Chapter 9 Privacy, confidentiality and consent
Upon completion of this chapter you should be able to:
INTRODUCTION
The nature of pharmacy practice, whether conducted in the private or public sectors, whether provided by sole owners or members of an institutional health care team, will almost always include access to patient and client information. This access to patient and client private and confidential information is based on the therapeutic relationship which exists between consumers of health services and health professionals who care for them. Indeed, it is a combination of the legal, professional and ethical obligations imposed on health professionals to keep the patient’s and client’s information confidential — and the patient’s and client’s perception that such information will be kept confidential — that underpins the therapeutic relationship. That is, a pharmacist needs patients and clients to disclose relevant health information to be able to make informed decisions regarding which treatment options may be most suitable and appropriate. The patient is only likely to disclose such information, however, if it is understood that their information will be kept confidential and used only for the purpose of clinical decision-making. It is therefore important that pharmacists have an understanding of the legal, professional and ethical obligations that maintain the confidentiality of patient information and the mechanisms by which privacy of, and access to, patient information is secured.
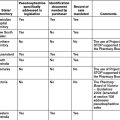
Various situations in pharmacy practice require pharmacists to follow privacy and confidentiality legislation, principles and guidelines. The Pharmacists Board of Queensland has identified the following practice situations that involve the improper disclosure of information:[1]
Skene notes that privacy and confidentiality are different issues in that privacy is focused on the collection of information, whereas confidentiality is focused on communication of that information.[2] Although the duties imposed on pharmacists in relation to these two issues differ conceptually, they are complimentary to one another in their application and there is a considerable overlap within a health care context.
THE OBLIGATION TO KEEP INFORMATION CONFIDENTIAL
All that may come to my knowledge in the exercise of my profession or outside of my profession or in daily commerce with men [and women], which ought not be spread abroad, I will keep secret and never reveal.[3]
[A person who] has received information in confidence shall not take unfair advantage of it. He [or she] must not make use of it to the prejudice of he [or she] who gave it without obtaining consent.
PROFESSIONAL AND ETHICAL OBLIGATIONS
Professional codes of conduct and ethics protect the rights of patients and clients to have their information kept confidential. The Pharmaceutical Society of Australia (PSA) Code of Professional Conduct (the code) expressly recognises the obligation imposed upon pharmacists to keep client information confidential. Principle three of the code states:[4]
The various pharmacy registering authorities in each of the Australian jurisdictions also make express reference to the professional obligation to maintain patient and client confidentiality. For example, the Pharmacy Board of Victoria Guidelines for Good Pharmaceutical Practice[5] includes provisions covering privacy and confidentiality and the Pharmacists Board of Queensland Guidelines on Privacy and Confidentiality[6] specifically provide guidance to registrants on privacy and confidentiality issues as they relate to pharmacy practice. Pharmaceutical Defence Limited (PDL) also refer to the pharmacists’ professional obligations to ensure privacy and confidentiality.[7]
The Society of Hospital Pharmacists of Australia’s Code of Ethics (2006) identifies that ‘ [A]ll patient services must be provided with courtesy, respect and confidentiality’. Pharmacists should also refer to the PSA document titled: Professional Practice and the Privacy Act[8] and always endeavour to maintain the relevant professional practice standards; for example, criterion 1 of the Fundamental Pharmacy Practice standard and criterion 2 of the Organisation of Pharmacy Practice standard.[9]
Strict adherence to privacy guidelines in community pharmacy is complicated by the retailing component and requires careful planning. The Pharmacists Board of Queensland suggests the following strategies:[10]
Pharmacies participating in the Diabetes Medication Assistance Service (DMAS) are required to have a separate counselling area.[11] As the profession moves towards the provision of more specialised services the requirement to have separate counselling areas may become more popular in the future. As these areas could also be used for patient counselling that is of a confidential nature, for example counselling involved in the provision of the morning after pill (MAP), this would assist the profession in complying with privacy requirements.
STATUTORY OBLIGATIONS
Legislation exists at state, territory and federal levels directed specifically to the maintenance of confidentiality in relation to patient and client information. The legislation generally provides that clients or users of health care services have the right to those services being provided in a way that respects their right to the confidentiality of their information. Health professionals, often referred to as the ‘designated person’ or ‘relevant person’, must not disclose that information either directly or indirectly to others and there is usually a statutory penalty in circumstances in which information is disclosed inappropriately. As an example, the Queensland Health Services Act 1991 sections 60–62 impose on public health sector employees a duty of confidentiality and a penalty for breach of that statutory duty. Section 62A states:
Maximum penalty — 50 penalty units.
Common law obligations
Negligence
The duty to keep information confidential is part of the duty of care owed by a pharmacist to their clients. In circumstances in which this duty is breached through the pharmacist divulging client information the pharmacist may be sued in negligence for the damage caused by the breach.[12]
Defamation
An action in defamation is founded on an allegation that the pharmacist makes a statement about a patient, which though untrue, is published and thereby lowers the reputation of the patient in the eyes of their peers. The law of defamation is not uniform across Australia, with certain jurisdictions such as New South Wales, Queensland and Victoria having enacted legislation.[13]
Equity
In my judgement, three elements are normally required if, apart from contract, a case of breach of confidence is to succeed. First, the information itself … must have the necessary quality of confidence about it. Secondly, that information must have been imparted in circumstances importing an obligation of confidence. Thirdly, there must be an unauthorised use of that information to the detriment of the party.
EXCEPTIONS TO THE DUTY TO CONFIDENTIALITY
Legal duty of disclosure
In all Australian states and territories there is legislation requiring the disclosure of certain patient and client information. Though the specific requirements of each jurisdiction are set out in the respective Acts it is mandatory in all jurisdictions, other than Western Australia, for nominated professionals to report suspected child abuse.[14] In most jurisdictions the diagnosis of a communicable disease and/or the presentation of a client with suspicious injuries are also reportable. There are also legislative provisions in the respective jurisdictions to provide information, or produce documents or other materials, as part of the court process. Though in a number of the states or territories there is no legal protection inherent in the health professional–patient relationship, in Victoria, Tasmania and the Northern Territory, doctor–patient privilege is permitted in civil proceedings.[15] In both Victoria and New South Wales there is privilege in the communication between victims of sexual assault and their counsellors.[16]
Public interest disclosure
The obligation imposed on a health professional to keep a patient’s or client’s information confidential may be overridden in circumstances in which the disclosure of the information is necessary in the public interest. This public interest exception is not clearly defined and arises only where there is a real and significant threat of harm, or the possibility of death; for example, where a pharmacist is told by the patient or client that they intended to kill or harm another person.[18] In the case of W v Edgell and Others [1990] 1All ER 855, the doctor was employed to provide an assessment of W, a forensic prisoner, for the purpose of his release to a less secure mental health facility. The psychiatric assessment carried out by Dr Edgell was unfavourable to the prisoner and his legal representative withdrew the application. Dr Edgell, believing W still presented a considerable danger, forwarded his report to the Secretary of State. The court dismissed W’s application based on a breach of doctor–patient confidentiality and held that the public interest in disclosing the information to the authorities outweighed W’s right to have his information kept confidential.
PRIVACY LAW
While there is an overlap between the concept of confidentiality and the privacy of patient or client information, as discussed previously, they are recognised as two different concepts and therefore the requirements in relation to privacy need to be addressed separately. The privacy of a patient’s or client’s personal information is secured under the provisions of the Commonwealth Privacy Act 1988. The Privacy Act 1988 (Cth), amended in 2001,[19] covers individuals, and the private and public sectors and establishes the 10 National Privacy Principles (NPPs),[20] which apply to parts of the private sector and to all health service providers. The Act also establishes the 11 Information Privacy Principles (IPPs)[21] which apply to the Commonwealth and Australian Capital Territory government agencies. These IPPs provide for the collection, storage, security, use and disclosure of personal information and, in addition, deal with the right of access to information and correction of information that is collected about an individual. The legislation creates the position of the Federal Privacy Commissioner to whom complaints may be directed when there is an alleged breach of the provisions.
Section 62A(2) of the Privacy Act 1988 (Cth) states that:
An ‘organisation’ is defined under the legislation so as to include an individual, a body corporate and a partnership; but not a government agency. While small businesses are generally excluded those that provide a health service are not.[22]
A private organisation or provider may withhold information and refuse access:
NPP 1: Collection and NPP 10: Sensitive Information and NPP 8: Anonymity — identify the provider’s obligations when collecting a patient or client’s health information. This includes an obligation on a pharmacist to collect fairly and lawfully only that health information that is necessary to provide a service. The information must be collected directly from the individual (if practicable) and only with the consent of the individual unless an exemption applies. If lawful and practicable, the individual has a right to remain anonymous during the interaction.[23]
NPP 2: Use and Disclosure — identifies how health information, once collected by the pharmacist can be used within the pharmacy, health care institution or disclosed to third parties outside the practice or the institution. As a general proposition the information can only be used for the purpose for which it was collected.[6]
NPP 3: Data Quality and NPP 4: Data Security — identify the standards required for keeping information up to date, accurate and complete. The principles also address the obligation to protect information from misuse, loss, unauthorised access, modification or disclosure. When information is no longer required to be kept it has to be permanently de-identified or destroyed.[6]
Application of the NPPs
In relation to pharmacy practice the NPPs will be applicable to every customer transaction and must be considered when handling patient’s or client’s health care information. The Competency Standards for Pharmacists in Australia expressly refers to the obligation upon pharmacists to comply with relevant legislation and requires that a pharmacist ‘considers the impact of privacy legislation on professional practice’, ‘understands the nature of patient consent’, and ‘obtains patient consent as required for professional services including those where health information will be collated and shared with other health.[27] The pharmacist must therefore decide the following:
State legislation and government schemes
In relation to health records, the Australian Capital Territory, New South Wales, Queensland and Victoria have enacted their own privacy legislation and adopted privacy schemes which operate in addition to the federal provisions.[28] The additional privacy legislation and schemes are summarised below.
New South Wales
The Health Records and Information Privacy Act 2002 establishes 15 Health Privacy Principles (HPPs), provides for the creation of ‘Statutory Guidelines’ to assist in the application of the principles and establishes a framework for managing complaints about the handling of health information. There are four statutory guidelines which are legally binding and apply to the use or disclosure of health information for the management of health services, for training purposes, for research purposes and the notification when collecting health information about a person from someone else. While the Health Records and Information Privacy Act 2002 applies to both the public and the private sectors, the Privacy and Personal Information Act 1998 applies only to the information held within the public sector.
ACCESS TO PATIENT AND CLIENT INFORMATION
At common law the physical property in the patient’s file or records is with the organisation or person who made that file or record.[29] If the pharmacist establishes and maintains a patient file, that file is the property of the pharmacist who made it. This means that a patient has no legal right at common law to access their file and must therefore gain access under the relevant legislative provisions. Some of the legislation discussed above (state legislation and government schemes) facilitates access in the private and public sectors. Additionally, there are also the Freedom of Information Acts at state, territory and federal levels that provide access to and production of personal records specifically in the public sector. The Freedom of Information Act 1982 (Cth) applies to the federal sector and provides any individual, subject to express exclusions, with a legally enforceable right to obtain access to their records in accordance with the Act. Similar legislation in place in the states and territories is contained in Table 9.1.
Table 9.1 State and territory freedom of information legislation
| Cth | Freedom of Information Act 1982 |
| ACT | Freedom of Information Act 1989 |
| NSW | Freedom of Information Act 1989 |
| NT | Information Act 2004 |
| Qld | Freedom of Information Act 1992 |
| SA | Freedom of Information Act 1991 |
| Tas | Freedom of Information Act 1991 |
| Vic | Freedom of Information Act 1982 |
| WA | Freedom of Information Act 1992 |
Children
Whether a child has the right to have their information kept confidential is inextricably connected to both the child’s capacity to make decisions on their own behalf and an assessment as to what is in the best interest of the child in the particular circumstances. Generally, there is an obligation on all health professionals to keep information about their patients and clients confidential unless there is express consent by the patient or client to disclosure. It could be suggested that similar obligations are imposed in relation to the information and data collected by pharmacists about those of their patients or clients who are children. This obligation, to keep information confidential, is based on the legislation at Commonwealth, state and territory levels, common law decisions and professional codes of ethics and conduct.
if the parents do not have the power to consent to the medical treatment their child seeks, they do not have the power to obtain medical information about that treatment.[30]
As with adults at common law, there is no right of access by a child to their medical records, and any person seeking such access must make an application under the existing legislative provision. The Commonwealth, state and territory legislation, in the form of the Freedom of Information Acts, operate in the public sector and give an individual a legally enforceable right to seek access to their records. While it is acceptable in most jurisdictions for a parent to make an application under this legislation on behalf of their child, they may be denied access where the information is potentially prejudicial or where it would be otherwise unreasonable for the parent to be given the access requested. The Privacy Act 1988 (Cth), in its application to health care delivery in the private sector, is silent as to the exact age at which the right to access information is acquired. A child’s right to access their own information would therefore appear to be dependent on similar criteria to that which determines their ability to give a legally valid consent. That is, their level of competence or capacity to understand the nature and effect of their decisions and their level of maturity and intelligence.
CONSENT
Obtaining a valid consent from a patient or client prior to providing any health care intervention converts what would otherwise be civil assault or battery into a lawful interaction. With the increase in medical technology, and the expanding role of the pharmacist into more diverse areas of patient and client care, it is essential that pharmacists are aware of their legal rights and obligations in relation to obtaining a legally valid consent from their patients and clients. The legal requirement for obtaining a valid consent from a patient or client, prior to any interference with their person, applies regardless of whether or not the patient or client would benefit from the treatment or be harmed by refusing the procedure.[31]
A pharmacist must therefore ensure that a valid consent is obtained prior to undertaking Home Medicine Reviews (HMRs), providing diabetes medication assistance services, initiating any weight reduction regime, carrying out any diagnostic or assessment procedures such as taking blood pressure, bone density screening, blood sugar monitoring and International Normalised Ratio testing for patients on warfarin.
A pharmacist must respect the clients’ autonomy and dignity and their right to make informed decisions relating to their treatment.[4]
Types of consent
With regard to core pharmacy services, it is most likely that consent will take the form of verbal or implied consent. Verbal consent is the type which is most frequently obtained within a health care context. The consent of a patient or client may also be implied from their conduct; for example, where a person holds out their wrist to have their pulse taken or their arm to have their blood pressure taken. However, in a health care context it is advisable to obtain a written or verbal consent so that the patient or client’s intention is clear rather than rely on the implication from their conduct.
What constitutes a valid consent?
Informed consent
As noted in Chatterton’s case, the amount and nature of information required to defend an action in trespass (civil assault and battery) is different from that required in an action in negligence. The amount and nature of information required to defend a claim in negligence, that there has been a breach of the duty to warn of risk, is set out in the respective civil liability legislation in each jurisdiction.[32] As an example, section 21 of the Queensland Civil Liability Act 2003 states:
Legal capacity to give a valid consent
A child who has the intellectual capacity to understand the nature of the proposed treatment is said to be Gillick competent and thereby competent and capable of providing a legally valid consent. The decision in this case was approved by the High Court of Australia in Secretary, Department of Health and Community Services v JWB and SMB (Marion’s case) (1992)175 CLR 218 at 238.
Patients and clients with an intellectual disability will have varying levels of capacity to make health care decisions. The capacity of an individual to make decisions will often be contingent on the nature of the decision and context in which the specific decision is to be made. That is, a patient with a mild level of an intellectual impairment may be quite capable of consenting to the administration of a medication or the performance of a diagnostic test. However, they may not have the capacity to give a legally valid consent to a highly technical and invasive procedure. In circumstances in which a patient or client lacks the intellectual capacity to provide a legally valid consent it will be necessary to identify and consult with the substitute decision-maker. Each jurisdiction has legislation which identifies and empowers a person or statutory entity who can give a valid consent for a person who has lost their capacity to consent on their own behalf. The guardianship legislation in each of the states and territories is contained in Table 9.2.
| ACT | Guardianship and Management of Property Act 1991 | Guardianship and Management of Property Tribunal |
| NSW | Guardianship Act 1987 | Guardianship Tribunal |
| NT | Adult Guardianship Act 1988 | Guardianship Panel, Local Court |
| Qld | Guardianship and Administration Act 2000 | Guardianship and Administration Tribunal, Queensland Civil and Administrative Tribunal |
| SA | Guardianship and Administration Act 1993 | Guardianship Board |
| Tas | Guardianship and Administration Act 1995 | Guardianship and Administration Board |
| Vic | Guardianship and Administration Act 1986 | Guardianship and Administration List, Victorian Civil and Administrative Tribunal |
| WA | Guardianship and Administration Act 1990 | State Administrative Tribunal |
Attorney-General’s Department. Online. Available: www.ag.gov.au/foi
Commonwealth Attorney-General’s Department (Privacy Division). Online. Available: www.law.gov.au/privacy
Coppock J. Privacy is critical to pharmacy. Australian Journal of Pharmacy. 87, October 2006.
Office of Federal Privacy Commissioner. Online. Available: www.privacy.gov.au and www.privacy.gov.au/privacy_rights/laws/index.html#5
Office of New South Wales Privacy Commissioner. Online. Available: www.lawlink.nsw.gov.au/pc/nsf/pages/index
Privacy Act 1988 and Privacy Amendment (Private Sector) Act 2000 (Cth). Online. Available: www.comlaw.gov.au
1 Pharmacy Board of Queensland. Guidelines on Pharmacy and confidentiality. July 2007
2 Skene L. Law and Medical Practice-Rights, Duties, Claims and Defences, 2nd edn. Sydney: Lexis Nexis Butterworths, 2004. paras 9.1, 9.8
3 Reproduction of the Hippocratic Oath. Mason J.K., Laurie G.T., McCall Smith R.A., editors. Law and Medical Ethics, 4th edn, London: Butterworths, 1994.
4 Pharmaceutical Society of Australia. Australian Pharmaceutical Formulary and Handbook (20th edn). Pharmaceutical Society of Australia, Deakin, ACT: 358–9
5 Pharmacy Board of Victoria. Guidelines for Good Pharmaceutical Practice. Effective from 1 February 2005
6 Pharmacy Board of Queensland. Guidelines on Pharmacy and Confidentiality. July 2007
7 Coppock J. Privacy is critical to pharmacy. Australian Journal of Pharmacy. 87, October 2006.
8 Pharmaceutical Society of Australia. Professional Practice and the Privacy Act. Canberra: Pharmaceutical Society of Australia; 2001.
9 Pharmaceutical Society of Australia. Professional Practice Standards (version 3). 2006. Online. Available: www.psa.org.au [accessed 28 May 2009]
10 Pharmacy Board of Queensland. Guidelines on Pharmacy and Confidentiality. Pharmacy Board of Queensland; July 2007.
11 Australian Government Department of Health and Ageing and the Pharmacy Guild of Australia. Diabetes Medication Assistance Service, Terms and Conditions. August 2008
12 Furniss v Fitchett [1958] NZLR 396 at 404
13 Defamation Act 2005 (NSW); Defamation Act 2005 (Qld); Defamation Act 2005 (Vic)
14 Children and Young People Act 1999 (ACT); Public Health Act 2005 (Qld); Children and Young Persons (Care and Protection) Act 1998 (NSW); Community Welfare Act (NT); Children’s Protection Act 1993 (SA); Children, Young Persons and their Families Act 1997 (Tas); Children and Young Persons Act 1989 (Vic)
15 Evidence Act 1958 (Vic); Evidence Act 2001 (Tas); Evidence Act (NT)
16 Evidence Act 1958 (Vic); Evidence Act 1995 (NSW)
17 Wisewoulds Lawyers correspondence to Pharmaceutical Defence Limited. The parameters of reporting a minor’s request to dispense MAP. 26 July 2005
18 Tarasoff v Regents of the University of California 551 P 2d 334 (1976)
19 Privacy Amendment (Private Sector) Act 2000
20 Schedule 3 Privacy Act 1988 (Cth)
21 Schedule 14 Privacy Act 1988 (Cth)
22 Privacy Act, s 16A(2) 6D(4)(b)
23 Summary of obligations for pharmacists. Guidelines on Privacy in the Private Health Sector. Office of the Federal Privacy Commissioner; October 2001.
24 Privacy Act Schedule 3 NPP 6.1 (b), (c), (e)
24 Privacy Act Schedule 3 NPP 6.1 (g), (h)
26 Privacy Act Schedule 3 NPP6.1 (i), (k)
27 Pharmaceutical Society of Australia. Competency Standards for Pharmacists in Australia. Canberra: Pharmaceutical Society of Australia; 2003.
28 Federal Privacy Commissioner. Online. Available: www.privacy.gov.au/privacy_rights [accessed 2 June 2009]
29 New South Wales Law Reform Commission. Issues Paper 24. Minor’s consent to medical treatment: disclosure of and access to young people’s health information. 2004: 3
30 Breen v Williams (1995) 186 CLR 71
31 Malette v Shulman (1990) 2 Med LR 162
32 Civil Law (Wrongs) Act 2002 (ACT); Civil Liability Act 2002 (NSW); Personal Injuries (Liabilities and Damages) Act 2003 (NT); Civil Liability Act 2003 (Qld); Civil Liability Act 1936 (SA); Civil Liability Act 2002 (Tas); Wrongs Act 1958 (Vic); Civil Liability Act 2002 (WA)