Chapter 24 HIRSUTISM
General Discussion
The following discussion of hirsutism focuses on adolescent girls. For a discussion of hirsutism in infants or children, please see Chapter 35, Precocious Puberty.
Key Physical Findings
 Blood pressure, height, weight
Blood pressure, height, weight
 Evaluation of hair distribution and characteristics
Evaluation of hair distribution and characteristics
 Consider quantifying degree of hirsutism using the Ferriman and Gallwey scoring system
Consider quantifying degree of hirsutism using the Ferriman and Gallwey scoring system
 Skin evaluation (for acanthosis nigricans, acne, striae, hyperpigmentation)
Skin evaluation (for acanthosis nigricans, acne, striae, hyperpigmentation)
 Breast examination for nipple discharge or galactorrhea
Breast examination for nipple discharge or galactorrhea
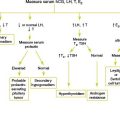
Suggested Work-up
| Serum testosterone and DHEA sulfate (DHEA-S) | To evaluate for ovarian and adrenal tumors. Total testosterone levels >1.5 ng/mL or DHEA-S levels >700 μg/dL are suggestive of androgen-producing neoplasms. |
| Serum 17α-hydroxyprogesterone (17-OHP) | To evaluate for late-onset adrenalhyperplasia |
| <200 ng/dL is unlikely to be 21-hydroxylase deficiency | |
| 200-400 ng/dL indicates low likelihood 21- hydroxylase deficiency, but ACTH stimulation test recommended | |
| 400-1000 ng/dL is suggestive of 21- hydroxylase deficiency and ACTH stimulation test is recommended | |
| >1000 ng/dL is diagnostic of 21- hydroxylase deficiency | |
| Serum prolactin | To evaluate for pituitary tumors |
| Thyroid-stimulating hormone (TSH) | To evaluate for thyroid dysfunction |
| Fasting serum glucose | To evaluate for insulin resistance in patients suspected of having PCOS |
Additional Work-up
| ACTH stimulation test with measurement of 17-OHP at baseline and 60 minutes after administration of 0.25 mg cosyntropin | When CAH is suspected. In 21-hydroxylase deficiency, an increase of 17-OHP to more than 1500 ng/dL at 60 minutes is usually seen. |
| LH and FSH | May be useful in confirming the diagnosis of PCOS. Elevated LH level is suggestive of PCOS, particularly when the LH-FSH ratio exceeds 2.5. |
| 24-hour urinary collection for free cortisol and creatinine levels | If Cushing syndrome is suspected |
| Dexamethasone suppression test (1 mg dexamethasone at 11 PM with 8 AM serum cortisol levels measured the next day) | If urinary free cortisol level is elevated. The morning cortisol level should be less than 5.0 μg/dL after the dexamethasone dosing. |
| Glucose tolerance test | In patients with suspected PCOS with elevated fasting serum glucose |
| Computed tomography (CT) of the abdomen and pelvis | To assess the adrenal glands and ovaries in patients whose history, physical examination, or laboratory evaluation suggest the presence of a virilizing tumor |
1. Bailey-Pridham D.D., Sanfilippo J.S. Hirsutism in the adolescent female. Pediatr Clin North Am. 1989;36:581–599.
2. Bates G.W. Hirsutism and androgen excess in childhood and adolescence. Pediatr Clin North Am. 1981;28:513–530.
3. Gilchrist V.J., Hecht B.R. A practical approach to hirsutism. Am Fam Physician. 1995;52:1837–1846.
4. Gordon C.M. Menstrual disorders in adolescents: excess androgens and the polycystic ovary syndrome. Pediatr Clin North Am. 1999;46:519–543.
5. Hunter M.H., Carek P.J. Evaluation and treatment of women with hirsutism. Am Fam Physician. 2003;67:2565–2572.
6. Leung A.K., Robson W.L. Hirsutism. Int J Dermatol. 1993;32:773–777.
7. Miller W.L. Pathophysiology, genetics, and treatment of hyperandrogenism. Pediatr Clin North Am. 1997;44:375–395.
8. Plouffe L. Disorders of excessive hair growth in the adolescent. Obstet Gynecol Clin. 2000;27:79–99.
9. Redmond G.P., Bergfeld W.F. Diagnostic approach to adrogen disorders in women: acne, hirsutism, and alopecia. Cleve Clin J Med. 1990;57:423–427.
10. Rosenfield R.L. Hyperandrogenism in peripubertal girls. Pediatr Clin North Am. 1990;37:1333–1358.
11. Speroff L., Glass R.H., Kase N.G. Clinical Gynecologic Endocrinology and Infertility, 6th ed. Baltimore: Lippincott Williams & Wilkins; 1999. 529–556