Chapter 35 Mental Health in the Wilderness
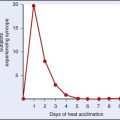
Wilderness environments often have beneficial effects on the overall emotional health of many individuals. Individuals who choose to pursue wilderness activities are often seeking relief from the stress of their hectic urban lives (Figure 35-1). However, remote wilderness environments can present unique stresses of their own. Mental health and mental health problems might improve in the wilderness, but psychiatric problems can emerge or become worse in response to the demands of wilderness experiences. This chapter discusses the diagnosis and management of emotional problems in the wilderness, including the use of psychotropic medications, both in people who have preexisting psychological difficulties and in those who develop new emotional problems in the wilderness.
The Diagnostic and Statistical Manual of Mental Disorders, fourth edition, text revision1 (DSM-IV-TR) is the most recent and widely used compendium of the nosology of psychiatric disorders. Most mental health problems can be thought of as falling into six broad groups of disorders: (1) anxiety disorders; (2) mood disorders; (3) psychotic disorders; (4) organic mental disorders; (5) personality disorders; and (6) substance abuse disorders. Specific diagnostic assessment with the use of the DSM-IV-TR and psychological testing in a wilderness setting is not practical. Appropriate triage and management in a wilderness setting depends on classifying emotional and behavioral problems as falling into one or more of these broad categories. Separating normal from abnormal human behaviors is the first step in the triage of emotional problems. It is not straightforward to differentiate what may be considered an adaptive response to the challenge of a wilderness experience from responses that are maladaptive and signal the onset of new emotional problems or the exacerbation of preexisting psychiatric problems. For example, at the end of a physically challenging day of backpacking with a group, one member of the group breaks down in tears. Such crying may be a healthy and adaptive response, or it may be a sign of depression or panic. The process of crying can relieve stress and result in the tearful backpacker receiving needed emotional support. Alternatively, such tears may suggest that the person feels mentally and physically overwhelmed. The person might be approaching a panic state, and, if appropriate interventions are not undertaken, the person’s mental state will deteriorate. The challenge is to determine whether a pat on the back and some encouraging words are all that are needed or if the individual has to be assisted out of the wilderness to prevent further emotional deterioration. In the following sections, four important topical areas for assessment and management of emotional problems in the wilderness are discussed: (1) the common characteristics of the six major categories of psychiatric disorders; (2) suicide and violence potential; (3) psychosomatic complaints; and (4) response to crisis (i.e., disasters and survival psychology). At the end of the chapter, Table 35-1 summarizes the triage of psychiatric problems in the wilderness.
TABLE 35-1 Mental Health Triage in the Wilderness
| Anxiety disorders | Provide reassurance, support, and lorazepam |
| Mood disorders, mild | Provide support and encouragement |
| Mood disorders, severe (e.g., mania, suicidal ideation, violence) | Observe constantly, contain or restrain, give lorazepam and haloperidol, and evacuate |
| Psychotic disorders | Observe constantly, contain or restrain, give lorazepam and haloperidol, and evacuate |
| Organic mental disorders | Identify the cause and eliminate it if possible, observe constantly, contain or restrain, give lorazepam and haloperidol, and evacuate |
| Personality disorders, mild | Avoid overreacting to annoying behaviors and intercede to prevent conflicts within the group |
| Personality disorders, severe (e.g., violence, extreme behaviors) | Expel the individual from the group if possible or obtain assistance and terminate the outing |
| Substance abuse (i.e., no delirium or psychosis) | Confiscate drugs and alcohol |
| Substance abuse or withdrawal, severe (e.g., unstable vital signs, delirium, psychosis) | Give lorazepam for withdrawal and haloperidol for psychosis or delirium, observe constantly, contain or restrain, and evacuate |
| Suicidal or violent behaviors | Observe constantly, contain or restrain, give lorazepam and haloperidol, and evacuate |
| Somatic symptoms of psychological origin | Exclude an organic cause and provide support, reassurance, and firm expectations |
| Disasters and post-traumatic stress disorder | Ensure physical and psychological security and safety, provide support, and discuss the disaster as guided by the victim |
| Wilderness survival | Stop, take time to develop a plan, attend to physical security (e.g., shelter, warmth, water), and avoid panic |
Psychiatric Disorders
Anxiety Disorders
The several types of anxiety disorders include generalized anxiety disorder, specific phobias, panic disorder, obsessive–compulsive disorder (OCD), and acute and post-traumatic stress disorder (see Response to Crisis, later). People with generalized anxiety disorder worry a lot. Their anxiety is out of proportion as compared with what most people would experience in similar circumstances. The afflicted individual may find it difficult to keep worrisome thoughts from interfering with attention that needs to be paid to current activities. The focus of the worries among people with generalized anxiety disorders are mundane and include such concerns as getting up on time for work, making appointments, and doing chores. These individuals experience somatic symptoms, such as sweating, nausea, and diarrhea. The prevalence of generalized anxiety disorders is approximately 1.5%.5 In a wilderness setting, the foci of worries might be bear attacks, getting lost, not keeping up, flash floods, and so forth. These anxieties will likely diminish the person’s enjoyment of a wilderness experience, affect his or her concentration, and drain his or her energies. People with generalized anxiety may negatively affect group morale. However, generalized anxiety problems are not emergencies; they are chronic problems that can be managed in the field. People with a generalized anxiety disorder require ample reassurance. A good leader can provide reassurance and appoint other group members to assist with reassuring the anxiety-ridden individual.4 Building rapport and trust with the afflicted person is a good first step to helping them. Trying to talk someone out of his or her worries is unlikely to be productive. In the field, a benzodiazepine (e.g., 0.5 to 2 mg of lorazepam two to three times a day) can be useful.11 Side effects include sedation, memory difficulties, and impairment of motor coordination. Sustained benzodiazepine use can lead to physical dependence and withdrawal symptoms with abrupt discontinuation. Thus, such medications must be used cautiously in the field, but they can provide short-term relief of anxiety-related symptoms.
Probably one of the more common specific phobias encountered during a wilderness outing is a fear of heights or exposure (e.g., to an edge with a drop-off). Other common phobias are to snakes, spiders, and water. A specific phobia is an unreasonable fear in anticipation of or on exposure to a particular object or situation.1 The intensity of anxiety with the exposure may vary from relatively mild to extreme panic. In some instances, phobias to heights cannot be overcome in the wilderness. For instance, a trail that crosses a bridge over a chasm or that involves a section of precipitous exposure might be more than can be managed by an individual with a specific phobia to heights. I have personally guided people who were so terrified of exposure that they were unable to complete some trails. Sometimes, gentle reassurance or distraction may be all that is required. Engaging height-phobic people in distracting conversations while backpacking in areas that involve dizzying exposure can be successful. However, if an individual is likely to respond with extreme anxiety and become unbalanced, then it is not safe to use such psychotherapeutic measures.
Panic disorders occur in approximately 1.6% to 5% of the population.5 Treatment with selective serotonin reuptake inhibitors (e.g., fluoxetine, sertraline) or benzodiazepines (e.g., alprazolam, clonazepam) or with a combination of the two and with psychotherapeutic intervention can be successful for controlling panic disorder and agoraphobia.5 People with panic disorder whose symptoms are not problematic may safely enjoy a wilderness adventure without difficulty. However, remote locations, bad weather, or physical challenges may increase the stress on such individuals, thereby causing them to experience a resurgence of symptoms. Having panic attacks in the wilderness may precipitate agoraphobia. The afflicted person may want to escape from the wilderness, and he or she may be completely intolerant of being left alone, even for brief periods.
Obsessive–Compulsive Disorder: Repetitive Behaviors
A person with OCD may not be able to adhere to the requirements of a wilderness trip. For instance, the chronic hand washer may slow a group so profoundly that the group cannot make reasonable progress. The example of the person who tries to control his or her anxiety about acting violently by counting may present less of a problem. People with OCD are not typically violent, but a person who is observed to be constantly counting to ward off violent behaviors may have difficulty fitting in with a group. In the general population, the prevalence of OCD is 1% to 2.5%.5 People with OCD are often successfully treated with clomipramine and psychotherapy.5 It is unlikely that OCD symptoms will appear suddenly on a wilderness trip. Frank disclosure to a wilderness group about the OCD symptoms of a member of the group can diminish the group’s anxieties about the person’s odd behaviors and make the afflicted person less likely to be isolated by the group.
Mood Disorders
Depressed people have difficulty sleeping, lose their appetites, have poor energy levels, lose concentration, withdraw socially, cry for no reason, and have difficulty enjoying anything. The most common diagnostic term for this type of depression is major depression; the prevalence of this disorder is approximately 2.5% to 10%.5 At their worst, people with severe depression may become psychotic and suicidal (see Suicide and Violence Potential as well as Psychotic Disorders, later).1 People who are having mild problems are unlikely to develop severe symptoms rapidly, because severe symptoms gradually appear over a period of weeks or months. The more likely problem on a wilderness adventure is finding someone who started out with mild symptoms that are becoming worse. Such individuals may already be taking antidepressant medications (e.g., citalopram, paroxetine). These medications work slowly over a period of weeks, so a change in dose in the midst of a wilderness trip probably would probably not provide significant benefit. The most common problem that the wilderness group may face with a depressed person is that person’s overall impact on group morale. Emotional outbursts, crying for no apparent reason, and offhand comments about suicide will likely concern and distress others in the group. If group members provide encouragement and emotional support, this may help the depressed person to get through the trip safely. However, severe symptoms may not respond to ordinary support. A lack of response can anger others, who may begin to feel conflicted, because they recognize that they are punishing someone who is already suffering. As the symptoms grow worse, it may become necessary to hasten the depressed person’s departure from the wilderness, especially if there is suicidal ideation.
Individuals with bipolar disorder experience episodes of major depression that alternate with periods of mania over a period of months, often with normal functioning occurring between the abnormal episodes. The prevalence of bipolar disorder is approximately 1%.5 During periods of normal mood or during the early stages of a manic phase (i.e., hypomania), bipolar persons may participate in wilderness adventures with no difficulty. During a period of hypomania, a person is very positive, productive, hardworking, energetic, and expansive. However, as the person becomes manic, problems become readily apparent. There is often rapid and pressured speech that is difficult to interrupt. Sufferers might not sleep at all, or they may be excessively gregarious and begin to believe that they have superhuman powers. An individual may try to awaken a wilderness group in the middle of the night to hike up a nearby peak. When rebuffed, the manic person might take off alone with no water or protection from the weather because of the belief that he or she is superhuman. A guide described a participant on a wilderness trip who became manic and could not be dissuaded from climbing to the top of a mountain to talk with God. An individual with mania who is in the wilderness should be considered a medical emergency and should be evacuated as rapidly as possible.
Careful questioning may reveal that the manic person is taking psychiatric medications such as mood stabilizers (e.g., lithium, divalproex), antipsychotic medications (e.g., risperidone, olanzapine), or both. People who take lithium must avoid dehydration, which can result in lithium toxicity. Lithium toxicity begins with tremulousness and can proceed to seizures and death. If lithium toxicity is suspected, the lithium should be stopped and the person should be well hydrated. The patient may require dialysis to resolve the toxicity, so evacuation is required. People with bipolar disorder sometimes stop their medications because they enjoy how they feel when they are hypomanic. The use of a benzodiazepine (e.g., lorazepam) or an antipsychotic medication (e.g., risperidone) can control some of the symptoms. Risperidone (2 to 6 mg) and lorazepam (4 to 8 mg) spread over the course of a day may be required to keep a manic individual calm.5 It may be possible to coax a manic person out of the wilderness with the use of encouragement and enticements. Manic individuals can be extremely irritable and sometimes aggressive. Weapons should be confiscated. If a manic individual will not voluntarily leave the wilderness, then assistance—including law enforcement—should be obtained as soon as possible. An evacuation may require the individual to be forcibly restrained and medicated. While waiting for help to arrive, members of the group must constantly contain the manic individual’s excesses to keep both the affected individual and the group safe.
Psychotic Disorders
Individuals with severe mental illnesses (e.g., schizophrenia, schizoaffective disorder) do not typically venture into the wilderness, especially if they are in a deteriorated state. Their overall functioning is too low for them to organize themselves to the point that they could join a wilderness group. Those persons who have been able to benefit from treatment, usually in the form of antipsychotic medications, sometimes venture with groups into the wild. There is an approximate 1% prevalence of schizophrenia worldwide.5 Tragically, the illness often manifests during young adulthood. The hallmark of these disorders is a substantial period, usually of at least 1 month, during which the individual becomes unable to rationally perceive reality. A person who believes that a sinister group worshiping the devil has implanted a transmitter in his mouth (delusion) and who hears mysterious people talking about him and saying that he is pathetic and should kill himself (auditory hallucination) is considered psychotic. People with delusions and hallucinations cannot be talked out of them. People who are successfully treated with medications may still have some unusual or even delusional beliefs, but the psychotic symptoms have receded into the background and are not an active concern for the individual. In addition to psychotic symptoms, people with schizophrenia or a schizoaffective disorder often seem awkward or distant interpersonally. Their thoughts may be jumbled and disorganized. Concrete thinking that is literal or obvious with little ability for abstraction is common. If they are receiving adequate treatment, such individuals might enjoy a wilderness adventure with no difficulty, although their personal contribution to the group may be nominal. Antipsychotic medications—especially older ones such as haloperidol—that are required for the treatment of symptoms cause a wide range of side effects, including extrapyramidal symptoms (e.g., Parkinsonism), acute dystonias, insomnia, sedation, and orthostatic hypotension.11 Side effects alone may preclude a person from participating in a wilderness adventure, but people who have been taking medication for weeks or months may have adapted to the side effects. Newer antipsychotic medications (e.g., aripiprazole [Abilify]) have fewer side effects.
Organic Mental Disorders
There any many medical problems in the wilderness that can cause behavioral symptoms, and these range from mild confusion that is associated with high-altitude hypoxemia to delirium that is associated with high-altitude cerebral edema. A person in the wilderness may have fallen and hit his or her head on a rock, which initially results in a minor scrape and a headache; however, this may progress to a subdural hematoma and delirium that may become life threatening. It is crucial to recognize which signs of delirium in the wilderness are true medical emergencies. A person with delirium has a fluctuating level of consciousness; he or she may be awake and alert for a few minutes and then become inexplicably sleepy. People with delirium are often confused and disoriented with regard to date, time, and place. Concentration, memory, and calculation ability may be impaired, and visual, tactile, or other types of hallucinations may appear. Paranoid delusions might be reported.5 The key sign for differentiating delirium from psychosis is that the psychotic person remains alert with no change in level of consciousness, whereas the delirious person’s level of consciousness fluctuates over minutes or hours.
Personality Disorders
Personality disorders are psychiatric disturbances that can cause considerable difficulty in the wilderness, although they rarely present as emergencies. Personality disorders are common, with an approximate 12% prevalence.5 There are 10 different categories of personality disorders that are described in the DSM-IV-TR. People with personality disorders have enduring maladaptive patterns of behavior that usually date from adolescence. The use of a narrow set of adaptive strategies inflexibly leads these individuals to have chronic problems at school and work and in their interpersonal relationships. Ironically, people with personality disorders do not tend to see themselves as having problems; rather, they blame others for their difficulties. Individuals with personality disorders unwittingly create their own special circle of misery. Depression and substance abuse are common in this population.
Substance abuse Disorders
Some people may be unaware that they have a substance abuse problem when they start a wilderness trip until they start to experience physical or psychological withdrawal. A careful history can establish if someone is experiencing alcohol or drug withdrawal. Alcohol withdrawal is considered a medical emergency because of seizures, psychotic symptoms, and delirium tremens.2 Withdrawal symptoms usually start with shakiness and increased heart rate and blood pressure. Withdrawal from barbiturates or benzodiazepines can manifest similarly to alcohol withdrawal, and can also be life threatening. If withdrawal is suspected, a benzodiazepine (e.g., lorazepam) can be given; several milligrams may be needed before the vital signs stabilize. Alcohol can be used to stop withdrawal symptoms, if necessary and available. People who abuse cocaine, methamphetamines, or narcotics will not experience life-threatening withdrawal, but their symptoms can be extremely uncomfortable and disabling. Withdrawal from substances such as cocaine (i.e., crashing) is associated with extreme irritability and fatigue. Aches and pains that are typical of influenza are seen in association with withdrawal from narcotics. Withdrawal symptoms may last several days. Individuals who are experiencing alcohol or drug withdrawal should be evacuated.
On a wilderness trip, someone may experiment with natural plants in hopes of achieving an induced high. Tea made with jimson weed or certain other plants can induce florid psychosis and delirium. Such individuals may shed clothes, develop severe sunburns, become dehydrated, and expose themselves to all manner of risks. Plants that can cause psychotic symptoms and delirium are common (see Chapter 64) and should be avoided.2 People who are experiencing psychotic symptoms or delirium as a result of the ingestion of toxic plants must be watched constantly until evacuation to a hospital can be arranged.
Suicide, Violence Potential, and Anger Management
Suicide is a major public health problem. The suicide rate in the United States is approximately 11.1 per 100,000, with a recent increase in suicides occurring among young people.5 Depression and alcoholism are frequently associated with suicide. People who are depressed, lonely, or physically ill sometimes commit suicide. Rejection, unemployment, and legal problems are often associated with suicide. In the context of a wilderness trip, factors to consider are depression and recent loss. For example, a wilderness traveler who has been divorced, widowed, or fired from his or her job shortly before the trip may be at higher risk for suicide. A family history of suicide or a history of suicidal behavior increases suicide risk. If there is a concern that someone might be suicidal, then he or she should be asked about suicidal thinking in a straightforward and concerned manner. Asking about suicide does not increase suicide risk. People who kill themselves often think about or become preoccupied with ending their lives. They plan how they will kill themselves, so they should be asked about their plans for suicide. If the suicide potential is judged to be significant, then the person must be watched closely. People who are delirious or psychotic can suddenly become impulsively suicidal in the midst of their confusion and frenzy. Suicidal individuals should be evacuated. More than 40 people have killed themselves below the rims of the Grand Canyon, some in spectacular fashion. Wilderness locations can be inviting places for people to end their lives because of the beauty and the access to effective means (e.g., high cliffs). Many more people think about suicide than those who attempt or complete suicide; however, there is not yet any reliable means for quantitatively assessing the seriousness of someone’s suicide risk. Caution should be the watchword when someone is assessed as being even mildly suicidal in a wilderness setting.
Anger is an adaptive and universal human experience. With modulation, expressions of anger can signal distress, conflict, fatigue, or fear. Allowing people who are not typically angry to have time to cool off and then approaching them in a supportive and concerned manner can lead to rapid resolution of the conflict. Asking an individual who has been angry how he or she is doing can be a good beginning to dealing with someone who is angry. These individuals may report fatigue, fear about some aspect of the journey, or conflict with someone in the group. Active and nonjudgmental listening can often identify the problem and help lead to a resolution. For example, the wilderness trip may need to be slowed down to allow rest for someone who has become exhausted or to provide empathy for a person who is struggling to keep up on the journey. More problematic are people with psychiatric disorders, especially those with borderline or antisocial personality disorders, who have maladaptive ways of expressing anger and hostility. These individuals may be chronically angry, hostile, sarcastic, and even menacing on a wilderness journey. Management of this type of anger should be characterized as attempting damage control. Intensive psychotherapy with the use of cognitive behavioral techniques can be useful, but this is beyond what can be provided in the field.5 People with these more serious forms of anger can have a very negative impact on a group, sometimes splitting the group into factions and causing an absence of camaraderie and an undercurrent of tension. Periodically taking problematic individuals aside in private, providing support, and allowing persons to ventilate while setting firm limits on their more troublesome behaviors can help to diminish the impact that these individuals might have on a group. For extreme behaviors that involve blatant threats or actual violence, more draconian interventions may be needed; these are described later in this chapter.
The culture in the United States is much more violent than those of other industrialized nations. Rape, child abuse, homicide, and other violent crimes are far too common. Men are 10 times more likely than women to be violent, and young men are particularly prone to violence.5 Substance abuse is highly correlated with violence. People who have a history of acting violently in the past are more likely to do so in the future, and people who are going to be violent often signal their intentions. They act aggressively, clench their fists or jaws, and speak loudly or shout. They may have thoughts of acting violently, so they should be asked if they are thinking about hurting anyone. People who have a personality disorder or who are psychotic are at an elevated risk for violence. If a concern exists about someone being violent in the wilderness, weapons should be removed, if possible, and everyone should be vigilant. The potentially violent person should be evacuated or assisted out of the wilderness, with the help of law enforcement personnel if necessary.
Somatic Complaints
Some people are more sensitive to physical irritations and discomfort than are others. For most people, a headache, a scrape, or a sore muscle is not cause for alarm. However, for some individuals, a headache is a sure sign of a brain tumor, the scrape will undoubtedly become gangrenous, and sore muscles are evidence of a smoldering systemic illness. Simple reassurance that there is no major pathologic process present may be enough for many people, but others continue to worry despite solid medical evidence to the contrary; these people suffer from hypochondriasis.1 Insomnia, gastric distress, and fatigue are common complaints that are associated with travel and are usually not cause for concern. However, persons who tend to magnify the significance of common somatic complaints worry excessively and may voice their concerns to the entire group. Occasionally, this can have the effect of creating a kind of “mass hysteria,” where other members of the group begin to experience the same symptoms. For a person who is very worried about his or her health, repeated reassurance might be successful for ameliorating the problem. The difficulty lies in discriminating symptoms of little consequence from genuine and potentially serious organic medical problems. A woman on a wilderness trip in the mountains had a minor fall and became nonresponsive to painful stimuli. She was evacuated to a hospital, where she was released from the emergency department with no ill effects and no cause for her unresponsiveness being found. This woman probably had a conversion disorder, which is rare but can manifest as sudden blindness, paraplegia, or unresponsiveness with no apparent etiology. Taking a good history to exclude an organic explanation for symptoms is important before concluding that the complaints are primarily of psychological origin. The Grand Canyon Park Service Rangers at Phantom Ranch and Indian Gardens regularly respond to individuals who report that they cannot physically hike out of the canyon. After taking a history to exclude organic illness, the rangers use a firm approach and tell these individuals that they can and will hike themselves out of the canyon. These individuals are encouraged to hike slowly, to avoid hiking during the hottest part of the day, and to remain hydrated, but they are not given a helicopter or mule ride to the rim.
Insomnia
Complaints of insomnia are exceedingly common, with a 1-year prevalence rate of 30% to 45%.1 Although individuals may complain about poor sleep and daytime sleepiness, sleep laboratory assessments frequently demonstrate that these individuals sleep better than they subjectively report. Common insomnia-related complaints include difficulty falling asleep, frequent awakenings, and early awakenings. As people age, they normally sleep less and more lightly, and they have more frequent awakenings; this leads to frequent sleep complaints in the elderly. Even for persons without baseline sleep problems, traveling long distances across several time zones to wilderness locations might lead to insomnia problems as a result of the disruption of their circadian rhythms. Individuals with insomnia often have poor sleep hygiene. They nap during the day, drink caffeine and alcohol, do not exercise, undertake stimulating activities like watching television while falling asleep, have irregular sleep schedules, and sleep in noisy and uncomfortable settings. In wilderness settings, sleep problems can be accentuated as a result of heat, cold, humidity, altitude, uncomfortable sleeping arrangements, and fears of bugs, snakes, and wild animals. However, wilderness settings can also have a salutary effect on sleep as a result of the associated quiet, darkness, exercise, and freedom from the stresses of work and other responsibilities.
Response to Crisis
Disasters
Avalanches, storms, rockfalls, climbing, whitewater accidents, and many other untoward events can lead to the death or serious injury of one or more group members. People who venture into the wilderness usually do not anticipate someone being seriously injured or killed (Figure 35-2). Even persons who have taken wilderness first-aid courses do not enter the wilderness expecting the worst, or else no one would participate in these types of activities. There are many descriptions of outdoor trips that have involved crises.10
Humans wrap a cloak of denial around themselves. Thus, when a crisis or tragedy occurs, it is almost always an emotional shock. When you watch your climbing partner fall and die or when your friend drowns when his kayak flips in whitewater, there is a reaction of horror, dread, and disbelief. The situation is overwhelming, and survivors or witnesses of these types of tragedies often describe a sense of unreality that is associated with the horrible event. People who are involved in tragedies often need to replay the event to put it into some type of meaningful personal context. People who are relatively intact psychologically and who have good social support can usually mentally process a trauma successfully without long-term mental health problems. As the size of a disaster grows and its impact on a person or a community’s support networks increases, the likelihood of long-term mental health problems grows. People who handle trauma by psychological avoidance and casting blame may have poorer outcomes.13
In response to natural disasters, some individuals develop acute stress disorder or post-traumatic stress disorder (PTSD). Estimates of the frequency of these disorders after disasters—either manmade or natural—vary from 2% to more than 50%.13 The symptoms that are typical of these disorders include efforts to avoid reminders of the traumatic event and markedly increased anxiety during exposure to such reminders. The affected person may be flooded with uncontrollable memories, including bad dreams and flashbacks (i.e., feeling and behaving as if the trauma was happening again). The person may feel a sense of emotional detachment from others. He or she may have difficulty concentrating and sleeping, feel restless, and be easily startled. Symptoms can begin immediately after a disaster. If they persist for more than 2 days but for less than 1 month, the disorder is called acute stress disorder; if the symptoms are present for more than 1 month, the disorder is called PTSD.1 For most people, symptoms diminish as time passes, although there is commonly intensification of symptoms around the time of the 1-year anniversary of the tragedy. Symptoms may become chronic and require ongoing psychiatric care. I have personally evaluated men who were held as prisoners of war during World Wars I and II and who were subjected to cruel deprivation or torture. Some did not experience symptoms of PTSD until they retired, which was many years after they were traumatized (i.e., delayed PTSD).1
There is no evidence-based consensus for mental health interventions during the immediate aftermath of a disaster. Available evidence indicates that psychological debriefing is not associated with benefits and may in fact complicate recovery after a disaster. Debriefing, which usually involves some review of the disaster, may increase physiologic hyperreactivity, increase the coding of traumatic memories, and promote rumination about the tragedy; debriefing can thus interfere with more adaptive and natural healing mechanisms (e.g., avoiding thinking about the trauma). If debriefing is used, it should be voluntary, involve clinical assessment, and only be performed by experienced and well-trained individuals. Clearly, more systematic research is needed in this area.13 However, despite a lack of systematic research, there have been attempts to promulgate a clinical consensus regarding desirable mental health interventions in the wake of disasters on the basis of current empiric evidence.8 The immediate and first response to a wilderness disaster should emphasize ensuring the safety and security of the survivors; this includes provision of food, water, warmth, and shelter. Second, efforts should be made to calm everyone who was involved in the disaster. Survivors should be accurately informed about what has happened and about what rescue efforts are underway. It is important to advise survivors about the status of others who were involved in the disaster and about the safety of family and loved ones. Communication with loved ones should be facilitated as soon as possible. Victims should be provided with a calm setting to decrease arousal as much as possible. Encouraging deep breathing and muscle relaxation may be helpful. Reassurance should be provided regarding any distortions that a survivor may experience, such as feelings of weakness or guilt or catastrophic perceptions that the world is a malevolent and dangerous place. Medication use is controversial, with selective serotonin reuptake inhibitors demonstrating some benefit during the weeks and months after the disaster. However, using psychotropic medications during the immediate aftermath may not be necessary and may even be harmful, particularly if the sedative properties interfere with survival behavior or motivation. It is expected that survivors will be very emotional after a disaster, but the experience of those emotions may be naturally adaptive, so artificially dampening them with medications can be counterproductive. Survivors should be approached with the expectation that they will recover psychologically, and they should be reassured about their future mental health. Further interventions are required in the initial aftermath of a disaster. Promoting a sense of self-efficacy is recognized as an important component of recovery efforts, and this includes providing survivors with continuing information about the effects of the disaster and the means to contact other survivors. Making psychological intervention accessible can be very useful during the weeks and months after a disaster. Specialized crisis counseling services were developed after Hurricane Katrina that proved very useful.7 Cognitive behavioral treatments have also demonstrated considerable value for survivors of disasters. Finally, promoting a sense of connectedness with the broader community and instilling a sense of hope (i.e., avoiding social withdrawal and hopelessness) can be crucial for people who are recovering from a disaster. Pragmatically, a feeling of hope can come from prompt reparation payments, which may allow someone to rebuild a home that was destroyed in a disaster.
Survival Psychology
It is not uncommon for people to become lost in the wilderness. Human spatial orientation abilities are limited; we often function under the illusion that we know exactly where we are when that is absolutely not the case.3 People rationalize disorientation in the wilderness by explaining away inconsistencies between their topographic map and the actual landmarks before them. As a person becomes convinced that he or she is completely lost, he or she may experience intense fear, panic, and disorientation that are unique to this type of dilemma. Lost people have been shown to tend to walk in circles.12 Even people with considerable experience in the wilderness may demonstrate inexplicable behaviors, such as abandoning provisioned backpacks or other potentially valuable items. Some have even removed clothing, which increased their exposure to the elements.3
After becoming lost, some persons develop a strategy and carry it through; however, when this plan fails, these individuals may abandon hope and resign themselves to fate. Ironically, children who are less than 6 years old fare better when they are lost as compared with older children and adults. The explanation for this paradox might be that younger children act on instinct and seek shelter when cold and water when thirsty, whereas older children and adults panic and sometimes overlook obvious and simple means to help them to survive.3 In groups that become lost, good leadership is often a key component of the survival of the group. Perhaps the most famous survival story is that of Ernest Shackleton’s ill-fated voyage to reach the South Pole in 1914. His ship, the Endurance, broke up in the ice. Under his leadership, the group survived months of incredible hardship. Against all odds, all 27 men survived.9
Leadership and Teamwork
Wilderness activities are usually not solo affairs. Outdoor adventures can range from a 5-mile day hike with a social group to an expedition that involves dozens of people who climb to the summit of Mt Everest. For adventures to be successful and safe, planning, preparation, leadership, and guidance are required. People who share wilderness activities together experience the same types of group interactions that occur among co-workers, families, and many other groups. A safe and rewarding wilderness adventure begins before the actual trip. Careful planning includes attention being given to numerous issues, including food, equipment, maps, screening of participants, impact on the environment, and necessary permits.4 The planning process itself may involve a group working together. Subsequent to the adventure, some type of communication may be essential to bring spiritual, emotional, or logistical closure to the experience.
Leadership skills should be taught and developed; otherwise, the leader will make the same mistakes repeatedly.4 Good leaders have a vision for the outings, but they are flexible enough to adapt according to the exigencies of evolving circumstances. Successful leaders care about their people and build teams that make use of the strengths of each member of the group. Caring, sensitivity, and empathic listening are crucial components of a successful and effective leader. When effective leaders convey caring and empathy to an entire group, the results are increased cohesiveness and solidarity. Sometimes leaders emerge during a crisis or disaster and are critical to the survival of a group.9 Leadership and interactions among group members evolve during the course of a trip. Leadership is often fluid, because people with different skills take leadership roles in different functional areas, such as building fires, reading maps, and maintaining good humor and morale. People can be remarkably courageous, kind, and ingenious, but they can also be petty, mean, and destructive. A group on a wilderness journey is a microcosm of society; in other words, the group is complex and multifaceted. This type of situation reflects the full range of strengths and weaknesses of both men and women.
Triage
Although mental illness is common, most emotional problems in the wilderness are mild and do not require evacuation or restraint. One of the most serious errors that can be made when assessing an individual with apparent mental problems is to fail to exclude an organic cause of his or her change in mental status. People can become agitated and irritable in response to encephalitis or dehydration. It is important to not forego the fundamentals of assessment, such as taking the vital signs and obtaining a thorough history. As with the assessment and treatment of any medical problem in the wilderness, a careful systematic approach will yield the best triage decisions. To help with this assessment, Table 35-1 provides a summary of the recommendations made in this chapter regarding simple triage and treatment decisions for a variety of mental health problems in the wilderness. In addition, the General Health Questionnaire—especially the 28-item version—is a widely used and studied mental health screening tool that is adaptable for use in wilderness settings.6
1 American Psychiatric Association. Diagnostic and statistical manual of mental disorders, ed 4, text revision. Washington, DC: American Psychiatric Association; 2000.
2 Galanter M, Kleber H, editors. The American Psychiatric Publishing textbook of substance abuse treatment, ed 4, Arlington, Va: American Psychiatric Publishing, 2008.
3 Gonzales L. Land of the lost. Adventure. Nov/Dec 2001:84.
4 Graham J. Outdoor leadership: Technique, common sense & self-confidence. Seattle: The Mountaineers; 1997.
5 Hales RE, Yudofsky SC, Gabbard GO, editors. The American Psychiatric Publishing textbook of psychiatry, ed 5, Arlington, Va: American Psychiatric Publishing, 2008.
6 Jackson C. The General Health Questionnaire. Occupational Med. 2007;57:79. doi:10.1093/occmed/kql169
7 Jones K, Allen M, Norris FH, et al. Piloting a new model of crisis counseling: Specialized crisis counseling services in Mississippi after Hurricane Katrina. Adm Policy Ment Health. 2009;36:195.
8 Hobfoll SE, Watson P, Bell CC, et al. Five essential elements of immediate and mid-term mass trauma intervention: Empirical evidence. Psychiatry. 2007;70:283.
9 Lansing A. Shackleton’s valiant voyage. New York: McGraw-Hill; 1960.
10 Nunn B. Panic rising: True-life survivor tales from the great outdoors. Seattle, Wash: Sasquatch Books; 2003.
11 Schatzberg AF, Cole JO, DeBattista C. Manual of clinical psychopharmacology, ed 6. Arlington, Va: American Psychiatric Publishing; 2007.
12 Souman JL, Frissen I, Sreenivasa MN, et al. Walking straight into circles. Curr Biol. 2009;19:1538.
13 Ursano RJ, Norwood AE, editors. Trauma & disaster: Responses & management. Washington, DC: American Psychiatric Publishing, 2003.