaced type IV fractures should be reduced and stabilized with internal fixation such as smooth Steinmann pins.
Distal Tibia Fractures.
Fractures of the distal end of the tibia in children often involve the growth plate. They may result in partial growth arrest, angulation, leg-length difference, or joint incongruity.20
Salter–Harris I and II fractures can usually be treated with closed reduction. A series of 56 type II fractures treated in casts resulted in no deformity or premature physeal closure21 (Level IV evidence). Acceptable alignment of displaced fractures in children with at least 2 years of growth remaining consists of no more than 15 degrees of plantar tilt, 10 degrees of valgus, and no varus. In children with less than 2 years of growth remaining, the amount of acceptable angulation is reduced to 5 degrees in all planes (Level V evidence, expert opinion).22
General agreement exists that type III and IV fractures require surgical intervention.15,23 In a retrospective series, it was concluded that major deformity can be avoided with aggressive follow-up and early corrective treatment.20 Open or arthroscopic visualization of the joint surface has been recommended to confirm reduction, and stabilization with 3.5- or 4.0-mm cannulated screws assessing the screw placement carefully in two planes.15
Treatment recommendation for Tillaux fractures (SH III of the anterolateral portion of the distal tibial epiphysis) is directed to reducing and holding the fragment with less than 2 mm displacement, and this is best judged with computed tomography.15 Closed reduction, open reduction, and a percutaneous method have been described.24
Treatment recommendations for Triplane fractures (complex Salter–Harris type IV fractures in three planes) include radiographic and computed tomographic evaluation initially. An articular step-off of more than 2 mm or a fracture gap of more than 2 to 4 mm is an indication for open reduction.15 This is based on a study that showed that more than 2 mm articular displacement leads to poorer long-term results according to a follow-up study by Ertl et al.25 An open exploration and fixation is usually necessary to achieve reduction.15
Distal Radius and Ulna.
The growth plate of the distal radius is the most frequently injured, usually with a SH type I or II pattern. Three quarters of the growth of the forearm occurs at the distal growth plates, with good potential for remodeling, but also potential for a significant mismatch if one of these paired bones has an arrest. Significant growth disturbance occurs in 7% of distal radius fractures.26 This is important as a study of 30 patients who had surgical management of distal radial growth arrest that was found to improve pain and range of motion in symptomatic patients and prevent symptoms in asymptomatic patients.27
BEST TREATMENT OF A CHRONIC GROWTH PLATE INJURY
In addition to the acute physeal injuries sustained through sports,28 there is an increasing body of evidence demonstrating that growth plate injuries can occur by repetitive physical loading required in sports. A recent systematic review found that most reports were case reports or case series.29
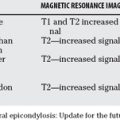
This injury appears to be related to mineralization of the hypertrophic zone because of altered metaphyseal perfusion.30 The hypertrophic zone continues to get wider, as shown experimentally by Jaramillo et al31 in rabbits with similar magnetic resonance imaging findings seen in competitive gymnasts. This is usually temporary,30 but it may lead to permanent changes, with either a partial or complete growth plate disturbance.
This is best known in conditions such as “little league shoulder”; there are many reports of stress changes in the proximal humeral physis of baseball pitchers’ throwing arms.29 Although this tends to improve with rest, there is one report of premature physeal closure.32 Similar reports of physeal widening in association with other sports, and even piano playing, in the upper and lower limbs of growing athletes can be found in the literature.29
BEST TREATMENT FOR AN INJURED GROWTH PLATE
An injured or disrupted growth plate may lead to premature fusion of part or all of the growth plate, with a bone “bar” across the area that should be made of the specialized arrangement of growth cartilage. There is consequent tethering that may lead to partial (angular) or complete (longitudinal) growth disturbance at the growth plate.33 This bar may be visible on a conventional radiograph, but multiplanar imaging such as computed tomography or magnetic resonance can be helpful in localizing the lesion.
Different forms of treatment have been described for growth plate arrest. The best treatment depends on the following factors: the location of the growth plate; the amount of growth remaining at that growth plate; whether complete arrest has been maintained; or if partial, the proportion of the growth plate that is involved and the circumstances of the child.1 No high-level evidence has compared outcomes of different treatments for these relatively rare events, and management recommendations are based on Level V evidence (expert opinion).
For complete arrest, treatment is directed to the management of length inequality. Management options include no intervention, compensatory orthoses (shoe lift), epiphyseodesis or shortening of the contralateral or companion bone, ipsilateral bone lengthening, or a combination.1
For partial growth arrest, treatment is directed to managing the length inequality and angulation. Treatment options include a combination of the following: no intervention; compensatory orthoses (shoe lift); epiphyseodesis of the remaining bone, or contralateral or companion bone; correction of the angulation by acute (osteotomy) or gradual correction (distraction osteogenesis); excision of the bar and interposition of an inert material; and distraction of the growth plate and bar (in children nearing maturity).1
Resection of a Bone Bridge
To prevent arrest of growth after physeal injury, investigators have performed bone bar resection and used various interposition materials: fat,33,34 muscle,35 polymeric silicone,36–39 bone wax,40 and bone cement.41 These studies are Level IV evidence (case series); regarding the results of treatment, no study shows the superiority of one material over the others.
Experts agree that resection is indicated if less than 30% to 50% of growth plate is involved1 (Level of Evidence V). Younger children tend to have a better prognosis. Less than 2 years of remaining growth is a relative contraindication for bone bridge resection. It has also been noted that central bars are more amenable to resection than peripheral, which is probably related to the adjacent periosteal stripping in peripheral lesions. Ischemic or septic-related bone bars have a poorer prognosis (Level of Evidence V).
In one study, 28 skeletally immature patients underwent 29 primary physeal bridge resections. Of 22 resections followed for 2 years, there were 11 excellent, 5 good, 2 fair, and 4 poor results. Overall mean growth was 83%, with 98% in the excellent group and 96% in the good group. The authors conclude that physeal bridge resection is an effective method of treating partial physeal growth arrest (Level IV evidence). Results with fat compare favorably with results of other interposition materials without the disadvantages of local reaction and implant removal.42
Physeal Distraction
Hemichondrodiastasis, closed gradual distraction of the growth plate, to correct angular deformity has been described.43,44 This technique in a group of 35 patients worked best in post-traumatic deformities when the bony bridge occupied less than 30% of the plate. It was used toward the end of growth (or earlier in the case of progressive deformity of more than 20 degrees).
Recent experimental studies have explored the use of autogenous chondrocytes to fill the defect.45,46 However there are still some problems to overcome. Principally, it is difficult to find suitable donor sites other than apophyses, and apophyseal cartilage may lack the growth potential of epiphyseal cartilage. These experimental studies are preclinical and do not receive level of evidence grades.
SUMMARY
The evidence for the best treatment of growth plate injuries is based mainly on epidemiologic studies, retrospective reviews, animal model experiments, and expert opinion. Table 29-1 provides a summary of recommendations for the treatment of growth plate injuries.
| STATEMENT | LEVEL OF EVIDENCE/GRADE OF RECOMMENDATION | REFERENCES |
|---|---|---|
| Most Salter–Harris type I and II fractures may be adequately treated by closed manipulation and stabilization in a cast. | IV | 21 |
| Open reduction and fixation is better than closed manipulation for most Salter–Harris type III and IV fractures. | IV | 15, 20, 25 |
| Salter–Harris type V fractures exist. | V | 5 |
| Chronic repetitive injury can result in physeal arrest that can be prevented by rest. | IV | 29 |
| Growth plate fractures with higher Salter–Harris grades have a greater risk for partial or complete growth arrest. | IV, V | 1, 5 |
| Approximately 50% of distal femur growth plate fractures are associated with growth disturbance, even the type I or II fractures. | IV | 13, 14 |
| Physeal bridge resection with interposition material is an effective way of treating partial growth arrest. | IV | 9, 33–42 |
1 Peterson HA. Physeal injuries and growth arrest. In: Beaty JH, Kasser JR, editors. Rockwood and Wilkins’ Fractures in Children. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2001:91-138.
2 Mann DC, Rajmaira S. Distribution of physeal and nonphyseal fractures in 2,650 long-bone fractures in children aged 0-16 years. J Pediatr Orthop. 1990;10:713-716.
3 Peterson HA, Madhok R, Benson JT, et al. Physeal fractures part 1 epidemiology in Olmsted county Minnesota, 1979-88. J Pediatr Orthop. 1994;41:423-430.
4 Harris HA. Lines of arrested growth in the long bones in childhood: The correlation of histological and radiographic appearance in clinical and experimental conditions. Br J Radiol. 1931;4:561-588.
5 Salter RB, Harris WR. Injuries involving the epiphyseal plate. J Bone Joint Surg Am. 1963;45-A:587-622.
6 Ogden JA. Injury to the growth mechanism of the immature skeleton. Skeletal Radiol. 1981;6:237-253.
7 Gomes LS, Valpon JB, Gonclaves RP. Traumatic separation of epiphyses; an experimental study in rats. Clin Orthop Relat Res.; 236; 1988; 286-295.
8 Canale ST. Physeal injuries. In: Green NE, Swiontowski MF, editors. Skeletal Trauma in Children. 2nd ed. Philadelphia: WB Saunders Company; 1997:17-58.
9 Bright RW. Physeal injuries. Fractures: Fractures in Children, 3rd ed., Philadelphia: Lippincott-Raven; 1991:87-186.
10 Makela EA, Bostman O, Kekomaki M, et al. Biodegradable fixation of distal humeral fractures. Clin Orthop Relat Res. 1992;283:237-243.
11 Rang M, editor. The Growth Plate and Its Disorders. Edinburgh and London: E&S Livingstone, 1969.
12 Bucholz RW, Ezaki M, Ogden JA. Injury to the acetabular triradiate physeal cartilage. J Bone Joint Surg Am. 1982;64:600-609.
13 Eid AM, Hafez MA. Traumatic injury of the distal femoral physis. Retrospective study on 150 cases. Injury. 2002;33:251-255.
14 Riseborough EJ, Barrett IR, Shapiro F. Growth disturbances following distal femoral physeal fracture separations. J Bone Joint Surg Am. 1983;65:885-893.
15 Flynn J, et al. The operative management of pediatric fractures of the lower extremity. J Bone Joint Surg Am. 2002;84:2288-2300.
16 Graham JM, Gross RH. Distal femoral physeal problem fractures. Clin Orthop Relat Res.; 255; 1990; 51-53.
17 Thomson JD, Stricker SJ, Williams MM. Fractures of the distal femoral epiphyseal plate. J Pediatr Orthop. 1995;15:474-478.
18 Shelton WR, Canale ST. Fractures of the tibia through the proximal tibial epiphyseal cartilage. J Bone Joint Surg Am. 1979;61:167-173.
19 Burkhart SS, Peterson HA. Fractures of the proximal tibial epiphysis. J Bone Joint Surg Am. 1979;61:996-1002.
20 Lalonde K-A, Letts M. Traumatic growth arrest of the distal tibia: a clinical and radiographic review. Can J Surg. 2004;48:143-147.
21 Dugan G, Herndon WA, McGuire R. Distal tibial injuries in children: a different treatment concept. J Orthop Trauma. 1987;1:63-67.
22 Cummings RJ. Distal tibial and fibular fractures. In: Rockwood CAJr, Wilkins KE, Beaty JH, editors. Fractures in Children. 4th ed. Philadelphia: Lippincott-Raven; 1996:1377-1428.
23 deSanctis N, Della Corte S, Pempinello C. Distal tibial and fibular epiphyseal fractures in children: Prognostic criteria and long term results in 158 patients. J Pediatr Orthop B. 2000;9:40-44.
24 Schlesinger L, Wedge JH. Percutaneous reduction and fixation of displaced juvenile Tillaux fractures: A new surgical technique. J Pediatr Orthop. 1993;13:389-391.
25 Ertl JP, Barrack RL, Alexander AH, VanBuecken K. Triplane fracture of the distal tibial epiphysis. Long-term follow-up. J Bone Joint Surg Am. 1988;70:967-976.
26 Lee BS, Esterhai JLJr, Das M. Fracture of the distal radial epiphysis. Characteristics and surgical treatment of premature, post-traumatic epiphyseal closure. Clin Orthop.; 185; 1984; 90-96.
27 Waters PM, Bae DS, Montgomery KD. Surgical management of post traumatic distal radial growth arrest in adolescents. J Pediatr Orthop. 2002;22:717-724.
28 Krueger-Franke M, Siebert CH, Pfoerringer W. Sports related epiphyseal injuries of the lower extremity. An epidemiological study. J Sports Med Phys Fitness. 1992;32:106-111.
29 Caine D, DiFiori J, Maffulli N. Physeal injuries in children’s and youth sports: Reason for concern? Br J Sports Med. 2006;40:749-760.
30 Ogden JA. Skeletal Injury in the Child. New York: Springer-Verlag, 2000.
31 Jaramillo D, Laor T, Zaleske DJ. Indirect trauma to the growth plate. Radiology. 1993;187:171-178.
32 Carson WG, Gasser SI. Little leaguer’s shoulder: A report of 23 cases. Am J Sports Med. 1998;26:575-580.
33 Langenskiöld A. The possibilities of eliminating premature partial closure of an epiphyseal plate caused by trauma or disease. Acta Orthop Scand. 1967;38:267-279.
34 Österman K. Operative elimination of partial premature epiphyseal closure. An experimental study. Acta Orthop Scand Suppl.; 147; 1972; 3-79.
35 Martiana K, Low CK, Tan SK, Pang MWY. Comparison of various interpositional materials in the prevention of transphyseal bone bridge formation. Clin Orthop. 1996;325:218-224.
36 Campbell CJ, Grisolia A, Zanconato G. The effects produced in the cartilaginous epiphyseal plate of immature dogs by experimental surgical trauma. J Bone Joint Surg Am. 1959;41:1221-1242.
37 Bright RW. Operative correction of partial epiphyseal plate closure by osseous bridge resection and silicone rubber implant. An experimental study in dogs. J Bone Joint Surg Am. 1974;56:655-664.
38 Macksoud WS, Bright R. Bar resection and silastic interposition in distal radial physeal arrest. Orthop Trans. 1989;13:1-2.
39 Lee EH, Gao GX, Bose K. Management of partial growth arrest: Physis, fat, or silastic? J Pediatr Orthop. 1993;13:368-372.
40 Broughton NS, Dickens DRV, Cole WG, Menelaus MB. Epiphysiolysis for partial growth plate arrest. J Bone joint Surg Br. 1989;71:13-16.
41 Klassen RA, Peterson MA. Excision of physeal bars: The Mayo Clinic experience 1968–1978. Orthop Trans. 1982;2:65.
42 Williamson RV, Staheli LT. Partial physeal growth arrest: Treatment by bridge resection and fat interposition. J Pediatr Orthop. 1990;10:769-776.
43 Aldegheri R, Trivella G, Lavini F. Epiphyseal distraction hemichondrodisatasis. Clin Orthop Relat Res.; 241; 1989; 128-136.
44 Canadell J, de Pablos J. Correction of angular deformities by physeal distraction. Clin Orthop Relat Res. 1992:98-105.
45 Olin A, Creasman C, Shapiro F. Free physeal transplantation in the rabbit. J Bone Joint Surg Am. 1984;66:7-20.
46 Lee EH, Chen F, Chan J, Bose K. Treatment of growth arrest by transfer of cultured chondrocytes into physeal defects. J Pediatr Orthop. 1998;18:155-160.