CHAPTER 12 Orbital blocks
Anatomy
Orbital cavity
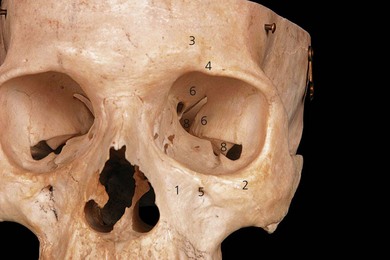
The superior orbital margin is formed by the frontal bone and contains the supraorbital foramen or notch, through which the superior orbital nerve emerges (Fig. 12.1). The inferior orbital margin is formed laterally by the zygomatic bone and medially by the maxilla. The roof of the orbit is formed by the frontal bone, the lateral or temporal wall by the zygomatic bone. The posterior wall of the orbit consists of the greater and lesser wings of the sphenoid bone. The orbital floor is formed by the maxilla, and the medial (nasal) wall of the orbit by the lacrimal bone and the orbital lamina of the ethmoid bone. The superior orbital fissure lies between the greater and lesser wings of the sphenoid bones, and the inferior orbital fissure lies between the maxilla and the superior wing of the sphenoid.
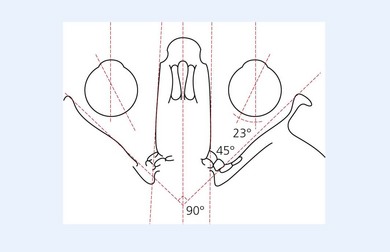
The medial walls of each orbit are parallel to each other (Fig. 12.2). The lateral or temporal wall of each orbit forms an angle of 90° to the contralateral lateral wall. The medial and lateral walls of the orbit make a 45° angle to each other. The floor of the orbit inclines at an angle of 10° anteriorly to posteriorly.
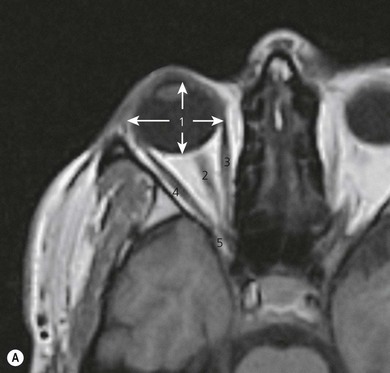
The A–P length of the orbit is 40–45 mm (Fig. 12.3) and the orbital volume is approximately 30 mL. The A–P diameter of a normal globe is 24 mm and the horizontal diameter is 23.5 mm. The globe lies eccentrically in the orbit, being displaced medially and superiorly.
Motor nerve supply
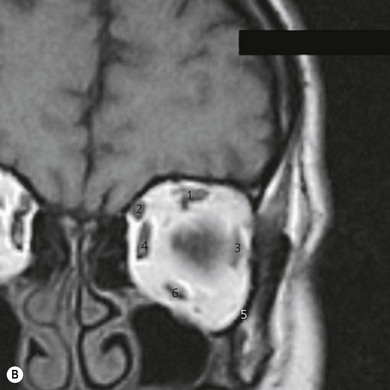
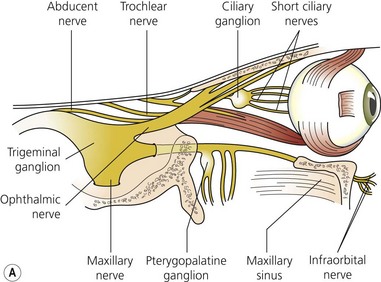
The motor nerve supply to the eye (Fig. 12.4) and surrounding structures comes from the cranial nerves. The third, fourth, and sixth cranial nerves supply the motor innervation to the recti muscles and partial motor innervation to the levator palpebrae superioris muscle. The seventh cranial nerve supplies motor function to the orbicularis oculi muscles. The parasympathetic nervous system supplies the circular muscle of the iris, while the sympathetic nervous system supplies the radial muscles of the iris and partial innervation to the levator palpebrae superioris muscle. The third, fourth, and sixth cranial nerves enter the orbit via the superior orbital fissure. The third cranial nerve (oculomotor) supplies all recti muscles with the exception of the lateral rectus muscle. The superior oblique muscle is supplied by the fourth cranial nerve (trochlear) and the lateral rectus muscle is supplied by the sixth cranial nerve (abducent). With the exception of the trochlear nerve, the motor nerves lie within the muscle cone formed by the four recti muscles. The nerves enter the muscle cone surrounding the optic nerve via the tendinous ring (annulus of Zinn).
Sensory nerve supply
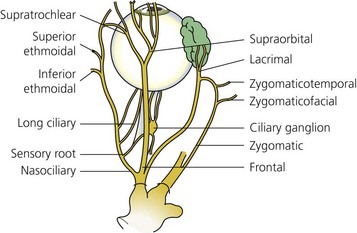
Sensory supply to the eye (Figs 12.4A and 12.5) and surrounding tissues is via the ophthalmic nerve, which is the first division of the trigeminal nerve. It supplies sensation to the eye, lacrimal gland, conjunctiva, part of the mucous membrane of the nose, skin of the nose, eyelids, forehead, and scalp. The ophthalmic nerve enters the orbit via the superior orbital fissure. It is the smallest division of the trigeminal nerve and arises from the anteromedial part of the trigeminal ganglion. Just before entering the superior orbital fissure it divides into three branches: the lacrimal, frontal, and nasociliary nerves.
Ocular muscles
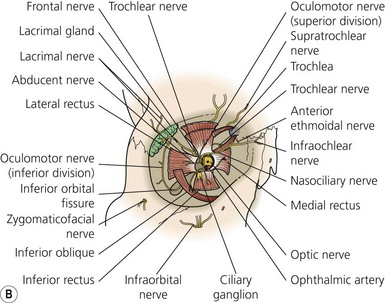
The muscles of the eyelids (Fig. 12.4B) include the levator palpebrae superioris and the orbicularis oculi muscles. The orbital muscles are the four recti muscles and the superior and inferior oblique muscles. The recti muscles arise from the semitendinous ring, which surrounds the optic canal. The muscles penetrate the fascial sheath of the eyeball (Tenon’s capsule) and are inserted in the sclera 5–6 mm posterior to the corneoscleral junction. The superior oblique muscle arises from the body of the sphenoid and, having traversed the trochlea, passes backward and is inserted into the sclera posterior to the equator. The inferior oblique muscle arises from the orbital surface of the maxilla medially and is inserted into the lateral part of the sclera behind the equator.
Tenon’s capsule (fascial sheath of the eyeball)
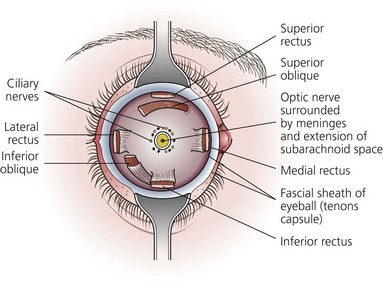
Tenon’s capsule (Fig. 12.6) is a thin membrane that envelops the eyeball from the optic nerve to the corneoscleral junction. It separates the eye from the orbital fat and forms a capsule within which the eye moves. It is separated from the sclera by the episcleral space. Tenon’s capsule is penetrated posteriorly by the ciliary vessels and nerves and fuses with the sheath of the optic nerve. Anteriorly, it fuses with the sclera just behind the corneoscleral junction. The tendons of the recti muscles penetrate the capsule anteriorly.
Surface anatomy
Extraconal retrobulbar and lateral peribulbar blocks
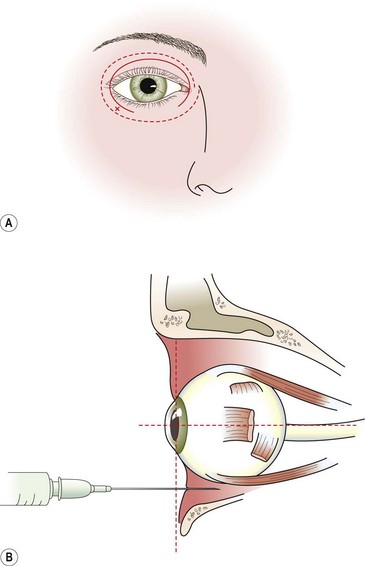
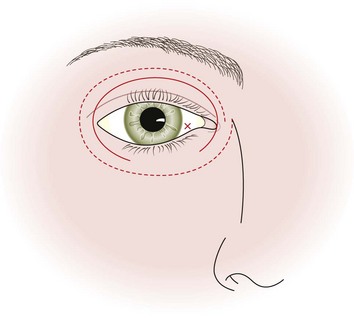
The needle insertion points for the extraconal retrobular (Fig. 12.7) and lateral peribulbar blocks are at the lowest margin of the inferior rim of the orbit. This approximates to the junction of the medial two-thirds and the lateral one-third of the lower lid. This will give the greatest distance from the globe and avoids the inferior rectus muscle.
Medial peribulbar block
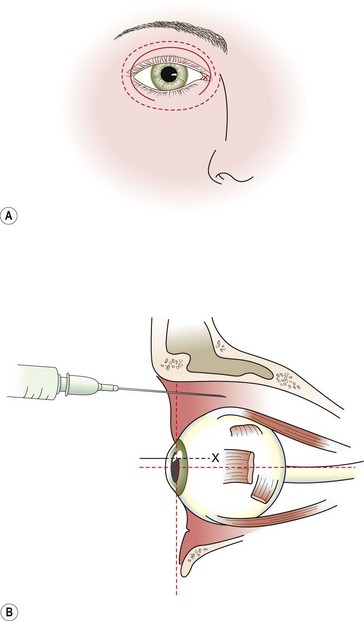
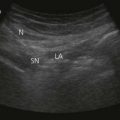
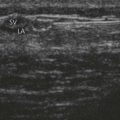
The plica semilunaris, which lies temporal to the caruncle, is the landmark for the medial peribulbar block (Fig. 12.8).
Adverse effects
Clinical pearls