[level-membership-for-dermatology-category]
Hyperhidrosis
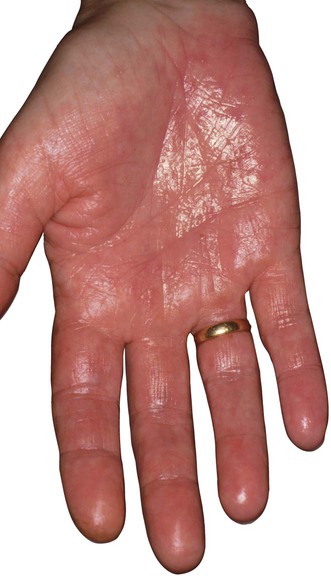
Hyperhidrosis can be classified as idiopathic or pathologic.
Management strategy
 Cryotherapy (very painful and poorly tolerated)
Cryotherapy (very painful and poorly tolerated)
 Thermal injury of localized sweat glands using a microwave based device or Nd: YAG laser
Thermal injury of localized sweat glands using a microwave based device or Nd: YAG laser
 Methods that remove subcutaneous tissue alone. A number of skin flaps/incisions are described to gain access to the subcutaneous axillary tissues, and the deep dermis and adjacent subcutis are trimmed away. Subcutaneous curettage and axillary liposuction are other methods described for achieving this objective
Methods that remove subcutaneous tissue alone. A number of skin flaps/incisions are described to gain access to the subcutaneous axillary tissues, and the deep dermis and adjacent subcutis are trimmed away. Subcutaneous curettage and axillary liposuction are other methods described for achieving this objective
 Methods that excise skin and subcutaneous tissue
Methods that excise skin and subcutaneous tissue
 Methods that combine cutaneous excision and resection of subcutaneous tissue.
Methods that combine cutaneous excision and resection of subcutaneous tissue.
First-line therapies
Second-line therapies
Third-line therapies
[/level-membership-for-dermatology-category][not-level-membership-for-dermatology-category]
Hyperhidrosis

Hyperhidrosis can be classified as idiopathic or pathologic.
Management strategy
 Cryotherapy (very painful and poorly tolerated)
Cryotherapy (very painful and poorly tolerated)
 Thermal injury of localized sweat glands using a microwave based device or Nd: YAG laser
Thermal injury of localized sweat glands using a microwave based device or Nd: YAG laser
 Methods that remove subcutaneous tissue alone. A number of skin flaps/incisions are described to gain access to the subcutaneous axillary tissues, and the deep dermis and adjacent subcutis are trimmed away. Subcutaneous curettage and axillary liposuction are other methods described for achieving this objective
Methods that remove subcutaneous tissue alone. A number of skin flaps/incisions are described to gain access to the subcutaneous axillary tissues, and the deep dermis and adjacent subcutis are trimmed away. Subcutaneous curettage and axillary liposuction are other methods described for achieving this objective
 Methods that excise skin and subcutaneous tissue
Methods that excise skin and subcutaneous tissue
 Methods that combine cutaneous excision and resection of subcutaneous tissue.
Methods that combine cutaneous excision and resection of subcutaneous tissue.
Selective ablation of the sympathetic innervation
[/not-level-membership-for-dermatology-category]



 Topical ACH solution in ethanol
Topical ACH solution in ethanol Topical anticholinergics
Topical anticholinergics Oral anticholinergics
Oral anticholinergics Iontophoresis
Iontophoresis Botulinum A neurotoxin
Botulinum A neurotoxin Botulinum A neurotoxin delivered by Dermojet
Botulinum A neurotoxin delivered by Dermojet Botulinum A neurotoxin delivered by iontophoresis
Botulinum A neurotoxin delivered by iontophoresis Botulinum B neurotoxin
Botulinum B neurotoxin Liposuction and surgical excision (axillae only)
Liposuction and surgical excision (axillae only) Sympathectomy
Sympathectomy Microwave based devices
Microwave based devices Biofeedback and behavioral modification
Biofeedback and behavioral modification Diltiazem
Diltiazem Clonazepam
Clonazepam Clonidine
Clonidine