Chapter 4
The musculoskeletal system and human movement
Lynne Newton Triggs1 and Jean Rogers2
1 Bedford Hospital, Bedford, UK
2 Stepping Hill Hospital, Stockport, UK
Introduction
The aim of this chapter is to provide an overview of musculoskeletal structure and function while relating it to human movement. Structure and function are linked and it is impossible to discuss one without the other. It is essential that orthopaedic and trauma practitioners know and understand the terms used to describe anatomical positions and the structures involved in musculoskeletal conditions, injuries and surgery to facilitate safe, high quality care. It is also essential to provide a common language which is effective in interdisciplinary communication as this ensures practitioners can explain specific conditions, injuries, surgery and treatment to other staff, patients and relatives to enable them to engage in their care.
Anatomical positioning
The human body is described as being in anatomical position when the body is upright with the head facing forward, hands at the side facing forward with the thumbs pointing away from the body and the feet hip-width apart with the feet and toes pointing forward (Figure 4.1). This position is known universally. When referring to the right and left of the body it is the right and left of the person who is the subject of discussion (e.g. the patient) not the left and right of the observer.
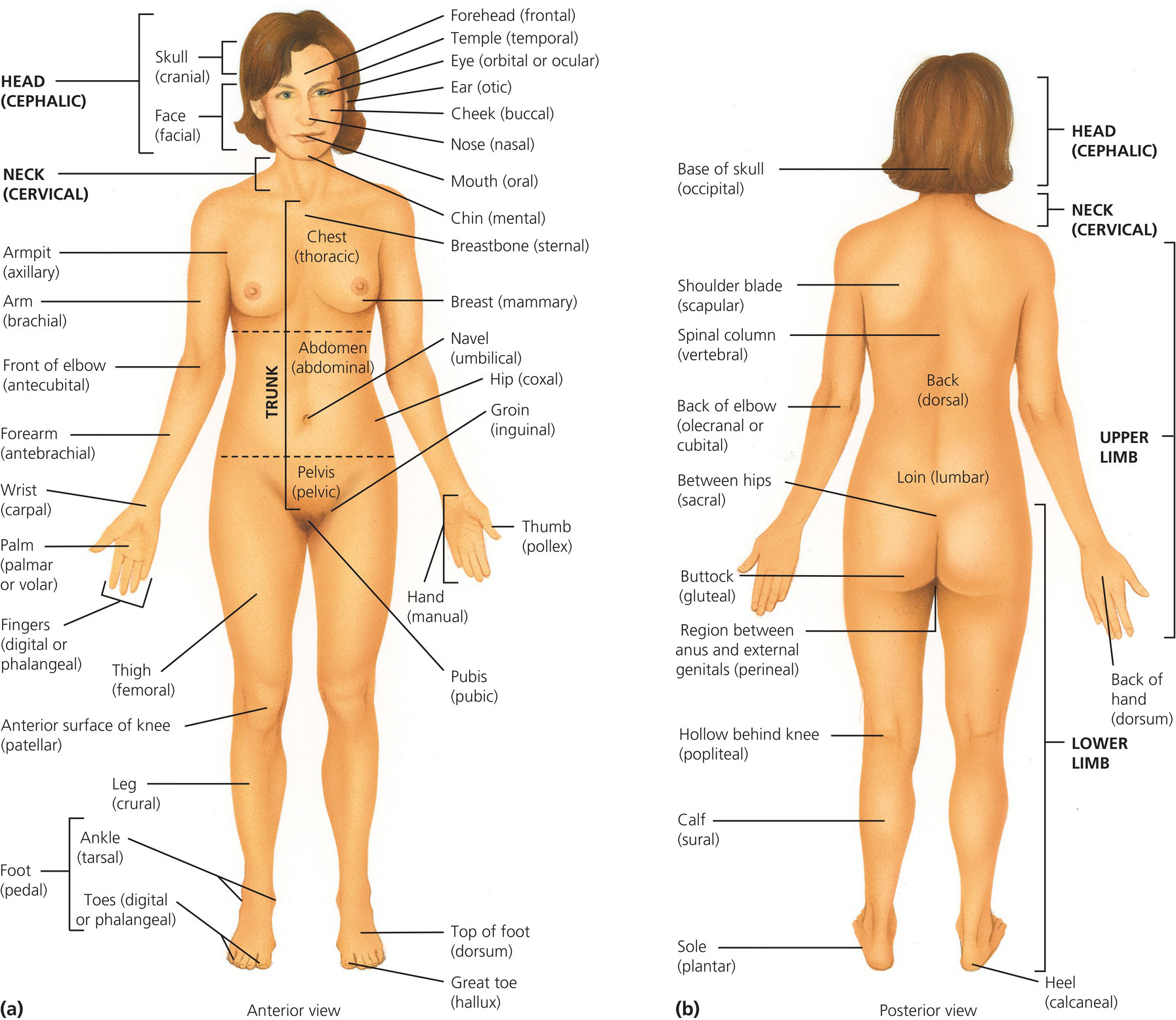
Figure 4.1 Anatomical position. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The skeleton has two distinct sections: The axial skeleton consists of the skull bones, inner ear, ribs, vertebrae and sternum. It provides structural support, attachment points for ligaments and muscles and protection for the brain, spinal cord and major organs of the chest. The appendicular skeleton consists of the pectoral girdle and the upper limbs, pelvic girdle and lower limbs that make movement possible and protect the organs of the pelvis.
Human movement is described in three dimensions (or planes) which divide the human body (Figure 4.2)
- The sagittal (vertical/median) plane – lies vertically through the body dividing it into left and right parts.
- The coronal (frontal) plane – lies vertically through the body dividing it into anterior and posterior parts.
- The transverse (horizontal) plane – lies horizontally through the body dividing it into superior and inferior parts.
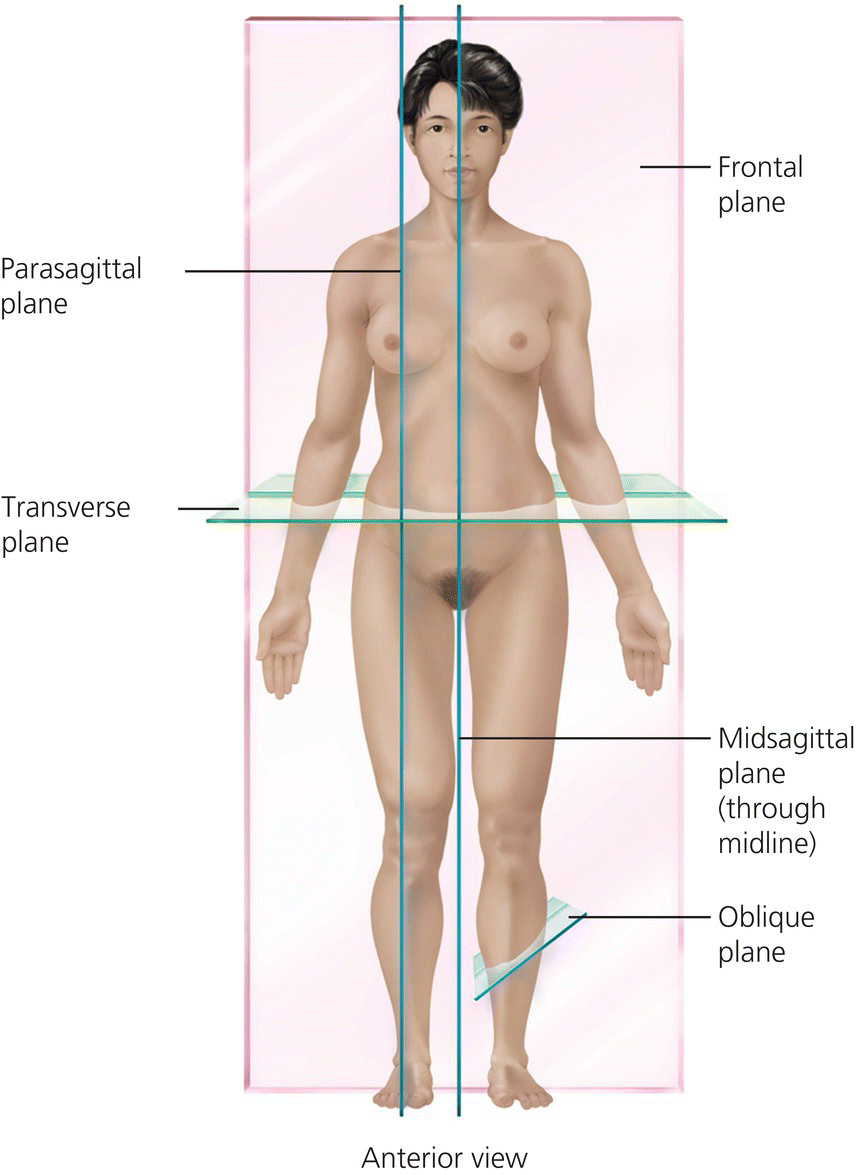
Figure 4.2 Planes of the body. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
Anatomical terminology and movement
Anatomical directions and terminology assists practitioners to use a systematic approach to describing and orientating the human body. Box 4.1 gives the most commonly used terms.
Box 4.1 Common anatomical terms
Movement can be described in a variety of ways depending on where and how the movement occurs. Types of movement are often described in pairs describing opposite movements (See Box 4.2).
The skeleton
The skeleton is made of bone, cartilage and ligaments. These structures work in unison to allow movement. The skeleton is strong, light and flexible, representing about 20% of the total body weight, half of which is water. At birth there are over 300 bones, some of which fuse later. Adults have approximately 206, varying slightly between individuals depending on small bone fusion during growth.
Bones are classified in many ways. Their shape and structure are governed by genetic, metabolic and mechanical factors (see Table 4.1).
Table 4.1 Bone classifications
| Bone | Examples | Features |
| Long bones | Femur, tibia, humerus | Tubular in shape with a central shaft (diaphysis) which contains bone marrow Two extremities (epiphyses) Completely covered (except for joint surfaces) in periosteum The epiphyses contain epiphyseal cartilage/plates near each end of the bone. These are active in growth and ossify when growth is completed in early adulthood |
| Short bones | Found in the wrist and ankle (carpals and tarsals) | Cuboid in shape No shaft Hard outer shell of compact bone Spongy (cancellous) bone in the centre |
| Flat bones | Cranium, scapula, pelvis and ribs | Hard compact bone outer casing with a soft cancellous bone centre Usually curved |
| Irregular bones | Bones of the face, vertebrae | Do not fit in other categories |
| Sesamoid bones | Patella, distal portion of first and second metacarpals, pisiform, first metatarsal | Embedded in tendons |
Bone physiology
Bone is a highly vascular tissue containing intercellular substance surrounding widely separated cells. This dynamic tissue is continuously remodelled and features four characteristic types of cells (see Table 4.2).
Table 4.2 Bone tissue cell types
| Osteoprogenitor (osteogenic) cells |
|
| Osteoblasts |
|
| Osteocytes |
|
| Osteoclasts |
|
Box 4.3 Functions of the skeleton
Bone is made up mainly of collagen and mineral salts; principally calcium phosphate and some calcium carbonate with small amounts of magnesium hydroxide, fluoride and sulphate. These salts are deposited in a framework of collagen fibres which then calcify. Bone is not completely solid, with some spaces between its hard components, providing channels for blood vessels and a lighter structure. Bone tissue can be categorised into compact or cancellous (spongy) depending on the size and distribution of the spaces.
Compact bone surrounds cancellous bone and is thicker in the diaphysis (shaft) than the epiphyses (ends). It provides support and protection and helps long bones resist the stress of weight bearing. Adult compact bone has a concentric ring structure with blood vessels and nerves traversing it from the periosteum through Volkmann’s canals that connect with the blood vessels and nerves of the medullary cavity and the central Haversian canals. The Haversian canals run longitudinally through the bone and are surrounded by rings of hard calcified bone – concentric lamellae between which are spaces called lacunae which contain osteocytes. Canaliculi radiate in all directions from the lacunae, forming an intricate network providing numerous routes for nutrients to reach the osteocytes and for the removal of waste. Each central canal with the surrounding lamellae, lacunae, osteocytes and canaliculi is known as a Haversian system or osteon (see Figure 4.3).
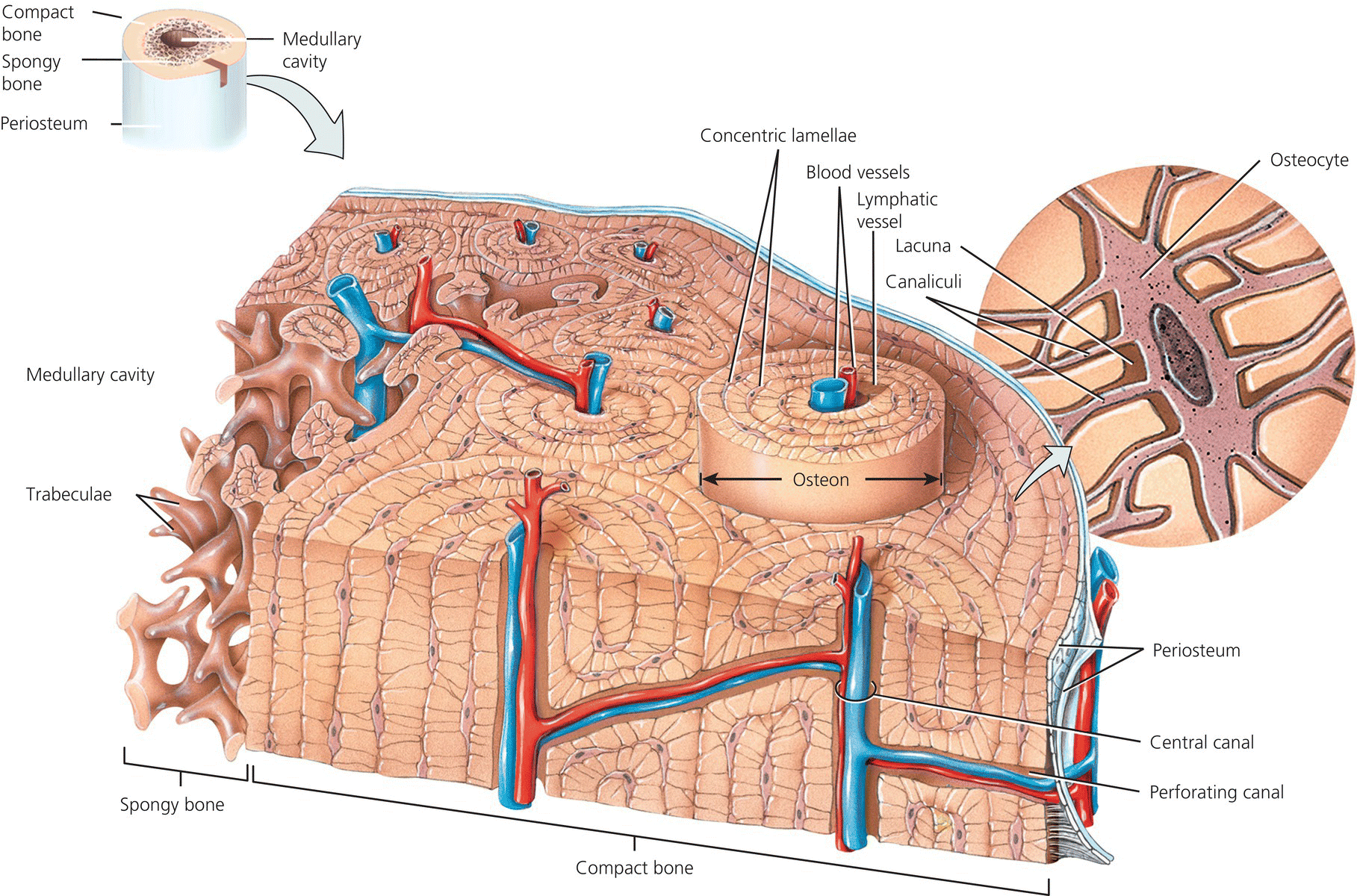
Figure 4.3 Haversian system (osteon). Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
Cancellous (spongy) bone consists of an irregular latticework of thin plates of bone called trabeculae within which lie lacunae containing osteocytes. The spaces between the trabeculae of some bones are filled with red marrow (responsible for red cell production). Blood vessels from the periosteum penetrate through to the cancellous bone.
Bone growth and development
The process of bone formation, ‘ossification’, begins in the embryo in which the ‘skeleton’ at this time is composed of fibrous membranes and hyaline cartilage shaped like bones and providing the medium for ossification. Ossification occurs in two ways:
Intramembranous ossification – osteoblasts cluster in a fibrous membrane forming a centre of ossification and secrete intercellular substances partly composed of collagenous fibres which form a framework around which calcium salts are deposited (calcification). When the cluster of osteoblasts is completely surrounded by the calcified matrix, it is called a trabecula (plural trabeculae). Trabeculae radiate out from each centre of ossification into a framework. The original connective tissue becomes the periosteum and the ossified area becomes cancellous (spongy) bone with a covering of compact bone. Bone is continuously destroyed and reformed until it reaches its final adult size and shape.
Endochondral ossification – the replacement of cartilage by bone. Most bones of the body are formed by this process. Early on in embryonic development a cartilage template of the future bone is laid down and covered by a membrane – the ‘perichondrium’. Midway along the shaft a blood vessel penetrates the perichondrium, stimulating osteoprogenitor cells within the perichondrium to enlarge and become osteoblasts. These cells then form osteocytes which form a periosteal collar of compact bone around the middle of the diaphysis of the cartilage model. This then forms the membranous covering of bone known as the periosteum. At the primary centre of ossification, chondrocytes hypertrophy and the matrix becomes mineralised and spaces in the shaft of the bone join together forming the medullary cavity which then fills with bone marrow. Secondary centres of ossification form at the extremities of long bones in the epiphyses and lay down spongy bone. One secondary ossification centre develops in the proximal epiphysis soon after birth and the other centre develops in the distal epiphysis during a child’s second year. After the two secondary ossification centres have formed, bone tissue completely replaces the cartilage except in two regions: cartilage continues to cover the articular surfaces of the epiphyses as ‘articular cartilage’ as well as in the region between the epiphysis and diaphysis (the ‘epiphyseal plate’) where lengthwise growth of bone continues into early adulthood.
Bones continue to grow in length and width following birth. Appositional growth is the growth in diameter of bone by the formation of new bone on the surface of existing bone. This occurs at the same time as growth in the length of bone. Bone lining the marrow cavity is destroyed by osteoclasts allowing the cavity to increase in size and at the same time osteoblasts from the periosteum produce new compact bone to cover the outer surface of the bone. The growth in length is known as endochondral growth which takes place in the epiphyseal plates until their ossification. The cartilage in the epiphysis is replaced by bone from the shaft side and this is matched by the production of new cartilage from the epiphyseal plate. This process continues until early adulthood when hormones cause the cartilage in the epiphyseal plate to ossify.
Bone growth is influenced by:
- nutrition
- sunlight
- hormones
- exercise.
Bone is constantly remodelling and re-appropriating its matrix and minerals along lines of mechanical stress allowing worn or damaged bone to be removed and replaced with new tissue. Bone also stores calcium and phosphorous. There is a delicate homeostasis maintained between the action of osteoclasts removing calcium and collagen from the bone and osteoblasts depositing calcium and collagen. If too much tissue or calcium is removed, the bones become weakened and break easily, leading to osteoporosis.
There are a number of other hormones involved in the metabolism of bone:
- Vitamin D (calcitriol) – regulates calcium and phosphorous levels and the mineralisation of bone.
- Calcitonin – inhibits the action of osteoclasts thus inhibiting the removal of calcium from bone.
- Parathyroid hormone – increases the number and activity of the osteoclasts which release calcium and phosphate from bones into blood.
- Oestrogens – inhibit the activity of osteoclasts, protecting the bones from excessive bone turnover.
- Human growth hormone – responsible for the general growth of bones at the epiphyseal plates.
Skeletal muscle
Skeletal muscle appears striated (striped) and has the fastest contraction rate under voluntary control of all muscles. It is controlled by the central and autonomic nervous system and provides force and power for movement. Muscles contract and relax to bring about movement and perform three main functions:
- movement (voluntary and reflex) – through the actions of bones, joints and the skeletal muscles attached to the bones
- maintenance of posture – through the contraction of muscles to support the body in a stationary position
- heat production – contraction produces most of the body’s heat.
Skeletal muscles are composed of collections of striated muscle fibres and some connective tissues such as blood vessels and nerves. Deep fascia is a dense connective tissue that lines the body wall and extremities as well as holding muscles together and separating them into functioning groups. The entire muscle is wrapped with a fibrous connective tissue called the epimysium. Bundles of muscle fibres called fasciculi are covered by fibrous connective tissue known as perimysium and endomysium – fibrous connective tissue that penetrates into the interior of each fascicle and surrounds and separates the muscle fibres. Individual muscle fibres are long and cylindrical structures with multiple nuclei and their length and width varies depending on the function and purpose of each muscle. Each muscle fibre contains thousands of microscopic contractile units known as myofibrils that bring about contraction following electrical stimulation in a complex process of sliding filaments within the myofibrils.
Muscles are named according to their shape, location, or a combination of both and according to function e.g. flexion, extension, or rotation.
Skeletal muscle attachment
Skeletal muscles produce movement by exerting force on tendons which in turn pull on bones. When a muscle contracts it draws one articulating bone towards the other. The attachment of a muscle tendon to the stationary bone is called the origin. The attachment of the other muscle tendon to the moveable bone is known as the insertion. Levers are created by the bones and joints. Tendons attach muscles to the bone and act on the skeleton by contracting and shortening or relaxing to allow two bones to move closer or move away.
Ligaments, tendons and cartilage
Ligaments, tendons and cartilage connect bones, joints and muscles and guide and protect movement that has been initiated by muscles.
Ligaments and tendons are formed from regularly arranged dense connective tissue with strong parallel fibres that attach muscles to bone. Aponeoroses are the flattened sheet-like tendons which connect muscle to bone or muscle to muscle. Large fibrous sacs known as bursae protect some tendons such as those at the hip, knee and elbow. Ligament elasticity allows stretch. They stabilise the joint to ensure movement remains within its normal planes.
Dense irregular connective tissue forms cartilage. Fibres are arranged irregularly, allowing them to endure more stress than ligaments and tendons. There is no blood or nerve supply and minimal ability for healing. There are two types of cartilage that relate to the skeletal system:
- hyaline cartilage – the most abundant type found at joints over the ends of the long bones as ‘articular cartilage’. It provides flexibility and support, absorbs shock and reduces friction.
- fibrocartilage – allows greater resistance to compression and tension due to its fibrous structure. It can be found at the symphysis pubis, the intervertebral discs between vertebrae and the menisci of the knee.
Neurovascular supply
Bone has a rich nerve and blood supply, supplying the nutrients for bone growth and muscle contraction and supporting biofeedback systems.
Bone has a rich blood supply from which it acquires nutrients required for growth, remodelling and repair. Large nutrient arteries enter bones through holes known as nutrient foramen into the diaphysis of the bone and then divide into the proximal and distal branches and supply the head of the bone. Blood vessels and capillaries divide from the nutrient artery and enter the central/Haversian canals to supply the compact bone. Perforating canals within the compact bone allow entry of the capillaries into the cancellous bone, supplying the nutrients required for bone cell and bone marrow activity. The central canal of long bones and central area of flat bones contain red marrow (haematopoietic tissue) which is responsible for the production of red blood cells.
Nerves are prolific throughout bone, allowing communication with the central nervous system and providing feedback as well as being responsible for some of the pain felt when there is bone disease or injury. Blood vessels and nerves run side by side and are most prolific in the ends of long bones where they provide autonomic feedback/proprioception from the joints.
Joints
Bones are held together at joints by flexible connective tissue where all movement takes place. The structure of the joint determines how it functions. Some joints permit no movement, whilst others permit slight or considerable movement. The structural classification of joints is based on whether there is a synovial cavity and the type of connective tissue that binds the bones together. Structurally joints are classified as:
- Fibrous Joints – lack a synovial cavity and the articulating bones fit very closely together. There is little or no movement. There are three types:
- Suture – between the bones of the skull. The bones are united by a thin layer of dense fibrous connective tissue. The irregular structure of sutures gives added strength and decreases the chance of fracture. Some sutures present during growth are replaced by bone in the adult and these are called synostoses.
- Syndesmosis – is a fibrous joint where the fibrous connective tissue is present in a greater amount than in a suture but the fit between the bones is not quite as tight. The fibrous connective tissue forms an interosseous membrane or ligament. The syndesmosis is slightly moveable because the bones are separated more than in a suture and some flexibility is permitted by the interosseous membrane e.g. the talo-fibular joint.
- Gomphosis – a type of fibrous joint where a cone-shaped peg fits into a socket e.g. the articulation of the roots of teeth with the sockets.
- Cartilagenous Joints – have no synovial cavity and articulating bones are tightly connected by cartilage, allowing little or no movement. There are two types:
- Synchondrosis – the connecting tissue is hyaline cartilage. The commonest type is the epiphyseal plate found between the epiphysis and diaphysis of a growing bone. The joint is eventually replaced by bone when growth ceases – synostosis e.g. the joint between the first rib and the sternum.
- Symphysis – a cartilaginous joint in which the connecting material is a broad flat disc of fibrocartilage e.g. between the bodies of the vertebrae and the symphysis pubis. These joints are slightly moveable – amphiarthrotic.
- Synchondrosis – the connecting tissue is hyaline cartilage. The commonest type is the epiphyseal plate found between the epiphysis and diaphysis of a growing bone. The joint is eventually replaced by bone when growth ceases – synostosis e.g. the joint between the first rib and the sternum.
- Synovial Joints – the most common joints have a space known as the synovial cavity between the articulating bones and are freely moveable. Synovial joints have five main features:
- Joint cavity – the space between articulating bones which provides the space for movement.
- Articular cartilage – covers the surfaces of the articulating bones and is formed of hyaline cartilage. Prevents friction and absorbs shock.
- Articular capsule – synovial joints are surrounded by a sleeve-like structure enclosing the synovial cavity and uniting the articulating bones. It is composed of two layers – the fibrous capsule and the synovial membrane. The fibrous capsule consists of dense connective tissue and is attached to the periosteum at a variable distance from the edge of the articular cartilage. The flexibility of the fibrous capsule allows for movement at the joint while its tensile strength resists dislocation.
- Synovial membrane – the inner layer of the articular capsule and covers all surfaces of the joint not already covered by articular cartilage. It is composed of loose connective tissue and secretes synovial fluid.
- Synovial fluid – secreted by the synovial membrane, fills the joint cavity, lubricates the joint, provides nourishment for the articular cartilage, reduces friction, supplies nutrients and removes metabolic wastes from the cells of the articular cartilage. Synovial fluid contains phagocytic cells that remove microbes and debris from wear and tear in the joint.
Synovial joints are further classified by their movement and the structures of the articulating bones:
- Hinge joint – the convex surface of one bone fits into the concave surface of another bone. The movement is in a single plane and is similar to that of a hinged door e.g. hinge joints are the knee, elbow and interphalangeal joints where the movement allowed is flexion and extension.
- Ball and Socket Joint – a ball-like surface of one bone fitted into a cuplike depression of another bone, allowing movement in three planes: flexion/extension, abduction/adduction and rotation/circumduction e.g. the shoulder joint and hip joint. The stability of the joint depends on how deep the socket is and the fit of the ball within the socket.
- Plane joint (gliding) – the articulating surfaces glide against each other in one plane only and are usually flat, allowing only limited movement e.g. the joints between the carpal bones, tarsal bones and the sternum and clavicle.
- Pivot joint – the conical surface of one bone articulates within a ring formed partly by another bone and a ligament, allowing rotation e.g. the joint between the atlas and axis allowing rotation of the head.
- Condyloid joint – an oval shaped condyle of one bone fits into an elliptical cavity of another bone, allowing side to side and back and forth movements and allowing flexion/extension, abduction/adduction and circumduction e.g. the joint at the wrist between the radius and carpals.
- Saddle joint – the articular surface of one bone is saddle shaped and the other articular surface is shaped like a rider sitting in the saddle – a modified condyloid joint with freer movement. Movements are side to side and back and forth e.g. the joint between the trapezium and the metacarpal of the thumb. Figure 4.4 illustrates the different types of synovial joints.
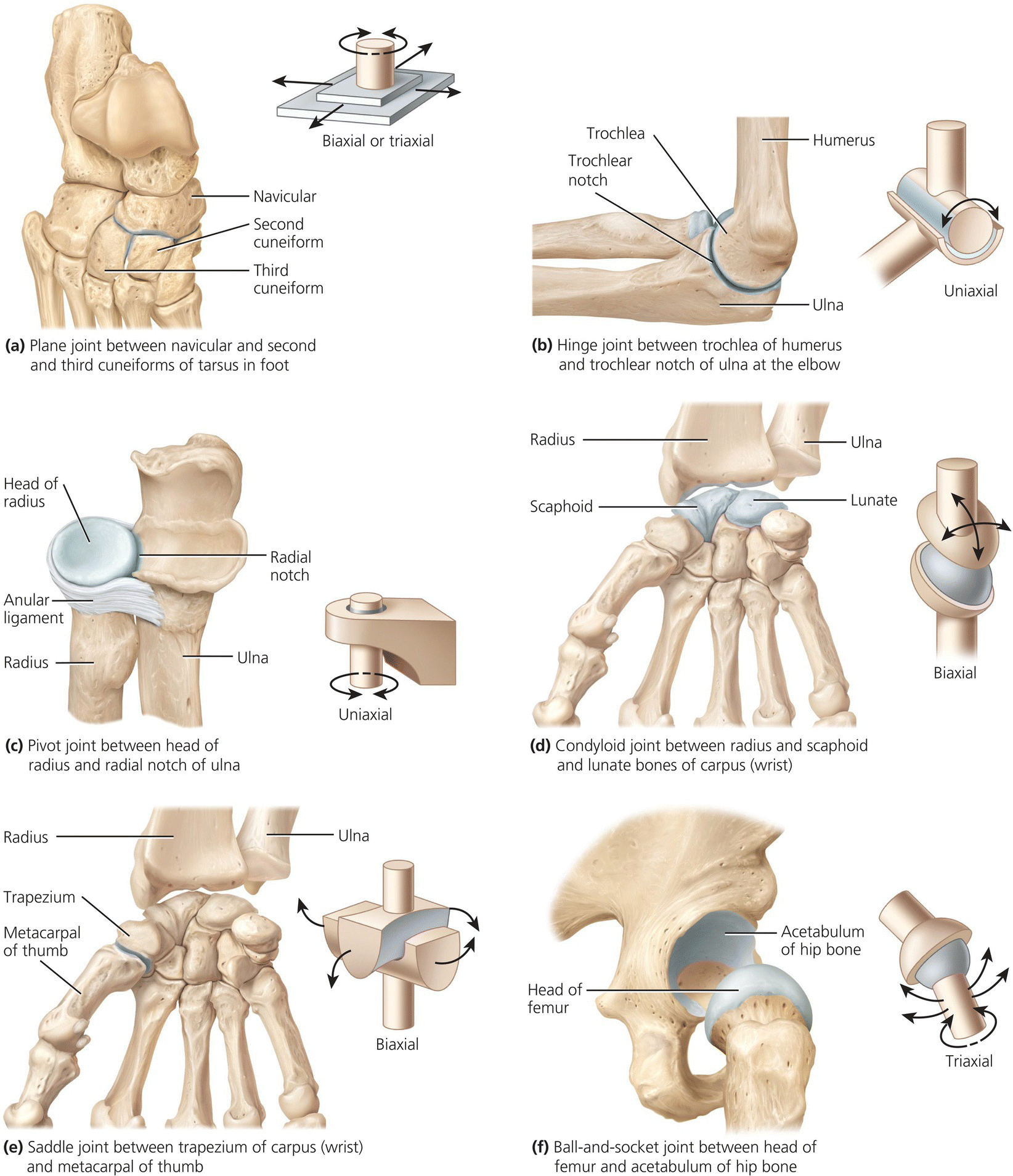
Figure 4.4 Types of synovial joint. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The cranium (the skull)
The bony skeleton of the head (cranium) supports the structure of the face and forms a cavity for the brain. It is thin, light and solid and is usually described via the eight bones that make it up (Table 4.3), sometimes referred to as the neurocranium. The inner surfaces attach to membranes that position and stabilise the brain, blood vessels and nerves. The outer surfaces act as an attachment for muscles so the head can move in various ways.
Table 4.3 The function of the bones of the skull
| Bones | Function |
| Frontal | Situated at the front of the head forming the forehead, the roof of the eye sockets and nasal cavity as well as the base of the anterior of the skull. |
| Occipital | Situated at the rear of the skull just above the nape of the neck. It has a hole at the base which is the channel of the spinal cord between skull and the spinal column. The occipital bone is connected to the top two vertebrae (atlas and axis) allowing the head to move freely. |
| Sphenoid | A wing shaped bone situated at the base of the skull in front of the temporal bones. It is the only bone that articulates with the other seven bones of the skull. It spans the skull laterally and helps form the base of the cranium, the sides of the skull, and the floors and sides of the eye sockets. The central body has two sinuses within it which lie side by side and are separated by a bony septum that projects downward into the nasal cavity, and channels for the optic nerve and other nerves. |
| Ethmoid | Separates the nasal cavity from the brain. It is spongy and light, can be easily damaged and is situated between the eye sockets at the roof of the nose. The external walls contain small sinuses. |
| Temporal x 2 | Found on each side of the skull and form part of the sides and the base. Each is divided anatomically into four parts: the mastoid, petrous, squamous, and tympanic parts. It is closely involved in the anatomy of the ear. They also form a projection from the cheekbone to the eye (the zygoma). |
| Parietal x 2 | Two of the largest bones of the skull and form the sides and roof. In the front each parietal bone adjoins the frontal bone; in the back, the occipital bone; and below, the temporal and sphenoid bones. |
The cranium is proportionally more developed at birth and grows more quickly during the first years of life than the rest of the skeleton. To allow flexion so that childbirth can take place, the bones of the cranium at birth are connected by non-ossified membranous regions (fontanelles). Ossification closes the fontanelles by a child’s second birthday. Where the bones meet they become connected to each other by immobile solid fibrous articulations called cranial sutures.
The cranium has four main functions:
- protection of the brain
- contains and supports the eyes and the face
- fixes the distance between the eyes to allow stereoscopic vision
- the ears are fixed into position to help the brain use auditory cues to judge direction and distance of sounds.
There are fourteen facial bones which hold the eyes in place and form the facial features. The face is sometimes referred to as the splanchnocranium and makes the cranium into the skull. These bones meet with the cranial bones to give each face unique individual form.
The hyoid bone is one further bone – it stands alone and is located in the neck below the tongue. It is held in place by ligaments and muscles of the styloid process of the temporal bone.
The spine
The vertebral column, (the ‘backbone’ or spine) extends from the base of the skull to the pelvis and has five distinct regions:
- Cervical spine (7 vertebrae) – the neck, supports the head and allows for nodding and shaking the head
- Thoracic spine (12 vertebrae) – attaches the ribs
- Lumbar spine (5 vertebrae) – forms the lower back, carrying most of the weight of the upper body and providing a stable centre of gravity
- Sacrum (5 fused vertebrae) – makes up the posterior wall of the pelvis
- Coccyx (4 small fused bones) – at the base of the spine.
The spine provides strong flexible support for the head and body and keeps the trunk straight whilst allowing the torso to move. It protects the spinal cord and acts as an attachment point for the ribs, the pelvic girdle and the muscles of the back. The strength and mobility of the spine is enhanced by four curves of the spine, two concave at the cervical and lumbar levels (lordosis/lordoses) and two convex at the dorsal and sacral areas (kyphosis/kyphoses). Figure 4.5 shows the overall structure of the spine.
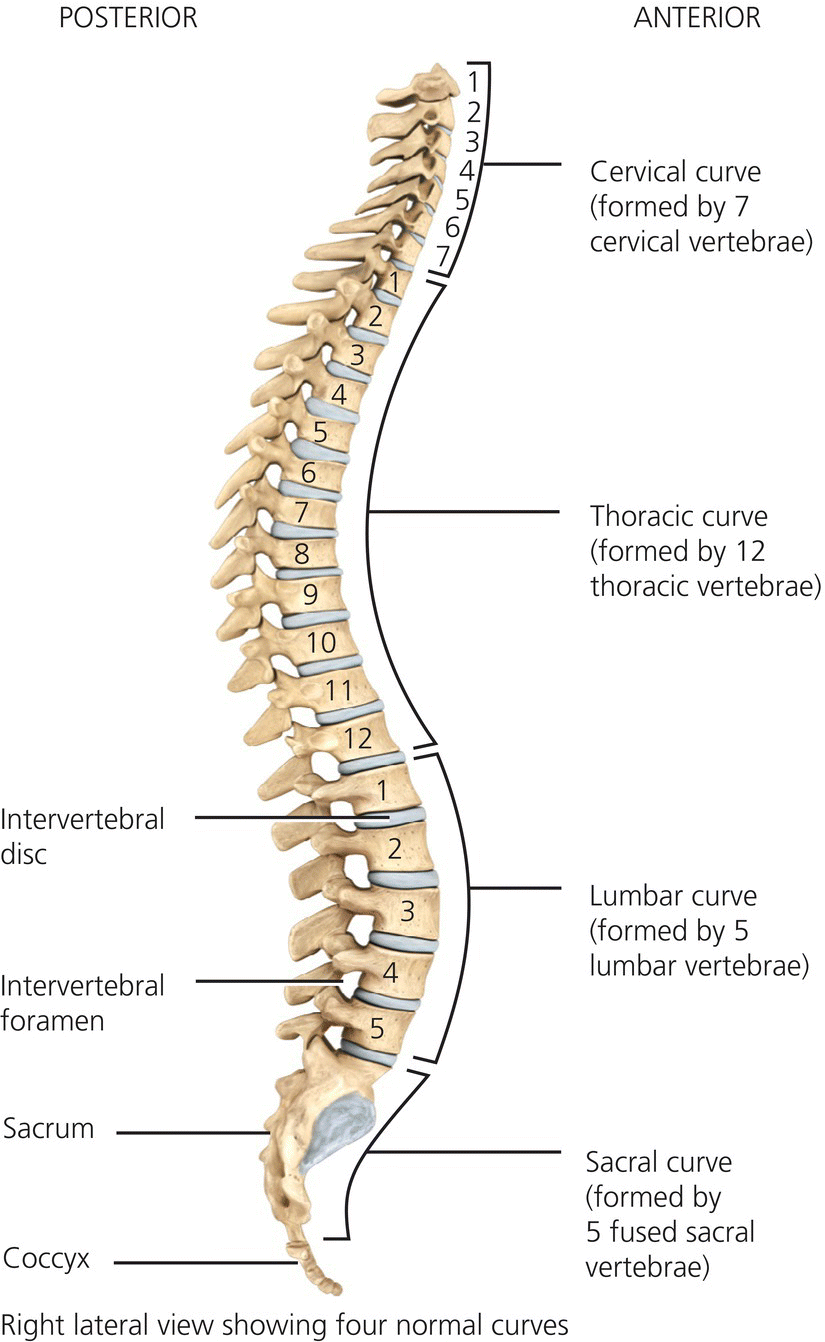
Figure 4.5 The spine. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The main functions of the spine are:
- protection of the spinal cord and nerve roots
- supports and balances the body in an upright position with the help of surrounding muscles and ligaments
- attachment for the ribs, pelvic girdle, muscles, ligaments and tendons
- mobility of the vertebrae and the intervertebral discs allow mobility in the trunk of the body.
The vertebrae
The vertebrae are named by using the initial of the area concerned i.e. C = cervical, D (or T) = dorsal (or thoracic) etc. and the number according to the vertebra’s position in the spine i.e. C3 is the third cervical vertebra. Figure 4.6 illustrates the structure of a typical vertebra. The basic structure is the same at all levels and consists of:
- A vertebral body which is the thickest and loadbearing part of the vertebrae. Rough surfaces provide excellent adhesion for the intervertebral discs. It also contains two foramina that allow blood vessels to pass through.
- A vertebral arch – composed of two thick projections (vertebral pedicles) and two flat sections of bone (vertebral laminae) and completed by the vertebral body. This forms the vertebral foramen that encloses the spinal cord. Once the vertebrae are stacked on each other the vertebral foramen form the vertebral canal. The stacked pedicles create a gap on each side, each allowing for the passage of a spinal nerve.
- Seven processes commence from the vertebral arch – two transverse, four articular and one spinous process. The four articular processes are covered in hyaline cartilage and articulate with the vertebrae above and below.
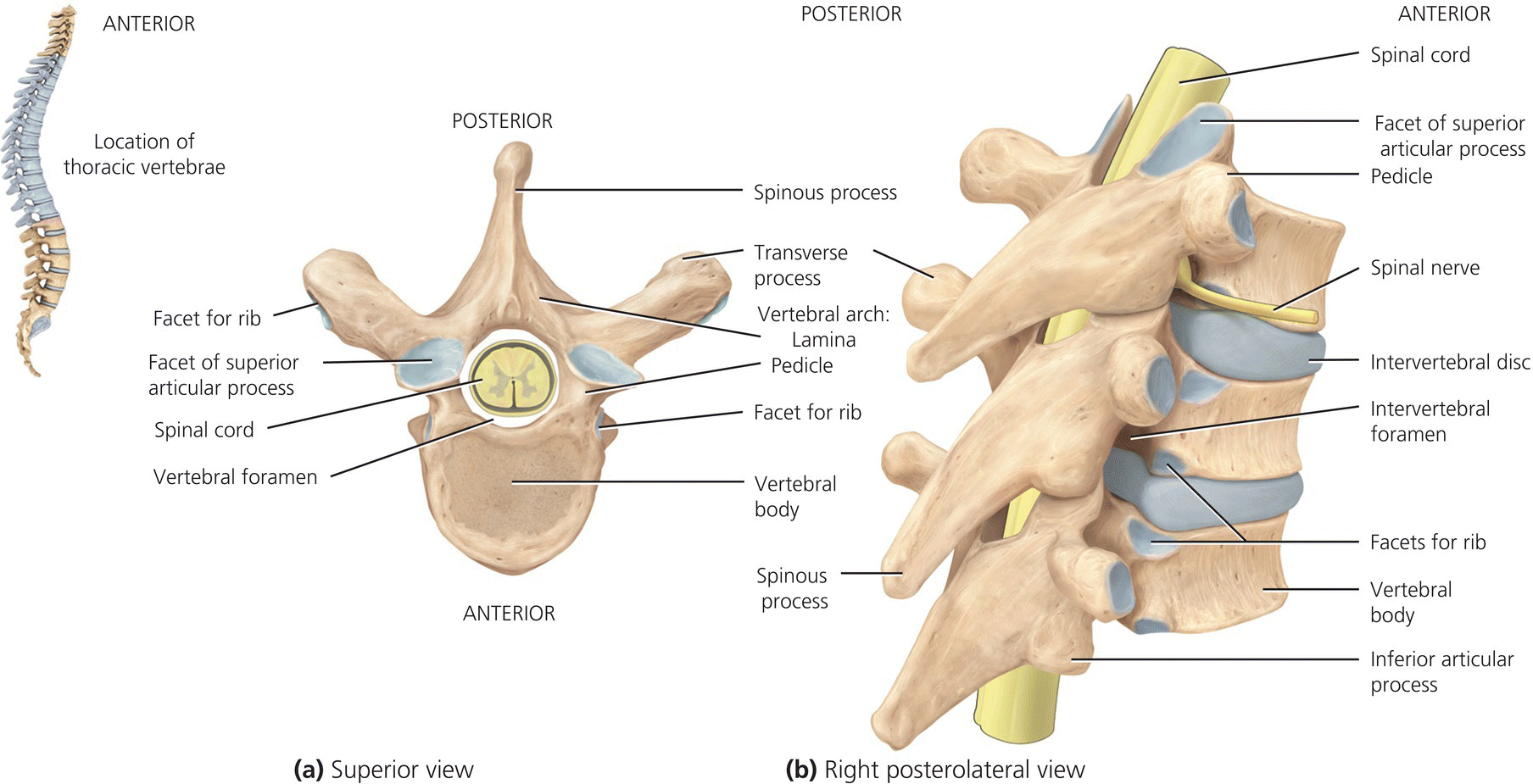
Figure 4.6 Structure of a typical vertebrae (illustrated by a thoracic vertebra). Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The vertebrae are different depending on the level of the spine they correspond to (see Table 4.4); however, two vertebrae are unique – C1 and C2.
- C1 (atlas) – supports the head and is a ring of bone with two transverse processes and has articular facets on its upper side that are concave and articulate with the occipital condyles allowing the head to move up and down. On the lower surfaces it articulates with the second vertebra.
- C2 (the axis) – has a characteristic protrusion on the upper surface known as the dens. This serves as a pivot for the rotation of the atlas and the head allowing it to rotate from side to side.
Table 4.4 The characteristics of vertebrae
| Vertebral position | Size and structure | Characteristics |
| Cervical (C1–C7) | Smaller than other vertebrae but with wider arches |
|
| Thoracic ( T1–T12) | Large and robust except for T11, T12, T1 and T2 they have longer transverse processes. |
|
| Lumbar (L1–L5) | Largest and most robust vertebrae with short thick processes. |
|
| Sacrum | 5 fused vertebrae |
|
| Coccyx | 4 fused vertebrae |
|
Soft tissues of the spine
Intervertebral discs have two functions:
- to attach the vertebrae to one another
- to absorb and dampen shock to the spine.
All the vertebrae are separated by the intervertebral discs except for C1 and C2 and the coccyx. These are made of varying thickness of cartilage – the thickest in the lumbar vertebrae which take the most stress.
The annulus fibrosus of the disc is a strong outer structure made up of concentric sheets of collagen fibres connected to the vertebral end plates. This encloses the nucleus pulposus. The nucleus pulposus contains a gel-like matter full of water that resists compression; the amount of water in the nucleus varies throughout the day depending on activity (see Figure 4.7).
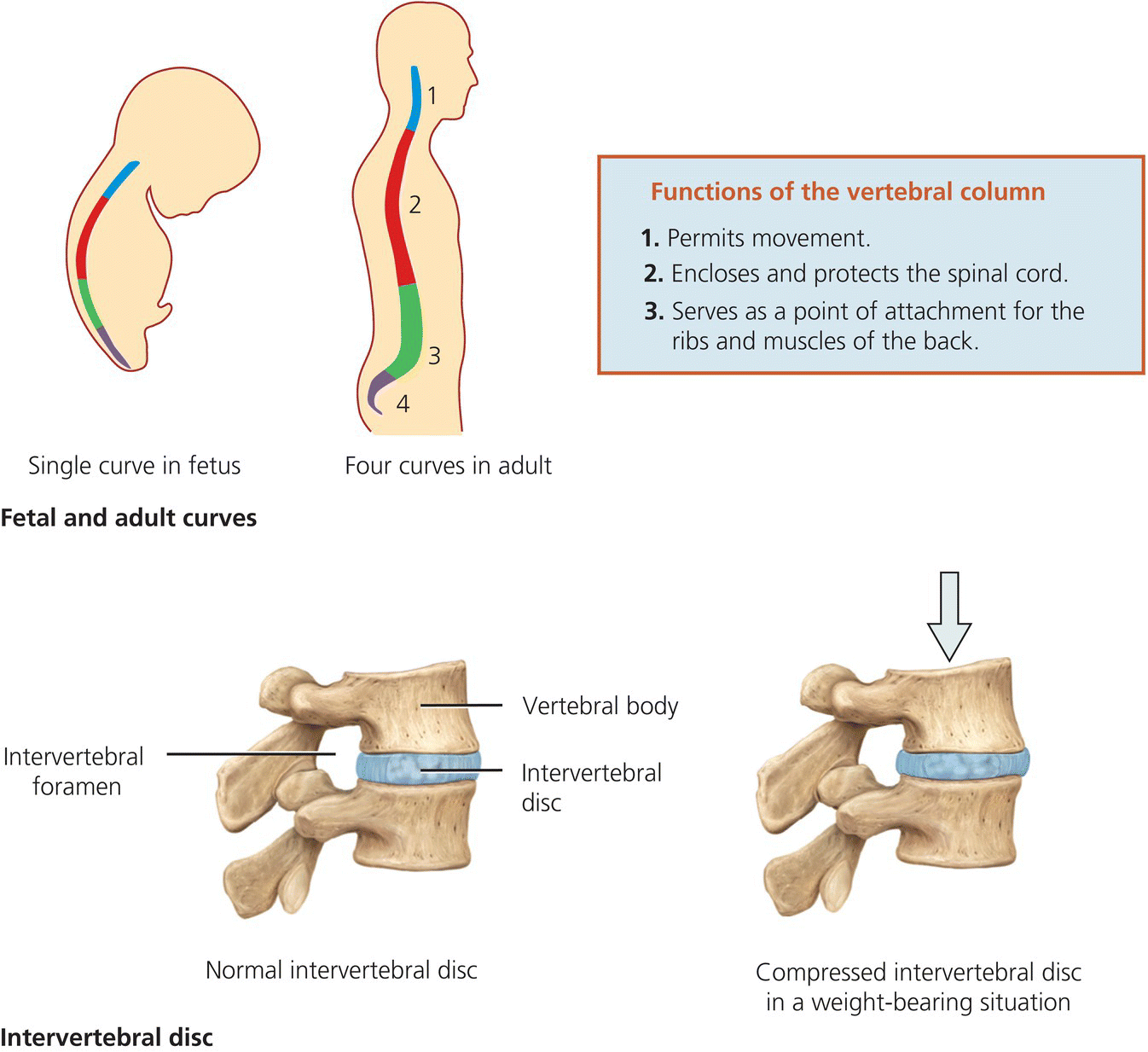
Figure 4.7 Intervertebral discs. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The ligaments of the spine (listed in Table 4.5) connect bone to bone and are fibrous connective tissues made up of densely packed collagen fibres. These help to provide structural stability and a natural brace along with the tendons and muscles which help to protect the spine from injury. There are two primary ligament systems in the spine. The intrasegmental system includes the ligamentum flavum, interspinous and intertransverse ligaments. This holds many vertebrae together. The intersegmental system includes the anterior and posterior longitudinal ligaments, and the supraspinous ligaments.
Table 4.5 The ligaments of the spine
| Ligament Name | System | Description |
| Anterior longitudinal ligament | Intersegmental system |
|
| Posterior longitudinal ligament | Intersegmental system |
|
| Supraspinous ligament | Intrasegmental system |
|
| Interspinous ligament | Intrasegmental system |
|
| Ligamentum flavum | Intrasegmental system |
|
The primary function of the complex muscle and tendon system of the spine is to support and stabilise the structure. Specific muscles are associated with movement of parts of the anatomy and have very important roles. For example, the sternocleidomastoid muscle (neck area) assists with movement of the head, while the spinalis thoracis is associated with extension of the vertebral column.
The spinal cord and spinal/vertebral nerves
The spinal cord consists of millions of nerve fibres which transmit electrical information to and from the brain to the limbs, trunk and organs of the body. The spinal cord descends through the vertebral foramen of each vertebra down to the cauda equina. The brain and the spinal cord are surrounded by the meninges which have three distinct layers:
- the dura mater – strong connective grey outer layer
- the arachnoid mater – a thinner layer resembling a loosely woven fabric of arteries and veins
- the pia mater – a delicate inner layer of highly vascular membrane providing blood to the neural structures.
The space between the arachnoid mater and pia mater (subarachnoid space) is filled with cerebrospinal fluid (CSF) – a clear fluid found in the ventricles, spinal canal and spinal cord that is secreted from a vascular part of the ventricles in the brain, the choroid plexus. This acts as a shock absorber to protect against injury and contains different electrolytes, proteins and glucose.
The communication system from the spinal cord is via spinal nerves which link to the peripheral nervous system which branch off and pass out from the cord through the foramen of the vertebra. Figure 4.8 shows the spinal cord and spinal nerves. There are four main groups of spinal nerves, which exit different levels of the spinal cord:
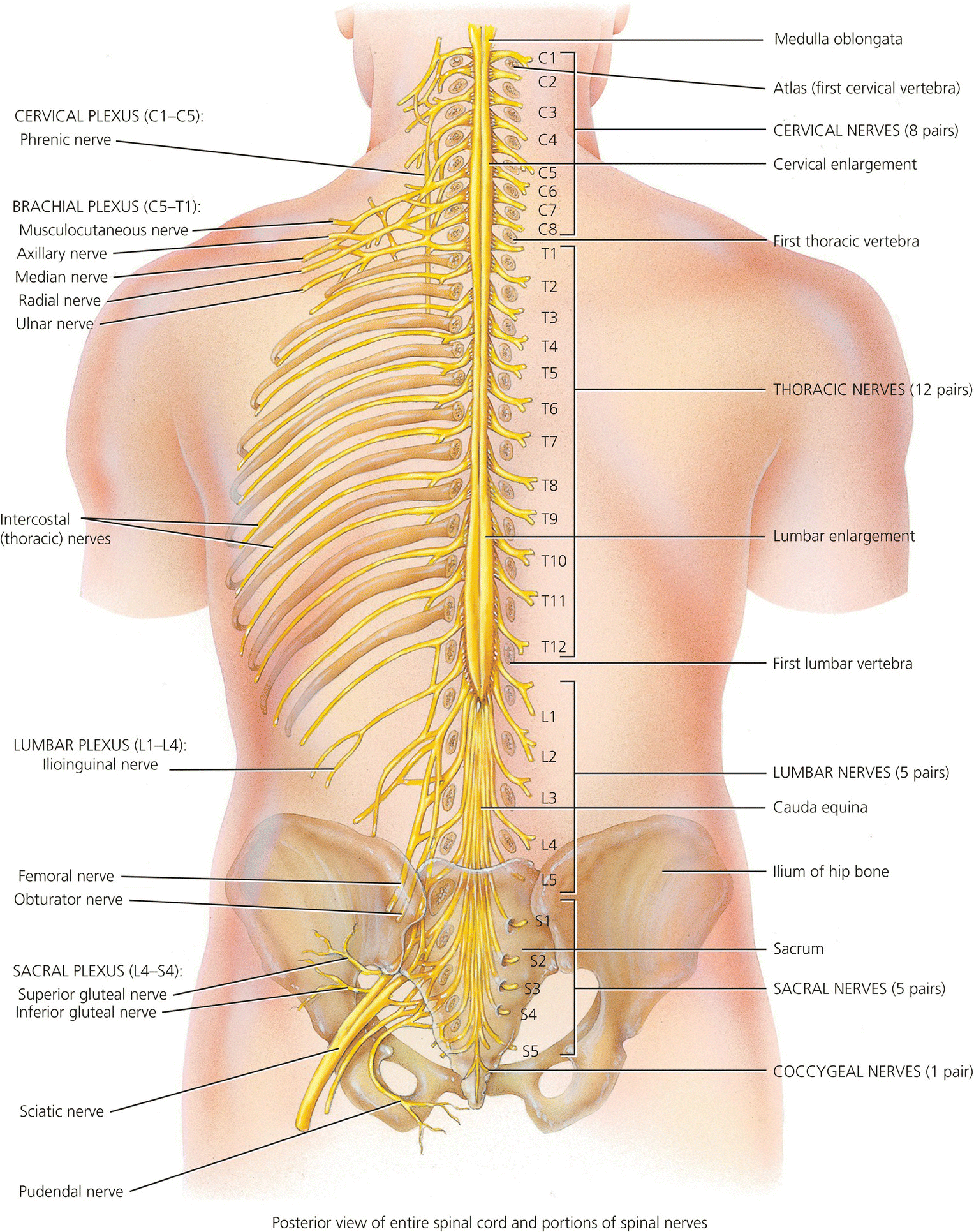
Figure 4.8 Spinal cord and spinal nerves. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
- cervical nerves – supply movement and feeling to the arms, neck and upper trunk and control breathing
- thoracic nerves – supply the trunk and abdomen
- lumbar and sacral nerves – supply the legs, bladder, bowel and sexual organs.
The spinal nerves carry information to and from different levels (segments) in the spinal cord. Both the nerves and the segments in the spinal cord are numbered in a similar way to the vertebrae e.g. T3. There are 31 pairs of spinal nerves, in the cervical region of the spinal cord. The spinal nerves exit above the vertebrae. However, this changes below the C7 vertebra where there is an 8th cervical spinal nerve although there is no 8th cervical vertebra. From the 1st thoracic vertebra all spinal nerves exit below their equivalent numbered vertebrae.
The upper limb
The pectoral or shoulder girdle attaches the bones of the upper limb to the axial skeleton. Each of the two pectoral girdles consists of a clavicle (collar bone) and a scapula (shoulder blade). The anterior component is the clavicle which articulates with the sternum at the sternoclavicular joint. The posterior component is the scapula which articulates with the clavicle at the acromion process and the humerus at the glenoid cavity. The scapula is a flat, triangular bone which lies over the ribs at the back of the rib cage and is held within a complex group of muscle attachments. The pectoral girdles do not articulate with the vertebral column.
The clavicle (collarbone) is a long slender bone with a double curve that lies horizontally in the superior anterior part of the thorax. The medial end articulates with the sternum at the sternoclavicular joint and the lateral end articulates with the acromion of the scapula at the acromioclavicular joint. The clavicle transmits forces from the upper limb to the trunk of the body.
The Scapula (shoulder blade) is a large triangular flat bone which sits posteriorly over the thoracic cage between the levels of the second and seventh rib. A sharp spine runs diagonally across the posterior surface and ends at a flattened projection known as the acromion which articulates with the clavicle at the acromioclavicular joint and can easily be felt as the high point of the shoulder. Below the acromion, the glenoid cavity articulates with the humerus to form the shoulder joint. Figure 4.9 shows the right upper limb.
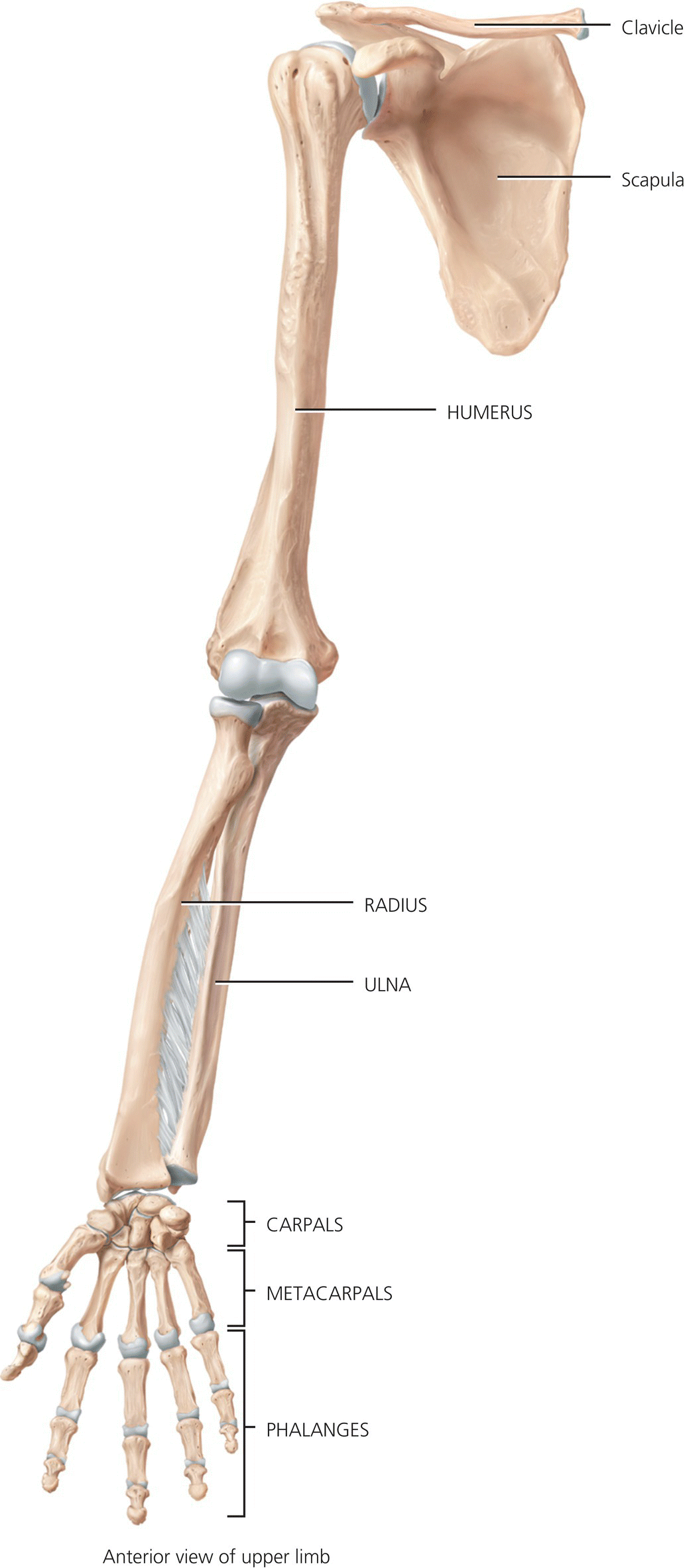
Figure 4.9 Right upper limb. Kuntzman, A.J. and Tortora, G.J. Anatomy and physiology for the manual therapies. 2010, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The ball and socket joint of the shoulder (glenohumeral joint) is freely moveable in many directions but is relatively unstable because the glenoid cavity is very shallow. The rim is slightly deepened by cartilage but has little effect on the stability of the joint. A number of ligaments and tendons help to secure the humeral head in the joint cavity along with the series of four tendons (subscapularis, supraspinatus, infraspinatus and teres minor) which make up the rotator cuff.
The humerus is the longest and largest bone of the upper limb. The proximal end consists of a head that articulates with the glenoid cavity. It has an anatomical neck just distal to the head. The neck of the humerus is a constricted area just distal to the greater and lesser tubercles and is liable to fracture. The shaft of the humerus is cylindrical but gradually becomes flattened and triangular at its distal end.
The elbow is a synovial hinge joint which allows flexion and extension and is important to the flexibility and function of the upper limb. Supination and pronation of the forearm take place at the proximal radioulnar joint contained within the elbow joint capsule. The distal end of the humerus articulates with the proximal end of the ulna and radius. At the distal end of the humerus:
- The capitulum is a rounded knob that articulates with the head of the radius.
- The radial fossa is a depression which receives the head of the radius when the elbow is flexed.
- The trochlea is the surface that articulates with the ulna.
- An anterior depression known as the coronoid fossa receives the ulna head when the forearm is flexed.
- The olecranon fossa is a posterior depression that receives the olecranon of the ulna when the elbow is extended.
Most of the muscles of the forearm are attached to the distal end of the humerus at the medial and lateral epicondyles and the ulnar nerve lies on the posterior surface of the medial epicondyle.
The radius is the lateral bone of the forearm situated on the thumb side and the ulna is the medial bone of the forearm situated on the little finger side. The head of the radius articulates with the capitulum of the humerus and the radial notch of the ulna. The shaft of the radius widens at its distal end and articulates with two of the wrist bones – lunate and scaphoid. At the proximal end of the ulna the olecranon process forms the point of the elbow. The elbow is stabilised by ligaments which prevent rotation and provide stability and strength.
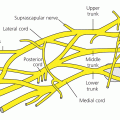
The wrist and hand are capable of very fine, flexible movements. The wrist consists of eight small bones – the carpals, in two transverse rows with four bones in each row, united by ligaments. The proximal row of carpal bones (from lateral to medial) are the scaphoid, lunate, triquetrum and pisiform. The distal row (from lateral to medial) are the trapezium, trapezoid, capitate and hamate. A passageway on the palmar side of the carpal bones known as the carpal tunnel provides a conduit through which the median nerve and flexor tendons of the hand pass. The nerve supply to the arm and hand, with specific reference to the brachial plexus is considered in some detail in Chapter 20.
The metacarpals which form the palm of the hand each consist of a proximal base which articulates with the distal row of carpal bones, a shaft and a distal head which articulate with the proximal phalanges of the fingers. The metacarpal bones are numbered 1 to 5. The phalanges are the bones of the fingers and there are 14 in each hand – 2 in the pollex (thumb) and 3 in each of the remaining four fingers. A single bone of the finger is referred to as a phalanx. The articulations between the metacarpal bones and the phalanges are referred to as the metacarpophalangeal (MCP) joints which flex and extend the fingers and thumb. The two joints in the fingers are known as the interphalangeal joints – the joint closest to the MCP joint is referred to as the proximal interphalangeal joint (PIP) and the joint near the end of the finger is called the distal interphalangeal joint (DIP). The thumb has only one interphalangeal joint.
The pelvis
The pelvis is a bowl-shaped ring of bones that transmits weight from the spine through the legs. Its two (right and left) innominate bones are made up of three bones – the ilium, ischium and pubis – which fuse together at puberty. The pelvic girdle consists of the innominate bones connected at the pubic symphysis anteriorly and the sacrum posteriorly at the sacroiliac joint to form the highly stable but immobile pelvic ring (see Figure 4.10). The pelvic cavity contains the reproductive organs, bladder and rectum. The female pelvis is wider and shallower than the male to facilitate childbirth. The functions of the pelvis are summarised in Box 4.4
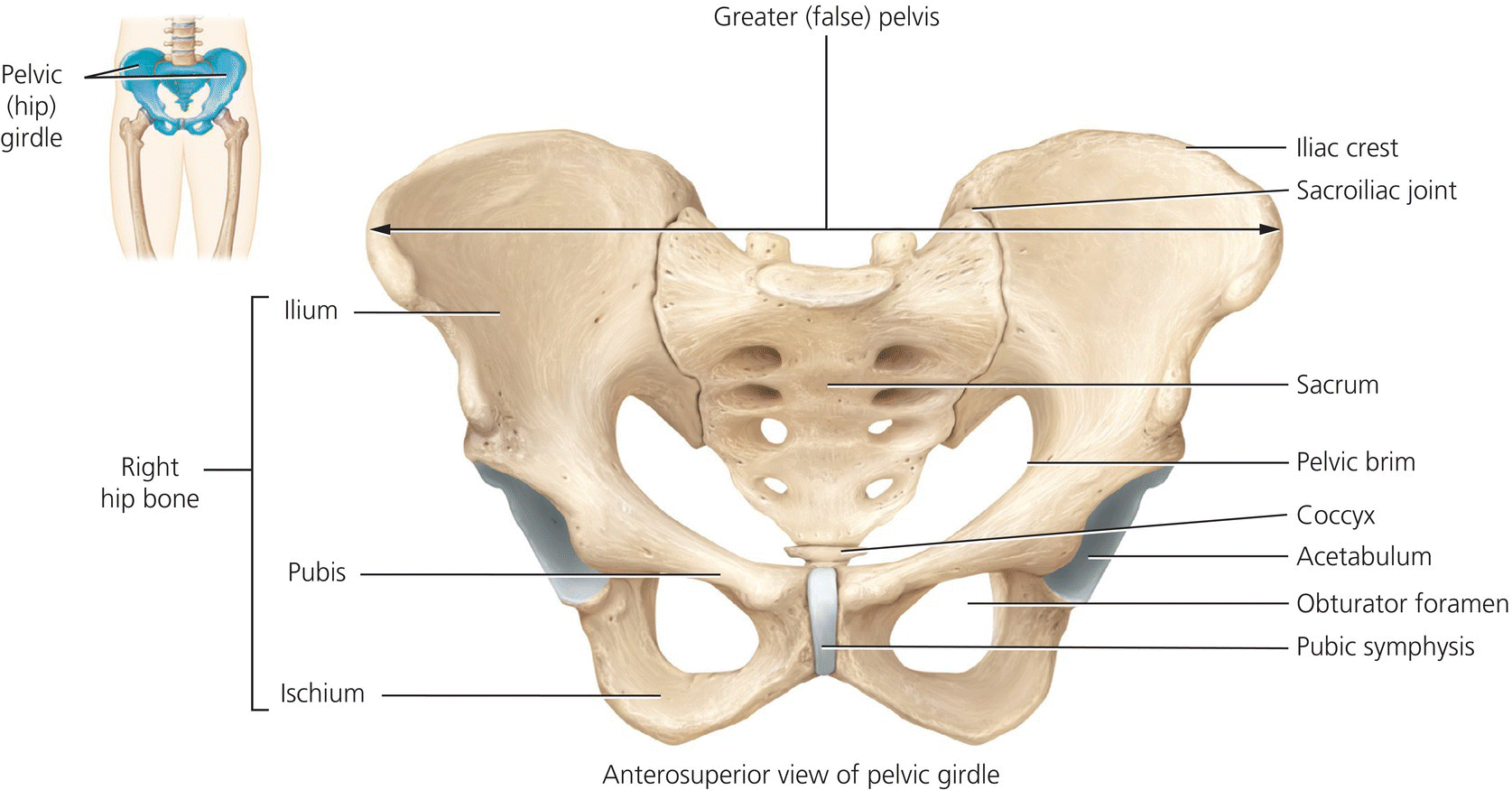
Figure 4.10 The female pelvis – anterior view. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The lower limb
The lower limbs are composed of 60 bones (see Figures 4.11 and 4.12). Each limb includes the femur, patella, tibia, fibula, tarsals, metatarsals and phalanges.
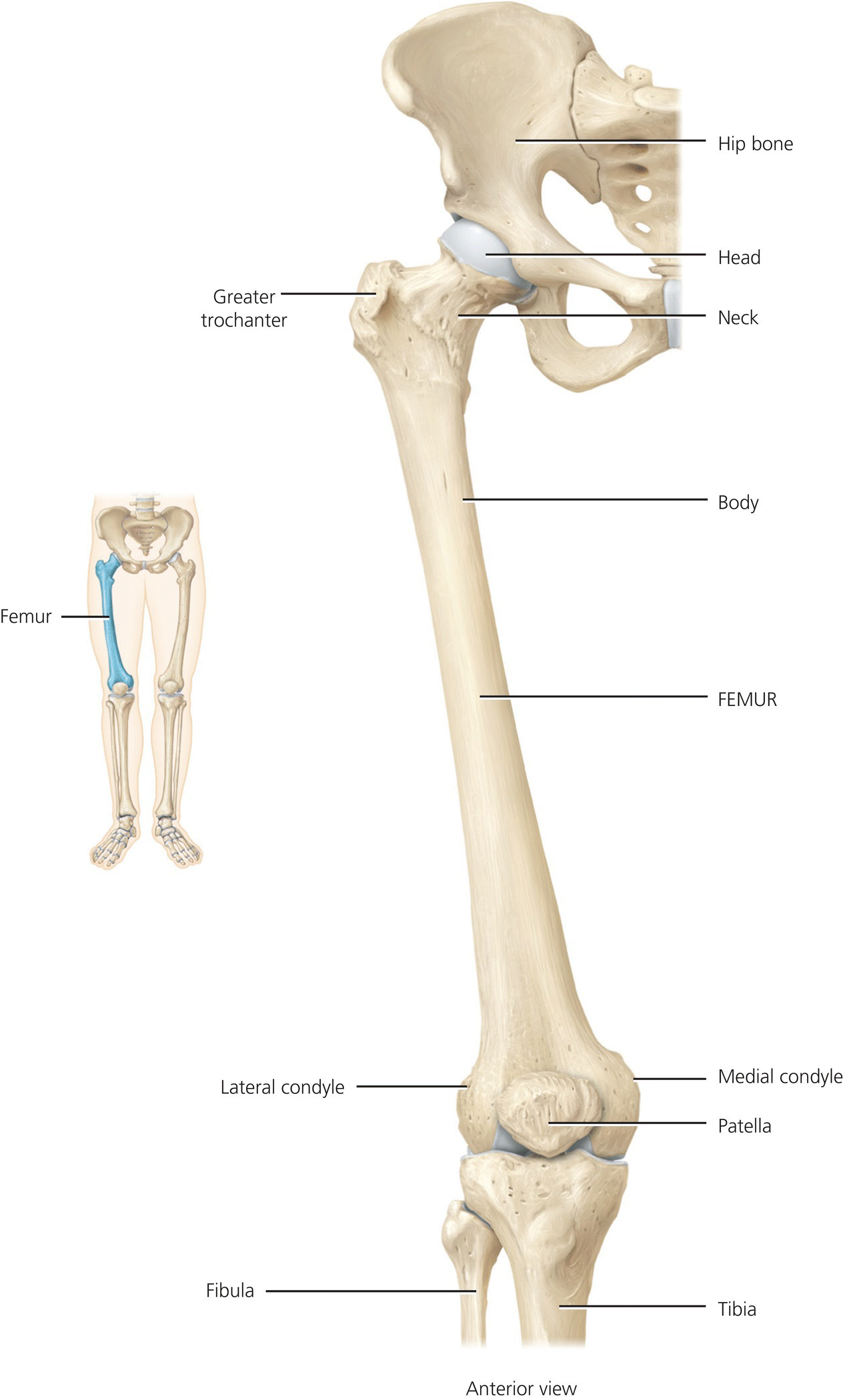
Figure 4.11 Lower limb – hip to knee. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
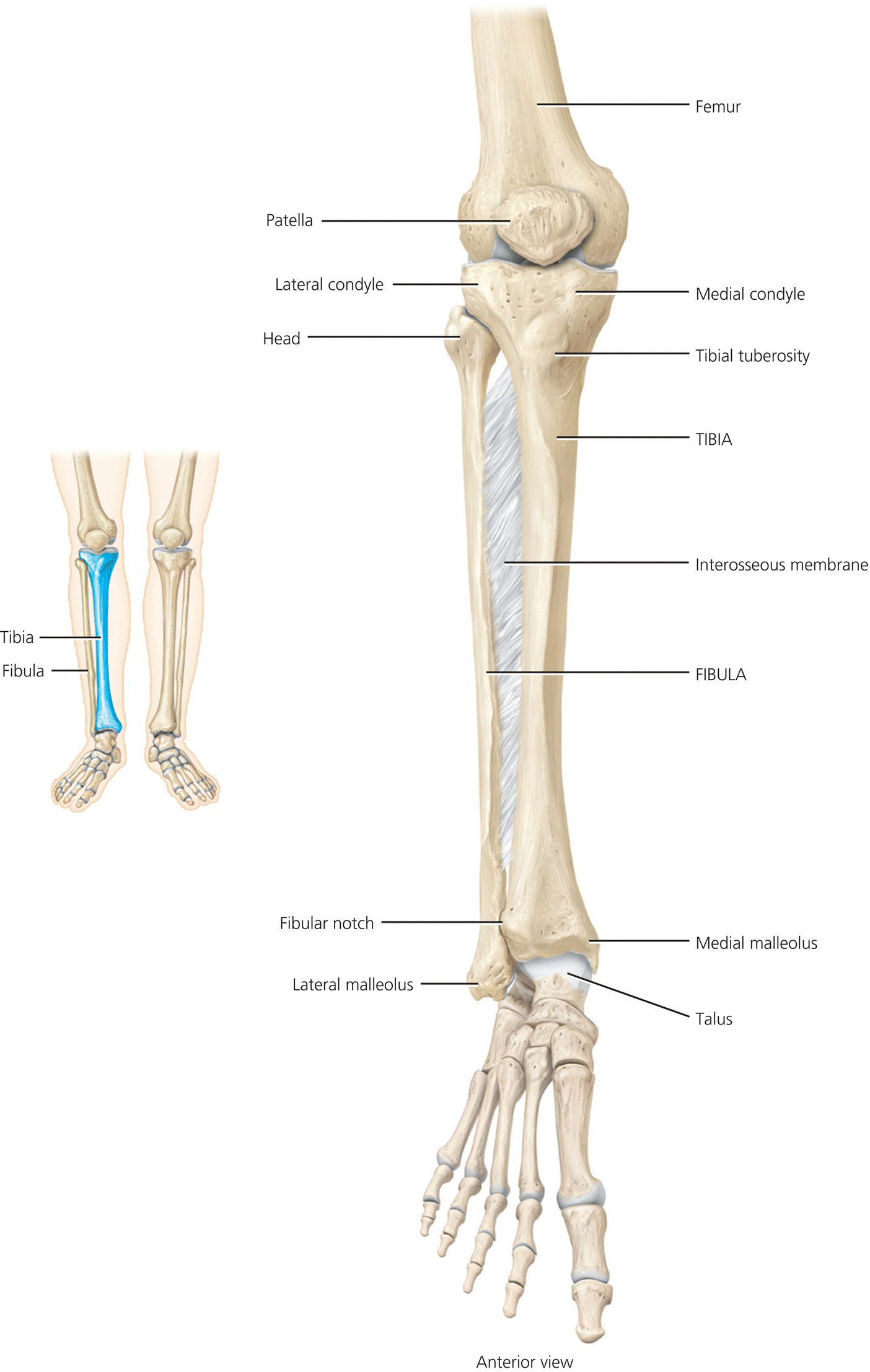
Figure 4.12 Lower limb – knee to foot. Tortora, G.J. and Derrickson, B.H. Essentials of Anatomy and Physiology. 2013, Wiley. This material is reproduced with permission of John Wiley & Sons, Inc.
The ball and socket arrangement of the hip joint allows flexion/extension, adduction/abduction and medial/lateral rotation and is central to the transfer of weight from the trunk and upper body to the legs. The proximal end, or head, of the femur articulates with the acetabulum of the innominate bone. The neck of the femur is a constricted region distal to the head. The greater and lesser trochanters are projections that serve as points for the attachment of some of the thigh and buttock muscles. The joint is supported by a series of strong muscles and ligaments with a main nerve supply from the femoral and obturator nerves formed from the lumbar plexus. The main blood supply comes from the femoral artery.
The femur is the longest and heaviest bone of the body and distally articulates with the tibia at the knee joint. The diaphysis of the femur has a rough vertical ridge on its posterior surface which serves as the attachment for several thigh muscles. The distal end of the femur expands and includes the medial and lateral condyles.
The knee is the largest joint. It is a hinge joint allowing flexion and extension supported by a complex system of ligaments and made up of three joints: the lateral and medial femorotibial and the patellofemoral. The two femorotibial joints are articulations between the lateral and medial condyles of the femur and the tibial condyles, separated by the intercondylar eminence. The patella is a small triangular sesamoid bone that sits in the quadriceps tendon anterior to the knee joint and provides protection to the knee joint during kneeling and glides over the distal femur during flexion and extension of the knee forming the patellofemoral joint. Stability is provided by the ligaments, cartilages and tendons of the joint, particularly the cruciate ligaments in the centre of the knee, but these are vulnerable to injury under excessive rotational forces. Two cartilage shock absorbers, the menisci, sit on the medial and lateral tibial condyles. The medial and lateral collateral ligaments lie external to the joint capsule and attach the medial and lateral femoral condyles to the medial tibial condyle and the head of the fibula laterally to prevent rotation.
There are 28 bones in the foot and ankle allowing adaptation to various surfaces, providing balance, mobility and weight bearing stability and shock absorbency. The ankle joint is the articulation between the distal ends of the tibia and fibula and the talus bone. During walking the talus initially bears the entire weight of the body and half of that weight is then transferred to the calcaneus. The remaining weight is transmitted to the other tarsal bones – cuboid, navicular and three cuneiform bones. The talus and calcaneum are located at the posterior part of the foot and the rest of the tarsal bones are located anteriorly. The cuneiform bone and cuboid bone articulate with the metatarsals. There are five metatarsals each consisting of a proximal base, shaft and distal head. Distally the metatarsals articulate with the proximal row of phalanges which consist of a proximal base, middle shaft, and distal head. The hallux (big toe) has two large heavy phalanges while the other four toes each have three phalanges – proximal, middle and distal. The bones of the foot are arranged in two arches which enable the foot to support and distribute weight. The arches of the foot are maintained by the bones, ligaments and tendons of the foot; these are not rigid, but yield when weight is applied and spring back when the weight is released.
Tendons and ligaments are vital to the foot for flexibility and movement and the muscles of the foot work in partnership with those of the lower leg. There are many nerves within the foot which permit sensation, particularly feeling the surface when walking.
Conclusion
A fundamental guide to musculoskeletal anatomy and physiology has been provided in this chapter. It is recognised, however, that considerable further detailed knowledge is required to support expert and effective practice. This can be gained from attention to further reading. This should include a deeper review of muscle anatomy and physiology than it has been possible to include here.
Anatomy and physiology act as part of the diverse evidence base that underpins musculoskeletal care. Practitioners cannot understand what has gone wrong with a system and meet patients’ needs if they do not know how it works when it is undamaged. To understand musculoskeletal diseases and disorders and the care and treatment associated with these health problems, the practitioner must have, as a priority, an in-depth working knowledge of the anatomy and physiology of the musculoskeletal system along with a general knowledge of other systems. Orthopaedic and trauma care covers the full span of life and most people will access some form of orthopaedic and trauma service in their lifetime A knowledge of anatomy and physiology is essential in facilitating prompt assessment and treatment as well as providing the tools for post-injury education of the patient.
Suggested further reading
- Kuntzman, A.J. and Tortora, G.J. (2010) Anatomy and Physiology for the Manual Therapies. : John Wiley & Sons, Inc., New Jersey.
- Palastanga, N. and Soames, R.W. (2012) Anatomy and Human Movement: Structure and Function 6th edn. Churchill Livingstone, Edinburgh.
References
- Kuntzman, A.J. and Tortora, G.J. (2010) Anatomy and Physiology for the Manual Therapies. John Wiley & Sons, Inc., New Jersey.
- Tortora, G.J. and Derrickson, B.H. (2013) Essentials of Anatomy and Physiology. John Wiley & Sons, Inc., New Jersey.