Chapter 5 Laser Facial Resurfacing and Dermabrasion
Summary
Introduction
While skin rejuvenation dates back to the Egyptian era, laser facial rejuvenation is a recent innovation. It is said that Cleopatra used soured milk (lactic acid) to rejuvenate her skin. Thus chemical peels as well as a variety of mechanical exfoliations have been practiced for thousands of years. The laser, however, is a recent addition to the skin rejuvenation armamentarium. In 1960, Theodore Maiman produced the first laser energy, utilizing a Ruby crystal.1 New laser development was primarily a product of the communications industry, and in fact much of the early work was done in Bell Laboratories. Many of the lasers used in medicine today were developed for industrial use and later adapted to medical applications. Patel published his discovery of the carbon dioxide laser in 1964.2
Laser application in medicine gained momentum in the late 1960s and early 1970s. Dr Leon Goldman commonly considered ‘the father of laser medicine’ and many other pioneers recognized the value of the laser in treating a variety of medical conditions.3 Ophthalmology was one of the early adopters of laser energy for treating intraocular neovascularization. The technology was soon applied to vascular birthmarks, such as port-wine stains. These early lasers, however, were very crude devices with poor control of the laser parameters, thus leading to mixed results. Commonly a port-wine stain was exchanged for a scarred, hypopigmented area of skin. The satisfactory treatment of many skin conditions awaited the development of new technology and understanding.
The concept of selective photothermolysis (SPTL) was introduced by Anderson and Parrish in 1983 and proved to be a turning point in the laser treatment of skin conditions.4 This theory recognized that the optimal treatment of a variety of skin disorders was dependent on optimization of several factors related to the target tissue and the laser parameters. The target of vascular disorders for instance, was the hemoglobin inside the vessels. The laser wavelength that was preferentially absorbed in hemoglobin was that wavelength which was heavily absorbed by hemoglobin and minimally absorbed by other competing pigments in the tissue. Absorption curves which plot percent absorption versus wavelength for a single tissue are not linear but have many peaks and troughs. When the absorption curves for the various absorbers, termed chromophores, in the target area are overlaid it is possible to choose optimal wavelengths that are heavily absorbed by the target (e.g. hemoglobin) and minimally absorbed by other chromophores such as water, xanthophyll, and melanin that would compete with the hemoglobin to absorb the laser energy. Since nearly all lasertissue interaction is thermally induced, the controlled heating of the target tissue is created by the absorption of the laser energy which is induced by photons impacting the molecules of the tissue. Vibrational energies disrupt the molecules and the cells of the tissue target.
As part of the SPTL theory, the concept of thermal relaxation time was introduced to explain the selective heating of the various tissue components. In essence, this concept states that the confinement of energy (heat) within a structure can be controlled by limiting the exposure time. This thermal relaxation time is proportional to the size of the structure, meaning that extremely small tissue components such as melanosomes have an extremely short thermal relaxation time, and thus should be treated with extremely short pulse duration. Typically these nanometer structures would be treated with a nanosecond pulse duration. By limiting the pulse duration the energy is thus inhibited from spreading to surrounding structures causing unwanted damage.
The result of the SPTL theory led to the development of the first laser which was specifically designed and produced to treat a medical condition. This was the pulsed dye laser used for treating port-wine stains. The pulsed dye laser was almost instantly accepted in treating port-wine stains in very young patients which had hitherto been very problematic.5 It was not long before new lasers were introduced, having been designed according to the theory of SPTL for treating a variety of ailments such as lentigines, tattoos, and skin aging.5,6
The carbon dioxide (CO2) laser with a wave length of 10,600 nm in the far infrared portion of the spectrum is capable of coagulation and ablation of tissue. Thus it is used to remove lesions by evaporation as well as to thermally stimulate the tissue. The normal response can therefore be quite varied, depending on a large number of factors such as tissue hydration as well as the laser parameters such as pulse duration and energy density. Although the traditional carbon dioxide laser does not meet any of the parameters of the theory of selective photothermolysis, nevertheless this laser can be designed to achieve satisfactory ablation or cutting while minimizing thermal damage.8
As an ablative instrument the carbon dioxide laser has been used to remove a variety of benign and malignant lesions.9 These include verrucae, syringomas, seborrheic keratoses, and other benign lesions. Actinic keratoses as well as superficial basal cell carcinoma can be removed with these lasers, however, due to a lack of histologic confirmation one can never be certain that the lesion is totally removed by the laser.10
Two conditions which respond extremely well to the carbon dioxide laser treatment are rhinophyma and actinic cheilitis.11,12 A generic treatment regimen for these types of lesion would include the use of a 1 mm handpiece with a focused and defocused beam, usually pulsed mode with sufficient energy to evaporate the tissue. Coagulated tissue may require removal by wiping between passes. Commonly some minor scarring and hypopigmentation can be seen at the site of treatment.
Laser Skin Resurfacing
Methods
As mentioned above, a variety of chemical and mechanical processes have been used in the past to rejuvenate the skin. Most of these required removal of a large portion of the epidermis as well as portions of the dermis, anticipating that the healing process would rejuvenate the epidermal elements including pigment, and contraction of the dermal collagen elements with additional collagen being deposited during the healing process. It was quickly recognized that the laser could produce a similar effect. In particular the carbon dioxide laser was used for treating photoaged skin in the 1980s. Early attempts with conventional carbon dioxide lasers however led to many unsatisfactory results, including scarring.13 With the advent of high peak power, rapidly pulsed or scanned carbon dioxide lasers, this difficulty was overcome in accordance with the theory of SPTL, mentioned above.
There are generally two methods of achieving the necessary energy in a sufficiently short time frame in order to achieve evaporation/ coagulation with minimal thermal damage. These would be the extremely short pulsed, high energy lasers as well as the rapidly scanned continuous-wave laser. The super pulsed carbon dioxide laser was a step in the direction of satisfactory laser rejuvenation. The UltraPulse laser by Coherent Inc. was capable of delivering 5 j/cm2 in a sufficiently short period of time in order to allow vaporization of 20 to 30 μ of tissue and residual thermal damage of 40 to 120 μ depth after two or three passes.14 Most of the laser resurfacing is accomplished with a robotic scanner which Coherent termed the computerized pattern generator (CPG). Histologically much of the epithelium is removed. Although elastin may persist, type I collagen is denatured between 60 ° and 70 °C, causing it to shorten.15 Epithelialization was complete in seven days, but total healing as indicated by an abating of the erythema required several weeks. In fact, collagen deposition may be seen for many months following the laser resurfacing. Comparison of laser resurfacing with chemical peel and dermabrasion showed similar healing and results, with the exception of the phenol peel which required considerably longer to heal. No scarring was observed in this treatment study.16
Indications and Contraindications
Although virtually every patient would receive some benefit from laser resurfacing, choosing the appropriate patient and preparation for treatment will achieve the optimal results. Most forms of photoaging including pigmentation disorders, as well as elastosis and laxity of the skin, will improve with laser resurfacing, although some lesions will not totally disappear. A sufficiently educated patient who has been informed of the procedure, alternatives and risks, and has a realistic expectation, is undoubtedly the best candidate. Patients who are prone to form keloids or aggressive scars are probably not good candidates. Other skin conditions such as scleroderma, and patients who have been treated within the past year with isotretinoin, are also probably not good candidates for laser resurfacing. In addition, patients who are receiving simultaneous cosmetic surgery such as facelifts are at risk of developing scars in the portion of skin that is undermined. Although there are reports describing treatment of the neck and other areas of the skin with the carbon dioxide laser, these generally require extreme care, because they are very susceptible to scarring and significant pigmentation changes. There are better modalities for treating these areas including the erbium laser, fractional laser or others.
Preoperative Considerations
Prophylactic treatment with antibiotics and antiviral medications preoperatively are advised.
Postoperative Care
A recent innovation is a silicone sealant which is applied immediately after the procedure. This is a two-part, epoxy-like, clear, flexible silicone material (Innovation Alley, Lyndhurst, OH). It is difficult to get this material to adhere to the skin, and the patient is advised to minimize movement such as talking and chewing. Frequently it will separate in the immediate postop period. Nevertheless, it is left in place for approximately 5 days unless it develops a green drainage underneath, possibly indicating infection, in which case it is removed and soaks are started with appropriate therapy. It is also sometimes removed around the mouth if food collects under the mask. The fifth day the patient is advised to sit in the shower soaking the face. The mask can be elevated from the skin with a cotton tip applicator lubricated with antibiotic ointment. Portions of the mask which are strongly adherent are left in place until they spontaneously loosen and fall off.
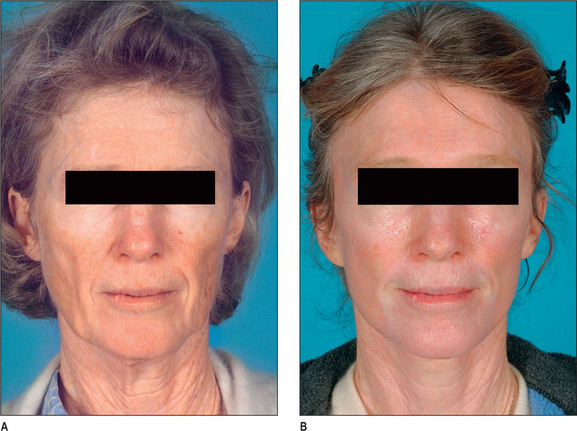
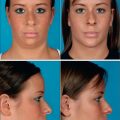
The results are often gratifying, especially when the laser resurfacing is combined with facial rejuvenation (Fig. 5.1A&B). In patients who undergo facial rhytidectomy at the time of facial laser resurfacing, the laser energy level should be reduced in the undermined area to minimize the potential for deeper thermal damage.22,23 The fluence will be set at a lower level on the lateral portion of the face (settings such as a density of 3, 60 watts, and 100 mJ). The density will be increased as the laser is advanced medially. It is also be safer to minimize the undermining of the skin during the rhytidectomy.
Complications and Sequelae
As previously mentioned, pigmentation changes are the most common sequelae following a laser resurfacing. Hyperpigmentation is frequently seen in Fitzpatrick skin types III and greater, especially during the summer in the southern latitudes. This is frequently self-limiting, but should be treated with tretinoin and bleaching agents. In a few patients, typically Fitzpatrick skin types I and II, a delayed hypopigmentation is sometimes seen.13–17 This may not appear until a year or more following the laser resurfacing procedure and generally is resistant to treatment. Inclusion cysts or milia are frequently seen, particularly in the periorbital area. These will usually spontaneously open, but sometimes have to be pricked. Infection, as indicated by ulcers or a worsening of the inflammation, may appear up to a week or more following the resurfacing procedure, and should be aggressively treated with cleansing, soaks and antibiotics in order to avoid scarring. Staphylococcus, Pseudomonas, Candida, and herpes simplex are among the more common pathogens. Conjunctivitis may result from the intraocular eye shields or topical ointments applied around the eye. In rare instances, these may require treatment with ophthalmic antiinflammatory drugs. Ectropion can result from aggressive resurfacing of the lower eyelid in susceptible individuals. Rarely, scarring results from overly aggressive laser treatment, secondary infections, or the patient traumatizing the skin. Pruritus is common in the postop period and should be treated with topical creams or antihistamines.
Alternative Applications/Technologies
Laser Blepharoplasty
I have been using the laser in blepharoplasty for over 12 years and have done approximately 1000 cases with it.17 Almost all of my blepharoplasties involve carbon dioxide laser for excision, transconjunctival fat removal, and laser resurfacing of the upper and lower eyelids. Although this lengthens the healing time, there are many advantages to it. It is simpler, safer, and faster. The technique will be described below.
Operative Approach
The concept of laser blepharoplasty was introduced by Baker in 1992.18 Roberts collected a series of 907 laser blepharoplasties with a 95% satisfaction rate in wrinkle reduction and a 0.3% ectropion incidence.19 The advantages were pointed out that this procedure was faster, safer, with less bruising than conventional blepharoplasty. The disadvantages include the cost of the equipment, a learning curve and a longer healing time. The exceptional patient with considerable festooning or marked laxity of the lower lid may not be a candidate for transconjunctival blepharoplasty, but these patients may still be candidates for the standard transcutaneous lower lid blepharoplasty with a subciliary incision made by the laser. Seckel, using the CO2 laser, was able to tighten the orbicularis oculi muscle through the transconjunctival approach.20
Methods Other Than Co2 Laser Technique
Fractionated laser
A very recent development in laser skin rejuvenation is the fractionated laser. This is an entirely new concept and laser treatment. Lasers in the past have been generally a surface phenomenon in which the entire surface of an area is treated. This means that frequently there is choroids elation or even ablation of the epidermal layer as well as deeper fracture on the dermal layer secondary to heat transfer. The fractionated laser however honeycombs the skin with individual pulses of energy, penetrating much more deeply. Pulse effects as deep as 1.5 mm can be achieved with this fractionated laser, depending on the wavelength and other factors. Only a small percentage, perhaps 1525% of the surface area, is treated at any one treatment because of the effect. These treatments then are administered every few weeks, perhaps monthly. The repetitive nature, however, generates new collagen as well as removing hyperpigmentation and other surface phenomena. Because a large percentage of the surface goes untreated with each treatment, there is essentially no crusting or weeping as with the other resurfacing lasers. There usually is some mild pigmentation change as well as inflammation which will disappear within a few days and generally is not incapacitating. As with these other lesser skin rejuvenation lasers anesthesia requirements are usually less than with the carbon dioxide laser. The technology of fractionated laser resurfacing is very much in its infancy, and has created somewhat of a paradigm shift in the science of laser skin rejuvenation. New protocols are currently under development, as well as refinements in technology which will extend the scope of this laser energy.
The Future
Many excellent articles and textbooks have been published, exhaustively discussing the concepts which have been superficially treated here. An example of these would be Lasers in Cutaneous and Aesthetic Surgery edited by Arndt, Dover and Olbricht.21 Clinicians wanting to become involved in laser medicine and keep abreast of the latest developments in this growing field would be well advised to attend the annual meeting of the American Society for Laser Medicine and Surgery (www.aslms.org).
1. Maiman T.H. Stimulated optical radiation in ruby. Nature. 1960;187:493.
2. Patel K.N.C. Continuous-wave laser action on vibrational-rotational transitions of CO2. Phys Rev. 1964;136A:1187.
3. Goldman L., Rockwell J.R.Jr. Laser reaction in living tissue. In: Lasers in medicine. New York: Gordon and Breach; 1971:163-185.
4. Anderson R.R., Parrish J.A. Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science. 1983;220:524-527.
5. Tan O.T., Sherwood K., Gilcrest B.A. Treatment of children with portwine stains using the flashlamp-pulsed tunable dye laser. N Engl J Med. 1989;320:416-420.
6. Goldberg D.J. Treatment of pigmented and vascular lesions of the skin with the Q-switched Nd:YAG laser. Laser Surg Med. 1993;13(suppl 5):55.
7. Taylor C.R., Gange R.W., Dover J.S., et al. Treatment of tattoos by Ruby laser: a dose-response study. Arch Dermatol. 1990;126:893-899.
8. Walsh J.T., Flotte T.G., Anderson R.R., Deutsch T.F. Pulsed CO2 laser tissue ablation: effect of tissue type and pulse duration on thermal damage. Lasers Surg Med. 1988;8:108-118.
9. Ohbricht S.O. Use of the carbon dioxide laser in dermatologic surgery: a clinically relevant update for 1993. J Dermatol Surg Oncol. 1993;19:367.
10. Lanzafame R.J., Rogers D.W., Naim J.O., et al. Reduction of local tumor recurrence by excision with the CO2 laser. Lasers Surg Med. 1986;6:439-441.
11. Greenbaum S.S., Krull E.A., Watnick K. Comparison of CO2 laser and electrosurgery in the treatment of rhinophyma. J Am Acad Dermatol. 1988;18:363-368.
12. Whitaker D.C. Microscopically proven cure of actinic cheilitis by CO2 laser. Lasers Surg Med. 1987;7:520-523.
13. David L.M., Lask G.P., Glassberg E., et al. Laser abrasion for cosmetic and medical treatment of facial actinic damage. Cutis. 1980;43:583-587.
14. Fitzpatrick R.E., Goldman M.P., Satur N.M., Tope W.D. Pulsed carbon dioxide laser resurfacing of photoaged facial skin. Arch Dermatol. 1996;132:469-471.
15. Brugmans M.J.P., Kemper J., Gijsbers G.H.M., et al. Temperature response of biological materials to pulsed non-ablative CO2 laser irradiation. Lasers Surg Med. 1991;11:587-594.
16. Fitzpatrick R.E., Tope W.D., Goldman M.E., Satur N.M. Pulsed carbon dioxide laser, trichloroacetic acid, Baker-Gordon phenol, and dermabrasion: a comparative clinical and histologic study of cutaneous resurfacing in a porcine model. Arch Dermatol. 1996;132:469-471.
17. Gregory R.O. Laser skin rejuvenation. Presented at the annual meeting of the American Society of Plastic Surgeons. 1997.
18. Baker S.S. Carbon dioxide laser upper lid blepharoplasty. Am J Cosmet Surg. 1992;9:141.
19. Roberts T.L. Laser blepharoplasty and laser resurfacing of the periorbital area. Clin Plast Surg. 1998;25:95-108.
20. Seckel B.R. Management of orbicularis hypertrophy with the CO2 laser. Presented at the annual meeting of the American Society for Aesthetic Plastic Surgery, New York, May. 1997:3-7.
21. Arndt K.A., Dover J.S., Olbricht S.M., editors. Lasers in cutaneous and aesthetic surgery. Philadelphia: Lippincott-Raven, 1997.
22. Wald D., Michelow B.J., Guyuron B., Gibb A. Fire hazards and CO2 laser resurfacing. Plast Reconstr Surg. 1998;101(1):185-188.
23. Guyuron B., Michelow B., Schmelzer R., Thomas T., Ellison M. Delayed healing of rhytidectomy flap resurfaced with CO2 laser. Plast Reconstr Surg. 1998;101(3):816-819.