Liver disease
Investigation
Outcome
Acute liver damage can progress in three ways:
 It may resolve, as indeed it does in the majority of cases.
It may resolve, as indeed it does in the majority of cases.
Hepatic failure
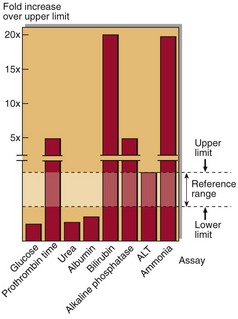
Hepatic failure may give rise to renal failure due to exposure of the glomeruli to toxins usually metabolized by the liver. There may be an increase in blood ammonia as a result of the failure to detoxify this to urea. The pattern of abnormalities found in hepatic failure is shown in Figure 30.2.
Chronic liver disease
Three forms of chronic liver damage are:
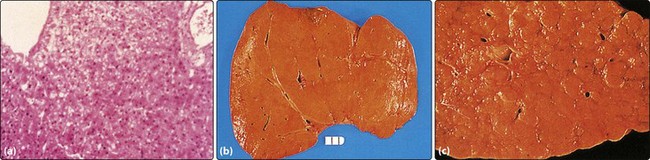
All of these conditions may progress to cirrhosis, a disease characterized by extensive liver fibrosis. Fibrosis is the formation of scar tissue, resulting in the disorganization of liver architecture and its shrinkage. (Fig 30.3).
Clinical features
Unusual causes of cirrhosis
Cirrhosis can develop in children as a result of α1-antitrypsin deficiency or Wilson’s disease, and in adults due to haemochromatosis. α1-antitrypsin deficiency can be detected in newborn infants in whom there may be a prolonged period of jaundice for several weeks. In some cases this progresses to juvenile cirrhosis. Haemochromatosis is a disorder of iron absorption, associated with deposition of iron in the hepatocytes and other tissues, which can lead to liver failure. The diagnosis is by measurement of serum iron, transferrin and ferritin (p. 115). Wilson’s disease is an inherited disorder of copper metabolism that leads to failure in copper excretion, low concentrations of caeruloplasmin, and deposition of copper in the liver and other tissues (p. 117). Cirrhosis may also occur following chronic ingestion of pyrrolizidine alkaloids, such as are found in some herbal teas.
Other liver problems
Primary hepatoma is associated with a number of conditions such as cirrhosis or hepatitis, although a number of causative carcinogens, such as aflatoxins generated by specific fungi infecting foodstuffs, have been identified. Alpha-fetoprotein is a useful marker of primary hepatic tumours (pp. 140–141).