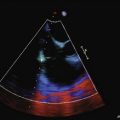
4 Right-Sided Valvular Disease
Background
Tricuspid Valve Structure and Function
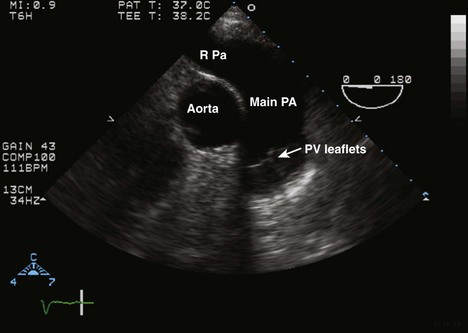
Pulmonic Valve Structure and Function
Overview of Echocardiographic Approach
Anatomic Imaging
Standard Scan Planes for Tricuspid and Pulmonic Valves
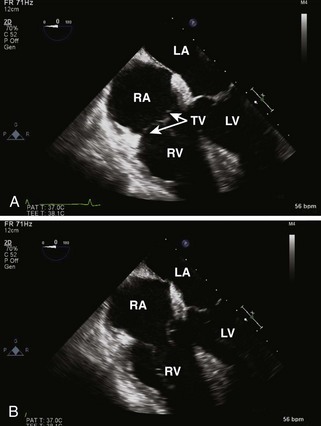
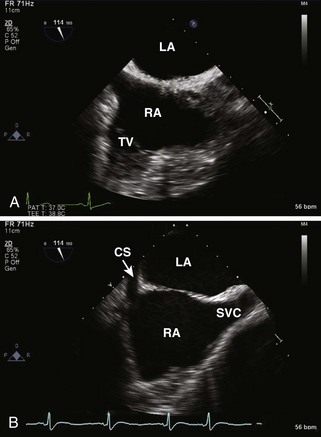
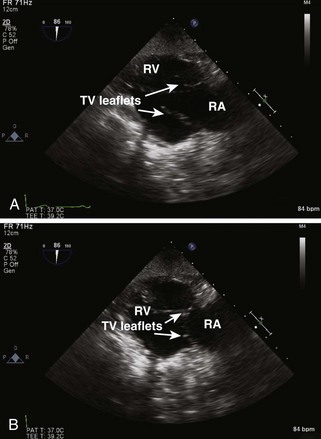
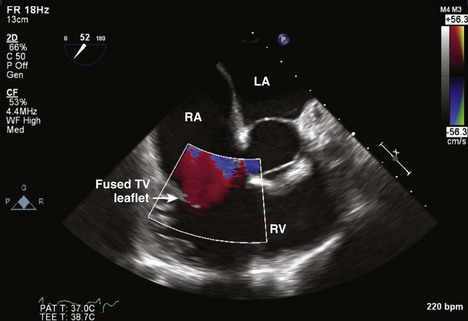
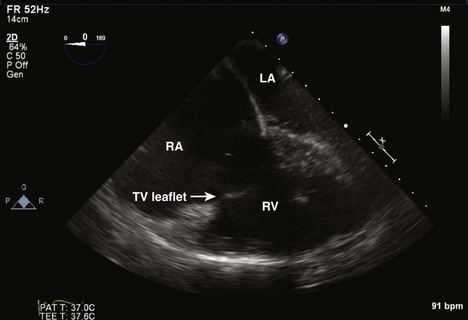
Tricuspid Valve
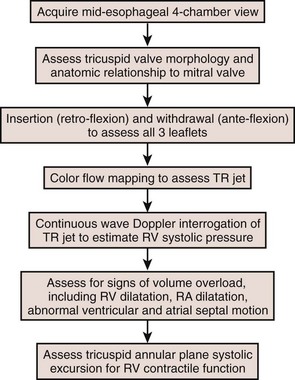
Step-by-Step Examination
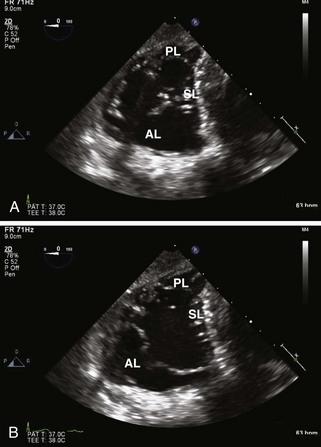
Step 1: 2D Examination
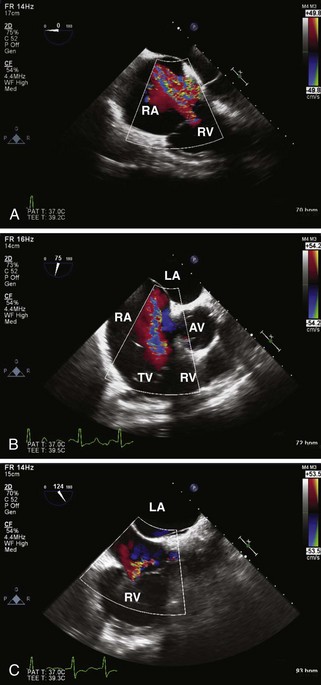
Step 2: CF Doppler
Step 3: Spectral PW Doppler and CW Doppler
Key Points
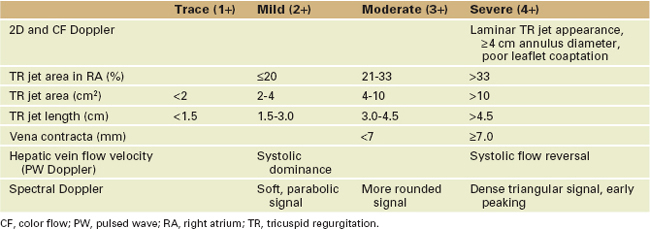
Tricuspid Regurgitation
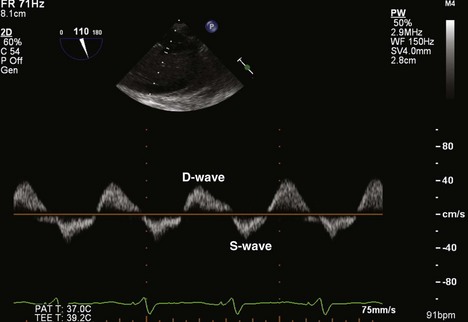
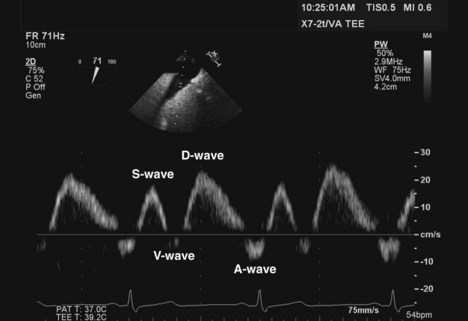
Figure 4-15 PW Doppler analysis of HV flow shows reversal of the S-wave in a patient with severe TR.
Box 4-2 Tricuspid Regurgitation
Etiology
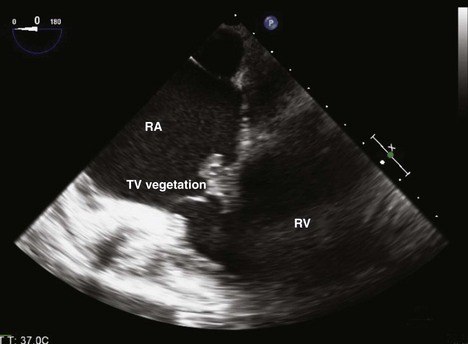
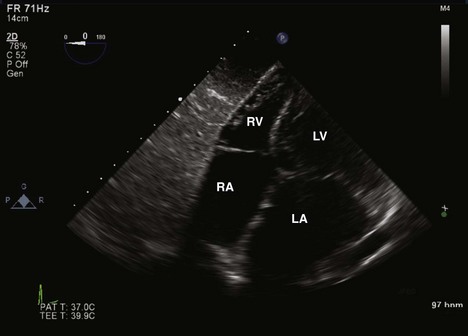
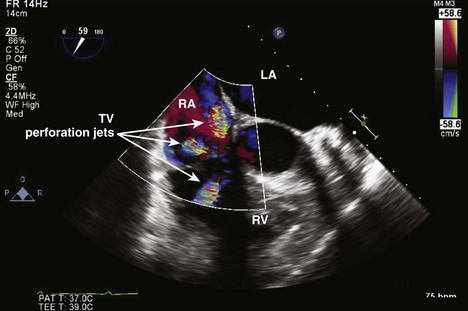
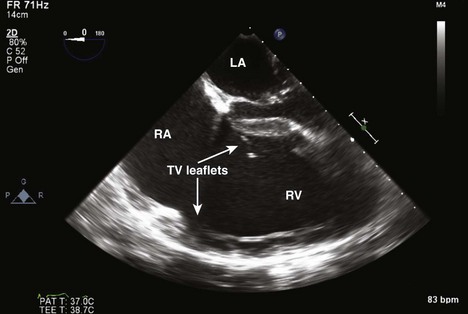
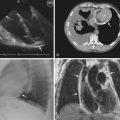
Figure 4-17 ME four-chamber view of the RA and RV shows a large vegetation arising from the leaflets of the TV.
Key Points
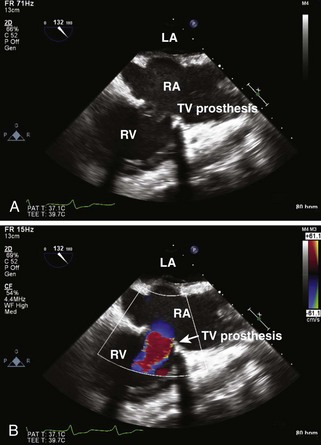
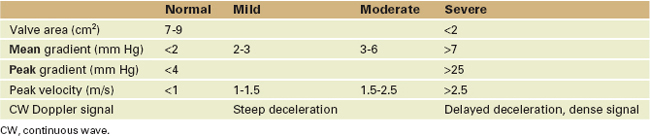
Tricuspid Stenosis
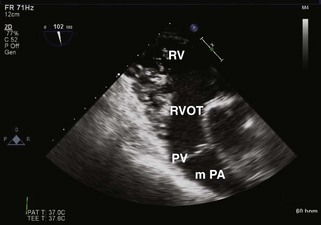
Pulmonic Valve
Step-by-Step Examination
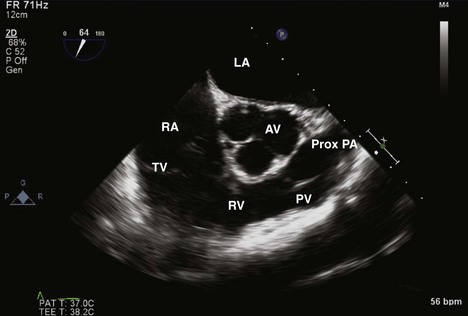
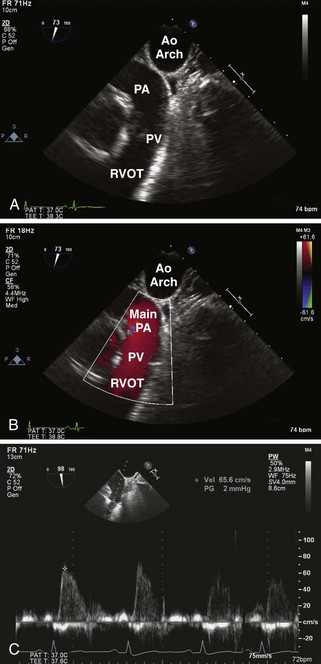
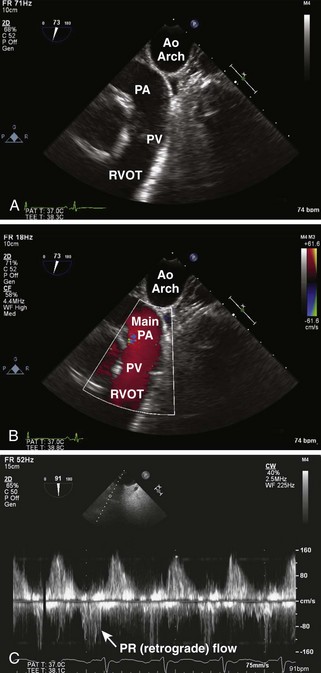
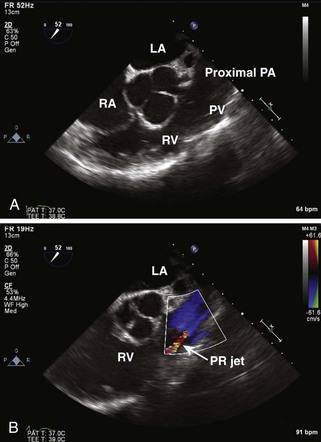
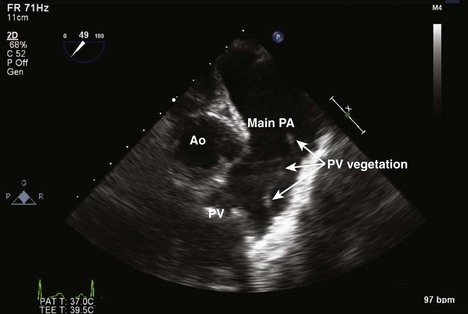
Step 1: 2D Examination
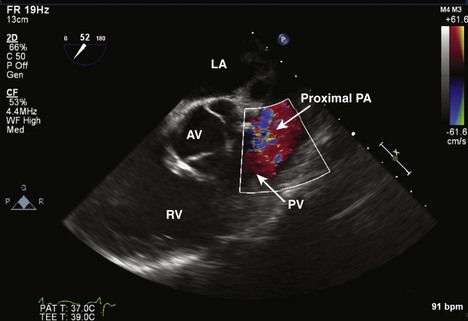
Step 2: CF Doppler
Step 3: Spectral PW Doppler and CW Doppler
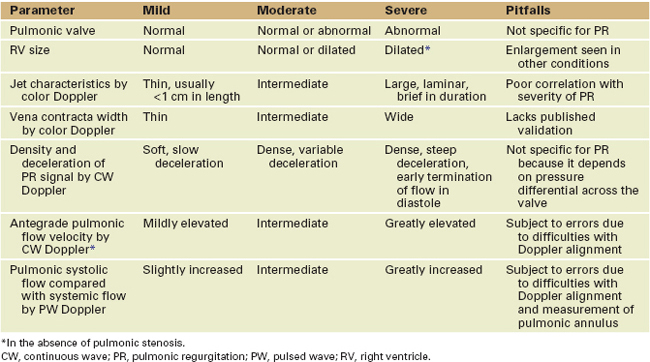
Pulmonic Regurgitation
Key Points
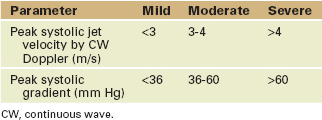
Pulmonic Stenosis
1 Attenhofer Jost CH, Connolly HM, Dearani JA, et al. Ebstein’s anomaly. Circulation. 2007;115:277-285.
2 Bonow RO, Carabello BA, Chatterjee K, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients with Valvular Heart Disease). J Am Coll Cardiol. 2006;48:e1-e148.
3 Maslow AD, Schwartz C, Singh AK. Assessment of the tricuspid valve: A comparison of four transesophageal echocardiographic windows. J Cardiothorac Vasc Anesth. 2004;18:719-724.
4 Bonow RO, Carabello BA, Chatterjee K, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: Executive summary. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients with Valvular Heart Disease). J Am Coll Cardiol. 2006;48:598-675.
5 Bruce CJ, Connolly HM. Right-sided valve disease deserves a little more RESPECT. Circulation. 2009;119:2726-2734.
6 David TE. Functional tricuspid regurgitation: A perplexing problem. J Am Soc Echocardiogr. 2009;22:904-906.
7 Pellikka PA, Tajik AJ, Khandheria BK, et al. Carcinoid heart disease. Clinical and echocardiographic spectrum in 74 patients. Circulation. 1993;87:1188-1196.
8 Zoghbi WA, Enriquez-Sarano M, Foster E, et al. Recommendations for evaluation of the severity of native valvular regurgitation with two-dimensional and Doppler echocardiography. J Am Soc Echocardiogr. 2003;16:777-802.