Chapter 11. Respiratory emergencies
Respiratory emergencies are a frequent part of the workload of a pre-hospital clinician. The following definitions are important in managing patients with respiratory problems:
• Hypoxaemia – inadequate oxygenation of the blood
• Hypoxia – inadequate oxygenation of the body
• Hypercarbia – high level of carbon dioxide in the blood, leads to acidaemia
• Acidaemia – where the blood becomes excessively acid (low pH), the body’s immediate response is to increase the respiratory rate (tachypnoea)
• Tachypnoea – a raised respiratory rate (usually >30 breaths/min)
• Hyperventilation – excessive breathing rate. In the absence of acidaemia will cause symptoms such as tingling around the lips and carpo-pedal spasm (seen in panic attacks).
Asthma
Approximately 1000 people die in the UK each year from this condition, so never underestimate the severity of an asthma attack. Individuals susceptible to other atopic disorders such as eczema, are more prone to developing asthma. There also appears to be a familial element.
Generalised airway obstruction is caused by:
• Inflammation of the airway passages, leading to oedema and swelling
• Increased production of thick mucus, leading to plugging of bronchioles
• Generalised bronchial smooth muscle constriction, leading to bronchospasm.
Precipitating causes of an acute exacerbation of asthma include:
• Exercise
• Infection
• Allergy to drugs or other substances
• Emotional upset.
Be especially cautious with patients who have a previous history of near-fatal asthma, with previous hospital admission or even a previous stay on intensive care for their asthma. These patients are sometimes referred to as ‘brittle’ asthmatics.
Life-threatening deterioration of an asthma attack may be very rapid.
Use of the peak flow meter
The patient’s peak expiratory flow rate (PEFR) is a useful predictor of the severity of an attack, particularly if the patient knows the value of their usual/normal PEFR. A predicted PEFR can be calculated if necessary, although the patient or parent (if the patient is a child) will often know it.
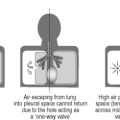
In rare cases, asthmatic patients develop spontaneous pneumothorax as a result of a ruptured bulla (lung cyst). They may also develop subcutaneous emphysema in the neck and anterior chest wall.
The differential diagnosis of a severe asthma attack includes pulmonary oedema, anaphylaxis, pneumothorax and airway obstruction.
Beware the asthma patient with a silent chest.
Management of asthma
• Maintain an air of calm
• Take a rapid history, including recent episodes and current treatment
• If the patient is unable to give a history, do not delay transfer to hospital
• Measure a PEFR if possible
• If severe or life-threatening features are present, or the patient does not respond to treatment, then warn the receiving hospital of your impending arrival.
Patients with severe or life-threatening asthma may not appear distressed or have all of these features. Make the diagnosis if any feature is present.
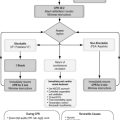
Prehospital treatment of severe and life-threatening asthma
The aim of emergency treatment is to reverse hypoxia with oxygen and reduce bronchospasm using β2-adrenoreceptor agonists. Oral or intravenous steroid therapy has no effect for at least 4 hours.
Adults
• Oxygen, high flow via a reservoir mask (10–15 L/min)
• Salbutamol 5 mg via an oxygen-driven nebuliser, repeated as necessary
• Intravenous access (consider crystalloid infusion if dehydrated)
• Hydrocortisone 200 mg IV
• ECG monitoring
• Immediate evacuation to hospital.
If the asthma is severe or life-threatening, ipratropium 0.5 mg should be added to the nebuliser.
Children
• Oxygen, high flow via a reservoir mask (10–15 L/min)
• Salbutamol 5 mg via an oxygen-driven nebuliser (the dose should be halved in children under 6 years old), repeated as necessary
• Intravenous access (consider crystalloid infusion if dehydrated)
• Hydrocortisone 200 mg IV
• ECG monitoring
• Immediate evacuation to hospital.
If the attack is severe or life-threatening, ipratropium 0.25 mg should be added to the nebuliser (0.125 mg in children under 1 year).
Unnecessary time should not be lost, in either adults or children, while intravenous access is obtained.
Transport to hospital
It is essential that time is not wasted in repeatedly attempting to perform clinical interventions that are not going according to plan. If problems are encountered, the patient should be immediately transferred to hospital. All of the above procedures can be carried out in the back of a moving ambulance. It is important to be prepared to intubate the patient if respiratory arrest occurs; airway pressures are likely to be high and ventilation will therefore be difficult. Cardiac arrest may ensue and the standard protocols should be followed.
Paramedics are well placed to deal with severe and life-threatening asthma, but they must act with speed and foresight to ensure a satisfactory outcome.
Pulmonary oedema
Pulmonary oedema is usually caused by acute left ventricular failure (LVF) and is common in the elderly. Heart failure leads to fluid collection in the alveoli of the lungs. The causes of ‘pump failure’ include:
• Acute myocardial infarction
• Dysrhythmias
• Antiarrhythmic drug overdose
• Inadequate heart rate (β-blocking drugs or post-infarction)
• Chronic valvular heart disease (usually aortic or mitral valve)
• Cardiac tamponade
• Fluid overload.
Symptoms of pulmonary oedema
• Breathlessness on exertion
• Paroxysmal nocturnal dyspnoea (waking at night with severe shortness of breath)
• Orthopnoea (breathlessness on lying down)
• Wheeze and cough are often reported
• Acute respiratory distress
• Coughing up pink froth or blood
• Chest pain may be present if an acute MI is the underlying cause.
Signs of pulmonary oedema
• Anxiety
• Pale, cold, clammy patient
• Cyanosis, tachypnoea, tachycardia
• Hypotension
• ECG monitoring may reveal an MI or a dysrhythmia
• Auscultation of the chest may reveal fine crepitations or a wheeze.
Management of pulmonary oedema
Treatment is aimed at improving oxygenation, reducing the volume of blood returned to the left ventricle and treating the underlying cause. Definitive treatment of acute pulmonary oedema requires hospital admission.
• Sit the patient up. This is vital and often forgotten
• Take a rapid history, noting the patient’s current medication
• Give high flow oxygen via a reservoir mask
• If systolic blood pressure is >90 mmHg, then give two puffs of glyceryl trinitrate (GTN) spray under the patient’s tongue
• Obtain intravenous access and give IV frusemide (a diuretic)
• Put the patient on ECG monitoring (treat any life-threatening dysrhythmia promptly)
• Consider morphine and Aspirin 300 mg if chest pain is present
• Transfer the patient to hospital
• Take a 12-lead ECG recording en route.
Anaphylaxis
• Anaphylaxis is an acute hypersensitivity (allergic) reaction to foreign protein (the allergen)
• Reactions worsen with repeated exposures to the allergen
• Common protein allergens include: antibiotics (particularly the penicillins), insect stings, shellfish, strawberries and nuts (e.g. peanuts)
• Colloid intravenous fluids (such as Hemaccel and Gelofusine) are rare causes of anaphylaxis
• The allergen is often never identified
• Some patients carry their own adrenaline for self-administration (such as the EpiPen®).
Allergic responses vary in severity, from a simple urticarial rash (‘nettle rash’) to a full-blown acute anaphylactic reaction with cardiorespiratory arrest. The speed of onset is variable and patients with marked sensitivity can progress to a severe reaction in a matter of minutes.
Symptom progression in anaphylaxis
• Urticarial rash (‘nettle rash’)
• Itchy skin
• Running eyes and nose
• Swelling of the face, eyes and lips, and occasionally the tongue
• Laryngeal oedema leading to airway obstruction
• Bronchospasm
• Tachycardia
• Tachypnoea
• Hypotension (shock)
• Cardiac arrest.
Management of anaphylaxis
• Try to reassure the patient and keep them calm
• Establish the history and if possible, the precipitating cause
• Oxygen 100%, 15 L/min via a reservoir mask, should be administered
• Establish intravenous access and give IV crystalloid fluids rapidly according to the patient’s requirements and local protocols
• If bronchospasm is present, this should be treated as asthma (see above)
• Hydrocortisone 200 mg IV (children 4 mg/kg) and chlorpheniramine 10 mg IV should be given.
Adrenaline
Severe cases must be treated with adrenaline 1:1000, 0.5 mL IM immediately. It may be necessary to repeat this. Airway obstruction must be treated promptly with basic and advanced techniques, and if necessary a surgical cricothyroidotomy.
| Age | Adrenaline 1:1000 (mL) |
|---|---|
| <6 months | 0.05 |
| 6 months–5 years | 0.12 |
| 6–11 years | 0.25 |
| >12 years | 0.5 |
Paediatric doses of adrenaline should be drawn up in small volume syringes and must be double checked with another practitioner before use. Note: Anaphylaxis is extremely rare in patients under the age of 2 years.
Chronic obstructive pulmonary disease
• Chronic obstructive pulmonary disease (COPD) was previously referred to as chronic obstructive airways disease (COAD) and includes chronic bronchitis and emphysema
• Chronic bronchitis is defined as the production of sputum for at least 3 months each year in two consecutive years. It causes obstruction by plugging the airways (bronchioles) with mucus, and by inflammation and thickening of the airway mucosa
• Emphysema is the dilation of alveolar airspaces by the destruction of their walls. The elastic recoil that holds the airways open in expiration is lost and obstruction to airflow occurs
• The main cause of COPD is smoking, although some cases are attributable to a rare inherited enzyme (α1-antitrypsin) deficiency
• The majority of patients demonstrate features of both bronchitis and emphysema
• Patients often present with recurrent pneumonias (lower respiratory tract infections)
• Patients with COPD rely on hypoxia as their drive to breathe because their respiratory centre, driven by a high carbon dioxide concentration in people without this condition, becomes relatively insensitive to carbon dioxide due to chronic exposure to elevated levels
• Patients often have wheeze, an element of their disease that may respond to the use of nebulisers.
Management of COPD
Patients with acute exacerbations of COPD are hypoxic. Emergency treatment is aimed at general supportive measures and relief of hypoxia. Rapid transport to hospital is mandatory. The preemptive siting of an IV cannula may be helpful in case of cardiorespiratory arrest.
HYPOXIA KILLS.
Patients with acute respiratory decompensation need supplemental oxygen. However, it is potentially dangerous to give supplemental oxygen to these patients unless they are carefully observed and the paramedic is prepared to assist ventilation if required. It is possible that administering oxygen will raise the oxygen concentration in the blood (PO 2) to a level at which the hypoxic drive is switched off, resulting in hypoventilation or apnoea. Patients can be verbally instructed to take additional breaths and can be assisted with a bag and mask with oxygen reservoir if necessary. The risk of shutting off hypoxic drive can be minimised by adjusting oxygen delivery to maintain SpO 2 at the patient’s usual level or at 90–92% if unknown.
NEVER WITHHOLD OXYGEN FROM A PATIENT WHO NEEDS IT.
Patients who die, do so from hypoxia, either because oxygen therapy is withheld or because practitioners fail to identify and support ventilation when the hypoxic drive is lost.
• HYPOXIA KILLS QUICKLY
• HYPERCARBIA KILLS SLOWLY
So give oxygen and support ventilation if the ‘hypoxic drive’ is lost.
If the patient has a wheeze, then give salbutamol 5 mg via nebuliser, repeated to effect. Mix 500 mg ipratropium with first dose of salbutamol.
For further information, see Ch. 11 in Emergency Care: A Textbook for Paramedics.