Chapter 6 PALPABLE BREAST MASS
Approximately 190,000 new cases of breast cancer are diagnosed annually in the United States; however, most breast masses are benign. In order to diagnose these cancers, well over 1 million breast biopsies are performed each year. Fibroadenoma is the most common benign breast mass, whereas invasive ductal carcinoma is the most common malignancy.
If FNA is not possible during the initial presentation, ultrasonography should be considered to rule out cystic disease and delineate lesion margins.
Risk Factors for Breast Cancer
Personal history of breast cancer
History of benign breast disease, especially cystic disease, proliferative types of hyperplasia, and atypical hyperplasia
Family history of breast cancer in a first-degree relative or several second-degree relatives, especially if the cancer was diagnosed premenopausally
BRCA1 and BRCA2 gene mutations
Oral contraceptive use (may minimally increase risk)
Key Historical Features
✓ Change in relation to menstrual cycle
✓ Medical history, especially of the following:
✓ Obstetric and gynecologic history
✓ Medications and history of hormone therapy
✓ Family history, especially history of breast disease or ovarian cancer, age at onset, and relationship to the patient
✓ Carcinogen exposure, especially tobacco use, radiation exposure, and chemical exposure
Key Physical Findings
Suggested Work-Up
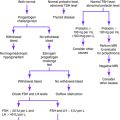
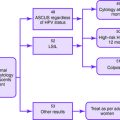
See the algorithm in Figure 6-1 for the management of a palpable breast mass. The triple test is discussed in the introduction to this chapter.
| Clinical breast examination | Best performed by a clinician 1 week after menses |
| Imaging | |
| Mammography | Recommended for routine screening of all asymptomatic women 40 years and older |
| Used for all women over age 40 with a solid mass, residual mass after cyst aspiration, or bloody fluid on cyst aspiration | |
| Ultrasonography | Useful to differentiate between solid and cystic breast masses when a palpable breast mass is not well seen on a mammogram |
| Especially helpful in young women with dense breast tissue when a palpable mass is not visualized on a mammogram | |
| Biopsy | |
| FNA | A 20- to 25-gauge needle is used to aspirate cystic fluid or sample solid lesions for cytologic study; if there is bloody fluid, or no fluid, the fluid or cells should be sent for cytologic analysis |
| Often the first step in evaluating patients with palpable breast masses | |
| Core-needle biopsy | A 14- to 18-gauge needle is used to sample a breast mass that is small or difficult to palpate |
| Produces a larger tissue sample than does FNA and may be used in conjunction with ultrasonography or stereotactic imaging for lesions that are small or difficult to palpate | |
| May be used when FNA result is nondiagnostic, when FNA result is benign but mammography yields positive results, or when FNA result is atypical or suspect; also may be used when FNA reveals cystic fluid that is bloody or if there is residual mass after cyst aspiration | |
| Useful in distinguishing atypical hyperplasia and ductal carcinoma in situ from invasive disease | |
| Excisional biopsy | The “gold standard” for evaluating breast masses |
| Indicated in patients with clinically suspicious lesions and lesions in which results of imaging or tissue studies are equivocal | |
Apantaku LM. Breast cancer diagnosis and screening. Am Fam Physician. 2000;62:596-602.
Esserman LJ. New approaches to the imaging, diagnosis, and biopsy of breast lesions. Cancer J. 2002;8(Supp 1):S1-S14.
Klein S. Evaluation of palpable breast masses. Am Fam Physician. 2005;71:1731-1738.
Morris KT, Pommier RF, Morris A, et al. Usefulness of the triple test score for palpable breast masses. Arch Surg. 2001;136:1008-1012.
Morris KT, Vetto JT, Petty JK, et al. A new score for the evaluation of palpable breast masses in women under age 40. Am J Surg. 2002;184:346-347.
Poggi MM, Harney KF. The breast. In: DeCherney AH, Nathan L, Goodwin TM, editors. Current Obstetrics & Gynecologic Diagnosis & Treatment. 10th. New York: McGraw-Hill; 2007:621-630.
Pruthi S. Detection and evaluation of a palpable breast mass. Mayo Clin Proc. 2001;76:641-648.
Steinberg JL, Trudeau ME, Ryder DE, et al. Combined fine-needle aspiration, physical examination and mammography in the diagnosis of palpable breast masses: their relation to outcome for women with primary breast cancer. Can J Surg. 1996;39:302-311. [Erratum in Can J Surg 1997;40:9.]