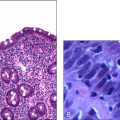
COMMON MALIGNANCIES
Approach to the patient
History
Ask about:
• initial presenting symptoms
• diagnostic investigations that have been carried out
• treatment received so far
• the patient’s risk factor profile
• exposure to carcinogens (quantification of the exposure may be necessary)
• past medical history (ulcerative colitis in patients with colonic carcinoma and cirrhosis in hepatic carcinoma)
• previous history of malignancy
• relevant family history
• relevant social habits (smoking, alcohol consumption, sexual promiscuity, sun exposure, asbestos exposure etc).
Treatment-related cancer is becoming common. Ask about immunosuppressive therapy, hormonal agents, past exposure to chemotherapeutic agents and exposure to radiation.
Enquire about chemotherapy, radiotherapy and surgery for the current diagnosis of cancer. Relevant information about chemotherapy includes the agents that have been used (if known), number of cycles the patient has had and is yet to have, any side effects experienced and the response to therapy. Ask about early side effects such as hypersensitivity, nausea, vomiting and oral mucositis, and how these side effects were managed. Other side effects such as hair loss, sepsis due to immunosuppression, debility, fatigue as well as organ-specific toxicity (pulmonary toxicity, hepatotoxicity, cardiotoxicity and bladder toxicity) should be enquired into.
Ask about sperm or ova harvesting in the young patient who has been treated with agents having gonadal toxicity. Ask about adverse effects associated with other therapeutic modalities, such as radiotherapy and surgery. Enquire about the patient’s insight into his or her condition and what expectations they have for the future.
Ask about pain and how it is managed. Ask whether the patient is depressed. Try to gain an insight into their social support network. Check how the patient is coping and whether any professional psychological help has been received.
Examination
1. Look for cachexia, alopecia, cushingoid body habitus, flat affect and any vascular access devices (e.g. Hickman catheter).
2. Look for radiation dermatitis, radiation burns, radiation tattoos (markings of the radiotherapy field) and surgical scars.
3. Look for organomegaly, particularly in the abdomen, lymphadenopathy and bone tenderness.
4. Define all mass lesions by quoting the exact measurements. With mass lesions, describe the consistency, fixation, mobility of skin above the lesion, temperature and shape.
5. Perform a detailed neurological examination to exclude deficit due to cord compression, cerebral metastases, paraneoplastic phenomena and neurotoxic chemotherapy.
6. Look for evidence of pneumonitis or pulmonary fibrosis in those who have received pulmonary toxic agents, such as cyclophosphamide or busulphan, as well as those who have received thoracic radiotherapy.
7. Check for evidence of cardiac failure in those who have been treated with cardiotoxic agents, such as the anthracyclines.
Investigations
Investigations should be tailored according to the clinical presentation, location of the malignancy, type of malignancy and the spread. Radiological imaging (X-ray, CT or MRI scan), basic blood tests (full blood count, electrolyte profile), invasive tests (e.g. endoscopy), organ-specific functional tests and tumour markers are other investigations of relevance.
Imaging tests help define the tumour and the staging process. Biopsy and anatomical pathology is important for defining the diagnosis and grading the cancer.
The candidate should be able to discuss the different investigations that need to be performed in the initial diagnostic work-up as well as in the staging process of different cancers.
Curative and palliative management
In discussing therapeutic options, the candidate should demonstrate a good working knowledge of chemotherapy, radiotherapy and surgical management. The candidate should be thoroughly familiar with the different means of monitoring for chemotherapy toxicity and the preventive and remedial steps that have to be taken.
Assess the patient’s performance status, as this has significant influence on the choice of therapy. Performance status is usually described according to the Eastern Cooperative Oncology Group (ECOG) classification system (see box overleaf) or Karnofsky Performance Scale. Patients who score poorly on these scales have poor tolerance to chemotherapy, and consideration should be given to the palliative options. It is important to possess some knowledge of the principles of palliative care, pain management and care of the terminally ill. Suitable patients should be referred to a palliative care service early in the management. Patients with terminal cancer should be referred to a community outreach palliative care service, which would work in liaison with a hospice facility. Hospice care is indicated for patients living in the community or discharged to the community but who require ongoing nursing care and have a life expectancy of less than 6 months. Following is a discussion on the different cancer types likely to be encountered in the long case setting.
ECOG (Eastern Cooperative Oncology Group) Performance Scale
0. Active with no restriction of performance.
1. Ambulatory and able to attend to light work activity. Unable to carry out strenuous physical activity.
2. Can manage self-care but unable to attend to any form of work activity. Ambulatory for more than 50% of the time while awake.
3. Can manage only limited amount of self-care. Bed-bound for more than 50% of the time while awake.
4. Disabled, with complete inability to attend to self-care. Completely bed bound.
(Adapted from Oken M M, Creech R H, Tormey D C et al 1982 Toxicity and response criteria of the Eastern Cooperative Oncology Group. American Journal of Clinical Oncology 5(6):649–655)
(Adapted from Oken M M, Creech R H, Tormey D C et al 1982 Toxicity and response criteria of the Eastern Cooperative Oncology Group. American Journal of Clinical Oncology 5(6):649–655)
BREAST CANCER
Case vignette
A 35-year-old woman presents with a painless, hard and immobile lump in her left breast. She has a family history of breast cancer, with her mother having been treated with mastectomy at the age of 56. Since the initial presentation she has had multiple tests and doctors have planned curative treatment. After definitive primary surgery she has had one cycle of chemotherapy so far. She has experienced distressing side effects and is currently feeling very debilitated and depressed.She has taken 3 months off from her job as a computer analyst and she has a 3-year-old daughter who is cared for by her partner.
The current screening recommendation for breast cancer surveillance is for all women between the ages of 50 and 70 to have a mammogram every 2 years. A discovery of a suspicious lump on palpation should be followed up with mammography, to further assess its anatomy and pattern of calcification, and ultrasonography, to define its consistency (cystic or solid). This should be followed up with fine-needle aspiration biopsy or core biopsy to obtain a tissue diagnosis. A thorough physical examination should be carried out to exclude any additional lumps in either breast, axillary lymphadenopathy, lymphadenopathy elsewhere, hepatomegaly and bone tenderness. If the lesion is confined to the breast alone, no staging is necessary, or minimal staging is carried out with chest X-ray and liver function tests (especially looking for an elevation of the alkaline phosphatase level) for apparent early disease. If there is evidence of significant nodal involvement at surgery, further staging investigations should be carried out. These include a bone scan and an ultrasound or CT scan of the liver, in addition to chest X-ray and liver function tests.
Management
Management of localised breast cancer is dependent upon the patient’s age, menopausal status, tumour size, axillary lymph node status, hormone receptor status and expression of protein HER2. Localised breast cancer with positive expression of protein HER2 benefits from treatment with humanised monoclonal antibody trastuzumab (Herceptin®). Patients with axillary-node-positive breast cancer should receive adjuvant systemic therapy upon complete local resection of the primary tumour. Premenopausal women have low rates of hormone receptor/protein-positive tumour, and therefore have better response to adjuvant chemotherapy. Older/postmenopausal patients are more likely to express hormone receptors and therefore be more responsive to hormonal therapy; however, they are also less likely to respond to chemotherapy.
Early-stage disease
Locally confined disease can be managed with breast-conserving surgery and radiotherapy, or modified radical mastectomy. Adjuvant therapy in early-stage disease may be either systemic chemotherapy or hormonal therapy. Treatment with adjuvant chemotherapy is dependent on the lymph node status, tumour size, histology of the tumour, hormone receptor status, and age and menopausal status of the patient.
Premenopausal patient
• Hormone-receptor-negative tumour is treated with adjuvant chemotherapy. The agents of preference include taxanes and anthracyclines. Trastuzumab can be given together with cytotoxics in node-positive tumours; however, when combined with anthracyclines, significant cardiotoxicity should be watched for.
• Hormone-receptor-positive tumour is treated with chemotherapy together with ovarian ablation or tamoxifen for a period of 5 years. With tamoxifen therapy it is important to be vigilant for ocular and endometrial side effects.
Postmenopausal patient
• Hormone-receptor-negative tumour is treated with adjuvant chemotherapy or radiotherapy.
• Hormone-receptor-positive tumour is treated with aromatase inhibitors or tamoxifen with or without cytotoxic chemotherapy. Follow-up after curative therapy for early-stage disease includes regular physical examination together with yearly mammography.
• HER2-positive disease is treated with trastuzumab.
Advanced-stage disease
Advanced-stage cancer could be locally advanced large tumours, those with significant nodal or cutaneous spread, recurrent cancer or metastatic disease. A decision to treat aggressively in a patient with good performance status who has locally advanced tumour would require multimodality combination therapy. This would include induction chemotherapy followed by loco-regional therapy in the form of surgery and/or radiotherapy. Inflammatory breast cancer is another form of locally advanced breast cancer that requires aggressive systemic and loco-regional therapy. High-dose chemotherapy with autologous stem cell transplantation has not shown any significant benefit over conventional therapy, and should therefore be considered only in the setting of a clinical trial. Younger patients with oestrogen-receptor-positive disease may benefit from oophorectomy or chemical castration with luteinising hormone receptor agonists. Other options of therapy in metastatic disease include tamoxifen, palliative chemotherapy or combination therapy.
For the older patient with receptor-positive metastatic disease, the management options include tamoxifen, aromatase inhibitor therapy or single-agent palliative chemotherapy with an agent such as mitozantrone. The postmenopausal patient with receptor-negative metastatic disease may benefit from palliative chemotherapy. Radiotherapy is indicated in this setting for pain management.
Screening of relatives
Screening of other first-degree female relatives of a young patient with breast cancer is a contentious issue and may be a subject of discussion at the examination. The implications of such screening should be discussed with the family members and the choice should be offered, if appropriate.
The cosmetic effects of mastectomy may be distressing, and options available to address such situations (e.g. breast reconstruction surgery) should be offered to the patient.
CARCINOMA OF UNKNOWN PRIMARY
Case vignette
A 58-year-old man has been hospitalised with fevers, rigors and severe mucositis. He has presented initially with a newly discovered lump above his left clavicle, which has grown in size rapidly. Upon biopsy, a diagnosis of cancer has been made and he has had multiple further tests. He has been told that the primary site of his cancer remains unknown, despite extensive investigation. He has had two cycles of chemotherapy so far, and has just completed the second cycle 4 days ago. He has recently retired from his job and has been planning to move back to Europe, where the rest of his family live.
An occult primary malignancy can manifest as metastases discovered incidentally for the first time in the lymph nodes, bone, liver or lung. Diagnosis is made by biopsy of the lesion. Further investigations to ascertain the origin of the tumour are directed at excluding potentially curable disease and deciding on appropriate treatment for symptomatic disease. Using the relatively novel techniques of immunohistochemistry, molecular genetics and electron microscopy, more precise characterisation of the origin of the tumour may be possible. Some immunoperoxidase tumour markers that help define the possible primary site of the cancer include vimentin for mesenchymal sarcoma, desmin for rhabdomyosarcoma, oestrogen or progesterone receptor status for breast cancer, prostate-specific antigen (PSA) for prostate cancer, S-100 or HMB-45 for malignant melanoma, and cytokeratin for squamous cell carcinoma.
The level of tumour differentiation has significant diagnostic and management implications. Elevated levels of tumour markers in the blood may give further clues to the origin of the tumour. Some such markers are CA125 for ovarian cancer, CA19-9 for cholangiocarcinoma, alpha-fetoprotein (AFP) for testicular carcinoma and hepatoma, and human chorionic gonadotrophin (hCG) for testicular carcinoma and choriocarcinoma. But the usefulness of these markers in the initial diagnostic process is questionable. They are more useful for the monitoring of tumour response to treatment.
Adenocarcinoma at different levels of differentiation is the most common pathological diagnosis in patients presenting with carcinoma of unknown primary site. Commonly, the origin will be in the lungs or the gastrointestinal tract, but an exhaustive search for the primary site is often not useful.
In the assessment process, in addition to a thorough history, physical examination and basic haematological and biochemical tests, PSA level should be checked in the male patient and a mammography should be performed in the female patient. All patients should have urine analysis and a chest X-ray performed. Other investigations should be performed as guided by the patient’s symptoms and signs. Most patients with this condition have a very poor prognosis, with life expectancy limited to a few months. However, some patients may respond favourably to chemotherapy, so this option should be given serious consideration.
Poorly differentiated carcinoma is the next most common pathology identified in patients presenting with carcinoma of unknown primary site. The patient may be relatively young and present with rapid progression of the disease. In addition to routine haematological and biochemical investigations, the patient should have a chest X-ray as well as CT of the thorax and abdomen, looking for mediastinal and retroperitoneal disease. Serum levels of hCG and AFP should be assessed to exclude germ cell tumour in the young male patient. These patients always warrant a trial of chemotherapy, as some (mostly those treated with platinum-based or taxane-based combined chemotherapy regimens) may show significant disease response and improvement of the clinical status.
CARCINOMA OF THE PROSTATE
Case vignette
A 61-year-old man has been admitted to the hospital with dyspnoea. He has a background history of acute myocardial infarction and significant heart failure. He was also diagnosed with prostate carcinoma 1 year ago and has been treated with radiotherapy. He has experienced multiple local complications from this. He has been told that he had localised disease and has been cured of his malignancy. Examination reveals stony dullness all over his left hemithorax posteriorly. Chest X-ray shows a complete white-out of the left lung.
1. Discuss his prognosis, taking into account the current clinical findings, his cardiac condition and the possible differential diagnoses.
2. How would you monitor for recurrent disease in prostate cancer. In cases of recurrence, what management is optimal?
3. What complications could he have had with radiotherapy?
4. What is the role of androgen blockade in prostate cancer management?
Approach to the patient
History
An older patient with multiple medical problems may also have a diagnosis of prostate cancer. In such a situation it is important to identify the relative importance of the prostate cancer in the patient’s clinical context. Ask about the initial diagnosis and the presenting symptoms. Some patients may present with prostatic symptoms such as frequency, urgency, hesitancy, urinary retention, or with urinary tract infection.
Enquire about the biopsy process and complications such as haematuria. Enquire about the different treatment protocols the patient has had, including prostatectomy. Ask about side effects such as incontinence, impotency and the management of them. Patients may complain about refractory bone pain. Check the patient’s mood and also the support structure that is in place. Ask how the patient is monitored for recurrence with regular assessment of serum PSA level.
Examination
Initial diagnosis is made by digital per rectum examination or measurement of serum PSA levels (case finding). In the physical examination look for surgical scars and radiotherapy tattoos. Do not forget to look for gynaecomastia and bone tenderness.
At the first presentation on clinical diagnosis, a transrectal biopsy is performed for histological diagnosis; however, this has limited sensitivity and therefore a series of core biopsies from multiple sites is preferred. Serum PSA level should be assessed in all patients, as its level correlates well with the extent of the disease. Other investigations in this setting include renal function indices, looking for any obstructive nephropathy, and IV pyelography, looking for irregularity of the prostatic urethra and dilatation of the renal pelvi-caliceal system. Staging investigations include, in addition to serum PSA level, pelvic CT scan, looking for local spread, and a three-phase radioisotope bone scan, looking for occult bony metastases. Staging is done according to the TNM (tumour, lymph nodes, metastases) classification system.
Investigations
1. Full blood count, electrolyte profile and renal function indices
2. Serum PSA level
3. Transrectal ultrasound
4. Intravenous pyelogram
5. Abdominal and pelvic CT (for staging)/MRI
6. Chest X-ray
7. Radioisotope bone scan
8. Core biopsy and staging biopsy
9. Most prostatic tumours are adenocarcinomas. Histological grading of the tumour has significant prognostic implications. Grading is interpreted according to the Gleason score (see box).
Gleason histological grade of prostate carcinoma
Grade 1—Well-differentiated tumour with a uniform glandular pattern
Grade 2—Well-differentiated tumour with glandular tissue of varying shape and type
Grade 3—Moderately differentiated tumour
Grade 4—Poorly differentiated tumour
Grade 5—Very poorly differentiated tumour with minimal or no glandular tissue formation
Management
Early disease
Clinical as well as pathological staging will determine the appropriate therapeutic approach. Other factors that influence the management approach include the patient’s functional capacity, age, other comorbidities and patient expectations.
Management of carcinoma of the prostate is complicated because opinions vary widely among the experts. The treatment options include radical prostatectomy, radical radiation therapy or active surveillance. However, most believe that localised disease should be treated aggressively with a curative intent. Radical radiotherapy, radical surgery or a combination is indicated for patients with disease confined to the prostate within the capsule with no lymph node metastases. Radiotherapy could be administered as external beam or brachytherapy. Complications associated with radiotherapy include bladder irritation, proctitis, impotence, diarrhoea, dysuria and severe perineal cutaneous reaction and, in the long term, urethral stricture formation. Complications of radical surgery include permanent impotence (in 90% of patients), urinary incontinence and, very rarely, rectovesical fistula formation. There is an operative mortality of less than 5%.
Active surveillance is preferred in elderly patients with multiple other medical problems. This process involves digital rectal examination and serum PSA assessment at regular intervals (usually every 3 months initially) and occasional re-biopsy. Detection of an abnormality indicating progression of disease would warrant active treatment.
Advanced disease
Locally advanced disease and recurrent disease together with metastatic disease have a worse prognosis. Palliative management of widespread disease is with androgen deprivation therapy and radiotherapy for painful bony metastases. Androgen deprivation also helps reduce bone pain and also effect some primary and secondary tumour regression. Even hormone-responsive tumours may become hormone refractory after a period of time (usually within 2 years). Attempts at managing hormone-resistant disease can be made with palliative radiotherapy, IV strontium-89 and chemotherapy with mitozantrone.
Hormonal therapy is the option for those not suitable for radical therapy and those with metastatic disease. This involves surgical or pharmacological castration together with antiandrogen therapy. The objective of this form of therapy is total androgen blockade (to block gonadal as well as adrenal androgen production). Pharmacological castration is achieved by the administration of luteinising hormone-releasing hormone agonist agents such as luprelide or goserelin. Concurrent administration of a non-steroidal antiandrogen drug such as flutamide (also bicalutamide/nilutamide) helps prevent the exacerbation of bone pain associated with the commencement of the luteinising hormone agonist. Cyproterone acetate is a steroidal antiandrogen that has also shown to be beneficial in this regard. With this form of palliative therapy, the patient’s survival could be expected to be around 3 years.
Hormonal therapy has side effects that need to be discussed with the patient. Many patients suffer from sexual dysfunction, gynaecomastia and hot flushes. Counselling the patient as well as the partner and offering support is important. Another significant side effect is osteoporosis and pathological fracture, which needs preventive therapy with vitamin D, calcium supplements and bisphosphonates.
Patients with hormone-therapy-refractory advanced prostate cancer may benefit from antiandrogen withdrawal, antifungal agent ketoconazole, corticosteroids or chemotherapy with docetaxel-based regimens.
CARCINOMA OF THE LUNG
Case vignette
A 69-year-old man presents with fevers, rigors and a productive cough. He reports significant weight loss over the preceding 3 months. He also complains of dry mouth, erectile dysfunction and progressive severe proximal muscle weakness. He has a history of chronic airways limitation and intermittent claudication. He has a significant smoking history. He also consumes 2–4 standard drinks of alcohol each day. On examination he has bronchial breath sounds in the left upper zone and a fixed inspiratory and expiratory wheeze. His sputum mug shows purulent sputum with large amounts of fresh blood.
A long case patient with a significant smoking history may present with chronic airways limitation, ischaemic heart disease and peripheral vascular disease, together with a recent diagnosis of lung cancer. As with prostate cancer, an important basic knowledge of the management of lung cancer will help you identify the stage of disease and decide on the relevant management plan.
Investigations
For the purpose of diagnosis of lung cancer, the following tests should be performed:
1. Chest X-ray
2. Flexible fibreoptic bronchoscopy and biopsy of the lesion
3. Fine-needle aspiration biopsy of the lesion if it is not accessible by bronchoscopy
4. Thoracoscopic or open biopsy of the lesion, if the above methods are not feasible
5. Sputum cytology may be useful, but usually its sensitivity is very low.
The following additional investigations should be carried out for the purpose of staging the disease:
Management
Non-small-cell lung cancer
For non-small-cell cancer of stages I and II, where the disease is confined to the lung or has spread only to ipsilateral peribronchial or hilar lymph nodes, surgical intervention in the form of lobectomy or pneumonectomy is indicated as a curative measure. Upon curative therapy, patients need surveillance every 3 months, with clinical assessment and a chest X-ray if indicated, for 2 years, and thereafter every 6 months for up to 5 years. Screening should continue annually thereafter.
In stage IIIA disease, where there is involvement of the mediastinal or subcarinal lymph nodes or there is spread to the chest wall, pleura or pericardium, management involves a combination of surgery, radiotherapy and chemotherapy. Locally advanced disease (IIIB) is usually treated with radiotherapy and chemotherapy.
For stage IV disease with systemic metastases, treatment objectives are best supportive care, palliation and prolongation of life. The patient’s performance status is crucial in the choice of best palliative modality. Double- or single-agent palliative chemotherapy is indicated, based on performance status. Patients with better performance status benefit from doublet chemotherapy (cisplatin with another agent). With this therapy, life expectancy can be marginally improved, with some preservation of quality of life.
Chemotherapeutic agents that can be used in this situation include cisplatin, taxanes, gemcitabine, vinorelbine or camphothecin.
Small-cell lung cancer
Small-cell lung cancer behaves in a very aggressive manner—it has a rapid doubling time and a propensity to spread widely within a very short period of time. Small-cell lung cancer is staged as either limited disease, where the disease can be encompassed in a single radiation field, or extensive disease, where there is metastatic disease or the involvement of the contralateral supraclavicular nodes, pleural effusion or pericardial effusion. This tumour is highly responsive to chemotherapy as well as radiotherapy. However, terminal and therapy-refractory recurrence happens within the first 2 years. Limited-stage disease is usually treated with a platinum-based agent and etoposide, where the life expectancy is expected to increase to about 18 months. The untreated patient has an average life expectancy of 9–12 months. In addition, the patient should be offered mediastinal radiotherapy and prophylactic cranial irradiation. Metastatic disease, too, can be treated with palliative gentle chemotherapy, but the prognosis is usually grave. Many patients may also manifest paraneoplastic syndromes with neurological features (e.g. Lambert-Eaton myasthenic syndrome), SIADH or Cushing’s syndrome.
CANCER OF THE COLON
Case vignette
A 74-year-old female presents with progressive exertional dyspnoea, weight loss and prolonged constipation followed by watery diarrhoea over a period of 2 months. She has also noted blood in her bowel motions. She has been well until the development of the current symptoms. She is not on any regular medications and denies any allergies or significant past medical history. She is the main carer of her husband, who has progressive Alzheimer’s disease.
Approach to the patient
History
Colon cancer is a common malignancy and a leading cause of death. Ask about the initial presentation. Most patients present with abdominal discomfort of varying degree, altered bowel habits (chronic constipation followed by spurious diarrhoea), melaena and per rectal bleeding. The patient may also have constitutional symptoms of malignancy, such as weight loss, weakness and lethargy, and features secondary to anaemia. Significantly advanced disease can present with bowel obstruction, bowel perforation or neurological symptoms due to the spread to the pelvic nerves. Advanced cancer can also present with regional lymphadenopathy or hepatic metastasis. Check for any family history of colon or other cancer. Familial adenomatous polyposis and hereditary non-polyposis colon cancer are genetic risk factors for colon cancer with an onset at a younger age. A history of ulcerative colitis is a definite risk factor for colonic cancer. Other risk factors include high alcohol consumption, obesity and diabetes. Ask about staging investigations and treatment so far. Ask how the patient manages the colostomy if relevant.
Examination
Look for evidence of generalised wasting, cachexia and features of anaemia. Perform a thorough abdominal examination and clearly define any mass lesions by location, magnitude, mobility and consistency. Exclude hepatomegaly and ascites. Look for lymphadenopathy by drainage zone. Look for obvious or occult blood in the rectal examination. Look for pigmented lesions in the buccal mucosa that may suggest Peutz-Jeghers syndrome, which is a risk factor for colon cancer. Look in the colostomy site for evidence of inflammation or infection.
Investigations
1. Full blood count, electrolyte profile, liver function tests (especially alkaline phosphatase (ALP) level), iron studies
2. Colonoscopy and biopsy/double contrast barium enema/sigmoidoscopy
3. Transrectal ultrasound—for evaluation of the degree of local invasion and local lymph node spread
4. Fine-needle aspiration biopsy—for detection of lymph node spread
5. CT scan of abdomen and pelvis
6. MRI or PET scans—may help in more occult disease
7. Chest X-ray—looking for metastasis
8. Serum carcinoembryonic antigen (CEA) and CA19-9 levels—particularly useful in prognostication of new diagnoses and monitoring of recurrence
9. Supine and erect abdominal X-rays in case of perforation/obstruction
10. Intraoperative evaluation for metastasis
Management
Management depends on the tumour stage (see box). Locally confined disease can be treated with surgery (hemicolectomy) with a curative intent. Isolated liver or pulmonary metastasis too may be amenable to curative surgery. Node-positive disease benefits from adjuvant chemotherapy with 5-fluorouracil (5-FU) or a combination of 5-FU with leucovorin and oxaliplatin. Neoadjuvant chemotherapy (with 5-FU) and radiotherapy has a potential role in rectal carcinoma prior to curative resection. Metastatic and advanced cancer may benefit from palliative surgery and/or chemotherapy.
CANCER OF THE HEAD AND NECK
Cancers of the head and neck are common among heavy smokers and those who abuse alcohol. They are staged according to the TNM staging system.
Early-stage disease (stage 1 and stage 2) can be treated with radiotherapy or surgery. Decision on the therapeutic modality is influenced by the performance status of the patient and the anatomical site. Where preservation of the architecture and organ function is required, radiotherapy may be preferred over surgery.
Advanced-stage disease (stage 3 or stage 4) should be treated with concurrent chemotherapy, radiotherapy and/or surgery in combination. Chemotherapy agents commonly used in the treatment of cancer of the head and neck are cisplatin and 5-FU.
All patients with cancer of the head and neck should have panendoscopy performed, to look for other primary lesions in the vicinity.