Disorders of the Subcutaneous Tissue
Bernard A. Cohen
Introduction
The subcutaneous fat cushions the overlying skin, insulates and provides energy storage, and protects underlying soft tissue and bony structures. Although not fully functional at birth, a well-developed fatty layer is present in the neonate, even when premature.1 Disorders of the fat can interfere with normal function and may have systemic implications.
The nomenclature and classification of subcutaneous fat disorders of the newborn are inconsistent and confusing. However, a number of entities have been recognized because of their distinctive clinical patterns, histopathology, biochemical and genetic markers, inheritance, and course. The clinician must distinguish disorders that are innocent and self-limiting from those that are associated with significant morbidity or underlying systemic disease.
Subcutaneous fat necrosis of the newborn
Subcutaneous fat necrosis of the newborn (SCFN) is an uncommon disorder that occurs primarily in full-term and post-mature infants during the first few weeks of life. Although lesions can develop in infants with a normal delivery and neonatal course, SCFN has been associated with perinatal complications, including asphyxia, hypothermia, seizures, pre-eclampsia, meconium aspiration, and intrapartum medication.2–5 Extensive subcutaneous fat necrosis has also been reported following therapeutic hypothermia used in newborns with severe perinatal asphyxia and surgical procedures.6–8
Although the first reports of SCFN appeared during the early nineteenth century, many investigators continued to use the terms scleroderma or scleredema to describe SCFN, as well as a number of diverse disorders of the subcutaneous tissue associated with the development of distinct nodules or widespread induration. Over a century later, the term subcutaneous fat necrosis was first applied to this clinically benign condition with histologic characteristics of fat necrosis.5
Cutaneous findings
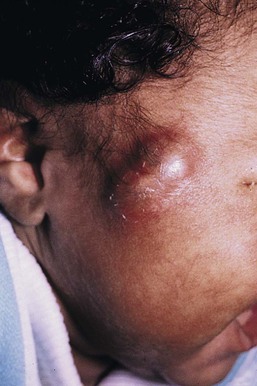
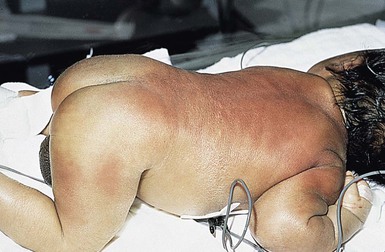
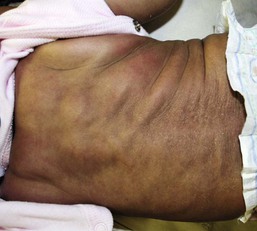
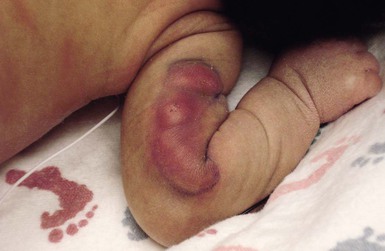
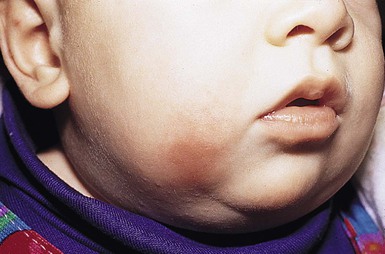
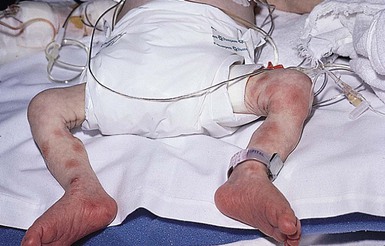
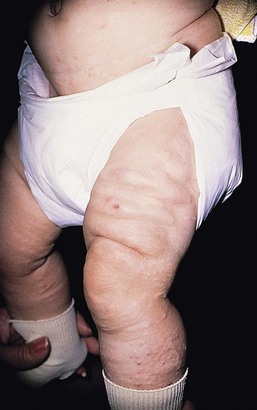
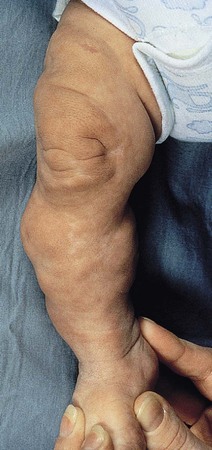
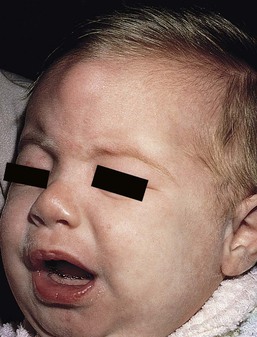
Affected infants typically present with one or several indurated, variably circumscribed, violaceous or red plaques or subcutaneous nodules from one to several centimeters in diameter on the buttocks, thighs, trunk, face, and/or arms (Figs 27.1–27.4). In some cases, the nodules may be subtle, not associated with overlying color change, and only appreciated by careful palpation of the underlying fat. Rarely, large plaques may cover extensive areas of the trunk or extremities. However, lesions are usually freely movable over subjacent muscles and fascia. Although SCFN may be tender, affected infants are afebrile and usually asymptomatic.
Most SCFN regresses spontaneously without scarring over several weeks to months. Rarely nodules persist for over 6 months.9 Occasionally, fluctuance and abscess-like changes occur, resulting in spontaneous drainage and scar formation. Variable amounts of calcification develop, which can be appreciated radiographically.10
Etiology and pathogenesis
Some investigators have proposed that SCFN results from hypoxic injury to fat caused by local trauma, particularly in the child with perinatal complications.11,12 This is supported by the observation that fat necrosis occurs commonly over bony prominences. Others have suggested that the susceptibility to SCFN results from an increased proportion of the saturated fats palmitic and stearic acid, relative to the monounsaturated fat oleic acid in neonatal subcutaneous tissue.9,11,13 Saturated fatty acids have a higher melting point than unsaturated fats, which may predispose newborn fat to crystallization at higher ambient temperatures than fat in older children and adults. Consequently, even in the setting of mild hypothermia, crystallization of fat may occur, with subsequent fat necrosis. Finally, an underlying defect in neonatal fat composition or metabolism, possibly related to immaturity, in the setting of perinatal stress, may lead to fat necrosis.
Diagnosis
Although SCFN is usually diagnosed clinically, when the presentation is atypical or the infant is ill, the diagnosis can be confirmed by skin biopsy showing the characteristic histopathologic findings of patchy areas of necrosis and crystallization of fat. The involved fat lobules contain pathognomonic needle-shaped clefts surrounded by a mixed inflammatory infiltrate composed of lymphocytes, histiocytes, fibroblasts, and foreign body giant cells.5 Fine-needle aspiration biopsy is a safe and reliable alternative.14
Although laboratory tests are usually normal, hypercalcemia occurs occasionally from 1 to 4 months after the appearance of skin lesions.9,11–13 The risk of hypercalcemia increases with the severity of the perinatal insult and extent of fat necrosis.15 Rarely hypercalcemia is severe, and has been implicated in the deaths of three infants. Nephrocalcinosis, vomiting, failure to thrive, poor weight gain, irritability, and seizures can complicate high calcium levels or chronic moderate elevations.2,7 Although the exact cause of hypercalcemia is unknown, several explanations, including elevated parathyroid hormone levels, prostaglandin E2 release, calcium release from necrotic fat, and elevated levels of vitamin D, have been proposed. Calcitriol produced by macrophages in the inflammatory infiltrate of SCFN with increased calcium absorption in the gastrointestinal tract is the favored explanation.4,5,11–13
Soft tissue calcification may occur in the absence of hypercalcemia and can be detected radiographically. Tests of parathyroid function, vitamin D metabolites, and urinary prostaglandins may be useful in the evaluation of infants with hypercalcemia. Hypocalcemia with pseudohypoparathyroidism requiring therapy,16 as well as transient hypoglycemia, hypertriglyceridemia, and thrombocytopenia,17 have also been reported in several children.
Differential diagnosis
The subcutaneous nodules that follow the abrupt withdrawal of systemic steroids can be difficult to distinguish from those of SCFN. However, they usually occur on the cheeks, arms, and trunk 1–2 weeks after discontinuation of steroids. SCFN can be distinguished from sclerema neonatorum, lipogranulomatosis, infectious panniculitis, and nodular panniculitis by the general well-being of the infant with SCFN and characteristic clinical and histopathologic features. Infants with sclerema neonatorum present with diffuse skin stiffness and severe multisystem disease. Deep soft tissue infections in neonates are usually associated with fever and other signs of sepsis. Subcutaneous hemangiomas, soft tissue tumors such as rhabdomyosarcomas, fibromatosis of infancy, and histiocytosis can be excluded by imaging studies, disease course, and histologic findings. When hypercalcemia and/or soft tissue calcification is present, primary hyperparathyroidism, osteoma cutis, and calcification associated with Albright osteodystrophy should be excluded.
Management
In most infants with SCFN, treatment is limited to parental reassurance and supportive measures.4,11–13 Hypercalcemia, if present, may have clinical signs such as poor growth or irritability, or may be entirely asymptomatic. Although onset is most commonly noted at 4–6 weeks of age and usually resolves by 4 months, some cases have reported to persist for 6 months. As a consequence, at-risk infants should be monitored for the first 6 months of life and should not receive vitamin D supplementation for rickets prophylaxis during this period.3,15 Treatment of hypercalcemia may require intravenous saline, calcium-wasting diuretics, and rarely, intravenous corticosteroids. Etidronate therapy has also been reported to be successful in controlling severe hypercalcemia in SCFN.13 Ulcerated lesions, which rarely occur in otherwise healthy infants, usually respond to topical antibiotics and bio-occlusive dressings.
Sclerema neonatorum
Sclerema neonatorum is a rare clinical finding rather than a distinct disorder that affects debilitated term and premature infants during the first 1–2 weeks of life.5 It occasionally occurs in older infants up to 4 months of age with severe underlying disease. Over the last decade, it has only rarely been reported in North America, but the persistence of cases in the developing world is probably related to an increased risk of malnutrition, diarrheal disease, low birthweight and subsequent sepsis.18,19
Cutaneous findings
Diffuse hardening of the skin usually appears suddenly on the 3rd or 4th day of life, starting over the lower extremities, especially the calves, spreading to the thighs, buttocks, and cheeks, and eventually the trunk.5,20–24 Sclerema eventually involves most of the skin, particularly in premature infants, with the exception of the palms, soles, and genitals. The skin feels cold, smooth, hard, and bound down. The joints are immobile, and the face appears mask-like.
Extracutaneous findings
Affected infants are usually poorly nourished, dehydrated, hypotensive, hypothermic, and septic. Necrotizing enterocolitis, pneumonia, intracranial hemorrhage, hypoglycemia, and electrolyte disturbances are also often associated with sclerema.5,21–26
In most cases, sclerema is limited to the subcutaneous fat. However, in two infants, autopsy revealed identical changes in the visceral fat.27
Etiology and pathogenesis
The development of sclerema is probably a result of dysfunction of the neonatal enzymatic system involved in the conversion of saturated palmitic and stearic acids to unsaturated oleic acid. Immaturity of the neonatal lipoenzymes is further compromised by hypothermia, infection, shock, dehydration, and surgical and environmental stresses. The relative abundance of saturated fatty acids and depletion of unsaturated fatty acid allows for fat solidification to occur more readily, with the subsequent development of sclerema.5,20,21
Diagnosis
On gross pathologic examination, the subcutaneous tissue of affected infants is markedly thickened, firm, and lard-like, with fibrous bands seen to extend from the fat into the lower dermis. Microscopically, early lesions demonstrate distinctive lipid crystals within fat cells, forming rosettes of fine, needle-like clefts.5,21 Although there is usually no inflammatory reaction to fat necrosis, occasionally some giant cells are present. Older lesions often show thickened septa, and rarely calcification.
Other laboratory findings in neonates with sclerema are nonspecific and usually reflect the underlying systemic medical problems. Thrombocytopenia, neutropenia, active bleeding, and worsening acidosis carry a poor prognosis.5,25,26
Differential diagnosis
In healthy infants who develop widespread slowly progressive scleroderma-like plaques on the trunk and proximal extremities, the diagnosis of stiff skin syndrome should be considered (see below). However, this is a primary disorder of fascia and, unlike sclerema, is not associated with systemic symptoms. The lack of inflammation and extensive involvement of the subcutis help to distinguish sclerema from SCFN and cold panniculitis, in which the lesions are localized and associated with exuberant granulomatous inflammation. Diffuse edema resulting from hemolytic anemia, renal, and/or cardiac dysfunction manifests as pitting edema, unlike sclerema. Congenital lymphedema or Milroy disease is nonpitting and often widespread. However, in lymphedema, the infant is otherwise healthy, and a skin biopsy reveals normal fat and dilated lymphatics. Erysipelas or lymphangitis is red, tender, and more localized than sclerema. Diffuse sclerodermatous changes associated with systemic sclerosis, which is extremely rare in the newborn, can also mimic sclerema. However, histology demonstrates characteristic hypertrophy and sclerosis of collagen, which eventually replaces the fat in scleroderma.
Treatment
Attention to the maintenance of a neutral thermal environment, electrolyte and water balance, adequate hydration and ventilation, and aggressive treatment of shock and infection in the modern nursery intensive care unit, undoubtedly account for the extremely low incidence of sclerema today. Although most infants with sclerema succumb to sepsis and shock, reversal of the underlying systemic disease can result in recovery.
The role of systemic steroids in the management of infants with sclerema is controversial. Several investigators have reported a favorable outcome when exchange transfusion was combined with conventional therapy.21,26
Stiff skin syndrome
In 1971, Esterly and McKusick28 described a disorder in infants and young children characterized by diffuse skin induration and thickening, with limitation of joint mobility, flexion contractures, and hypertrichosis. This condition, which has been called ‘congenital fascial dystrophy’ or the ‘stiff skin syndrome’ was further defined by Jablonska and colleagues29 as a generalized, noninflammatory disease of fascia without evidence of visceral or muscle involvement, immunologic abnormalities, or vascular hyperreactivity. Although most cases have been sporadic, disease affecting two siblings,30 a mother and two siblings,28 and another family with affected family members in multiple generations, support a hereditary transmission.31
Cutaneous findings
Stiff skin syndrome presents in infancy or early childhood with scleroderma-like plaques initially affecting the trunk and proximal extremities, particularly the buttocks and thighs. In the first stages, the condition may seem subtle and somewhat localized. Progression of the rock-hard indurated bound-down skin over large areas of the body, including the extremities, results in contractures, scoliosis, a narrow thorax, and a characteristic tiptoe gait. A variable increase in hair may be noted over areas of cutaneous involvement.28,29,31–35
Extracutaneous findings
Orthopedic abnormalities result from the cutaneous and fascial plaques that produce contractures, especially over large joints. Although restrictive pulmonary changes and growth retardation have occasionally been reported, immunologic, visceral, bony, muscular, and vascular involvement is characteristically absent.29,32–34
Etiology and pathogenesis
Although the cause is unclear, investigators have proposed a primary fibroblastic defect resulting in increased mucopolysaccharide deposition in the dermis, a primary fascial dystrophy resulting from increased collagen, and an inflammatory process.29,32–34 Some patients with stiff skin syndrome have been noted to have increased myofibroblastic activity in fascia, with overproduction of type VI collagen. Similar findings have been observed in extra-abdominal desmoid tumors, juvenile hyaline fibromatosis, scleroderma, and the tight skin mouse model which is transmitted in an autosomal dominant pattern and is located on chromosome 2.36 Cutaneous fibrosis in the Tsk mouse appears to be caused by a mutation in Fibrillin-1. A mutation in Fibrillin-1 has also been demonstrated in 4 families with autosomal dominant stiff skin syndrome.31
Diagnosis
In infants and young children with progressive bound-down plaques beginning on the trunk, limited joint mobility, and no evidence of systemic disease, stiff skin syndrome should be considered. Varying histologic changes from patient to patient and in the same patient over time, may reflect different triggers which result in similar clinical findings.32–34,36 In some cases, thickening of the collagen in the fascia was noted, whereas in others the fascia was normal and increased mucopolysaccharide deposition was found in the dermis. Noninflammatory sclerosis in the deep reticular dermis extending into the subcutaneous fat has also been noted. A recent report suggests that, although noninflammatory fibrosis of the fat and fascia is typical but not specific for incisional biopsies of stiff skin syndrome, the presence of a lattice-like array of thickened, horizontally oriented collagen bundles may be a clue to diagnosis.37
Differential diagnosis
Firm, woody induration of the skin with joint contractures may occur in geleophysic dysplasia, progeria, neonatal mucolipidosis II, and Farber lipomatosis. These disorders can be distinguished from stiff skin syndrome by their characteristic clinical, histologic, biochemical, and genetic findings. The clinical features of scleroderma overlap with some cases of stiff skin syndrome. Although thickening of the fascia does not usually occur in scleroderma, in some cases of linear scleroderma, deep soft tissues and bone can be involved. However, the lesions are usually self-limited. Eosinophilic fasciitis, which presents with acral scleroderma-like changes, can also be distinguished by characteristic clinical features, course, and histology. Sclerema neonatorum and subcutaneous fat necrosis of the newborn demonstrate a distinctive panniculitis and clinical course, and infantile systemic hyalinosis can be distinguished by the presence of hyaline deposits in the skin, multiorgan failure, and death in early childhood. In milder cases, the condition may mimic a connective tissue nevus, smooth muscle hamartoma, or myofibroma.
Treatment
Although the disorder is usually slowly progressive, in some patients lesions have been noted to stabilize or improve. Treatment is generally limited to supportive and rehabilitative care.
Panniculitis caused by physical agents
Although physical agents may contribute to the development of SCFN and sclerema neonatorum, a number of environmental factors can cause direct injury to the fat. Cold, heat, mechanical trauma, and chemical injury can lead to the formation of nodules in the fat. The overlying epidermis is usually unaffected in cold and mechanical trauma, whereas bullae, erosions, and ulcerations from epidermal and dermal necrosis characterize heat and chemical insults.
Cold panniculitis
The development of panniculitis following exposure to subfreezing temperatures was first noted over 70 years ago, by Haxthausen who described four young children and an adolescent with facial plaques.38,39 In his paper, he referred to several earlier reports of hardening of the fat associated with cold exposure and the application of ice directly to the skin.40,41 Similar cases have been reported following the use of ice to induce hypothermia before cardiac surgery,40 and the application of ice bags to the face for management of supraventricular tachycardia.41,42 Popsicle panniculitis is a term coined by Epstein in 1970 to refer to a specific subset of cold panniculitis triggered by infants sucking on flavored ice.43 Although lesions may develop in older children and adults, most cases occur in infants under 1 year.
Cutaneous findings
Symmetric, tender, indurated nodules and plaques 1–3 cm in diameter typically appear on the cheeks of infants 1–2 days after cold exposure.38,39,42–44 The overlying skin appears red to violaceous (Fig. 27.5), and the infant is otherwise well. In a study by Rotman39 the application of an icecube to the volar aspect of the forearm of an 8-month-old girl resulted in mild transient erythema for 15 min. A red plaque developed 12–18 h later and resolved after 13 days. Lesions usually soften, flatten, and heal over 2–3 weeks, leaving post-inflammatory pigmentary changes, particularly in darkly pigmented individuals.
Etiology and pathogenesis
As in subcutaneous fat necrosis of the newborn and sclerema neonatorum, exposure to low ambient temperatures is thought to result in crystallization of the subcutaneous tissue in infants, which is relatively high in saturated fats compared to that of older children and adults. Applying ice to the skin for 50 seconds results in nodules in all newborns, but only in 40% of 6-month-old and only occasionally in 9-month-old infants.43 In 1966, Duncan and colleagues45 described a child in whom nodules followed the application of ice for several minutes at 6 months of age, and 8 min at 18 months of age. When the child was 22 months old, ice applied for 15 min did not trigger panniculitis. The resistance to cold injury correlates with the relative increase in unsaturated fats in the subcutaneous tissue of older infants and children.
Diagnosis
The development of subcutaneous nodules in any neonate or young infant exposed to ice or subfreezing temperatures in the preceding 1–3 days should suggest the diagnosis of cold panniculitis. Histologic changes evolve over several days.45 The earliest changes 24 h after cold injury include an infiltrate of macrophages and lymphocytes at the dermoepidermal junction extending into the dermis and fat. At 48 h, the inflammation is more intense and fat necrosis is present. Lipid from ruptured fat cells forms large cystic structures surrounded by histiocytes, neutrophils, and lymphocytes. These changes become more pronounced over the next few days, and subside completely in 2 weeks.
Other laboratory studies, including blood counts, cold agglutinins, cryoglobulins, and general chemistry studies, are usually normal.
Differential diagnosis
The history of cold exposure in an otherwise healthy infant will help to distinguish cold panniculitis from other causes of subcutaneous nodules. Clinical lesions of SCFN can overlap with those of cold panniculitis. Although a skin biopsy is not usually necessary to distinguish these two disorders, the distribution of nodules and histological changes is usually distinctive. Cellulitis should also be considered in any child with tender red facial nodules. However, the lack of progression of lesions or fever in a healthy-appearing infant is against the diagnosis of infection.
Post-steroid panniculitis can be clinically indistinguishable from cold panniculitis.46 Subcutaneous nodules or plaques appear on the cheeks of infants within 2 weeks of rapidly discontinuing high-dose systemic steroids after a prolonged course. A biopsy reveals granulomatous inflammation in the fat lobules and needle-shaped clefts within histiocytes identical to those of SCFN. However, in a child with a typical history, a biopsy is unnecessary, and nodules resolve over a period of months without treatment.
Treatment and course
Although skin lesions are self-limiting and no treatment is recommended, early recognition of cold panniculitis is important to prevent unnecessary parental anxiety or laboratory studies. Nodules heal in 1–3 weeks without scarring.
Mechanical trauma
Cutaneous findings
Firm, subcutaneous nodules may follow blunt trauma to the skin, especially in areas prone to trauma where the fat is in close proximity to the underlying bone.47 This occurs most commonly on the cheeks in children between 6 and 12 years old. However, nodules can also develop in infants and over other bony prominences after accidental or deliberate injury.
Diagnosis
Traumatic fat injury should be considered in any child with subcutaneous nodules over injury-prone areas. Skin biopsies will demonstrate fat necrosis with granulomatous inflammation. Late histologic changes may include fibrosis, small fat cysts, and dystrophic calcification.48 However, a biopsy is usually not necessary.
Treatment and course
Nodules slowly resolve over 6–12 months without treatment. In some patients localized lipoatrophy can lead to a depression with normal overlying epidermis and dermis.
Injection-site granuloma
Cutaneous findings
Firm, asymptomatic, itchy, or tender, subcutaneous nodules commonly appear 1–2 days after vaccinations in the buttocks or thighs in infants, and in the deltoid area in older children and adults.49,50 Although lesions occasionally result from direct trauma to the subcutaneous tissue when the needle is accidentally placed in the fat, some patients develop aluminum granulomas when an aluminum-adsorbed vaccine is used.
Diagnosis
The diagnosis is apparent when one or several nodules develop in a vaccination injection site. Skin biopsies demonstrate characteristic findings, including lymphoid follicles with germinal centers and a dense surrounding infiltrate of lymphocytes, histiocytes, plasma cells, and eosinophils. Staining for aluminum is also positive, confirming the diagnosis.49
Differential diagnosis
Other foreign material injected into the skin can produce panniculitis, with nodule formation and fat necrosis. This can occur with certain medications and intravenous fluid extravasation.51 Munchhausen syndrome by proxy should be considered when recurrent panniculitis with associated cellulitis and/or ulceration occurs in an otherwise healthy infant without a clear diagnosis.
Treatment and course
Injection-site granulomas usually resolve without scarring within 2 weeks, although they can last much longer. Occasionally, liponecrosis leads to ulceration and/or lipoatrophy, with persistent dimpling of the skin.
Infectious panniculitis
Although this entity usually occurs in immunocompromised adults, there are rare reports of affected children in the pediatric and infectious disease literature.52–54 In infants, infectious panniculitis can occur as an extension of primary cutaneous infection, direct hematogenous dissemination to fat, or inoculation from a penetrating wound or indwelling catheter.20
Cutaneous findings
Septic emboli produce tender, red, subcutaneous nodules that are usually confined to one area, such as a portion of an extremity, but widespread dissemination can occur (Fig. 27.6).
In primary cutaneous infection, superficial tissue destruction by the invading organism and ischemia from invasion of local blood vessels and lymphatics leads to necrosis and ulceration of the skin and deeper soft tissue structures.
Etiology and pathogenesis
Infectious panniculitis has been associated with Gram-positive (Staphylococcus aureus, S. epidermidis, Streptococcus sp.) and Gram-negative (Pseudomonas sp., Klebsiella sp., Fusobacterium, Fusarium) bacteria, fungi (Candida sp., Nocardia sp.), and atypical mycobacteria.
Differential diagnosis
Other conditions to be considered in the setting of possible panniculitis associated with fever include erythema nodosum, Henoch–Schönlein purpura (HSP), and cellulitis. The most difficult of these to exclude is erythema nodosum, an immunologically mediated phenomenon commonly associated with streptococcal and other infections. In erythema nodosum, the panniculitis occurs primarily in the fat septa, and the infecting organisms are not found in the skin nodules. HSP is not usually associated with fever, and skin biopsy shows leukocytoclastic vasculitis.
Treatment and course
Treatment should be directed against the specific organism. Skin biopsy for pathology and cultures, blood cultures, and other appropriate cultures will hopefully identify a specific organism and direct antibiotic and/or antifungal therapy.
Tumors of fat
Tumors of fat include a number of neoplasms and hamartomatous malformations. A specific diagnosis is important to distinguish between those disorders with isolated cutaneous findings and those with systemic implications.
Lipoma
Cutaneous findings
Although lipomas represent the most common tumor of the mesenchyme in adults, they are rare in infants and account for <5% of tumors of childhood. Lipomas are soft, rounded or lobulated, mobile, slightly compressible, subcutaneous tumors with smooth margins (Fig. 27.7). Lumbosacral lipomas are usually congenital and occur in conjunction with intraspinal lipomas and anomalies of the spine (Fig. 27.8).56–59 They are often softer and less discrete than lipomas found in other sites. When infants and young children present with multiple lipomas, especially when the lesions are congenital, the clinician should do a careful medical and cutaneous examination to exclude rare underlying systemic disorders.
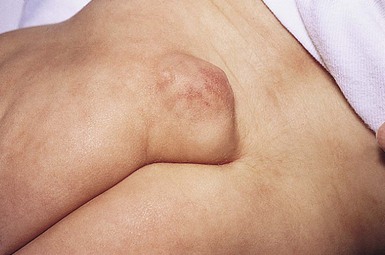
Extracutaneous findings
In 1967, Lassman and James56 described 26 cases of lumbosacral lipomas associated with laminar defects on X-ray and spinal anomalies at surgery. The recognition of lipomas as markers of underlying spinal dysraphism has been re-emphasized by a number of investigators.56–59 Conversely, most cases of intraspinal lipoma are associated with congenital lumbosacral cutaneous markers, including lipoma, myelocele closure scar, hairy patch, vascular lesions, and dimpling (see also Chapter 9).58
A sporadic, nonhereditary, genetic, mosaic disorder with lipomas and segmental fat hypoplasia was recently described with the acronym CLOVE syndrome (congenital lipomatous overgrowth, vascular malformations, and epidermal nevi).60 This disorder is characterized by linear epidermal nevi, progressive, complex, and mixed truncal vascular malformations (typically combined venous lymphatic malformations), dysregulation of adipose tissue, and enlarged bony structures without progressive bony overgrowth. Heterogeneous central system structural anomalies have also been described. In 2012 investigators reported a distinct somatic activating mutation in the P1K3CA gene as the cause of CLOVE syndrome.61 When CLOVE syndrome is suspected, a systemic evaluation and imaging studies should be directed by clinical findings. CLOVE syndrome should be distinguished from PTEN-associated lipomatous disorders including Proteus syndrome, Bannayan–Riley–Ruvalcaba syndrome, and Cowden syndrome which share a number of clinical findings with CLOVE.62,63 Children with PTEN-associated disorders are also at risk for the development of malignant tumors in adulthood and should be screened accordingly.63
Diagnosis
The presence of a soft, spongy congenital mass in the lumbosacral area is characteristic, and requires a radioimaging evaluation to exclude anomalies of the underlying cord and bony spine. Ultrasound is a reliable noninvasive screening tool for infants during the first 6 months of life. In older children, or when the findings are equivocal on ultrasound, MRI may be required.64,65 Histologic findings are typical of lipomas in other sites and show mature adipocytes within a thin connective tissue capsule.
Treatment, course, and management
Although the need for surgical management of intraspinal lipomas associated with lumbosacral lipomas is controversial, it should be recognized that the development of neurologic impairment can be delayed for years.56–59 Unfortunately, many patients present in later childhood and adolescence with neurologic defects in the lower extremities, including weakness and foot deformities. Consequently, immediate neurosurgical evaluation and long-term neurologic follow-up are required.
Nevus lipomatosus cutaneous superficialis
Nevus lipomatosus cutaneous superficialis (NLCS) is a malformation of the subcutaneous tissue consisting of multiple or solitary papules, usually occurring on the lower trunk, buttocks, or upper thighs.66–69 Based on the paucity of reports, NLCS is either rare or underdiagnosed. In 1921, Hoffmann and Zurhelle69 described the original case of a 25-year-old man with multiple papules on the left buttock. In 1975, Jones and colleagues70 summarized the findings of an additional 40 cases subsequently reported in the literature, and 20 of their own patients. A number of other reports have expanded our understanding of the clinical expression and pathogenesis of NLCS.
Cutaneous findings
Most patients report that lesions were present at birth or appeared in the first two decades of life.66–69 However, a number of reports suggest that appearance of lesions may be delayed until the third to fifth decades of life.71 NLCS typically presents as multiple, soft, skin-colored to yellowish lobules that may coalesce into plaques with a cerebriform surface. Unilateral involvement of the buttock is most common, but plaques may extend to the adjacent skin of the upper thigh or lower back. Lesions may be confined to the upper thigh, lower back, hip, or abdomen. Usually lesions do not cross the midline, but bilateral involvement of opposing surfaces of the buttocks has been reported. Once formed, papules usually remain stable. However, new lobules may develop slowly for decades, and recurrent lesions after excision or progression may be associated with infiltration of the underlying muscle.72
Solitary nevi have been described at various sites, including the scalp, ear, and neck, but these lesions probably represent fibromas or polypoid fibrolipomas rather than true NLCS.
Extracutaneous findings
NLCS is not usually associated with extracutaneous findings.66–69 Cases reported with bony, dental, and other anomalies probably represent focal dermal hypoplasia (Goltz syndrome), which can be confused clinically and histologically with NLCS. However, there are several reports of NLCS associated with pigment anomalies, including café-au-lait spots and hypopigmented macules.
Etiology and pathogenesis
Although the origin of NLCS is unclear, electron microscopic studies support the hypothesis of several investigators that the hamartomatous lesion arises from pluripotential vascular elements in the dermis.67 The presence of varying amounts of other connective tissue components also suggests a relationship with connective tissue nevi.
Diagnosis
Although the clinical appearance of NLCS varies, the presence of typical nodules and plaques in the pelvic girdle region should suggest the diagnosis. Histopathology shows some hyperkeratosis and acanthosis of the epidermis and a marked increase in mature fat cells throughout the dermis.67,69 Adipocytes are most prominent in the reticular dermis, where they are arranged in clusters and interspersed by broad, interwoven, collagen bundles. However, they may extend into the papillary dermis, and the distinction between the dermis and subcutaneous fat may be poorly defined. Although the remainder of the dermis often appears normal, other connective tissue anomalies, including thickening of collagen and elastic fibers, and increased numbers of fibroblasts and blood vessels with a perivascular mononuclear infiltrate, may also develop.
Differential diagnosis
The varying clinical findings explain the wide range of clinical diagnoses suspected before skin biopsy. These include pigmented nevi, supernumerary nipples, lipomas, neurofibromas, connective tissue nevi, sebaceous nevi, epidermal nevi, and warts.
Encephalocraniocutaneous lipomatosis and congenital diffuse lipomatosis (‘Michelin tire baby’) may represent distinctive variants of NLCS (see below).
Treatment, course, and management
Although new lobules may develop in adolescence and adult life, NLCS is usually static and not associated with pain, pruritus, or other symptoms. Consequently, treatment is not necessary, but surgical excision, particularly for small lesions, gives a good cosmetic result. Moreover, excision should be considered in lesions that demonstrate progressive growth.73
Encephalocraniocutaneous lipomatosis
In encephalocraniocutaneous lipomatosis (ECL), unilateral cerebral malformations are associated with ipsilateral scalp, face, and eye lesions.74 Since the first description of this congenital neurocutaneous disorder in 1970 by Haberland and Perou,75 at least 60 additional cases with similar clinical and histologic findings have been reported.76–80
Cutaneous findings
Soft, spongy, hairless, pink-yellowish tumors characteristically involve the scalp, often in a linear configuration, but may extend to the legs and paravertebral area.74–80 On the scalp, these lesions are sometimes referred to as nevus psiloliparus (see Chapter 31).76 Although lesions are usually unilateral, bilateral involvement has been reported. Papular and polypoid nodules, often contiguous to the scalp lesions, are constant features on the face of affected infants. Atrophic hairless patches may also be present on the scalp and face.74
Extracutaneous findings
Characteristic papules and nodules on the bulbar conjunctivae show histologic features of desmoid tumors.74 Anomalies of the hyaloid vessel system, lens, and cornea are also common.81
Cerebral defects are usually ipsilateral to the main cutaneous scalp lesions and include ventricular dilatation and cerebral atrophy.74,82 Other anomalies, including arachnoidal cyst, pontocerebellar lipoma, porencephaly, agenesis of the corpus callosum, and paramedullary lipomas, have also been described.
Affected children seem to be prone to the development of benign osseous lesions, including ossifying fibromas, odontomas, osteomas, and fibrous dysplasia.79 Recently, low-grade gliomas79 and intracranial vascular malformations have also been described.80
Etiology and pathogenesis
There is no evidence of familial transmission or chromosomal aberration, and all cases have been sporadic. Happle83 proposed that ECL might be caused by a lethal autosomal mutation that survives in the mosaic state.
Diagnosis
Biopsies of the cutaneous nodules show normal epidermis overlying a dermis with irregularly shaped collagen fibers that extend into the subcutis and form large fibrous septa associated with increased amounts of fat.74–78 These histologic features typical of fibrolipoma seen in children with characteristic cutaneous, ocular, and cerebral features should suggest the diagnosis of ECL.
Differential diagnosis
The clinical features of ECL may overlap with those of focal dermal hypoplasia (Goltz syndrome), oculoauricular vertebral dysplasia (Goldenhar syndrome), Schimmelpenning syndrome, oculocerebrocutaneous (Dellman) syndrome, Proteus syndrome, and the epidermal nevus syndrome. However, careful analysis of clinical and histologic features will help to distinguish these neurocutaneous genodermatoses.
Treatment and course
The care of affected children is determined by neurologic symptoms, which range from normal to global neurodevelopmental retardation, unilateral spasticity, and mental retardation.74 Seizures are variable and may develop later in childhood. Moreover, the severity of neurologic symptoms does not seem to correlate with the extent of cutaneous involvement. Ocular and cutaneous lesions appear to be static and amenable to surgical repair. Children without clinical evidence of neurologic involvement should be screened for occult spinal anomalies.82
Congenital diffuse lipomatosis
Congenital diffuse lipomatosis (Michelin tire baby) was initially referred to by Ross in 1969,84 who described a child with ringed creases of the skin reminiscent of the mascot of the French tire manufacturer Michelin. Since then, a number of cases of this rare hamartomatous disorder have been reported, demonstrating the variability of clinical and histologic findings.84–89
Cutaneous findings
Symmetric ringed creases of the extremities may be associated with hirsutism of the arms, legs, shoulders, and buttocks (Fig. 27.9).84–88 The palmar and plantar skin may also demonstrate excessive folding. Although scalp hair is usually normal, long curled eyelashes and thick eyebrows are typical.
Extracutaneous findings
Although affected children may be otherwise normal, a number of anomalies have been reported.84–88 Facial dysmorphisms have included epicanthal folds, hypertelorism, an antimongoloid slant to the eyes, a flat nasal bridge, and low-set ears. Variable oral anomalies, including cleft lip and palate, a high-arched palate, dental hypoplasia, and micrognathia, are common. Orthopedic defects such as rocker-bottom feet, metatarsus abductus, coxa valga, genu valgus, overlapping of toes, and pectus excavatum may require surgical intervention. Psychomotor delay and the development of seizures are also variable.
Etiology and pathogenesis
Although no specific chromosomal abnormality has been identified in congenital diffuse lipomatosis, autosomal dominant inheritance has been noted in two families in which the cutaneous findings occurred as isolated defects.87 In two other patients with multiple associated anomalies, unrelated cytogenetic defects were found.85 Further studies may help to detect a Michelin tire baby gene, although this syndrome may represent disparate disorders with similar phenotypic expression.
Diagnosis
Skin biopsies from the extremities of affected children have shown changes in the dermis consistent with nevus lipomatosus cutaneous superficialis or smooth muscle hamartoma.85,86 A report in which histopathology showed fragmented elastic fibers and decreased deposition of elastin on electron microscopy suggests that some cases may result from a primary defect in elastic fibers.86
Differential diagnosis
Although congenital diffuse lipomatosis may be confused histologically with localized smooth muscle hamartoma, Becker nevus, and nevus lipomatosis cutaneous superficialis, the diffuse, symmetric, and dramatic cutaneous findings are distinctive.
Treatment, course, and management
Management of affected individuals depends on the presence of associated anomalies. Clinicians should look carefully for oral and orthopedic anomalies, which may require early surgical intervention. Neurodevelopmental parameters will also require long-term follow-up.
Congenital pedal papules
Congenital papules or nodules of the plantar surface of the feet have been described under a variety of names, including congenital pedal papules, congenital piezogenic-like papules, plantar fibromatosis of the heel, ‘podalic papules of the newborn,’ and precalcaneous fibrolipomatous hamartoma.90–93
Cutaneous findings
Pedal nodules are asymptomatic, symmetric, flesh-colored nodules of the medial plantar surface of the feet, generally 0.5–1.5 cm in size (Fig. 27.10). They are ill-defined and may go unnoticed by caregivers. Lesions undergo minimal change over time, though proportionate growth may be seen.
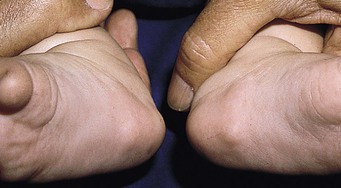
Etiology and pathogenesis
The pathogenesis is uncertain. Possible etiologies include a hamartomatous condition with incomplete regression of fetal tissue or a developmental defect in the plantar aponeurosis. The nodules may occur in a familial pattern.94 Histopathology displays increased mature adipocytes in the mid and deep dermis within fibrous sheaths.
Diagnosis and differential diagnosis
The diagnosis is a clinical one. Differential diagnosis includes piezogenic papules seen on the lateral surface of the feet in older children, fibrous hamartoma of infancy, and aponeurotic fibroma.
Treatment and course
Although the natural history is not fully known, lesions seem to persist over time. Treatment is unnecessary.
Lipoblastoma and lipoblastomatosis
Lipoblastoma is a term first used by Jaffe95 in 1926 to describe recurrent fatty tumors of the groin in infants and young children. Van Meurs96 subsequently wrote of his experience with an infant with a lipomatous tumor in the right axilla that required four surgeries over a 2-year period before she was free of recurrence. Histologic changes from biopsies over the 2-year period in Van Meurs’ case demonstrated maturation from a tumor comprised primarily of lipoblasts to a mature lipoma. In 1973 Chung and Enzinger97 reported a large series of lipomatous tumors in infancy and proposed that the term lipoblastoma be used to describe the well-encapsulated variant and that lipoblastomatosis be reserved for unencapsulated infiltrating lesions.
Cutaneous findings
Clinically, the tumors are soft, subcutaneous or deep, soft tissue masses ranging in size from 1 to 12 cm in diameter.98–101 Although cases have been diagnosed in children as old as 10 years, most appear before 3 years of age, and congenital tumors are common. In a recent review of 410 cases, 68% were encapsulated and 32% had a diffuse growth pattern; 80% were on the trunk and extremities (Fig. 27.11), 17% head and neck, and 5% face and head. However, unusual sites, including the parotid gland, mediastinum, and tonsils, have been reported. Some 98% were under 20 years old and 78% under 3, and there was a 1.5 : 1 male to female predominance.101
Etiology and pathogenesis
Although the cause of lipoblastoma is unknown, several reports demonstrate an association with rearrangements of chromosome band 8q 11–13 which targets the gene PLAG1.101,102 Electron microscopic findings suggest a close resemblance to human fetal adipose tissue.103 Some investigators propose that lipoblastoma results from the continued proliferation of fetal lipoblasts in the postnatal period. This is supported by observations of histologic maturation of adipose cells in recurrent tumors.
Diagnosis
Histologically, lipoblastoma is encapsulated or well circumscribed, whereas in lipoblastomatosis the tumor infiltrates surrounding normal structures.97–99,101 The diagnostic feature is the presence of lobules of mature and immature fat cells, primitive mesenchymal cells, and lipoblasts with varying degrees of differentiation. The lobules are separated by fibrous septa containing small blood vessels, hyaline collagen, and fibroblasts. There is no evidence of atypia, and mitotic figures are rare.
Differential diagnosis
Lipoblastomatosis should be differentiated from liposarcoma, an exceedingly rare tumor in children under 10 years of age.99 Although histologic distinction is occasionally difficult, the lack of cytologic atypia and mitotic figures and the presence of a uniform growth pattern and extensive lobulation favor lipoblastoma. MRI features showing enhancing cystic lesions and enhancing soft tissue nodules may help to distinguish lipoblastoma from other lipomatous tumors in young children.104
Treatment and course
Encapsulated tumors represent the majority of lesions and generally respond well to simple excision. However, in some series lipoblastomatosis accounts for nearly a third of cases. Metastases do not occur, but recurrences are common. Although extensive infiltration into local muscle and fascial structures precludes complete excision, in most cases maturation of recurrent tumor results in a favorable outcome.
Lipodystrophies
The lipodystrophies are a rare group of disorders characterized by complete or partial loss of fat. The congenital variants are inherited in an autosomal recessive pattern and express variable abnormalities in carbohydrate and lipid metabolism and insulin resistance.
Leprechaunism
Donohue and Uchida105,106 were the first to describe this rare syndrome when they reported their observations on two sisters of consanguineous parents, with intrauterine growth retardation, gnome-like facies, and severe endocrine dysfunction evidenced by emaciation, enlargement of the breasts and clitoris, and histologic changes in the ovaries, pancreas, and breasts.107 Leprechaunism was the term applied to the elfin facial features and poor growth characteristic of this disorder.
The incidence of this autosomal recessive disorder has been estimated at 1 in 4 million live births, and the prevalence of the carrier state as at least 1 in 1000 individuals.108
Cutaneous findings
In a review of 31 patients with leprechaunism reported since the original description by Donohue in 1948, Elsas and colleagues109 summarized the clinical findings, including severe growth retardation; an elfin face with large, protuberant, low-set ears; depressed nasal bridge with a broad nasal tip and flared nares; thick lips; distended abdomen; relatively large hands, feet, nipples, and genitalia; and abnormal skin with hyperpigmentation, café-au-lait spots, hypertrichosis, acanthosis nigricans, pachyderma, and decreased subcutaneous fat (Fig. 27.12).109–111 The virtual absence of fat gives a cachectic appearance, with wrinkled skin hanging loosely over the skeletal frame.
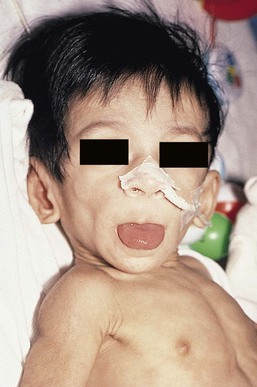
Etiology and pathogenesis
Initially leprechaunism was identified as a primary endocrinologic disorder because of the associated cystic changes of the gonads and hyperplasia of the islet cells of the pancreas. In the 1970s and 1980s, laboratory advances led to the identification of severe insulin resistance resulting from a genetic defect of the insulin receptor system in infants with leprechaunism.109,110 Using molecular genetic techniques, the first defect in the insulin receptor gene was discovered in a child with leprechaunism in 1988.112 Subsequently, multiple mutations have been described, indicating that there is great genetic heterogeneity in this disorder.113 Overactivation of insulin-like growth factor-1 (IGF-1) by high levels of insulin and lack of functional insulin receptors in a number of organ systems lead to growth failure, lipodystrophy, and other cutaneous findings.
Diagnosis
Diagnosis can be made by identifying characteristic clinical, biochemical (fasting hypoglycemia, postprandial hyperglycemia, and extreme hyperinsulism), and genetic findings.113 The diagnosis can be confirmed by DNA analysis of fibroblasts grown in culture from skin biopsies from affected infants. Specific mutations in the insulin receptor gene can be identified. Prenatal diagnosis is possible by similar evaluation of chorionic villus biopsy specimens.
Differential diagnosis
Leprechaunism shares many features with congenital total lipoatrophy, including insulin resistance, absence of subcutaneous fat, acanthosis nigricans, and hyperpigmentation. The differential also includes Rabson–Mendenhall syndrome, and HAIR-AN syndrome.114 However, the elfin facies, wrinkled skin, and other cutaneous markers are distinctive.
Treatment and course
Postnatal growth is invariably poor, and affected children are severely motor and mentally retarded. Infants rarely survive beyond the first few months of life unless they have some residual insulin receptor function. Stabilization of blood glucose during early infancy is critical for survival. Recent data suggest that the administration of recombinant IGF1 may be effective in managing the primary defect.115
Congenital generalized lipodystrophy (seip–berardinelli syndrome)
Congenital generalized lipodystrophy (CGL) was first described by Berardinelli in 1954, and in greater detail by Seip in 1959.116,117 In 1996, Seip published a follow-up study of the original patients and summarized the findings from over 90 cases reported in the literature.118 Over the last decade, the discovery of genetic markers has resulted in the identification of four distinctive CGL variants.119
Cutaneous findings
A partial to complete absence of subcutaneous fat and marked muscular hypertrophy are evident at birth and persist through adolescence. The findings at birth are most dramatic in infants with Berardinelli–Seip syndrome (CGL2). The skin tends to become coarse, particularly in boys, and patients often develop warty fibromas on the upper half of the body.107,116,118 Acanthosis nigricans develops to a variable degree in early childhood but disappears in adolescence. Excessive, curly scalp hair and hypertrichosis are also common.
Extracutaneous features
An anabolic state develops, with increased height velocity, advanced bone and dental age, muscular hypertrophy, masculine body build, acromegaloid stigmata, organomegaly, and enlarged genitals.116–118 Growth velocity is already advanced at birth and continues throughout childhood. The absence of facial fat pads and enlarged muscles gives adolescent girls a female ‘body-builder’ look.
Patients tend to be hypermetabolic with a voracious appetite, increased energy consumption, and associated hyperhidrosis and decreased heat tolerance. Cardiac muscle hypertrophy is also present at birth and may result in progressive hypertrophic cardiomyopathy with decrease in cardiac function. Most patients with CGL demonstrate mild to moderate developmental delay and mental retardation.
Infants with CGL1 lack metabolically active fat but retain mechanical adipose tissue (e.g., foot and finger pads, bone marrow). In CGL3, patients demonstrate short stature, and vitamin D resistance, and CGL4 infants present with congenital myopathy, pyloric stenosis, and cardiomyopathy.119
Etiology and pathogenesis
Although the clinical findings in CGL disorders overlap considerably, the identification of four distinct genetic mutations has allowed for the definition of a number of variants.119,120 Most affected children have CGL1 or CGL2 (Berardinelli–Seip syndrome). CGL1 is associated with a mutation in the AGPAT2 gene, which is necessary for the production of key enzymes required for biosynthesis of triglycerides and phospholipids. CGL2 results from mutations in the BSCL2 gene which encodes seipin, which plays a role in the fusion of small lipid droplets and adipose differentiation. CAV1 mutations in CGL3 and PTRF mutations in CGL4 result in defects in adipose membranes.
Diagnosis
This is a well-characterized disorder inherited in an autosomal recessive fashion, with clinical, metabolic, and genetic features that allow for diagnosis at birth. Metabolic features include insulin resistance, hyperinsulinemia, hypertriglyceridemia, and nonketotic diabetes. Skin biopsies demonstrate a marked decrease in adipocyte size and number.118 Unlike the subcutaneous fat, glycogen and triglycerides are abundant in the liver, where variable amounts of connective tissue with liver cirrhosis have been noted. Hypertriglyceridemia varies from patient to patient, but tends to increase at puberty and with increased dietary fat consumption. In childhood, glucose and insulin levels tend to be normal except with large glucose challenges. However, at or shortly after puberty, glucose metabolism deteriorates, with the development of clinical diabetes with hyperinsulinemia, elevated serum glucose, and glycosuria. When clinical and metabolic findings suggest a diagnosis of CGL, the diagnosis can be confirmed with genetic markers.
Differential diagnosis
CGL can be distinguished from other lipodystrophies by the characteristic congenital onset and associated clinical, metabolic, and genetic findings. CGL can also be distinguished from neonatal progeroid syndrome, which presents with generalized decreased subcutaneous fat, by the presence of increased buttock fat, absence of the typical CGL metabolic findings and the presence of progeroid features including sparse scalp hair, prominent scalp veins, hypoplastic facial bones, and convex nasal bridge. Neonatal progeroid syndrome, described in the late 1970s by Wiedemann and Rautenstrauch is inherited as an autosomal recessive disorder but the genetic marker has not yet been identified. However, investigators have suggested that a defect in biosynthesis of proteins in the nucleus may be involved.121
Treatment and course
Treatment is complex and should emphasize dietary measures to control energy consumption, hyperglycemia, and hypertriglyceridemia.118 Appetite suppressants have been used with some success. Therapy is further complicated by moderate to severe mental retardation in most individuals with CGL. Despite therapy, many patients die in childhood of liver cirrhosis or associated complications and/or cardiomyopathy.
Congenital disorders of glycosylation (CDG)
CDG, previously known as carbohydrate-deficient glycoprotein syndrome (CDGS), represents a heterogeneous group of disorders, which all share clinical features that result from a defect in the synthesis of N-linked oligosaccharides.122–124 During the last decade the discovery of a number of genetic defects has resulted in the categorization of type 1 and type 2 CDG. Type 1 disorders are the most common and usually associated with congenital onset.125
This entity was first recognized by Jaeken and colleagues in 1980,126 who reported monozygotic twins with psychomotor retardation, increased CSF protein, delayed nerve conduction velocity, thyroxine-binding deficiency, and increased serum arylsulfatase A activity. Carbohydrate analysis of a number of subsequent patients resulted in identification of the common defect in N-linked glycoproteins.
Cutaneous findings
Dysmorphic features typical of CDG type 1 appear in infancy, including inverted nipples and an abnormal distribution of fat over the suprapubic region and labia majora.122–124 Peculiar fat pads, which tend to disappear in later childhood, are noted on the superior lateral portion of the buttocks. Lipoatrophy can be marked on the rest of the buttocks, and lipoatrophic streaks often extend down the legs. Variable facial dysmorphisms include a high nasal bridge, prominent jaw, and large pinnae.
Extracutaneous findings
Neurologic features include hypotonia, hyporeflexia, and alternating esotropia.118 Infants often suck poorly and present with feeding difficulties. Even when nutritional intake is good, lipoatrophy gives many children an emaciated appearance. Although most infants are full term and appropriate weight for gestational age, developmental delay, and failure to thrive usually occur by 3 months of age.
Significant coagulopathy may result in stroke-like episodes, and hepatomegaly with hepatic dysfunction is common. Renal cysts, pericardial effusions, pericardial tamponade, and hypertrophic obstructive cardiomyopathy have been reported.
Although the central nervous system involvement tends to be static, musculoskeletal complications, including muscular atrophy, contractures, and spinal deformities, progress in later childhood and adulthood. In females, defective peptide hormone glycosylation results in hypogonadotrophic hypogonadism with failure to undergo pubertal sexual development. Males are virilized at puberty, but may exhibit decreased testicular volume. Other endocrinologic findings result from hyperglycemia-induced growth hormone release, hyperprolactinemia, and insulin resistance.
Etiology and pathogenesis
In both type 1 and type 2 disorders, multiple variants based on specific genetic defects have been named based on the chronological order in which they were discovered. For type 1 and 2 there are groups a–o and a–h, respectively. These autosomal dominant inherited disorders have been tied to specific defects in N-linked oligosaccharide synthesis.125
Diagnosis
Typical clinical features seen in association with the presence of abnormally glycosylated serum proteins, typically transferrin detected by cathodal migration on serum isoelectric focusing, may allow for diagnosis in the neonatal period. This can be confirmed by specific genetic analysis.
Prenatal diagnosis can be made with mutational studies along with enzymatic analysis of amniotic fluid or chorionic villus cells.125,127
Differential diagnosis
Although other lipodystrophies should be considered, the clinical features are usually distinctive. When dysmorphic features are subtle, biochemical studies are required to distinguish CDG from related disorders.
Treatment and course
Supportive treatment is necessary to avoid complications from the central nervous system, as well as ophthalmologic and hematologic manifestations of CDG. Mannose has been used to deal with some of the acute crises of infancy, including intractable seizures, severe coagulopathy, and pericardial effusions, but does not change the dismal prognosis.
Farber lipogranulomatosis
Farber disease is a rare autosomal recessive disorder of lipid metabolism that usually presents with a fatal course in early infancy.124,128,129 Although skin, joint, and laryngeal symptoms associated with neurodegeneration are characteristic, some patients may present with later onset of primarily neurologic findings.
Clinical findings
Tender, red, subcutaneous nodules and swelling appear during the first few weeks of life over joints and areas of trauma, particularly the wrists and ankles. Granulomatous infiltration of the larynx results in a weak, hoarse cry.128,129 Infants are usually irritable, and psychomotor retardation is severe. Reticuloendothelial involvement may produce generalized lymphadenopathy and marked hepatosplenomegaly.
Etiology and pathogenesis
In Farber disease, ceramide, a normal intermediate in the metabolism of gangliosides and structurally important sphingolipids and glycolipids, accumulates as a result of a deficiency of lysosomal acid ceramidase.128 Variable storage of ceramide occurs in visceral organs and brain white matter.
Diagnosis
The biochemical defect can be demonstrated in kidney, liver, cultured fibroblasts, and leukocytes and specific defects in the human acid ceramidase gene ASAH1 can be demonstrated.128–130 Prenatal diagnosis is also possible by amniocentesis and chorionic villus sampling for biochemical and genetic analysis.
Differential diagnosis
In the young infant, the diagnosis can usually be made clinically when the classic findings are present. However, when various aspects are missing, Farber disease can be confused with juvenile rheumatoid arthritis, multicentric reticulohistiocytosis, and juvenile hyaline fibromatosis.129 Ceramide levels are normal in all of these conditions.
Treatment and course
The clinical course is usually characterized by recurrent fever and pulmonary infiltrates, with death occurring by 2 years of age. Rarely, patients present with later onset of neurologic disease followed by extraneuronal granulomas in skin and viscera. Some patients with little or no involvement of the central nervous system develop normally and survive longer.
Access the full reference list at ExpertConsult.com ![]()