Chapter 500 Rare Tumors
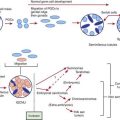
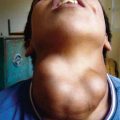
500.1 Thyroid Tumors
Cooper DS, Doherty GM, Haugen BR, et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2009;19:1167-1214.
DeLellis RA, Lloyd RV, Heitz PU, et al. Pathology and genetics of tumours of endocrine organs World Health Organization classification of tumours (vol 8). Lyon, France: IARC Press; 2004.
Grubbs EG, Rich TA, Li G, et al. Recent advances in thyroid cancer. Curr Probl Surg. 2008;45:156-250.
Kloos RT, Eng C, Evans DB, et al. Medullary thyroid cancer: management guidelines of the American Thyroid Association. Thyroid. 2009;19:565-612.
Waguespack S, Wells S, Ross J, et al. Thyroid cancer. In: Bleyer A, O’Leary M, Barr R, et al, editors. Cancer epidemiology in older adolescents and young adults 15 to 29 years of age, including SEER incidence and survival 1975–2000. Bethesda, MD: National Cancer Institute, 2006.
Waguespack SG, Sherman SI, Williams MD, et al. The successful use of sorafenib to treat pediatric papillary thyroid carcinoma. Thyroid. 2009;19:407-412.
Ying AK, Huh W, Bottomley S, et al. Thyroid cancer in young adults. Semin Oncol. 2009;36:258-274.
500.2 Melanoma
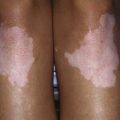
The incidence of melanoma in persons <20 yr of age in the USA is 4.2 cases per million, with almost all of these cases occurring in adolescents (Chapter 643). Melanoma is more common among adolescent females than males. In the USA, incident rates of melanoma in younger age groups are increasing, although at a slower rate than in adults. Although sun exposure is a well-known risk factor for melanoma in adults, its role in pediatric melanoma is less clear. Pediatricians should counsel patients regarding avoidance of sun exposure to decrease the risk of later development of melanoma. Patients with fair skin and a family history of melanoma are at particularly high risk. Known risk factors for children are giant hairy nevus (>20 cm), dysplastic nevus syndrome, and xeroderma pigmentosum.
Lange JR, Palis BE, Chang DC, et al. Melanoma in children and teenagers: an analysis of patients from the National Cancer Data Base. J Clin Oncol. 2007;25:1363-1368.
Livestro DP, Kaine EM, Michaelson JS, et al. Melanoma in the young: differences and similarities with adult melanoma. Cancer. 2007;110:614-624.
Strouse JJ, Fears TR, Tucker MA, et al. Pediatric melanoma: risk factor and survival analysis of the surveillance, epidemiology and end results database. J Clin Oncol. 2005;23:4735-4741.
500.3 Nasopharyngeal Carcinoma
Bray F, Haugen M, Moger TA, et al. Age-incidence curves of nasopharyngeal carcinoma worldwide: bimodality in low-risk populations and aetiologic implications. Cancer Epidemiol Biomarkers Prev. 2008;17:2356-2365.
Ozyar E, Selek U, Laskar S, et al. Treatment results of 165 pediatric patients with non-metastatic nasopharyngeal carcinoma: a Rare Cancer Network study. Radiother Oncol. 2006;81:39-46.
Tsao SW, Lo KW, Huang DP. Nasopharyngeal carcinoma. In: Tselis A, Jenson HB, editors. Epstein-Barr virus. New York: Taylor and Francis; 2006:273-295.
500.4 Adenocarcinoma of the Colon and Rectum
Durno C, Aronson M, Bapat B, et al. Family history and molecular features of children, adolescents, and young adults with colorectal carcinoma. Gut. 2005;54:1146-1150.
Durno CA, Gallinger S. Genetic predisposition to colorectal cancer: new pieces in the pediatric puzzle. J Pediatr Gastroent Nutr. 2006;43:5-15.
Ferrari A, Rognone A, Casanova M, et al. Colorectal carcinoma in children and adolescents: the experience of the Istituto Nazionale Tumori Milan, Italy. Pediatr Blood Cancer. 2008;50:588-593.
500.5 Adrenal Tumors
Armstrong R, Sridhar M, Greenhalgh KL, et al. Phaeochromocytoma in children. Arch Dis Child. 2008;93:899-904.
Baid SK, Lai EW, Wesley RA, et al. Brief communication: radiographic contrast infusion and catecholamine release in patients with pheochromocytoma. Ann Intern Med. 2009;150:27-32.
Barontini M, Levin G, Sanso G. Characteristics of pheochromocytoma in a 4- to 20-year-old population. Ann N Y Acad Sci. 2006;1073:30-37.
DeLellis RA, Lloyd RV, Heitz PU, et al. Pathology and genetics of tumours of endocrine organs World Health Organization Classification of Tumours (vol 8). France: Lyon; 2004.
Hanna AM, Pham TH, Askegard-Giesmann JR, et al. Outcome of adrenocortical tumors in children. J Pediatr Surg. 2008;43:843-849.
Ludwig AD, Feig DI, Brandt ML, et al. Recent advances in the diagnosis and treatment of pheochromocytoma in children. Am J Surg. 2007;194:792-796. discussion 796–797
Michalkiewicz E, Sandrini R, Figueiredo B, et al. Clinical and outcome characteristics of children with adrenocortical tumors: a report from the International Pediatric Adrenocortical Tumor Registry. J Clin Oncol. 2004;22:838-845.
Pham TH, Moir C, Thompson GB, et al. Pheochromocytoma and paraganglioma in children: a review of medical and surgical management at a tertiary care center. Pediatrics. 2006;118:1109-1117.
Rodriguez-Galindo C, Figueiredo BC, Zambetti GP, et al. Biology, clinical characteristics, and management of adrenocortical tumors in children. Pediatr Blood Cancer. 2005;45:265-273.
Waguespack SG, Rich T, Grubbs E, et al. A current review of the etiology, diagnosis, and treatment of pediatric pheochromocytoma and paraganglioma. J Clin Endocrinol Metab. 2010;95:2023-2037.
Young WFJr. Pheochromocytoma in children. UpToDate Online. 2008. 17.1