[level-membership-for-basic-science-category]
Chapter 2 Topics in drug therapy
Practical prescribing
The case histories are all real. The data given in the text and figures come from a study commissioned by the General Medical Council.1
Prescribing
Getting it right
Good prescribing starts with taking a good history:
• Does your patient have other medical conditions – some may be worsened by treatment you would normally give for their presenting complaint.
• What drugs is your patient taking now? What are they for? Are they all still needed? Could they be causing the symptoms or signs that have brought the patient to you? Could they interact with whatever you might think of prescribing?
• What drugs has your patient taken in the past? Why were they stopped? Did they cause side-effects?
• Is the patient allergic to any drugs?
• Are they taking any non-prescription (over-the-counter) drugs? If so, could they interact with whatever you might prescribe (for example, St John’s wort is an enzyme-inducer)?
• Making a diagnosis – or at least having a range of possibilities. Know what it is you are wishing to achieve and the evidence for the likely efficacy of the drug treatment you wish to give.
• Knowing your patient’s kidney and liver function – most drugs are eliminated by these organs; and some drugs can damage them.
• Getting the dose right. For many drugs you will not know the dose, so do not pretend you do. Never, ever guess. Never be afraid to ask. Never be too busy to look up a dose – better to check now than make a trip to the Coroner’s Court later.
• Explaining to your patient why you think this treatment will work, the likelihood of it working, the more common side-effects and what your plans are if it does not work.
• Being alert to the development of adverse drug reactions. If a patient develops new symptoms after starting a drug, it is probably the drug. If the adverse effect is in a fairly new drug – or is not already well known – you should report the event to the national body responsible for monitoring and recording adverse drug reactions.
• Being very clear about what it is you are prescribing.
• If using a hand-written prescription, write clearly.
• If working in a different hospital, remember that the prescription chart may not be the same as where you have just been.
• If using electronic prescribing, beware drop-down menus and drugs with similar looking names, e.g. carbimazole and carbamazepine.
Examples of when things went wrong
Forgetting that a newly prescribed drug can interact with long-term drug treatment
A 64-year-old man had been taking warfarin for many years. He developed a chest infection and an out of hours doctor prescribed amoxicillin. Later that week he was admitted with a large, painful right knee haemarthrosis and an INR > 10 (see p. 489). New drugs may interact with those the patient has been taking for a long time!
Why do mistakes happen?
There are also factors specific to the medical environment, including:
• Not familiar with the drug chart (usually on moving to a new hospital).
• Unfamiliar patient – and not taking the time to become familiar with the full medical and drug history.
• Arithmetical errors in calculating dose.
• Omitting drugs for a newly admitted patient because of inadequate information.
When lack of knowledge does play a part, it is often the flawed application of knowledge in that particular patient – i.e. the right drug for the presenting condition, but the wrong drug for that patient because of coexisting medical or drug factors.
The General Medical Council expects that, by the time they graduate, medical students will be able to:2
• Prescribe drugs safely, effectively and economically.
• Establish an accurate drug history, covering both prescribed and other medication.
• Plan appropriate drug therapy for common indications, including pain and distress.
• Provide a safe and legal prescription.
• Calculate appropriate drug doses and record the outcome accurately.
• Provide patients with appropriate information about their medicines.
• Access reliable information about medicines.
• Detect and report adverse drug reactions.
• Demonstrate awareness that many patients use complementary and alternative therapies, and awareness of the existence and range of these therapies, why patients use them, and how this might affect other types of treatment that patients are receiving.
The therapeutic situation
Some background
Remarkably, this system persisted among ‘learned and rational’ (i.e. university-trained) physicians until it was challenged in the 17th century. Thomas Sydenham3 (1624–1689) showed that during epidemics, many people could suffer the same disease, and different epidemics had distinct characteristics. Later, Giovanni Morgagni (1682–1771), by correlating clinical and autopsy findings, demonstrated that diseases related to particular organs. Now the study of disease, rather than the patient, became the centre of attention. Yet it was only in the 19th century that medicine developed as a science, when the microscope revealed the cell as the basic construction unit of the body and specific entities of pathology became recognisable, most notably in the case of infection with microorganisms (‘germ theory’).
Throw out opium …; throw out a few specifics …; throw out wine, which is a food, and the vapours which produce the miracle of anaesthesia, and I firmly believe that if the whole materia medica, as now used, could be sunk to the bottom of the sea, it would be all the better for mankind, – and all the worse for the fishes…4
Treating patients with drugs
A book can provide knowledge and contribute to the formation of judgement, but it can do little to impart skill and wisdom, which are the products of example of teachers and colleagues, of experience and of innate and acquired capacities. But: ‘It is evident that patients are not treated in a vacuum and that they respond to a variety of subtle forces around them in addition to the specific therapeutic agent.’5
When a patient receives a drug, the response can be the result of numerous factors:
• The pharmacodynamic effect of the drug and interactions with any other drugs the patient may be taking.
• The pharmacokinetics of the drug and its modification in the individual by genetic influences, disease, other drugs.
• The act of medication, including the route of administration and the presence or absence of the doctor.
• What the doctor has told the patient.
• The patient’s past experience of doctors.
• The patient’s estimate of what has been received and of what ought to happen as a result.
• The social environment, e.g. whether it is supportive or dispiriting.
Drugs can do harm
Efficacy and safety do not lie solely in the molecular structure of the drug. Doctors must choose which drugs to use and must apply them correctly in relation not only to their properties, but also to those of the patients and their disease. Then patients must use the prescribed medicine correctly (see Compliance p. 21).
Uses of drugs/medicines
Prevention
1. Should I interfere with the patient at all?
2. If so, what alteration in the patient’s condition do I hope to achieve?
3. Which drug is most likely to bring this about?
4. How can I administer the drug to attain the right concentration in the right place at the right time and for the right duration?
5. How will I know when I have achieved the objective?
6. What other effects might the drug produce, and are these harmful?
7. How will I decide to stop the drug?
8. Does the likelihood of benefit, and its importance, outweigh the likelihood of damage, and its importance, i.e. the benefit versus risk, or efficacy against safety?
Physician-induced (iatrogenic) disease
It is a salutary thought that each year medical errors kill an estimated 44 000–98 000 Americans (more than die in motor vehicle accidents) and injure 1 000 000.7 Among inpatients in the USA and Australia, about half of the injuries caused by medical mismanagement result from surgery, but therapeutic mishaps and diagnostic errors are the next most common. In one survey of adverse drug events, 1% were fatal, 12% life-threatening, 30% serious and 57% significant.8 About half of the life-threatening and serious events were preventable. Errors of prescribing account for one-half and those of administering drugs for one-quarter of these. Inevitably, a proportion of lapses result in litigation, and in the UK 20–25% of complaints received by the medical defence organisations about general practitioners follow medication errors.
The most shameful act in therapeutics, apart from actually killing a patient, is to injure a patient who is but little disabled or who is suffering from a self-limiting disorder. Such iatrogenic disease,9 induced by misguided treatment, is far from rare.
In 1917 the famous pharmacologist Sollmann felt able to write:
Pharmacology comprises some broad conceptions and generalisations, and some detailed conclusions, of such great and practical importance that every student and practitioner should be absolutely familiar with them. It comprises also a large mass of minute details, which would constitute too great a tax on human memory, but which cannot safely be neglected.10
Benefits and risks of medicines
Unavoidable risks
Consider, for the sake of argument, the features that a completely risk-free drug would exhibit:
• The physician would know exactly what action is required and use the drug correctly.
• The drug would deliver its desired action and nothing else, either by true biological selectivity or by selective targeted delivery.
• The drug would achieve exactly the right amount of action – neither too little, nor too much.
These criteria may be completely fulfilled, for example in a streptococcal infection sensitive to penicillin in patients whose genetic constitution does not render them liable to an allergic reaction to penicillin.
Some reasons why drugs fail to meet the criteria of being risk-free include the following:
• Drugs may be insufficiently selective. As the concentration rises, a drug that acts at only one site at low concentrations begins to affect other target sites (receptors, enzymes) and recruit new (unwanted) actions; or a disease process (cancer) is so close to normal cellular mechanisms that perfectly selective cell kill is impossible.
• Drugs may be highly selective for one pathway but the mechanism affected has widespread functions and interference with it cannot be limited to one site only, e.g. atenolol on the β-adrenoceptor, aspirin on cyclo-oxygenase.
• Prolonged modification of cellular mechanisms can lead to permanent change in structure and function, e.g. carcinogenicity.
• Insufficient knowledge of disease processes (some cardiac arrhythmias) and of drug action can lead to interventions that, although undertaken with the best intentions, are harmful.
• Patients are genetically heterogeneous to a high degree and may have unpredicted responses to drugs.
• Dosage adjustment according to need is often unavoidably imprecise, e.g. in depression.
Reduction of risk
Strategies that can limit risk include those directed at achieving:
Two broad categories of risk
1. First are those that we accept by deliberate choice. We do so even if we do not exactly know their magnitude, or we know but wish they were smaller, or, especially when the likelihood of harm is sufficiently remote though the consequences may be grave, we do not even think about the matter. Such risks include transport and sports, both of which are inescapably subject to potent physical laws such as gravity and momentum, and surgery to rectify disorders that we could tolerate or treat in other ways, as with much cosmetic surgery.
2. Second are those risks that cannot be significantly altered by individual action. We experience risks imposed by food additives (preservatives, colouring), air pollution and some environmental radioactivity. But there are also risks imposed by nature, such as skin cancer due to excess ultraviolet radiation in sunny climes, as well as some radioactivity.
It seems an obvious course to avoid unnecessary risks, but there is disagreement on what risks are truly unnecessary and, on looking closely at the matter, it is plain that many people habitually take risks in their daily and recreational life that it would be a misuse of words to describe as necessary. Furthermore, some risks, although known to exist, are, in practice, ignored other than by conforming to ordinary prudent conduct. These risks are negligible in the sense that they do not influence behaviour, i.e. they are neglected.12
Elements of risk
There is general agreement that drugs prescribed for disease are themselves the cause of a significant amount of disease (adverse reactions), of death, of permanent disability, of recoverable illness and of minor inconvenience. In one major UK study the prevalence of adverse drug reactions as a cause of admission to hospital was 6.5% (see Chapter 9 for other examples).
Three major grades of risk
Risks are among the facts of life. In whatever we do and in whatever we refrain from doing, we are accepting risk. Some risks are obvious, some are unsuspected and some we conceal from ourselves. But risks are universally accepted, whether willingly or unwillingly, whether consciously or not.13
Whenever a drug is taken a risk is taken
In some chronic diseases that ultimately necessitate suppressive drugs, the patient may not experience benefit in the early stages. Patients with early Parkinson’s disease may experience little inconvenience or hazard from the condition, and premature exposure to drugs can exact such a price in unwanted effects that they prefer the untreated state. What patients will tolerate depends on their personality, their attitude to disease, their occupation, mode of life and relationship with their doctor (see Compliance, p. 21).
Public view of drugs and prescribers
There are obvious areas where some remedial action is possible:
• Improvement of prescribing by doctors, including better communication with patients, i.e. doctors must learn to feel that introduction of foreign chemicals into their patients’ bodies is a serious matter, which many or most do not seem to feel at present.14
• Introduction of no-fault compensation schemes for serious drug injury (some countries already have these).
• Informed public discussion of the issues between the medical profession, industrial drug developers, politicians and other ‘opinion-formers’ in society, and patients (the public).
• Restraint in promotion by the pharmaceutical industry including self-control by both industry and doctors in their necessarily close relationship, which the public is inclined to regard as a conspiracy, especially when the gifts and payments made to doctors get into the news. (This is much less prevalent than it was in the 1990s.)
If restraint by both parties is not forthcoming, and it may not be, then both doctor and industry can expect even more control to be exercised over them by politicians responding to public demand. If doctors do not want their prescribing to be restricted, they should prescribe better.
Criticisms of modern drugs
Two examples of inappropriate measurements will suffice:
1. In the case of many infections it is not disputed that environmental changes have had a greater beneficial effect on health than the subsequently introduced antimicrobials. But this does not mean that environmental improvements alone are sufficient in the fight against infections. When comparisons of illnesses in the pre- and post-antimicrobial eras are made, like is not compared with like. Environmental changes achieved their results when mortality from infections was high and antimicrobials were not available; antimicrobials were introduced later against a background of low mortality as well as of environmental change; decades separate the two parts of the comparison, and observers, diagnostic criteria and data recording changed during this long period. It is evident that determining the value of antimicrobials is not simply a matter of looking at mortality rates.
2. About 1% of the UK population has diabetes mellitus, a figure which is increasing rapidly, and about 1% of death certificates mention diabetes. This is no surprise because all must die and insulin is no cure15 for this lifelong disease. A standard medical textbook of 1907 stated that juvenile-onset ‘diabetes is in all cases a grave disease, and the subjects are regarded by all assurance companies as uninsurable lives: life seems to hang by a thread, a thread often cut by a very trifling accident’. Most, if not all, life insurance companies now accept young people with diabetes with no or only modest financial penalty, the premium of a person 5–10 years older. Before insulin replacement therapy was available few survived beyond 3 years16 after diagnosis; they died for lack of insulin. It is unjustified to assert that a treatment is worthless just because its mention on death certificates (whether as a prime or as a contributory cause) has not declined. The relevant criteria for juvenile-onset diabetes are change in the age at which the subjects die and the quality of life between diagnosis and death, and both of these have changed enormously.
Drug-induced injury17 (see also Ch. 9)
Negligence and strict and no-fault liability
All civilised legal systems provide for compensation to be paid to a person injured as a result of using a product of any kind that is defective due to negligence (fault: failure to exercise reasonable care).18 But there is a growing opinion that special compensation for serious personal injury, beyond the modest sums that general social security systems provide, should be automatic and not dependent on fault and proof of fault of the producer, i.e. there should be ‘liability irrespective of fault’, ‘no-fault liability’ or ‘strict liability’.19 After all, victims need assistance (compensation) regardless of the cause of injury and whether or not the producer and, in the case of drugs, the prescriber deserves censure. The question why a person who has suffered injury due to the biological accident of disease should have to depend on social security payments while an identical injury due to a drug (in the absence of fault) should attract special added compensation receives no persuasive answer except that this is what society seems to want.
Many countries are now revising their laws on liability for personal injury due to manufactured products and are legislating Consumer Protection Acts (Statutes) which include medicines, for ‘drugs represent the class of product in respect of which there has been the greatest pressure for surer compensation in cases of injury’.20
Issues that are central to the debate include:
• Capacity to cause harm is inherent in drugs in a way that sets them apart from other manufactured products; and harm often occurs in the absence of fault.
• Safety, i.e. the degree of safety that a person is entitled to expect, and adverse effects that should be accepted without complaint, must often be a matter of opinion and will vary with the disease being treated, e.g. cancer or insomnia.
• Causation, i.e. proof that the drug in fact caused the injury, is often impossible, particularly where it increases the incidence of a disease that occurs naturally.
• Contributory negligence. Should compensation be reduced in smokers and drinkers where there is evidence that these pleasure drugs increase liability to adverse reactions to therapeutic drugs?
• The concept of defect, i.e. whether the drug or the prescriber or indeed the patient can be said to be ‘defective’ so as to attract liability, is a highly complex matter and indeed is a curious concept as applied to medicine.
Nowhere has a scheme that meets all the major difficulties yet been implemented. This is not because there has been too little thought, it is because the subject is so difficult. Nevertheless, no-fault schemes operate in New Zealand, Scandinavia and France.21 The following principles might form the basis of a workable compensation scheme for injury due to drugs:
• New unlicensed drugs undergoing clinical trial in small numbers of subjects (healthy or patient volunteers): the developer should be strictly liable for all adverse effects.
• New unlicensed drugs undergoing extensive trials in patients who may reasonably expect benefit: the producer should be strictly liable for any serious effect.
• New drugs after licensing by an official body: the manufacturer and the community should share liability for serious injury, as new drugs provide general benefit. An option might be to institute a defined period of formal prospective drug surveillance monitoring, in which both doctors and patients agree to participate.
• Standard drugs in day-to-day therapeutics: there should be a no-fault scheme, operated by or with the assent of government that has authority, through tribunals, to decide cases quickly and to make awards. This body would have authority to reimburse itself from others – manufacturer, supplier, prescriber – wherever that was appropriate. An award must not have to wait on the outcome of prolonged, vexatious, adversarial, expensive court proceedings. Patients would be compensated where:
Complementary, alternative and traditional medicine
Practitioners of complementary and alternative medicine (CAM)23 are severely critical of modern drugs, and use practices according to their own special beliefs. It is appropriate, therefore, to discuss such medical systems here.
The term ‘complementary and alternative medicine’ covers a broad range of heterogeneous systems of therapy (from acupuncture to herbalism to yoga), and diagnosis (from bioresonance to pulse and tongue diagnosis). The present discussion relates largely to CAM but recognises that traditional or indigenous medicinal therapeutics has developed since before history in all societies. This comprises a mass of practices varying from the worthless to highly effective remedies, such as digitalis (England), quinine (South America), reserpine (India), atropine (various countries). It is the task of science to find the gems and to discard the dross,24 and at the same time to leave intact socially valuable supportive aspects of traditional medicine.
There is no doubt that the domain of CAM has grown in popularity in recent years; a survey estimated that about 20% of the UK population had consulted a CAM practitioner in the previous year.25 In Germany, the figure exceeds 60%, with $2.06 billion in over-the-counter sales in 2003.26 Usage rises sharply among those with chronic, relapsing conditions such as cancer, multiple sclerosis, human immunodeficiency virus (HIV) infection, psoriasis and rheumatological diseases. It is difficult to resist the conclusion that when scientific medicine neither guarantees happiness nor wholly eliminates the disabilities of degenerative diseases in long-lived populations, and when drugs used in modern medicine cause serious harm, public disappointment naturally leads to a revival of interest in alternatives that alluringly promise efficacy with complete safety. These range from a revival of traditional medicine to adoption of the more modern cults.27
Features common to medical cults are: absence of scientific thinking, naive acceptance of hypotheses, uncritical acceptance of causation, e.g. reliance on anecdote or opinion (as opposed to evidence), assumption that if recovery follows treatment it is due to the treatment, and close attention to the patient’s personal feelings. Lack of understanding of how therapeutic effects may be measured is also a prominent feature. An extensive analysis of recommendations of CAM therapies for specific medical conditions from seven textbook sources revealed numerous treatments recommended for the same condition – for example: addictions (120 treatments recommended), arthritis (121), asthma (119) and cancer (133) – but there was lack of agreement between these authors as to the preferred therapies for specified conditions.28 The question must arise that if numerous and heterogeneous treatments are effective for the same condition, could they not have some common feature, such as the ability of the practitioner to inspire confidence in the patient?
Some common false beliefs of CAM practitioners are that synthetic modern drugs are toxic, but products obtained in nature are not.29 Scientific medicine is held to accept evidence that remedies are effective only where the mechanism is understood, that it depends on adherence to rigid and unalterable dogmas, and recognises no form of evaluation other than the strict randomised controlled trial. Traditional (pre-scientific) medicine is deemed to have special virtue, and the collection and formal analysis of data on therapeutic outcomes, failures as well as successes, is deemed inessential. There is also a tenet that if the patient gets better when treated in accordance with certain beliefs, this provides evidence for the truth of these beliefs (the post hoc ergo propter hoc30 fallacy).
CAM does not compete with the successful mainstream of scientific medicine. Users of CAM commonly have chronic conditions and have tried conventional medicine but found that it has not offered a satisfactory solution, or has caused adverse effects. The problems, when they occur, are often at the interface between CAM and mainstream medicine. A doctor prescribing a conventional medicine may be unaware that a patient is taking herbal medicine, and there is ample scope for unwanted herb–drug interaction by a variety of mechanisms.31 These include the following:
• CYP450 enzyme induction – St John’s wort (by reducing the plasma concentration or therapeutic efficacy of warfarin, ciclosporin, simvastatin, oral contraceptives).
• CYP450 enzyme inhibition – piperine (by increasing plasma concentrations of propranolol and theophylline).
• Additive action – St John’s wort on serotonin-specific reuptake inhibitors (by increasing their unwanted effects).
More troubling is the issue of conflicting advice between CAM and mainstream drugs, as witnessed by the advice to travellers from some homoeopathic pharmacies to use their products for malaria prophylaxis in place of conventional drugs (an action that drew criticism from the Society of Homoeopaths). Regulations being introduced by European Union Directive (and voluntarily in the UK) will move towards formal registration of practitioners of some forms of CAM (notably herbal medicines), according to agreed standards of qualification.
Homoeopathy
Homoeopathy32 is a system of medicine founded by Samuel Hahnemann (German physician, 1755–1843) and expounded by him in the Organon of the Rational Art of Healing.33 Hahnemann described his position:
After I had discovered the weakness and errors of my teachers and books I sank into a state of sorrowful indignation, which had nearly disgusted me with the study of medicine. I was on the point of concluding that the whole art was vain and incapable of improvement. I gave myself up to solitary reflection, and resolved not to terminate my train of thought until I had arrived at a definite conclusion on the subject.34
By understandable revulsion at the medicine of his time, by experimentation on himself (a large dose of quinine made him feel as though he had a malarial attack) and by search of records he ‘discovered’ a ‘law’ that is central to homoeopathy35, and from which the name is derived:
In addition to the above, Hahnemann ‘discovered’ that dilution potentiates the effect of drugs, but not of trace impurities (provided the dilution is shaken correctly, i.e. by ‘succussion’), even to the extent that an effective dose may not contain a single molecule of the drug. It has been pointed out36 that the ‘thirtieth potency’ (1 in 1030), recommended by Hahnemann, provided a solution in which there would be one molecule of drug in a volume of a sphere of literally astronomical circumference.
The therapeutic efficacy of a dilution at which no drug is present (including sodium chloride prepared in this way) is explained by the belief that a spiritual energy diffused throughout the medicine by the particular way in which the dilutions are shaken (succussion) during preparation, or that the active molecules leave behind some sort of ‘imprint’ on solvent or excipient.37 The absence of potentiation of the inevitable contaminating impurities is attributed to the fact that they are not incorporated by serial dilution. Thus, writes a critic: ‘We are asked to put aside the whole edifice of evidence concerning the physical nature of materials and the normal concentration–response relationships of biologically active substances in order to accommodate homoeopathic potency’.38 But no hard evidence that tests the hypothesis is supplied to justify this, and we are invited, for instance, to accept that sodium chloride merely diluted is no remedy, but that ‘it raises itself to the most wonderful power through a well prepared dynamisation process’ and stimulates the defensive powers of the body against the disease.
Pharmacologists have felt, in the absence of conclusive evidence from empirical studies that homoeopathic medicines can reproducibly be shown to differ from placebo, that there is no point in discussing its hypotheses.39 But empirical studies can be made without accepting any particular theory of causation; nor should the results of good studies be disregarded just because the proposed theory of action seems incredible or is unknown.
A meta-analysis of 186 double-blind and/or randomised placebo-controlled trials of homoeopathic remedies found that 89 had adequate data for analysis. The authors concluded that their results ‘were not compatible with the hypothesis that the clinical effects are completely due to placebo’, but also found ‘insufficient evidence from these studies that homoeopathy is clearly efficacious for any single clinical condition’.40 A subsequent analysis of 110 homoeopathic and 110 conventional medicine trials found that there was ‘weak evidence for a specific effect of homeopathic remedies, but strong evidence for a specific effect of conventional interventions’. The authors concluded: ‘This finding is compatible with the notion that the clinical effects of homeopathy are placebo effects’.41 These studies evoked strong reactions from practitioners of homoeopathy and others, but they raise the possibility that patients’ reactions to homoeopathy, and indeed some other forms of CAM, may rest within an understanding of the complex nature of the placebo response and, in particular, its biology (see below).
Placebo medicines
A placebo42 is any component of therapy that is without specific biological activity for the condition being treated.
Placebo medicines are used for two purposes:
• As a control in scientific evaluation of drugs (see Therapeutic trials, p. 45).
• To benefit or please a patient, not by any pharmacological actions, but for psychological reasons.
All treatments have a psychological component, whether to please (placebo effect) or, occasionally, to vex (negative placebo or nocebo43 effect).
A placebo medicine is a vehicle for ‘cure’ by suggestion, and is surprisingly often successful, if only temporarily.44 All treatments carry a placebo effect – physiotherapy, psychotherapy, surgery, entering a patient into a therapeutic trial, even the personality and style of the doctor – but the effect is most easily investigated with drugs, for the active and the inert can often be made to appear identical to allow comparisons.
Modern brain-scanning techniques provide evidence that the placebo effect has a physiological basis. Positron emission tomography showed that both opioid and placebo analgesia were associated with increased activity in the same cortical area of the brain, the greatest responses occurring in high placebo responders.45 Functional magnetic resonance imaging demonstrated that strong cortical activation correlated with greater placebo-induced pain relief.46
Tonics are placebos, often expensive multivitamin supplements. They may be defined as substances that aspire to strengthen and increase the appetite of those so weakened by disease, misery, overindulgence in play or work, or by physical or mental inadequacy, that they cannot face the stresses of life. The essential feature of this weakness is the absence of any definite recognisable defect for which there is a known remedy. As tonics are placebos, they must be harmless.47
Guidelines, ‘essential’ drugs and prescribing
Even the pharmaceutical industry, in its more sober moments, recognises that their ideal world in which doctors, advised and informed by industry alone, were free to prescribe whatever they pleased,48 to whomsoever they pleased, for as long as they pleased with someone other than the patient paying, is an unrealisable dream of a ‘never-never land’.
‘Essential’ drugs
Economically disadvantaged countries may seek help to construct formularies. Technical help comes from the World Health Organization (WHO) with its ‘Model List of Essential Medicines’,49 i.e. drugs (or representatives of classes of drugs) ‘that satisfy the health care needs of the majority of the population; they should therefore be available at all times in adequate amounts and in the appropriate dosage forms’. Countries seeking such advice can use the list as a basis for their own choices (the WHO also publishes model prescribing information).50 The list, updated regularly, contains about 300 items.
Cost-containment
1. Generic substitution, where a generic formulation (see Chap. 7) is substituted (by a pharmacist) for the proprietary formulation prescribed by the doctor.
2. Therapeutic substitution, where a drug of different chemical structure is substituted for the drug prescribed by the doctor. The substitute is of the same chemical class and is deemed to have similar pharmacological properties and to give similar therapeutic benefit. Therapeutic substitution is a particularly controversial matter where it is done without consulting the prescriber, and legal issues may be raised in the event of adverse therapeutic outcome.
The following facts and opinions are worth some thought:
• UK National Health Service (NHS) spending on drugs has been 9–11% per year (of the total cost) for nearly 50 years.
• General practitioners (i.e. primary care) spend some 80% of the total cost of drugs.
• In the past 25 years, the number of NHS prescriptions has risen from 5.5 to over 13 per person.
• The average cost per head of medicines supplied to people aged over 75 years is nearly five times that of medicines supplied to those below pensionable age (in the UK: women 62 years, men 65 years, but under revision).
• Under-prescribing can be just as harmful to the health of patients as over-prescribing.
Taking a drug history
The reasons for taking a drug history from patients are:
• Drugs are a cause of disease. Withdrawal of drugs, if abrupt, can also cause disease, e.g. benzodiazepines, antiepilepsy drugs.
• Drugs can conceal disease, e.g. adrenal steroid.
• Drugs can interact, producing a positive adverse effect or a negative adverse effect, i.e. therapeutic failure. This is an increasing problem with polypharmacy, especially in the elderly.
• Drugs can give diagnostic clues, e.g. ampicillin and amoxicillin causing rash in infectious mononucleosis – a diagnostic adverse effect, not a diagnostic test.
• Drugs can cause false results in clinical chemistry tests, e.g. plasma cortisol, urinary catecholamine, urinary glucose, serum renin and aldosterone.
• Drug history can assist choice of drugs in the future.
• Drugs can leave residual effects after administration has ceased, e.g. chloroquine, amiodarone.
• Drugs available for independent patient self-medication are increasing in range and importance.
(See also Appendix: the prescription.)
Prescribing should be appropriate:51
Prescribing that is inappropriate is the result of several factors:
• Giving in to patient pressure to write unnecessary prescriptions. The extra time spent in careful explanation will, in the long run, be rewarded.
• Continuing patients, especially the elderly, on courses of medicinal treatment over many months without proper review of their medication.
• Doctors may ‘prescribe brand-name drugs rather than cheaper generic equivalents, even where there is no conceivable therapeutic advantage in so doing. The fact that the brand-name products often have shorter and more memorable names than their generic counterparts’ contributes to this (Report). (See also Ch. 7.)
• ‘Insufficient training in clinical pharmacology. Many of the drugs on the market may not have been available when a general practitioner was at medical school. The sheer quantity of new products may lead to a practitioner becoming over-reliant on drugs companies’ promotional material, or sticking to “tried and tested” products out of caution based on ignorance’ (Report).
• Failure of doctors to keep up to date (see below, Doctor compliance). Computerising prescribing addresses some of these issues, for example by prompting regular review of a patient’s medication, by instantly providing generic names from brand names, by giving ready access to formularies and prescribing guidelines.
Warnings and consent
There is no formal legal or ethical obligation on doctors to warn all patients of all possible adverse consequences of treatment. It is their duty to adapt the information they give (not too little, and not so much as to cause confusion) so that the best interest of each patient is served. If there is a ‘real’ (say 1–2%) risk inherent in a procedure of some misfortune occurring, then doctors should warn patients of the possibility that the injury may occur, however well the treatment is performed. Doctors should take into account the personality of the patient, the likelihood of any misfortune arising and what warning was necessary for each particular patient’s welfare.52
Legal hazards for prescribers
The provision of information to patients is treated by (English) law as but one part of the way a doctor discharges the obligation he owes to a patient to take reasonable care in all aspects of his treatment of that patient. The provision of information is a corollary of the patient’s right to self-determination which is a right recognised by law. Failure to provide appropriate information will usually be a breach of duty and if that breach leads to the patient suffering injury then the basis for a claim for compensation exists.53
Compliance
Successful therapy, especially if it is long term, comprises a great deal more than choosing a standard medicine. It involves patient and doctor compliance.54 The latter is liable to be overlooked (by doctors), for doctors prefer to dwell on the deficiencies of their patients rather than of themselves.
Patient compliance
Patient non-compliance or non-adherence is identified as a major factor in therapeutic failure in both routine practice and in scientific therapeutic trials; but, sad to say, doctors are too often non-compliant about remedying this. All patients are potential non-compliers;55 clinical criteria cannot reliably predict good compliance, but non-compliance often can be predicted.
Non-compliance may occur because:
• the patient has not understood the instructions, so cannot comply,56 or
• the patient understands the instructions, but fails to carry them out.
Prime factors for poor patient compliance are:
• Frequency and complexity of the drug regimen. Many studies attest to polypharmacy as an inhibitor of compliance, i.e. more than three drugs taken concurrently or more than three drug-taking occasions in the day (the ideal of one occasion only is often unattainable).
• Unintentional non-compliance, or forgetfulness,57 may be addressed by associating drug-taking with cues in daily life (breakfast, bedtime), by special packaging (e.g. calendar packs) and by enlisting the aid of others (e.g. carers, teachers).
• ‘Intelligent’ or wilful non-compliance.58 Patients decide they do not need the drug (asymptomatic disease) or they do not like the drug (unwanted effects), or take 2–3-day ‘drug holidays’.
• Illness. This includes cognitive impairment and psychological problems, with depression being a particular problem.
• Lack of information. Oral instructions alone are not enough; one-third of patients are unable to recount instructions immediately on leaving the consulting room. Lucid and legible labelling of containers is essential, as well as patient-friendly information leaflets, which are increasingly available via doctors and pharmacists, and as package inserts.
• Poor patient–doctor relationship and lack of motivation to take medicines as instructed offer a major challenge to the prescriber whose diagnosis and prescription may be perfect, yet loses efficacy by patient non-compliance. Unpleasant disease symptoms, particularly where these are recurrent and known by previous experience to be quickly relieved, provide the highest motivation (i.e. self-motivation) to comply. But particularly where the patient does not feel ill, adverse effects are immediate, and benefits are perceived to be remote, e.g. in hypertension, where they may be many years away in the future, doctors must consciously address themselves to motivating compliance. The best way to achieve compliance is to cultivate the patient–doctor relationship. Doctors cannot be expected actually to like all their patients, but it is a great help (where liking does not come naturally) if they make a positive effort to understand how individual patients must feel about their illnesses and their treatments, i.e. to empathise with their patients. This is not always easy, but its achievement is the action of the true professional, and indeed is part of their professional duty of care.
Suggestions for doctors to enhance patient compliance/adherence
• Form a non-judgemental alliance or partnership with the patient, giving the patient an opportunity to ask questions.
• Plan a regimen with the minimum number of drugs and drug-taking occasions, adjusted to fit the patient’s lifestyle. Use fixed-dose combinations, sustained-release (or injectable depot) formulations, or long t½ drugs as appropriate; arrange direct observation of each dose in exceptional cases.
• Provide clear oral and written information adapted to the patient’s understanding and medical and cultural needs.
• Use patient-friendly packaging, e.g. calendar packs, where appropriate; or monitored-dose systems, e.g. boxes compartmented and labelled (Dosette boxes).
• See the patient regularly and not so infrequently that the patient feels the doctor has lost interest.
• Enlist the help of family members, carers, friends.
• Use computer-generated reminders for repeat prescriptions.
Directly observed therapy
What every patient needs to know59
• An account of the disease and the reason for prescribing.
 to relieve symptoms, i.e. how important the medicine is, whether the patient can judge its efficacy and when benefit can be expected to occur.
to relieve symptoms, i.e. how important the medicine is, whether the patient can judge its efficacy and when benefit can be expected to occur.• How and when to take the medicine.
• Whether it matters if a dose is missed and what, if anything, to do about it (see p. 24).
• For how long the medicine is likely to be needed.
• How to recognise adverse effects and any action that should be taken, including effects on car driving.
A remarkable instance of non-compliance, with hoarding, was that of a 71-year-old man who attempted suicide and was found to have in his home 46 bottles containing 10 685 tablets. Analysis of his prescriptions showed that over a period of 17 months he had been expected to take 27 tablets of several different kinds daily.60
Factors that are insignificant for compliance are: age61 (except at extremes), sex, intelligence (except at extreme deficiency) and educational level (probably).
Doctor compliance
Doctor compliance is the extent to which the behaviour of doctors fulfils their professional duty:
• to adopt new advances when they are sufficiently proved (which doctors are often slow to do)
• to tell patients what they need to know
• to warn, i.e. to recognise the importance of the act of prescribing (see also p. 6).
On a harsher note, in recent years doctors who gave drugs about which they later admitted ignorance (e.g. route of administration and/or dose) stood charged with manslaughter64 and were convicted. Shocked by this, fellow doctors have written to the medical press offering understanding sympathy to these, sometimes junior, colleagues, in effect saying ‘There, but for the grace of God, go I ’.65 The public response, however, is not sympathetic. Doctors put themselves forward as trained professionals who offer a service of responsible, competent provision of drugs that they have the legal right to prescribe. The public is increasingly inclined to hold them to that claim, and, where doctors seriously fail, to exact retribution.66
Pharmacoeconomics (see also Ch. 5)
Health-care resources are rationed67 in one way or another, whether according to national social policies or to individual wealth. The debate on supply is not about whether there should be rationing, but about what form rationing should take; whether it should be explicit or concealed (from the public).
The economists’ objective
A health economist68 writes:
• Opportunity cost means that which has to be sacrificed in order to carry out a certain course of action, i.e. costs are benefits foregone elsewhere. Money spent on prescribing is not available for another purpose; wasteful prescribing is as an affront to those who are in serious need, e.g. institutionalised mentally handicapped citizens who everywhere would benefit from increased resources, or patients requiring hip replacement.
• Cost–effectiveness analysis is concerned with how to attain a given objective at minimal financial cost, e.g. prevention of post-surgical venous thromboembolism by heparins, warfarin, aspirin, external pneumatic compression. Analysis includes the cost of materials, adverse effects, any tests, nursing and doctor time, duration of stay in hospital (which may greatly exceed the cost of the drug).
• Cost–benefit analysis is concerned with issues of whether (and to what extent) to pursue objectives and policies; it is thus a broader activity than cost–effectiveness analysis and puts monetary values on the quality as well as on the quantity (duration) of life.
• Cost–utility analysis is concerned with comparisons between programmes, such as an antenatal drug treatment which saves a young life, or a hip replacement operation which improves mobility in a man of 60 years. Such differing issues are also the basis for comparison by computing quality-adjusted life years (see below).
Blake D.R. Alternative prescribing and negligence. Br. Med. J.. 2003;326:455.
Buetow S., Elwyn G. Patient safety and patient error. Lancet. 2007;369:158–161.
De Smet P.A.G.M. Health risks of herbal remedies. Clin. Pharmacol. Ther.. 2004;76(1):1–17.
Ernst E. A historical perspective on placebo. Clin. Med. (Northfield Il). 2008;8(1):9–10.
Kandela P. Sketches from The Lancet: doctors’ handwriting. Lancet. 1999;353:1109.
Ker K., Edwards P., Roberts I. Misadventures to patients during surgical and medical care in England and Wales: an analysis of deaths and hospital episodes. J. R. Soc. Med.. 2011;104:292–298.
Loudon I. A brief history of homeopathy. J. R. Soc. Med.. 2006;99:607–610.
Mason S., Tovey P., Long A.F. Evaluating complementary medicine: methodological challenges of randomised controlled trials. Br. Med. J.. 2002;325:832–834.
McGuffin M. Should herbal medicines be regulated as drugs? Clin. Pharmacol. Ther.. 2008;83(3):393–395.
Meltzer M.I. Introduction to health economics for physicians. Lancet. 2001;358:993–998. (and subsequent papers in this quintet)
Neale G., Chapman E.J., Hoare J., Olsen S. Recognising adverse events and critical incidents in medical practice in a district general hospital. Clin. Med. (Northfield Il). 2006;6(4):157–162.
Osterberg L., Blaschke T. Adherence to medication. N. Engl. J. Med.. 2005;353(5):487–497.
Panesar S.S., Cleary K., Sheikh A. Reflections on the National Patient Safety Agency’s database of medical errors. J. R. Soc. Med.. 2009;102:256–258.
Rawlins M.D. NICE work – providing guidance to the British National Health Service. N. Engl. J. Med.. 2004;351(3):1381–1385.
Robertson J., Hill S.R. The Essential Medicines List for a global patient population. Clin. Pharmacol. Ther.. 2007;82(5):498–500.
Simpson S.H., Eurich D.T., Majumdar S.R., et al. A meta-analysis of the association between adherence to drug therapy and mortality. Br. Med. J.. 2006;333:15.
Appendix: the prescription
Prescriptions of pure drugs or of formulations from the British National Formulary (BNF)70 are satisfactory for almost all purposes. The composition of many of the preparations in the BNF is laid down in official pharmacopoeias, e.g. British Pharmacopoeia (BP). There are also many national and international pharmacopoeias.
3. Name and address of patient: date of birth is also desirable for safety reasons; in the UK it is a legal requirement for children aged under 12 years.
4. 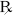 . This is a traditional esoteric symbol71 for the word ‘Recipe’ – ‘take thou’, which is addressed to the pharmacist. It is pointless; but as many doctors gain a harmless pleasure from writing it with a flourish before the name of a proprietary preparation of whose exact nature they may be ignorant, it is likely to survive as a sentimental link with the past.
. This is a traditional esoteric symbol71 for the word ‘Recipe’ – ‘take thou’, which is addressed to the pharmacist. It is pointless; but as many doctors gain a harmless pleasure from writing it with a flourish before the name of a proprietary preparation of whose exact nature they may be ignorant, it is likely to survive as a sentimental link with the past.
5. Name and dose of the medicine.
6. Directions to the pharmacist, if any: ‘mix’, ‘make a solution’. Write the total quantity to be dispensed (if this is not stated in 5 above); or duration of supply.
7. Instruction for the patient, to be written on container by the pharmacist. Here brevity, clarity and accuracy are especially important. It is dangerous to rely on the patient remembering oral instructions. The BNF provides a list of recommended ‘cautionary and advisory labels for dispensed medicines’, representing a balance between ‘the unintelligibly short and the inconveniently long’, for example: ‘Do not stop taking this medicine except on your doctor’s advice’.
Pharmacists nowadays use their own initiative in giving advice to patients.
Example of a prescription
for a patient with an annoying unproductive cough:
Computer-issued prescriptions must conform to recommendations of professional bodies. Computer-generated facsimile signatures do not meet the legal requirement.
If altered by hand (undesirable), the alteration must be signed.
Unwanted medicines
Patients should be encouraged to return these to the original supplier for disposal.
Abbreviations
(see also Weights and measures, below)
| b.d.: bis in die | twice a day (b.i.d. is also used) |
| BNF | British National Formulary |
| BP | British Pharmacopoeia |
| BPC | British Pharmaceutical Codex |
| i.m.: intramuscular | by intramuscular injection |
| IU | International Unit |
| i.v.: intravenous | by intravenous injection |
| NP: nomen proprium | proper name |
| o.d.: omni die | every day |
| o.m.: omni mane | every morning |
| o.n.: omni nocte | every night |
| p.o.: per os | by mouth |
| p.r.: per rectum | by the anal/rectal route |
| p.r.n.: pro re nata | as required. It is best to add the maximum frequency of repetition, e.g. aspirin and codeine tablets, 1 or 2 p.r.n., 4-hourly |
| p.v.: per vaginam | by the vaginal route |
| q.d.s.: quater die sumendus | four times a day (q.i.d. is also used) |
| rep.: repetatur | let it be repeated, as in rep. mist(ura), repeat the mixture |
| s.c.: subcutaneous | by subcutaneous injection |
| stat: statim | immediately |
| t.d.s.: ter (in) die sumendus | three times a day (t.i.d. is also used) |
Percentages, proportions, weight in volume
Some solutions of drugs (e.g. local anaesthetics, adrenaline/epinephrine) for parenteral use are labelled in a variety of ways: percentage, proportion, or weight in volume (e.g. 0.1%, 1: 1000, 1 mg/mL). In addition, dilutions may have to be made by doctors at the time of use. Such drugs are commonly dangerous in overdose and great precision is required, especially as any errors are liable to be by a factor of 10 and can be fatal. Doctors who do not feel confident with such calculations (because they do not do them frequently) should feel no embarrassment,73 but should recognise that they have a responsibility to check their results with a competent colleague or pharmacist before proceeding.
1 http://www.gmc-uk.org/about/research/research_commissioned_4.asp (accessed 4 October 2011).
2 http://www.gmc-uk.org/education/undergraduate/tomorrows_doctors_2009.asp (accessed 4 October 2011).
3 His work had such a profound influence on medicine that he was called the ‘English Hippocrates’.
4 Medical Essays (1891). American physician and poet, and Dean of Harvard Medical School; he introduced the term anaesthesia instead of ‘suspended animation’ or ‘etherisation’. Address delivered before the Massachusetts Medical Society, 30 May 1860 (Oliver Wendell Holmes, Medical Essays. Kessinger Publishing, p. 140).
5 Sherman L J 1959 The significant variables in psychopharmaceutic research. American Journal of Psychiatry 116:208–214.
6 Michel de Montaigne (1533–1592). French essayist.
7 Kohn L, Corrigan J, Donaldson M (eds) for the Committee on Quality of Health Care in America, Institute of Medicine 2000 To Err is Human: Building a Safer Health System. National Academy Press, Washington, DC.
8 Bates D W, Cullen D J, Laird N et al 1995 Incidence of adverse drug events and potential adverse drug events. Journal of the American Medical Association 274:29–34.
9 Iatrogenic means ‘physician-caused’, i.e. disease consequent on following medical advice or intervention (from the Greek iatros, physician).
10 Sollman T A 1917 Manual of Pharmacology. Saunders, Philadelphia.
11 This phrase is commonly used in the context of motor vehicle accidents, but applies equally well to the prescribing of drugs.
12 Sometimes the term minimal risk is used to mean risk about equal to going about our ordinary daily lives; it includes travel on public transport, but not motor bicycling on a motorway.
13 Pochin E E 1975 The acceptance of risk. British Medical Bulletin 31:184–190.
14 Doctors who seek to exculpate themselves from serious, even fatal, prescribing errors by appealing to undoubted difficulties presented by the information explosion of modern times, allied to pressures of work, are unlikely to get sympathy, and increasingly are more likely to be told, ‘If you can’t stand the heat, get out of the kitchen’ (a dictum attributed to Harry S Truman, US President 1948–52, though he assigns it to US Army General Harry Vaughn). Pharmacists and nurses stand ready and willing to relieve doctors of the burden of prescribing.
15 A cure eliminates a disease and may be withdrawn when this is achieved.
16 Even if given the best treatment. ‘Opium alone stands the test of experience as a remedy capable of limiting the progress of the disease’, wrote the great Sir William Osler, successively Professor of Medicine in Pennsylvania, McGill, Johns Hopkins and Oxford universities, in 1918, only 3 years before the discovery of insulin.
17 This discussion is about drugs that have been properly manufactured and meet proper standards, e.g. of purity, stability, as laid down by regulatory bodies or pharmacopoeias. A manufacturing defect would be dealt with in a way no different from manufacturing errors in other products.
18 A plaintiff (person who believes he/she has been injured) seeking to obtain compensation from a defendant (via the law of negligence) must prove three things: (1) that the defendant owed a duty of care to the plaintiff; (2) that the defendant failed to exercise reasonable care; and (3) that the plaintiff has a suffered actual injury as a result.
19 The following distinction is made in some discussions of product liability. Strict liability: compensation is provided by the producer/manufacturer. No-fault liability or scheme: compensation is provided by a central fund.
20 Royal Commission on Civil Liability and Compensation for Personal Injury 1978 HMSO, London: Cmnd. 7054. Although the Commission considered compensation for death and personal injury suffered by any person through manufacture, supply or use of products, i.e. all goods whether natural or manufactured, and included drugs and even human blood and organs, it made no mention of tobacco and alcohol.
21 Gaine W J 2003 No-fault compensation schemes. British Medical Journal 326:997–998.
22 This is the criterion for (UK) civil law, rather than ‘beyond reasonable doubt’, which is the criterion of criminal law.
23 The definition adopted by the Cochrane Collaboration is as follows: ‘Complementary and alternative medicine (CAM) is a broad domain of healing resources that accompanies all health systems, modalities, and practices and their accompanying theories and beliefs, other than those intrinsic to the politically dominant health system of a particular society or culture in a given historical period. CAM includes all such practices and ideas self-defined by their users as preventing or treating illness or promoting health and well-being. Boundaries within CAM and between the CAM domain and that of the dominant system are not always sharp or fixed.’
24 Traditional medicine is fostered particularly in countries where scientific medicine is not accessible to large populations for economic reasons, and destruction of traditional medicine would leave unhappy and sick people with nothing. For this reason, governments are supporting traditional medicine and at the same time initiating scientific clinical evaluations of the numerous plants and other items employed, many of which contain biologically active substances. The World Health Organization is supportive of these programmes.
25 Ernst E 2000 The role of complementary and alternative medicine. British Medical Journal 32:1133–1135.
26 De Smet P A G M 2005 Herbal medicine in Europe – relaxing regulatory standards. New England Journal of Medicine 352:1176–1178.
27 A cult is a practice that follows a dogma, tenet or principle based on theories or beliefs of its promulgator to the exclusion of demonstrable scientific experience (definition of the American Medical Association). Scientific medicine changes in accord with evidence obtained by scientific enquiry applied with such intellectual rigour as is humanly possible. But this is not the case with cults, the claims for which are characterised by absence of rigorous intellectual evaluation and unchangeability of beliefs. The profusion of medical cults prompts the question why, if each cult has the efficacy claimed by its exponents, conventional medicine and indeed the other cults are not swept away. Some practitioners use conventional medicine and, where it fails, turn to cult practices. Where such complementary practices give comfort they are not to be despised, but their role and validity should be clearly defined. No community can afford to take these cults at their own valuation; they must be tested, and tested with at least the rigour required to justify a therapeutic claim for a new drug. It is sometimes urged in extenuation that traditional and cult practices do no harm to patients, unlike synthetic drugs. But, even if that were true (which it is not), investment of scarce resources in delivering what may be ineffective, though sometimes pleasing, experiences, e.g. dance therapy, exaltation of flowers or the admittedly inexpensive urine therapy, means that resources are not available for other desirable social objectives, e.g. housing, art subsidies, medicine. We do not apologise for this diversion to consider medical cults and practices, for the world cannot afford unreason, and the antidote to unreason is reason and the rigorous pursuit of knowledge, i.e. evidence-based medicine.
28 Ernst E (ed) 2001 The Desktop Guide to Complementary and Alternative Medicine. Harcourt, Edinburgh.
29 Black cohosh (Cimicifuga racemosa), taken for hot flushes and other menopausal symptoms (but no better than placebo in clinical trial), can cause serious liver disorder. Herbal teas containing pyrrolizidine alkaloids (Senecio, Crotalaria, Heliotropium) cause serious hepatic veno-occlusive disease. Comfrey (Symphytum) is similar but also causes hepatocellular tumours and haemangiomas. Sassafras (carminative, antirheumatic) is hepatotoxic. Mistletoe (Viscum) contains cytotoxic alkaloids. Ginseng contains oestrogenic substances that have caused gynaecomastia; long-term users may show ‘ginseng abuse syndrome’ comprising central nervous system excitation; arterial hypertension can occur. Liquorice (Glycyrrhiza) has mineralocorticoid action. An amateur ‘health food enthusiast’ made himself a tea from ‘an unfamiliar [ to him ] plant’ in his garden; unfortunately this was the familiar foxglove (Digitalis purpurea) and as a result he became very ill, but happily recovered. Other toxic natural remedies include lily of the valley (Convallaria) and horse chestnut (Aesculus). ‘The medical herbalist is at fault for clinging to outworn historical authority and for not assessing his drugs in terms of today’s knowledge, and the orthodox physician is at fault for a cynical scepticism with regard to any healing discipline other than his own’ (Penn R G 1983 Adverse reactions to herbal medicines. Adverse Drug Reaction Bulletin 102:376–379). The Medicines and Healthcare products Regulatory Agency provides advice at: http://www.mhra.gov.uk.
30 Latin: after this; therefore on account of this.
31 Hu Z, Yang X, Ho P C L et al 2005 Herb–drug interactions: a literature review. Drugs 65:1239–1281.
32 Greek: homos = same; patheia = suffering.
33 1810: trans. Wheeler C E 1913 (Organon of the Rational Art of Healing.) Dent, London.
34 Hahnemann S 1805 Aesculapius in the Balance. Leipzig.
35 By contrast, allopathy was a system of medicine based on the principle that induction of a new disease would drive out an existing disease. It was practised by measures that included purging, bleeding and sweating. Use of the word to distinguish homoeopathy from conventional scientific medicine is clearly incorrect.
36 Clark A J 1937 General pharmacology. In: Hefter’s Handbuch. Springer, Berlin.
37 Homoeopathic practitioners repeatedly express their irritation that critics give so much attention to dilution. They should not be surprised, considering the enormous implications of their claim.
38 Cuthbert A W 1982 Pharmaceutical Journal (15 May):547.
39 Editorial 1988 When to believe the unbelievable. Nature 333:787. A report of an investigation into experiments with antibodies in solutions that contained no antibody molecules (as in some homoeopathic medicines). The editor of Nature took a three-person team (one of whom was a professional magician, included to detect any trickery) on a week-long visit to the laboratory that claimed positive results. Despite the scientific seriousness of the operation, it developed comical aspects (codes of the contents of test tubes were taped to the laboratory ceiling); the Nature team, having reached an unfavourable view of the experiments, ‘sped past the (laboratory) common-room filled with champagne bottles destined now not to be opened’. Full reports in this issue of Nature (28 July 1988), including an acrimonious response by the original scientist, are highly recommended reading, both for scientific logic and for entertainment. See also Nature (1994) 370:322.
40 Linde K, Clausius N, Melchart D et al 1997 Are the clinical effects of homoeopathy placebo effects? A meta-analysis of placebo-controlled trials. Lancet 350:834–843.
41 Shang A, Huwiler-Müntener K, Nartey L et al 2005 Are the clinical effects of homeopathy placebo effects? Comparative study of placebo-controlled trias of homeopathy and allopathy. Lancet 366:726–732.
42 Latin: placebo = shall be pleasing or acceptable. For a comment on its historical use, see Edwards M 2005 Lancet 365:1023.
43 Latin: nocebo = shall injure; the term is little used.
44 As the following account by a mountain rescue guide illustrates: ‘The incident involved a 15-year-old boy who sustained head injuries and a very badly broken leg. Helicopter assistance was unavailable and therefore we had to carry him by stretcher to the nearest landrover (several miles away) and then on to a waiting ambulance. During this long evacuation the boy was in considerable distress and we administered Entonox (a mixture of nitrous oxide and oxygen, 50% each) sparingly as we only had one small cylinder. He repeatedly remarked how much better he felt after each intake of Entonox (approximately every 20 minutes) and after 7 hours or so, we eventually got him safely into the ambulance and on his way to hospital. On going to replace the Extonox we discovered the cylinder was still full of gas due to the equipment being faulty. There was no doubt that the boy felt considerable pain relief because he thought he was receiving Entonox.’
45 Petrovic P, Kalso E, Petersson K et al 2002 Placebo and opioid analgesia – imaging a shared neuronal network. Science 295:1737–1740.
46 Wager T D, Rilling J K, Smith E S et al 2004 Placebo induced changes in fMRI in anticipation and experience of pain. Science 303:1162–1167.
47 Tonics (licensed) available in the UK include: Gentian Mixture, acid (or alkaline) (gentian, a natural plant bitter substance, and dilute hydrochloric acid or sodium bicarbonate); Labiton (thiamine, caffeine, alcohol, all in low dose).
48 It is difficult for us now to appreciate the naive fervour and trust in doctors that allowed them almost unlimited rights to prescribe in the early years of the UK National Health Service (founded in 1948). Beer was a prescription item in hospitals until, decades later, an audit revealed that only 1 in 10 bottles reached a patient. More recently (1992): ‘There could be fewer Christmas puddings consumed this year. The puddings were recently struck off a bizarre list of items that doctors were able to prescribe for their patients. They were removed by Health Department officials without complaint from the medics, on the grounds they had “no therapeutic or clinical value”.’ (Lancet (1992) 340:1531).
49 Available on the WHO website: http://www.who.org.
50 There is an agency for WHO publications in all UN countries.
51 The text on appropriate prescribing and some quotations (designated ‘Report’) are based on a UK Parliamentary Report (The National Health Service Drugs Budget 1994 HMSO, London). Twelve members of Parliament took evidence from up to 100 organisations and individuals orally and/or in writing.
52 Legal correspondent 1980 British Medical Journal 280:575.
54 The term ‘compliance’ meets objection as having undertones of obsolete, authoritarian attitudes, implying ‘obedience’ to doctors’ ‘orders’. The words adherence or concordance are preferred by some, the latter because it expresses the duality of drug prescribing (by the doctor) and taking (by the patient), i.e. a therapeutic alliance. We retain compliance, pointing out that it applies equally to those doctors who neither keep up to date, nor follow prescribing instructions, and to patients who fail, for whatever reason, to keep to a drug regimen.
55 Even where the grave consequences of non-compliance are understood (glaucoma: blindness) (renal transplant: organ rejection), significant non-compliance has been reported in as many as 20% of patients; psychologists will be able to suggest explanations for this.
56 Cautionary tales. (1) A 62-year-old man requiring a metered-dose inhaler (for the first time) was told to ‘spray the medicine to the throat’. He was found to have been conscientiously aiming and firing the aerosol to his anterior neck around the thyroid cartilage, four times a day for 2 weeks (Chiang A A, Lee J C 1994 New England Journal of Medicine 330:1690). (2) A patient thought that ‘sublingual’ meant able to speak two languages; (3) another that tablets cleared obstructed blood vessels by exploding inside them (E A Kay) – reference, no doubt, to colloquial use of the term ‘clot-busting drugs’ (for thrombolytics). These are extreme examples; most are more subtle and less detectable. Doctors may smile at the ignorant naivety of patients, but the smile should give way to a blush of shame at their own deficiencies as communicators.
57 Where non-compliance, whether intentional or unintentional, is medically serious it becomes necessary to bypass self-administration (unsupervised) and to resort to directly observed (supervised) oral administration or to injection (e.g. in schizophrenia).
58 Of the many causes of failure of patient compliance, the following case must be unique. On a transatlantic flight the father of an asthmatic boy was seated in the row behind two doctors. He overheard one of the doctors expressing doubt about the long-term safety in children of inhaled corticosteroids. He interrupted the conversation, explaining that his son took this treatment; he had a lengthy conversation with one of the doctors, who gave his name. Consequently, on arrival, he faxed his wife at home to stop the treatment of their son immediately. She did so, and 2 days later the well controlled patient had a brisk relapse that responded to urgent treatment by the family doctor (who had been conscientiously following guidelines recently published in an authoritative journal). The family doctor later ascertained that the doctor in the plane was a member of the editorial team of the journal that had so recently published the guidelines that were favourable to inhaled corticosteroid (Cox S 1994 Is eavesdropping bad for your health? British Medical Journal 309:718).
59 After: Drug and Therapeutics Bulletin 1981; 19:73. Patient information leaflets. In economically privileged countries, original or patient-pack dispensing is becoming the norm, i.e. patients receive an unopened pack just as it left the manufacturer. The pack contains a patient information leaflet (PIL) (which therefore accompanies each repeat prescription). Regulatory authorities increasingly determine its content. In this litigious age, requirements to be comprehensive and, to protect both manufacturer and regulatory authority, impair the patient-friendliness of PILs. But studies have shown that patients who receive leaflets are more satisfied than those who do not. Doctors need to have copies of these leaflets so that they can discuss with their patients what they are (or are not) reading.
60 Smith S E, Stead K C 1974 Non-compliance or mis-prescribing? Lancet i:937 [letter].
61 But the elderly are commonly taking several drugs – a major factor in non-compliance – and monitoring compliance in this age group becomes particularly important. The over-60s in the UK are, on average, each receiving two or three medications.
62 Hippocrates (460–377 BC) noted that patients are liars regarding compliance. The way the patient is questioned may be all important, e.g. ‘Were you able to take the tablets?’ may get a truthful reply, whereas ‘Did you take the tablets?’ may not, because the latter question may be understood by the patient as implying personal criticism (Pearson R M 1982 Who is taking their tablets? British Medical Journal 285:757).
63 Accuracy includes legibility: a doctor wrote Intal (sodium cromoglicate) for an asthmatic patient; the pharmacist read it as Inderal (propranolol) – the patient died. See also, Names of drugs (Ch. 7).
64 Unlawful killing in circumstances that do not amount to murder (which requires an intention to kill), e.g. causing death by negligence that is much more serious than mere carelessness; reckless breach of the legal duty of care.
65 Attributed to John Bradford, an English preacher and martyr (16th century), on seeing a convicted criminal pass by.
66 A doctor wrote a prescription for isosorbide dinitrate 20 mg 6-hourly, but because of the illegibility of the handwriting the pharmacist dispensed felodipine in the same dose (maximum daily dose 10 mg). The patient died and a court ordered the doctor and pharmacist to pay compensation of $450 000 to the family. Charatan F 1999 Family compensated for death after illegible prescription. British Medical Journal 319:1456.
67 The term ‘rationing’ is used here to embrace the allocation of priorities as well as the actual withholding of resources (in this case, drugs).
68 Professor Michael Drummond.
69 Williams A 1983 In: Smith G T (ed) Measuring the Social Benefits of Medicine. Office of Health Economics, London.
70 Supplied free to all doctors practising in the UK National Health Service.
71 Derived from the eye of Horus, Ancient Egyptian sun god.
72 Spell out in full in prescriptions.
73 Called to an emergency tension pneumothorax on an intercontinental flight, two surgeons, who chanced to be passengers, were provided with lidocaine 100 mg in 10 mL (in the aircraft medical kit). They were accustomed to thinking in percentages for this drug and ‘in the heat of the moment’ neither was able to make the conversion. Chest surgery was conducted successfully with an adapted wire coat-hanger as a trocar (‘sterilised’ in brandy), using a urinary catheter. The patient survived the flight and recovered in hospital. Wallace W A 1995 Managing in-flight emergencies: a personal account. British Medical Journal 311:374.
[/level-membership-for-basic-science-category][not-level-membership-for-basic-science-category]
Chapter 2 Topics in drug therapy
Practical prescribing
The case histories are all real. The data given in the text and figures come from a study commissioned by the General Medical Council.1
Prescribing
Getting it right
Good prescribing starts with taking a good history:
• Does your patient have other medical conditions – some may be worsened by treatment you would normally give for their presenting complaint.
• What drugs is your patient taking now? What are they for? Are they all still needed? Could they be causing the symptoms or signs that have brought the patient to you? Could they interact with whatever you might think of prescribing?
• What drugs has your patient taken in the past? Why were they stopped? Did they cause side-effects?
• Is the patient allergic to any drugs?
• Are they taking any non-prescription (over-the-counter) drugs? If so, could they interact with whatever you might prescribe (for example, St John’s wort is an enzyme-inducer)?
• Making a diagnosis – or at least having a range of possibilities. Know what it is you are wishing to achieve and the evidence for the likely efficacy of the drug treatment you wish to give.
• Knowing your patient’s kidney and liver function – most drugs are eliminated by these organs; and some drugs can damage them.
• Getting the dose right. For many drugs you will not know the dose, so do not pretend you do. Never, ever guess. Never be afraid to ask. Never be too busy to look up a dose – better to check now than make a trip to the Coroner’s Court later.
• Explaining to your patient why you think this treatment will work, the likelihood of it working, the more common side-effects and what your plans are if it does not work.
• Being alert to the development of adverse drug reactions. If a patient develops new symptoms after starting a drug, it is probably the drug. If the adverse effect is in a fairly new drug – or is not already well known – you should report the event to the national body responsible for monitoring and recording adverse drug reactions.
• Being very clear about what it is you are prescribing.
• If using a hand-written prescription, write clearly.
• If working in a different hospital, remember that the prescription chart may not be the same as where you have just been.
• If using electronic prescribing, beware drop-down menus and drugs with similar looking names, e.g. carbimazole and carbamazepine.
Examples of when things went wrong
Forgetting that a newly prescribed drug can interact with long-term drug treatment
A 64-year-old man had been taking warfarin for many years. He developed a chest infection and an out of hours doctor prescribed amoxicillin. Later that week he was admitted with a large, painful right knee haemarthrosis and an INR > 10 (see p. 489). New drugs may interact with those the patient has been taking for a long time!
Why do mistakes happen?
There are also factors specific to the medical environment, including:
• Not familiar with the drug chart (usually on moving to a new hospital).
• Unfamiliar patient – and not taking the time to become familiar with the full medical and drug history.
• Arithmetical errors in calculating dose.
• Omitting drugs for a newly admitted patient because of inadequate information.
When lack of knowledge does play a part, it is often the flawed application of knowledge in that particular patient – i.e. the right drug for the presenting condition, but the wrong drug for that patient because of coexisting medical or drug factors.
The General Medical Council expects that, by the time they graduate, medical students will be able to:2
• Prescribe drugs safely, effectively and economically.
• Establish an accurate drug history, covering both prescribed and other medication.
• Plan appropriate drug therapy for common indications, including pain and distress.
• Provide a safe and legal prescription.
• Calculate appropriate drug doses and record the outcome accurately.
• Provide patients with appropriate information about their medicines.
• Access reliable information about medicines.
• Detect and report adverse drug reactions.
• Demonstrate awareness that many patients use complementary and alternative therapies, and awareness of the existence and range of these therapies, why patients use them, and how this might affect other types of treatment that patients are receiving.
The therapeutic situation
Some background
Remarkably, this system persisted among ‘learned and rational’ (i.e. university-trained) physicians until it was challenged in the 17th century. Thomas Sydenham3 (1624–1689) showed that during epidemics, many people could suffer the same disease, and different epidemics had distinct characteristics. Later, Giovanni Morgagni (1682–1771), by correlating clinical and autopsy findings, demonstrated that diseases related to particular organs. Now the study of disease, rather than the patient, became the centre of attention. Yet it was only in the 19th century that medicine developed as a science, when the microscope revealed the cell as the basic construction unit of the body and specific entities of pathology became recognisable, most notably in the case of infection with microorganisms (‘germ theory’).
Throw out opium …; throw out a few specifics …; throw out wine, which is a food, and the vapours which produce the miracle of anaesthesia, and I firmly believe that if the whole materia medica, as now used, could be sunk to the bottom of the sea, it would be all the better for mankind, – and all the worse for the fishes…4
Treating patients with drugs
A book can provide knowledge and contribute to the formation of judgement, but it can do little to impart skill and wisdom, which are the products of example of teachers and colleagues, of experience and of innate and acquired capacities. But: ‘It is evident that patients are not treated in a vacuum and that they respond to a variety of subtle forces around them in addition to the specific therapeutic agent.’5
When a patient receives a drug, the response can be the result of numerous factors:
• The pharmacodynamic effect of the drug and interactions with any other drugs the patient may be taking.
• The pharmacokinetics of the drug and its modification in the individual by genetic influences, disease, other drugs.
• The act of medication, including the route of administration and the presence or absence of the doctor.
• What the doctor has told the patient.
• The patient’s past experience of doctors.
• The patient’s estimate of what has been received and of what ought to happen as a result.
• The social environment, e.g. whether it is supportive or dispiriting.
Drugs can do harm
Efficacy and safety do not lie solely in the molecular structure of the drug. Doctors must choose which drugs to use and must apply them correctly in relation not only to their properties, but also to those of the patients and their disease. Then patients must use the prescribed medicine correctly (see Compliance p. 21).
Uses of drugs/medicines
Prevention
1. Should I interfere with the patient at all?
2. If so, what alteration in the patient’s condition do I hope to achieve?
3. Which drug is most likely to bring this about?
4. How can I administer the drug to attain the right concentration in the right place at the right time and for the right duration?
5. How will I know when I have achieved the objective?
6. What other effects might the drug produce, and are these harmful?
7. How will I decide to stop the drug?
8. Does the likelihood of benefit, and its importance, outweigh the likelihood of damage, and its importance, i.e. the benefit versus risk, or efficacy against safety?
Physician-induced (iatrogenic) disease
It is a salutary thought that each year medical errors kill an estimated 44 000–98 000 Americans (more than die in motor vehicle accidents) and injure 1 000 000.7 Among inpatients in the USA and Australia, about half of the injuries caused by medical mismanagement result from surgery, but therapeutic mishaps and diagnostic errors are the next most common. In one survey of adverse drug events, 1% were fatal, 12% life-threatening, 30% serious and 57% significant.8 About half of the life-threatening and serious events were preventable. Errors of prescribing account for one-half and those of administering drugs for one-quarter of these. Inevitably, a proportion of lapses result in litigation, and in the UK 20–25% of complaints received by the medical defence organisations about general practitioners follow medication errors.
The most shameful act in therapeutics, apart from actually killing a patient, is to injure a patient who is but little disabled or who is suffering from a self-limiting disorder. Such iatrogenic disease,9 induced by misguided treatment, is far from rare.
In 1917 the famous pharmacologist Sollmann felt able to write:
Pharmacology comprises some broad conceptions and generalisations, and some detailed conclusions, of such great and practical importance that every student and practitioner should be absolutely familiar with them. It comprises also a large mass of minute details, which would constitute too great a tax on human memory, but which cannot safely be neglected.10
Benefits and risks of medicines
Unavoidable risks
Consider, for the sake of argument, the features that a completely risk-free drug would exhibit:
• The physician would know exactly what action is required and use the drug correctly.
• The drug would deliver its desired action and nothing else, either by true biological selectivity or by selective targeted delivery.
• The drug would achieve exactly the right amount of action – neither too little, nor too much.
These criteria may be completely fulfilled, for example in a streptococcal infection sensitive to penicillin in patients whose genetic constitution does not render them liable to an allergic reaction to penicillin.
Some reasons why drugs fail to meet the criteria of being risk-free include the following:
• Drugs may be insufficiently selective. As the concentration rises, a drug that acts at only one site at low concentrations begins to affect other target sites (receptors, enzymes) and recruit new (unwanted) actions; or a disease process (cancer) is so close to normal cellular mechanisms that perfectly selective cell kill is impossible.
• Drugs may be highly selective for one pathway but the mechanism affected has widespread functions and interference with it cannot be limited to one site only, e.g. atenolol on the β-adrenoceptor, aspirin on cyclo-oxygenase.
• Prolonged modification of cellular mechanisms can lead to permanent change in structure and function, e.g. carcinogenicity.
• Insufficient knowledge of disease processes (some cardiac arrhythmias) and of drug action can lead to interventions that, although undertaken with the best intentions, are harmful.
• Patients are genetically heterogeneous to a high degree and may have unpredicted responses to drugs.
• Dosage adjustment according to need is often unavoidably imprecise, e.g. in depression.
Reduction of risk
Strategies that can limit risk include those directed at achieving:
Two broad categories of risk
1. First are those that we accept by deliberate choice. We do so even if we do not exactly know their magnitude, or we know but wish they were smaller, or, especially when the likelihood of harm is sufficiently remote though the consequences may be grave, we do not even think about the matter. Such risks include transport and sports, both of which are inescapably subject to potent physical laws such as gravity and momentum, and surgery to rectify disorders that we could tolerate or treat in other ways, as with much cosmetic surgery.
2. Second are those risks that cannot be significantly altered by individual action. We experience risks imposed by food additives (preservatives, colouring), air pollution and some environmental radioactivity. But there are also risks imposed by nature, such as skin cancer due to excess ultraviolet radiation in sunny climes, as well as some radioactivity.
It seems an obvious course to avoid unnecessary risks, but there is disagreement on what risks are truly unnecessary and, on looking closely at the matter, it is plain that many people habitually take risks in their daily and recreational life that it would be a misuse of words to describe as necessary. Furthermore, some risks, although known to exist, are, in practice, ignored other than by conforming to ordinary prudent conduct. These risks are negligible in the sense that they do not influence behaviour, i.e. they are neglected.12
Elements of risk
There is general agreement that drugs prescribed for disease are themselves the cause of a significant amount of disease (adverse reactions), of death, of permanent disability, of recoverable illness and of minor inconvenience. In one major UK study the prevalence of adverse drug reactions as a cause of admission to hospital was 6.5% (see Chapter 9 for other examples).
Three major grades of risk
Risks are among the facts of life. In whatever we do and in whatever we refrain from doing, we are accepting risk. Some risks are obvious, some are unsuspected and some we conceal from ourselves. But risks are universally accepted, whether willingly or unwillingly, whether consciously or not.13
Whenever a drug is taken a risk is taken
In some chronic diseases that ultimately necessitate suppressive drugs, the patient may not experience benefit in the early stages. Patients with early Parkinson’s disease may experience little inconvenience or hazard from the condition, and premature exposure to drugs can exact such a price in unwanted effects that they prefer the untreated state. What patients will tolerate depends on their personality, their attitude to disease, their occupation, mode of life and relationship with their doctor (see Compliance, p. 21).
Public view of drugs and prescribers
There are obvious areas where some remedial action is possible:
• Improvement of prescribing by doctors, including better communication with patients, i.e. doctors must learn to feel that introduction of foreign chemicals into their patients’ bodies is a serious matter, which many or most do not seem to feel at present.14
• Introduction of no-fault compensation schemes for serious drug injury (some countries already have these).
• Informed public discussion of the issues between the medical profession, industrial drug developers, politicians and other ‘opinion-formers’ in society, and patients (the public).
• Restraint in promotion by the pharmaceutical industry including self-control by both industry and doctors in their necessarily close relationship, which the public is inclined to regard as a conspiracy, especially when the gifts and payments made to doctors get into the news. (This is much less prevalent than it was in the 1990s.)
If restraint by both parties is not forthcoming, and it may not be, then both doctor and industry can expect even more control to be exercised over them by politicians responding to public demand. If doctors do not want their prescribing to be restricted, they should prescribe better.
Criticisms of modern drugs
Two examples of inappropriate measurements will suffice:
1. In the case of many infections it is not disputed that environmental changes have had a greater beneficial effect on health than the subsequently introduced antimicrobials. But this does not mean that environmental improvements alone are sufficient in the fight against infections. When comparisons of illnesses in the pre- and post-antimicrobial eras are made, like is not compared with like. Environmental changes achieved their results when mortality from infections was high and antimicrobials were not available; antimicrobials were introduced later against a background of low mortality as well as of environmental change; decades separate the two parts of the comparison, and observers, diagnostic criteria and data recording changed during this long period. It is evident that determining the value of antimicrobials is not simply a matter of looking at mortality rates.
2. About 1% of the UK population has diabetes mellitus, a figure which is increasing rapidly, and about 1% of death certificates mention diabetes. This is no surprise because all must die and insulin is no cure15 for this lifelong disease. A standard medical textbook of 1907 stated that juvenile-onset ‘diabetes is in all cases a grave disease, and the subjects are regarded by all assurance companies as uninsurable lives: life seems to hang by a thread, a thread often cut by a very trifling accident’. Most, if not all, life insurance companies now accept young people with diabetes with no or only modest financial penalty, the premium of a person 5–10 years older. Before insulin replacement therapy was available few survived beyond 3 years16 after diagnosis; they died for lack of insulin. It is unjustified to assert that a treatment is worthless just because its mention on death certificates (whether as a prime or as a contributory cause) has not declined. The relevant criteria for juvenile-onset diabetes are change in the age at which the subjects die and the quality of life between diagnosis and death, and both of these have changed enormously.
Drug-induced injury17 (see also Ch. 9)
Negligence and strict and no-fault liability
All civilised legal systems provide for compensation to be paid to a person injured as a result of using a product of any kind that is defective due to negligence (fault: failure to exercise reasonable care).18 But there is a growing opinion that special compensation for serious personal injury, beyond the modest sums that general social security systems provide, should be automatic and not dependent on fault and proof of fault of the producer, i.e. there should be ‘liability irrespective of fault’, ‘no-fault liability’ or ‘strict liability’.19 After all, victims need assistance (compensation) regardless of the cause of injury and whether or not the producer and, in the case of drugs, the prescriber deserves censure. The question why a person who has suffered injury due to the biological accident of disease should have to depend on social security payments while an identical injury due to a drug (in the absence of fault) should attract special added compensation receives no persuasive answer except that this is what society seems to want.
Many countries are now revising their laws on liability for personal injury due to manufactured products and are legislating Consumer Protection Acts (Statutes) which include medicines, for ‘drugs represent the class of product in respect of which there has been the greatest pressure for surer compensation in cases of injury’.20
Issues that are central to the debate include:
• Capacity to cause harm is inherent in drugs in a way that sets them apart from other manufactured products; and harm often occurs in the absence of fault.
• Safety, i.e. the degree of safety that a person is entitled to expect, and adverse effects that should be accepted without complaint, must often be a matter of opinion and will vary with the disease being treated, e.g. cancer or insomnia.
• Causation, i.e. proof that the drug in fact caused the injury, is often impossible, particularly where it increases the incidence of a disease that occurs naturally.
• Contributory negligence. Should compensation be reduced in smokers and drinkers where there is evidence that these pleasure drugs increase liability to adverse reactions to therapeutic drugs?
• The concept of defect, i.e. whether the drug or the prescriber or indeed the patient can be said to be ‘defective’ so as to attract liability, is a highly complex matter and indeed is a curious concept as applied to medicine.
Nowhere has a scheme that meets all the major difficulties yet been implemented. This is not because there has been too little thought, it is because the subject is so difficult. Nevertheless, no-fault schemes operate in New Zealand, Scandinavia and France.21 The following principles might form the basis of a workable compensation scheme for injury due to drugs:
• New unlicensed drugs undergoing clinical trial in small numbers of subjects (healthy or patient volunteers): the developer should be strictly liable for all adverse effects.
• New unlicensed drugs undergoing extensive trials in patients who may reasonably expect benefit: the producer should be strictly liable for any serious effect.
• New drugs after licensing by an official body: the manufacturer and the community should share liability for serious injury, as new drugs provide general benefit. An option might be to institute a defined period of formal prospective drug surveillance monitoring, in which both doctors and patients agree to participate.
• Standard drugs in day-to-day therapeutics: there should be a no-fault scheme, operated by or with the assent of government that has authority, through tribunals, to decide cases quickly and to make awards. This body would have authority to reimburse itself from others – manufacturer, supplier, prescriber – wherever that was appropriate. An award must not have to wait on the outcome of prolonged, vexatious, adversarial, expensive court proceedings. Patients would be compensated where:
[/not-level-membership-for-basic-science-category]