Chapter 10 Brain Stem
The brain stem consists of the medulla oblongata, pons and midbrain. It is sited in the posterior cranial fossa, and its ventral surface lies on the clivus. It contains numerous intrinsic neurone cell bodies and their processes, some of which are the brain stem homologues of spinal neuronal groups. These include the sites of termination and cells of origin of axons that enter or leave the brain stem through the cranial nerves. They provide the sensory, motor and autonomic innervation of structures that are mostly in the head and neck. Autonomic fibres, which arise from the brain stem, are distributed more widely. Additional groups of neurones receive input related to the special senses of hearing, vestibular function and taste (Ch. 12). The reticular formation is an extensive and often ill-defined network of neurones that extends throughout the length of the brain stem and is continuous caudally with its spinal counterpart. Some of its nuclei are concerned with cardiac, respiratory and alimentary control; some are involved in aspects of many neural activities, and others provide or receive massive afferent and efferent cerebellar projections.
The brain stem is the site of termination of numerous ascending and descending fibres and is traversed by many others. The spinothalamic (spinal lemniscal), medial lemniscal and trigeminal systems ascend through the brain stem to reach the thalamus (see Figs 8.32, 10.22). Prominent corticospinal projections descend through the brain stem, and corticobulbar projections end within it (see Fig. 8.41).
Overview of Cranial Nerves and Cranial Nerve Nuclei
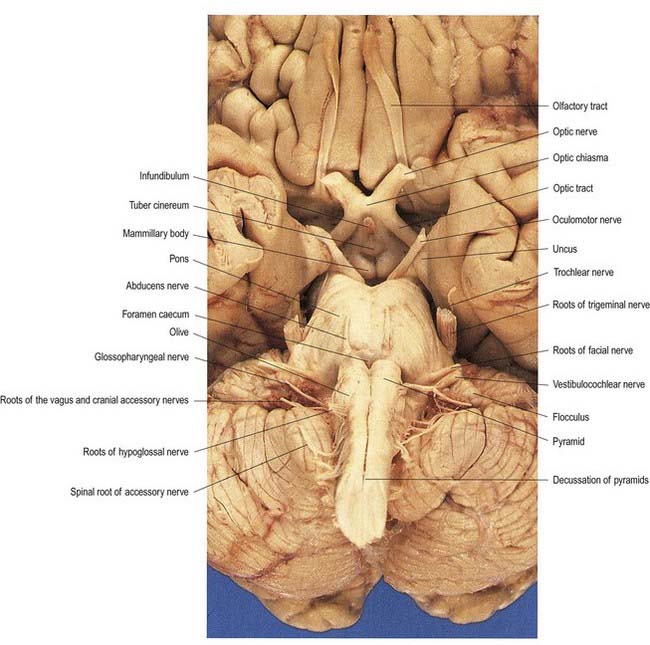
The cranial nerves are individually named and numbered (using roman numerals) in a rostrocaudal sequence (see Table 1.1). Cranial nerve I (olfactory) terminates directly in cortical and subcortical areas of the frontal and temporal lobes. It is closely associated functionally with the limbic system and is described in that context (Ch. 16). The fibres of cranial nerve II (optic) pass into the optic chiasma and emerge as the optic tract, which terminates in the lateral geniculate nucleus of the thalamus. Cranial nerves III (oculomotor) and IV (trochlear) attach to the midbrain. Cranial nerve V (trigeminal) attaches to the pons, medial to the middle cerebellar peduncle. Cranial nerves VI (abducens), VII (facial) and VIII (vestibulocochlear) attach to the brain stem at or close to the junction of the pons and the medulla. Cranial nerves IX (glossopharyngeal) and X (vagus), the cranial part of cranial nerve XI (accessory) and cranial nerve XII (hypoglossal) all attach to the medulla.
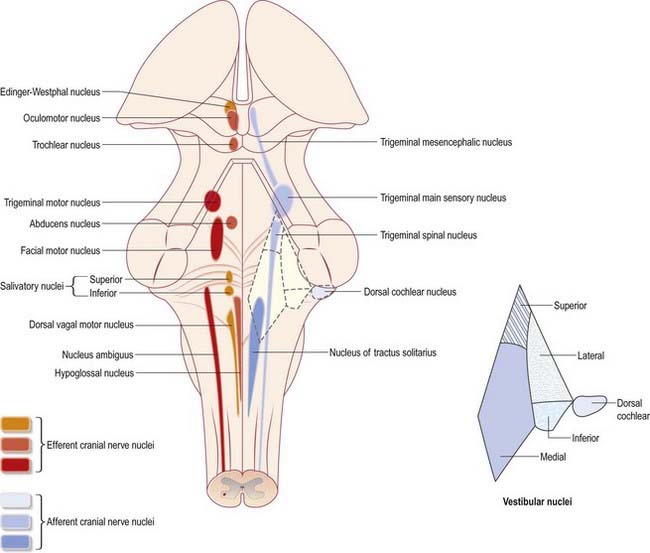
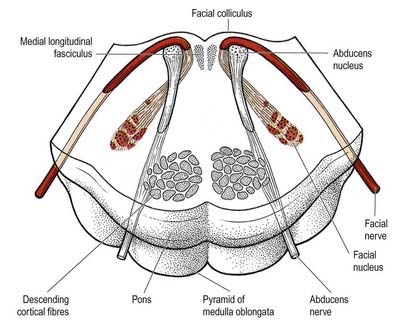
Cranial nerves III to XII, which attach to the brain stem, are associated with a number of cell groupings of varying size, referred to collectively as the cranial nerve nuclei (Fig. 10.1). The nuclei are either the origin of efferent cranial nerve fibres or the site of termination of cranial nerve afferents. For convenience, they are considered to be organized into six discontinuous, longitudinal cell columns that correspond to the columns that can be identified in the embryo (see Fig. 1.4). Three columns are ‘sensory’ and three are ‘motor’ in function.
Medulla Oblongata
External Features and Relations
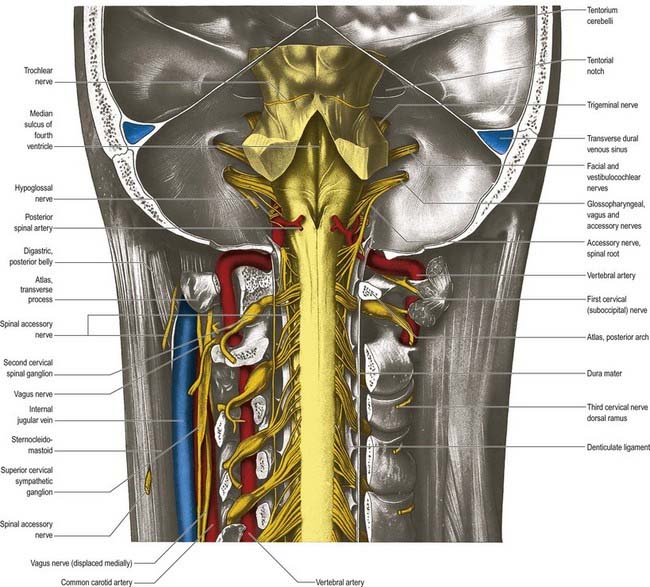
The medulla oblongata extends from the lower pontine margin to a transverse plane that is above the first pair of cervical spinal nerves and intersects the upper border of the atlas dorsally and the centre of the dens ventrally (Fig. 10.2). It is approximately 3 cm long and 2 cm in diameter at its widest. The ventral surface of the medulla is separated from the basilar part of the occipital bone and apex of the dens by the meninges and occipito-axial ligaments. Caudally, the dorsal surface of the medulla occupies the midline notch between the cerebellar hemispheres.
The ventral and dorsal surfaces of the medulla (Fig. 10.3; see also Fig. 5.11) possess a longitudinal median fissure and sulcus, respectively, which are continuous with their spinal counterparts. Caudally, the ventral median fissure is interrupted by the obliquely crossing fascicles of the pyramidal decussation. Rostrally, it ends at the pontine border in a diminutive depression, the foramen caecum. Immediately lateral to the ventral median fissure is a prominent elongated ridge called the pyramid, which contains descending pyramidal, or corticospinal, axons (see Fig. 10.3). The lateral margin of the pyramid is indicated by a shallow ventrolateral sulcus. From this emerges, in line with the ventral spinal nerve roots, a linear series of rootlets that constitute the hypoglossal nerve. The abducens nerve emerges at the slightly narrowed rostral end of the pyramid, where it adjoins the pons. Caudally, the pyramid tapers into the spinal ventral funiculus. Lateral to the pyramid and the ventrolateral sulcus is an oval prominence, the olive (Figs 10.3, 10.4), which contains the inferior olivary nucleus. Lateral to the olive is the posterolateral sulcus. The glossopharyngeal, vagus and accessory nerves join the brain stem along the line of this sulcus, in line with the dorsal spinal nerve roots.
The spinal central canal extends into the caudal half of the medulla, migrating progressively more dorsally until it opens out into the lumen of the fourth ventricle. This divides the medulla into a closed part, which contains the central canal, and an open part, which contains the caudal half of the fourth ventricle (see Figs 10.2, 5.11).
In the closed part of the medulla, a shallow posterointermediate sulcus on either side of the dorsal median sulcus, continuous with its cervical spinal counterpart, indicates the location of the ascending dorsal columns (fasciculus gracilis and fasciculus cuneatus). The ascending fasciculi are at first parallel to each other, but at the caudal end of the fourth ventricle they diverge, and each develops an elongated swelling, the gracile and cuneate tubercles, produced by the subjacent nuclei gracilis and cuneatus, respectively (Figs 10.5, 10.6). Most fibres in the fasciculi synapse with neurones in their respective nuclei, and these project to the contralateral thalamus, which in turn projects to the primary somaesthetic cortex (see Fig. 8.32). The inferior cerebellar peduncle forms a rounded ridge between the caudal part of the fourth ventricle and the glossopharyngeal and vagal rootlets. The two peduncles diverge and incline to enter the cerebellar hemispheres, where they are crossed by the striae medullares, which run to the median ventricular sulcus (see Fig. 5.11). Here also the peduncles form the anterior and rostral boundaries of the lateral recess of the fourth ventricle. This becomes continuous with the subarachnoid space through the lateral apertures of the fourth ventricle, the foramina of Luschka. A tuft of choroid plexus, continuous with that of the fourth ventricle, protrudes from the foramina on either side. The fibre composition of the inferior cerebellar peduncle is described in Chapter 13.
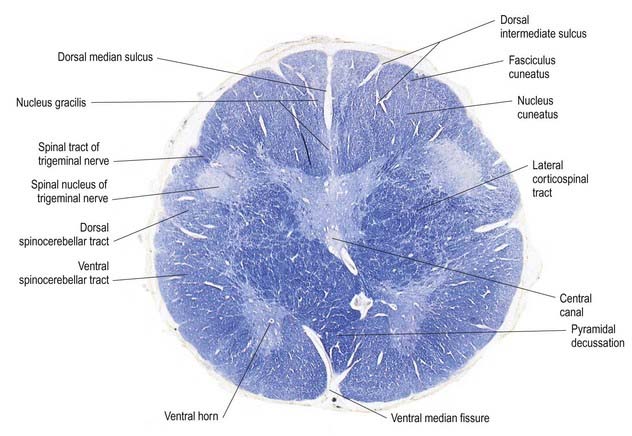
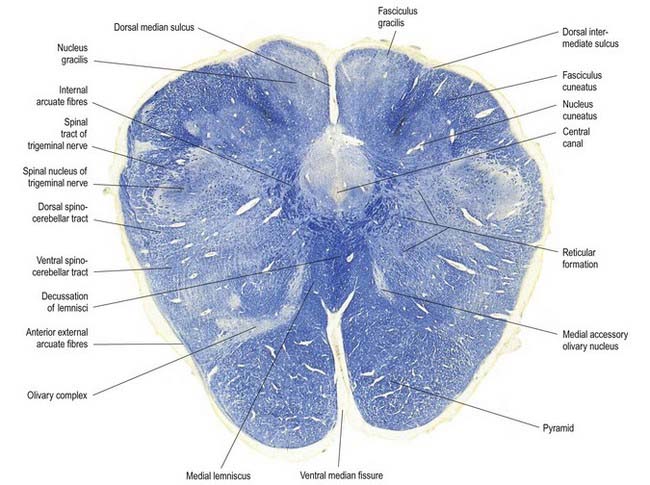
Fig. 10.5 Transverse section through the medulla oblongata at the level of the pyramidal decussation.
CASE 1 Downbeat Nystagmus and Arnold–Chiari Malformation
A 24-year-old woman presents with a long history of increasing headache, blurred vision when attempting to read and an increasingly unsteady gait with intermittent falls. Neurological examination reveals downbeat nystagmus with the eyes in the primary position, amplified by down-gaze; dysmetria of the lower extremities with heel-to-shin testing; and hyperreflexia in both lower extremities.
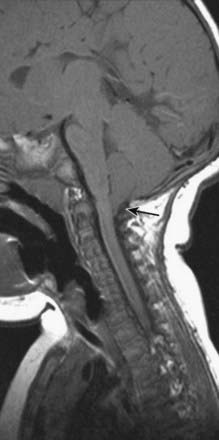
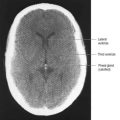
Magnetic resonance imaging (MRI) shows ‘beaking’ of the dorsal midbrain and enlargement of the lateral and third ventricles, with herniation of the cerebellar tonsils through the foramen magnum. See Figure 10.7.
A ventriculoperitoneal shunt is placed, with marked symptomatic improvement.
Internal Structure
Transverse Section of the Medulla at the Level of the Pyramidal Decussation
A transverse section across the lower medulla oblongata (see Fig. 10.5) intersects the dorsal, lateral and ventral funiculi, which are continuous with their counterparts in the spinal cord. The ventral funiculi are separated from the central grey matter by corticospinal fibres, which cross in the pyramidal decussation to reach the contralateral lateral funiculi (see Fig. 10.11). The decussation displaces the ventral intersegmental tract, the central grey matter and the central canal dorsally. Continuity between the ventral grey column and central grey matter, which is maintained throughout the spinal cord, is lost. The column subdivides into the supraspinal nucleus (continuous above with that of the hypoglossal nerve), which is the efferent source of the first cervical nerve, and the spinal nucleus of the accessory nerve, which provides some spinal accessory fibres and merges rostrally with the nucleus ambiguus.
Transverse Section of the Medulla at the Level of the Decussation of the Medial Lemniscus
The medullary white matter is rearranged above the level of the pyramidal decussation (see Fig. 10.6). The pyramids contain ipsilateral corticospinal and corticonuclear fibres, the latter distributed to nuclei of cranial nerves and other medullary nuclei. At this level, they form two large ventral bundles flanking the ventral median fissure. The accessory olivary nuclei and lemniscal decussation are dorsal.
The medial lemniscus ascends from the lemniscal decussation on each side as a flattened tract near the median raphe. As the tracts ascend, they increase in size because fibres join from upper levels of the decussation. Corticospinal fibres are ventral, and the medial longitudinal fasciculus and tectospinal tract are dorsal. Fibres are rearranged in the decussation, so that those from the nucleus gracilis come to lie ventral to those from the nucleus cuneatus. Above this, the medial lemniscus is also rearranged, with ventral (gracile) fibres becoming lateral and dorsal (cuneate) fibres medial. At this level, medial lemniscal fibres show a laminar somatotopy on a segmental basis, in that fibres from C1 to S4 spinal segments are segregated sequentially from medial to lateral.
The nucleus of the spinal tract of the trigeminal nerve (see Fig. 10.22) is separated from the central grey matter by internal arcuate fibres; it is separated from the lateral medullary surface by the trigeminal spinal tract, which ends in it, and by some dorsal spinocerebellar tract fibres. The latter progressively incline dorsally and enter the inferior cerebellar peduncle at a higher level.
Two other nuclei occur at this level. One is dorsolateral to the pyramid, and the other is medial to it and near the median plane. These are parts of the precerebellar medial accessory olivary nucleus, described with the inferior olivary nuclear complex. Precerebellar nuclei of the vestibular, pontine and reticular system are described in Chapter 13.
Transverse Section of the Medulla at the Caudal End of the Fourth Ventricle
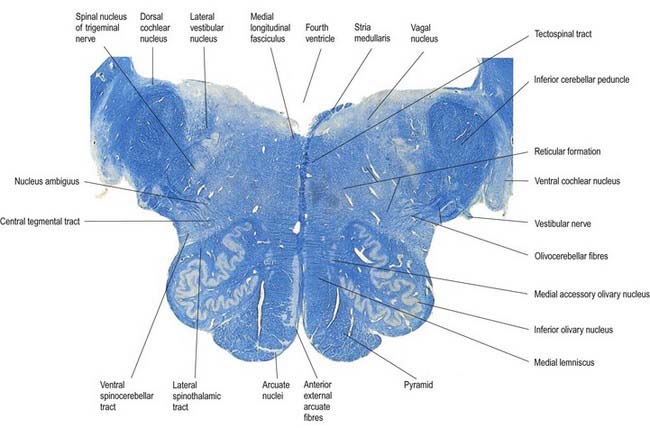
A transverse section level with the lower end of the fourth ventricle shows some new features, along with most of those already described (Fig. 10.8). The total area of grey matter is increased by the presence of the large olivary nuclear complex and nuclei of the vestibulocochlear, glossopharyngeal, vagus and accessory nerves.
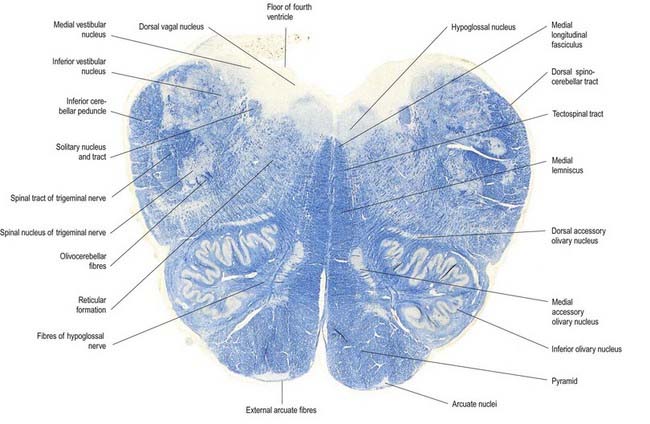
Fig. 10.8 Transverse section through the medulla oblongata at the caudal end of the fourth ventricle.
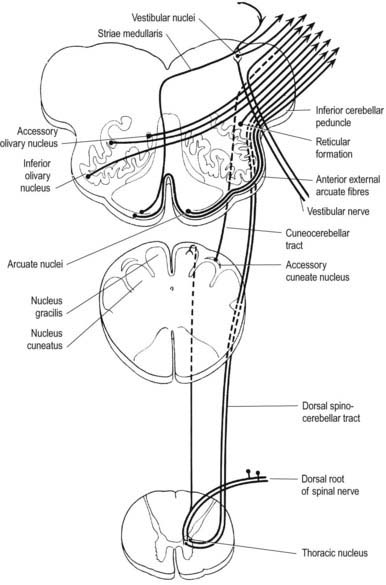
A smooth, oval elevation—the olive—lies between the ventrolateral and dorsolateral sulci of the medulla. It is formed by the underlying inferior olivary complex of nuclei and lies lateral to the pyramid, separated from it by the ventrolateral sulcus and emerging hypoglossal nerve fibres. The roots of the facial nerve emerge between its rostral end and the lower pontine border, in the cerebellopontine angle. The arcuate nuclei are curved, interrupted bands, ventral to the pyramids, and are said to be displaced pontine nuclei. Anterior external arcuate fibres and those of the striae medullares are derived from them. They project mainly to the contralateral cerebellum through the inferior cerebellar peduncle (Fig. 10.9).
The tractus solitarius and its associated circumferential nucleus solitarius extend throughout the length of the medulla. The tract is composed of general visceral afferents from the vagus and glossopharyngeal nerves. The nucleus and its central connections with the reticular formation subserve the reflex control of cardiovascular, respiratory and cardiac functions. The rostral fibres of the tract consist of gustatory fibres from the facial, glossopharyngeal and vagal nerves that project to the rostral pole of the nucleus solitarius, which is sometimes referred to as the gustatory nucleus.
The medial longitudinal fasciculus, a small, compact tract near the midline and ventral to the hypoglossal nucleus, is continuous with the ventral vestibulospinal tract. At this medullary level it is displaced dorsally by the pyramidal and lemniscal decussations. It ascends in the pons and midbrain, maintaining its relationship to the central grey matter and midline, so it is near the somatic efferent nuclear column. Fibres from a variety of sources course for short distances in the tract.
CASE 2 Avellis’ Syndrome
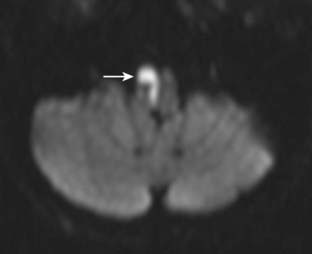
COMMENT: The patient demonstrated the classic features of Avellis syndrome due to a lesion (infarction) in the medial aspect of the lower medulla involving to variable extents. The neuro-anatomic structures involved include the corticospinal tracts causing contralateral hemiparesis, the medial lemniscus leading to impaired posterior column sensibility, the accessory nerve causing mild atrophy of the sternomastoid muscle, and the hypoglossal nerve producing atrophy of the tongue with fasciculations. This syndrome is rare, and variably described; in a number of cases, palatal weakness has been observed. See Figure 10.10.
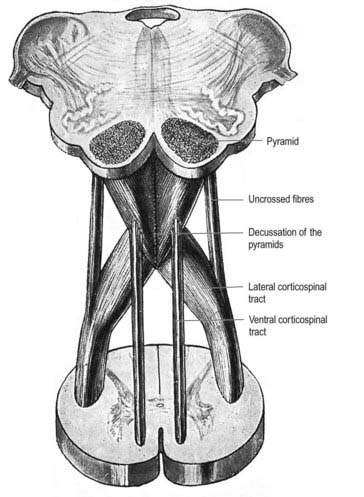
Pyramidal Tract
Each pyramid contains descending corticospinal fibres, derived from the ipsilateral cerebral cortex, which have traversed the internal capsule, midbrain and pons (Fig. 10.11). Approximately 70% to 90% of the axons leave the pyramids in successive bundles, crossing in and deep to the ventral median fissure as the pyramidal decussation. In the rostral medulla, fibres cross by inclining ventromedially, whereas more caudally, they pass dorsally, decussating ventral to the central grey matter. The decussation is orderly, with fibres destined to end in the cervical segments crossing first. They continue to pass dorsally as they descend, reaching the contralateral spinal lateral funiculus as the crossed lateral corticospinal tract. Most uncrossed corticospinal fibres descend ventromedially in the ipsilateral ventral funiculus, as the ventral corticospinal tract. A minority run dorsolaterally to join the lateral corticospinal tracts as a small uncrossed component. The corticospinal tracts display somatotopy at almost all levels. In the pyramids the arrangement is like that at higher levels, in that the most lateral fibres subserve the most medial arm and neck movements. Similar somatotopy is ascribed to the lateral corticospinal tracts within the spinal cord.
Dorsal Column Nuclei
The nuclei gracilis and cuneatus are part of the pathway that is considered the major route for discriminative aspects of tactile and locomotor (proprioceptive) sensation. The upper regions of both nuclei are reticular and contain small and large multipolar neurones with long dendrites. The lower regions contain clusters of large, round neurones with short and profusely branching dendrites. Upper and lower zones differ in their connections, but both receive terminals from the dorsal spinal roots at all levels. Dorsal funicular fibres from neurones in the spinal grey matter terminate only in the superior, reticular zone. Variable ordering and overlap of terminals, on the basis of spinal root levels, occur in both zones. The lower extremity is represented medially, the trunk ventrally and the digits dorsally. There is modal specificity; that is, lower levels respond to low-threshold cutaneous stimuli, and upper reticular levels respond to inputs from fibres serving receptors in the skin, joints and muscles. The cuneate nucleus is divided into several parts. Its middle zone contains a large pars rotunda, in which rostrocaudally elongated, medium-sized neurones are clustered between bundles of densely myelinated fibres. The reticular poles of its rostral and caudal zones contain scattered but evenly distributed neurones of various sizes. The pars triangularis is smaller and laterally placed. There is a somatotopic pattern of termination of cutaneous inputs from the upper limb on the cell clusters of the pars rotunda. Terminations are diffuse in the reticular poles.
The accessory cuneate nucleus, dorsolateral to the cuneate, is part of the spinocerebellar system of precerebellar nuclei (see Fig. 10.9); it contains large neurones like those in the spinal thoracic nucleus. These form the posterior external arcuate fibres, which enter the cerebellum by the ipsilateral inferior peduncle. The nucleus receives the lateral fibres of the fasciculus cuneatus, carrying proprioceptive impulses from the upper limb (which enter the cervical spinal cord rostral to the thoracic nucleus). Its efferent fibres form the cuneocerebellar tract. A group of neurones, called nucleus Z, has been identified in animals between the upper pole of the nucleus gracilis and the inferior vestibular nucleus and is said to be present in the human medulla. Its input is probably from the dorsal spinocerebellar tract, which carries proprioceptive information from the ipsilateral lower limb, and it projects through internal arcuate fibres to the contralateral medial lemniscus.
Trigeminal Sensory Nucleus
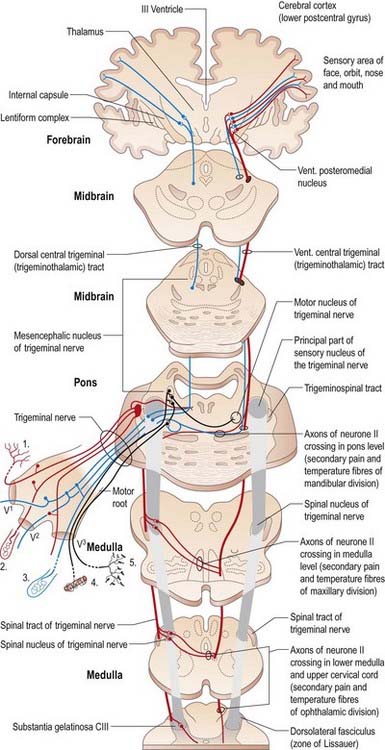
On entering the pons, the fibres of the sensory root of the trigeminal nerve run dorsomedially toward the principal sensory nucleus, which is situated at this level (Fig. 10.12). Before reaching the nucleus, approximately 50% of the fibres divide into ascending and descending branches; the others ascend or descend without division. The descending fibres, 90% of which are less than 4 µm in diameter, form the spinal tract of the trigeminal nerve, which reaches the upper cervical spinal cord. The tract embraces the spinal trigeminal nucleus (Figs 10.5, 10.6, 10.8, 10.13, 10.14). There is a precise somatotopic organization in the tract. Fibres from the ophthalmic root lie ventrolaterally, those from the mandibular root lie dorsomedially and the maxillary fibres lie between them. The tract is completed on its dorsal rim by fibres from the sensory roots of the facial, glossopharyngeal and vagus nerves. All these fibres synapse in the nucleus caudalis.
The detailed anatomy of the trigeminospinal tract excited early clinical interest because it was recognized that dissociated sensory loss could occur in the trigeminal area. For example, in Wallenberg’s syndrome (see Case 3), occlusion of the posterior inferior cerebellar branch of the vertebral artery leads to loss of pain and temperature sensation in the ipsilateral half of the face, with retention of common sensation.
The spinal nucleus is considered to consist of three parts: the subnucleus oralis (which is most rostral and adjoins the principal sensory nucleus), the subnucleus interpolaris and the subnucleus caudalis (which is the most caudal part and is continuous below with the dorsal grey column of the spinal cord). The structure of the subnucleus caudalis is different from that of the other trigeminal sensory nuclei. It has a structure analogous to that of the dorsal horn of the spinal cord, with a similar arrangement of cell laminae, and it is involved in trigeminal pain perception. Cutaneous nociceptive afferents and small-diameter muscle afferents terminate in layers I, II, V and VI of the subnucleus caudalis. Low-threshold mechanosensitive afferents of Aβ neurones terminate in layers III and IV of the subnucleus caudalis and rostral (interpolaris, oralis and main sensory) nuclei.
There are distinct subtypes of cells in lamina II. Afferents from ‘higher centres’ arborize within it, as do axons from nociceptive and low-threshold afferents. Descending influences from these higher centres include fibres from the periaqueductal grey matter and from the nucleus raphe magnus and associated reticular formation.
Vagal Nucleus
The vagal nucleus (also known as the dorsal motor nucleus of the vagus) lies dorsolateral to the hypoglossal nucleus, from which it is separated by the nucleus intercalatus. It extends caudally to the first cervical spinal segment and rostrally to the open part of the medulla under the vagal triangle (see Fig. 10.1).
Hypoglossal Nucleus
The prominent hypoglossal nucleus lies near the midline in the dorsal medullary grey matter. It is approximately 2 cm long. Its rostral part lies beneath the hypoglossal triangle in the floor of the fourth ventricle, and its caudal part extends into the closed part of the medulla (see Figs 10.2, 10.6, 5.11).
Hypoglossal fibres emerge ventrally from their nucleus, traverse the reticular formation lateral to the medial lemniscus, pass medial to (or sometimes through) the inferior olivary nucleus and curve laterally to emerge superficially as a linear series of 10 to 15 rootlets in the ventrolateral sulcus between the pyramid and olive (see Fig. 10.3).
Inferior Olivary Nucleus
The olivary nuclear complex consists of the large inferior olivary nucleus and the much smaller medial and dorsal accessory olivary nuclei. They are the so-called precerebellar nuclei, a group that also includes the pontine, arcuate, vestibular, reticulocerebellar and spinocerebellar nuclei, all of which receive afferents from specific sources and project to the cerebellum. The inferior olivary nucleus contains small neurones, most of which form the olivocerebellar tract, which emerges either from the hilum or through the adjacent wall to run medially and intersect the medial lemniscus (see Fig. 10.9). Its fibres cross the midline and sweep either dorsal to or through the opposite olivary nucleus. They intersect the lateral spinothalamic and rubrospinal tracts and the spinal trigeminal nucleus and enter the contralateral inferior cerebellar peduncle, where they constitute its major component. Fibres from the contralateral inferior olivary complex terminate on Purkinje cells in the cerebellum as climbing fibres; there is a one-to-one relationship between Purkinje cells and neurones in the complex. Afferent connections to the inferior olivary nucleus are both ascending and descending. Ascending fibres, mainly crossed, arrive from all spinal levels in the spino-olivary tracts and via the dorsal columns. Descending ipsilateral fibres come from the cerebral cortex, thalamus, red nucleus and central grey of the midbrain. In part, the two latter projections make up the central tegmental tract (fasciculus) that forms the olivary amiculum.
The medial accessory olivary nucleus is a curved grey lamina that is concave laterally and located between the medial lemniscus and pyramid and the ventromedial aspect of the inferior olivary nucleus. The dorsal accessory olivary nucleus is a similar lamina dorsomedial to the inferior olivary nucleus. Both nuclei are connected to the cerebellum. The accessory nuclei are phylogenetically older than the inferior and are connected with the palaeocerebellum. In all connections—cerebral, spinal and cerebellar—the olivary nuclei sometimes display very specific somatotopy, particularly in their cerebellar connections, which are described in detail in Chapter 13.
Nucleus Solitarius
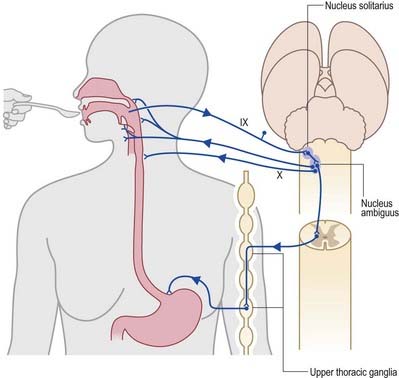
Swallowing and Gag Reflexes
During the normal processes of eating and drinking, passage of material to the rear of the mouth stimulates branches of the glossopharyngeal nerve in the oropharynx (Fig. 10.15). This information is relayed via the nucleus solitarius to the nucleus ambiguus, which contains the motor neurones innervating the muscles of the palate, pharynx and larynx. The nasopharynx is closed off from the oropharynx by elevation of the soft palate. The larynx is raised, its entrance narrows and the glottis is closed. Peristaltic activity down the oesophagus to the stomach is mediated through the pharyngeal plexus.
Nucleus Ambiguus
Cough and Sneeze Reflexes
A similar mechanism underlies sneezing (Fig. 10.16), except that the stimulus arises from the nasal mucosa, and afferent impulses are conveyed by the ophthalmic or maxillary divisions of the trigeminal nerve to the trigeminal sensory nucleus. After sharp inhalation, explosive exhalation occurs, with closure of the oropharyngeal isthmus by action of the palatoglossus, which diverts air through the nasal cavity and expels the irritant.
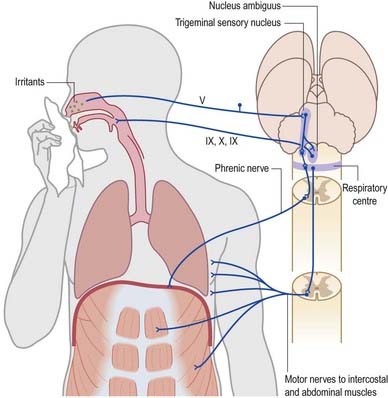
Fig. 10.16 Sneeze and cough reflexes.
(Redrawn from MacKinnon, P., Morris, J. (Eds.), 1990. Oxford Textbook of Functional Anatomy, vol 3, Head and Neck. Oxford University Press, Oxford. By permission of Oxford University Press.)
Pons
External Features and Relations
The pons lies rostral to the medulla and caudal to the midbrain. Ventrally, the site of transition with the medulla is demarcated superficially by a transverse sulcus. Laterally, in a region known as the cerebellopontine angle (see Figs 10.2, 10.3), the facial, vestibulocochlear and glossopharyngeal roots and the nervus intermedius all lie on the choroid plexus of the fourth ventricle (which protrudes from the foramen of Luschka into the subarachnoid space). The ventral surface of the pons (see Fig. 10.3) is separated from the clivus (basisphenoid and dorsum sellae) by the cisterna pontis. It is markedly convex transversely and less so vertically; it grooves the petrous part of the temporal bone laterally up to the internal acoustic meatus. The surface has a shallow vertical median sulcus in which the basilar artery runs, bounded bilaterally by prominences that are formed partly by underlying corticospinal fibres as they descend through the pons. Bundles of transverse fibres, bridging the midline and originating from nuclei in the basal pons (nuclei pontis), converge on each side into the large middle cerebellar peduncle and project to the cerebellum. The trigeminal nerve emerges near the mid-pontine level. It has a small superomedial motor root and a large inferolateral sensory root.
The dorsal surface of the pons is hidden by the cerebellum, which covers the rostral half of the rhomboid fossa, into which the aqueduct of the midbrain empties. The roof of the fossa is formed by a thin sheet of tissue, the superior medullary velum, and is overlain by the lingula of the vermis of the cerebellum. The velum is attached on each side to the superior cerebellar peduncles and is enclosed by pia mater above and ependyma below (see Fig. 5.11). The abducens nerves decussate in the velum.
Internal Structure
Transverse Sections of the Pons
Transverse sections (see Figs 10.12, 10.14) reveal that the pons consists of a dorsal tegmentum, which is a continuation of the medulla (excluding the pyramids), and a ventral (basilar) part. The latter contains bundles of longitudinal descending fibres, some of which continue into the pyramids; others end in the many pontine or medullary nuclei. It also contains numerous transverse fibres and scattered pontine nuclei.
Ventral Pons
Corticopontine fibres from the frontal, temporal, parietal and occipital cortices end in the pontine nuclei (see Fig. 10.14). Axons from the latter constitute the transverse pontine (pontocerebellar) fibres, which, after decussation, continue as the contralateral middle cerebellar peduncle. Frontopontine axons end in the pontine nuclei above the level of the emerging trigeminal roots and are relayed to the contralateral cerebellum in the upper transverse pontine fibres. All pontocerebellar fibres end as mossy fibres in the cerebellar cortex, and a degree of somatotopy is maintained in these connections.
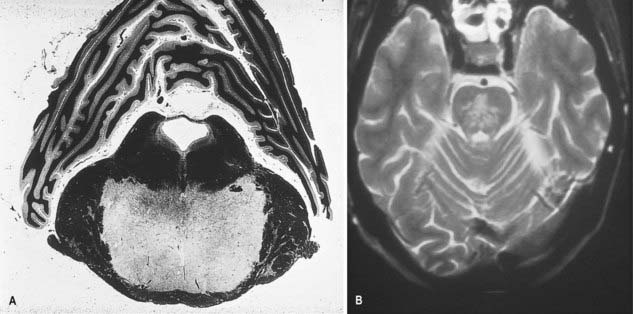
CASE 4 Central Pontine Myelinolysis
A 58-year-old poorly nourished chronic alcoholic is found to have severe hyponatremia when brought to the emergency room. The sodium deficit is corrected vigorously, but within a day or two of admission, he experiences a rapidly progressive motor deficit, with flaccid paralysis of all limbs and inability to speak or swallow, along with a facial diplegia. Ocular motility is preserved, and although he is unable to speak, he can communicate by eye-blinking responses.
Discussion: This patient exhibits a so-called locked-in syndrome, reflecting the development of central pontine myelinolysis (also called osmotic demyelination syndrome), with extensive demyelination of the mid and upper basis pontis. Paralysis of the limbs with bulbar palsy is due to an extensive symmetrically placed lesion in the basis pontis, with involvement of the descending corticobulbar and corticospinal fibres. The pontine tegmentum is usually preserved; there is little if any significant impairment of consciousness. Rapid shifts in serum osmolarity due to overvigorous correction of hyponatremia is generally believed to be the cause of this disorder. In some patients, extrapontine lesions may appear. See Figure 10.18.
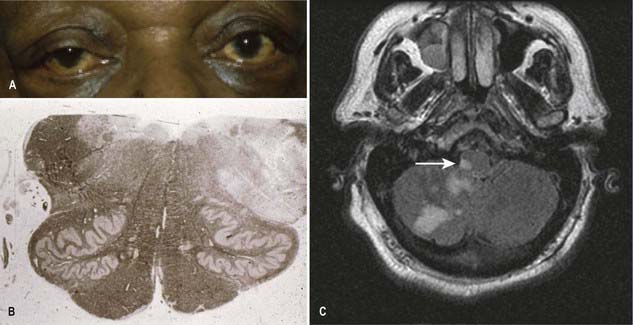
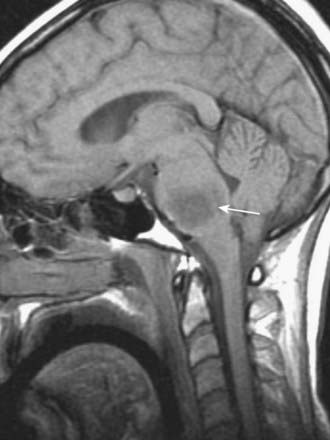
CASE 5 Brain Stem Glioma
Discussion: This subacutely evolving syndrome is most suggestive of a brain stem (pontine) glioma, a slow-growing brain stem tumor that, by virtue of its infiltrating growth characteristics, presents initially with segmental brain stem signs such as ocular palsies. Long tract signs and increased intracranial pressure due to hydrocephalus appear late in the course. See Figure 10.19.
Pontine Tegmentum
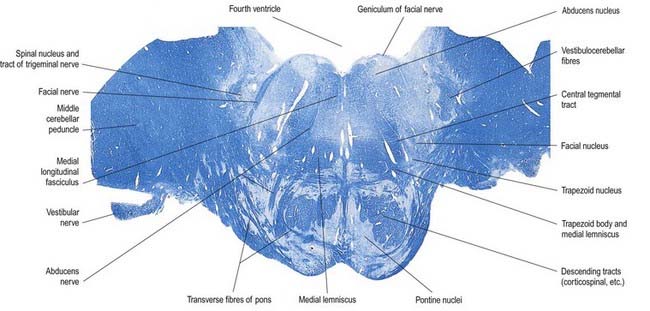
The pontine tegmentum varies in cytoarchitecture at different levels. A transverse section through the lower pontine tegmentum transects the facial colliculi (Figs 10.14, 10.20). Each colliculus contains the motor nucleus of the abducens nerve and the geniculum of the facial nerve. More deeply placed are the facial nuclei, the nearby vestibular and cochlear nuclei and other isolated neuronal groups. The medial vestibular nucleus continues from the medulla slightly into the pontine tegmentum and is separated from the inferior cerebellar peduncle by the lateral vestibular nucleus.
The vestibular nuclei are laterally placed in the rhomboid fossa of the fourth ventricle, subjacent to the vestibular area, which spans the rostral medulla and caudal pons (see Fig. 10.1). They consist of medial, lateral (Deiters’ nucleus), superior and inferior vestibular groups. They all receive fibres from the vestibulocochlear nerve and send axons to the cerebellum, medial longitudinal fasciculus, spinal cord and lateral lemniscus. Evidence suggests that the vestibular apparatus is spatially represented in the nuclei. The medial vestibular nucleus broadens, then narrows, as it ascends from the upper olivary level into the lower pons, where it separates the vagal nucleus from the floor of the fourth ventricle. It is crossed by the striae medullares nearer the floor. Below, it is continuous with the nucleus intercalatus. The inferior vestibular nucleus (which is the smallest) lies between the medial vestibular nucleus and inferior cerebellar peduncle from the level of the upper end of the nucleus gracilis to the pontomedullary junction. It is crossed by descending fibres of the vestibulocochlear nerve and the vestibulospinal tract. The lateral vestibular nucleus lies just above the inferior nucleus and ascends almost to the level of the abducens nucleus. It is composed of large multipolar neurones, which are the main source of the vestibulospinal tract. The superior vestibular nucleus is small and lies above the medial and lateral nuclei.
Vestibular fibres of the vestibulocochlear nerve enter the medulla between the inferior cerebellar peduncle and the trigeminal spinal tract and approach the vestibular area, where they bifurcate into descending and ascending branches. The former descend medial to the inferior cerebellar peduncle and end in medial, lateral and inferior vestibular nuclei, and the latter enter the superior and medial nuclei. A few vestibular fibres enter the cerebellum directly through the inferior peduncle (superficially in the juxtarestiform body) and end in the fastigial nucleus, flocculonodular lobe and uvula. Vestibular nuclei project extensively to the cerebellum and also receive axons from the cerebellar cortex and the fastigial nuclei. Their uncrossed spinal projections run in the vestibulospinal tracts. Vestibular axons also reach the spinal cord in the medial longitudinal fasciculus (see Figs 8.42, 10.26). Some reach cerebral levels, possibly for bilateral cortical representation. The vestibular nuclear complex projects to the pontine reticular nuclei and to motor nuclei of the ocular muscles in the medial longitudinal fasciculus.
The striae medullares of the fourth ventricle (see Figs 5.11, 10.13) are an aberrant cerebropontocerebellar connection in which the arcuate nuclei and external arcuate fibres are involved. Axons from arcuate nuclei spread around the medulla, above and below the inferior olive, where they are superficially visible as the circumolivary fasciculus. All these fibres, which are known collectively as the external arcuate fibres, enter the inferior cerebellar peduncle (see Fig. 10.8). Some fibres from arcuate nuclei pass dorsally through the medulla near its midline, decussate near the floor of the fourth ventricle, then turn laterally under the ependyma and enter the cerebellum through the inferior peduncle.
In addition to the tracts already noted at lower levels, the lower pontine tegmentum contains the trapezoid body, lateral lemniscus and emerging fibres of the abducens and facial nerves. The medial lemniscus is ventral, its transverse outline now a flat oval. It extends laterally from the median raphe (see Figs 10.12, 10.14) and is laterally related to the lateral spinothalamic tract and trigeminal lemniscus. The fibres of the latter originate from neurones of the contralateral spinal nucleus, serving pain and thermal sensibility in facial skin and mucosa of the conjunctiva, tongue, mouth, and nose. Here the lemnisci form a transverse band composed of, in lateral order from the midline, the medial and trigeminal lemnisci, the lateral spinothalamic tract and the lateral lemniscus.
The trapezoid body contains cochlear fibres, mainly from the ventral cochlear and trapezoid nuclei. They ascend transversely in the ventral tegmentum, pass either through or ventral to the vertical medial lemniscal fibres and decussate with the contralateral fibres in the median raphe. Below the emerging facial axons, the trapezoid fibres turn up into the lateral lemniscus. As the lateral lemniscus ascends, it lies near the dorsolateral surface of the brain stem. Above, its fibres enter the inferior colliculus and medial geniculate body. The ascending auditory pathway is described in detail in Chapter 12.
The medial longitudinal fasciculus is paramedian, ventral to the fourth venticle and near the abducens nucleus, from which it is separated by facial nerve fibres. It is the main intersegmental tract in the brain stem, particularly for interactions between nuclei of cranial nerves innervating the extraocular muscles and the vestibular system (see Fig. 10.26). In the lower pons it receives fibres from vestibular and perhaps dorsal trapezoid nuclei. Its greater part is formed by vestibulocochlear contributions.
A transverse section at an upper pontine tegmental level contains trigeminal elements (see Fig. 10.12) but otherwise shows little notable alteration from a section through a lower pontine tegmental level. Its dorsolateral parts are invaded by the superior cerebellar peduncles. The small lateral lemniscal nucleus is medial to its tract in the upper pons and receives some lemniscal terminals. Some of its efferent fibres enter the medial longitudinal fasciculus; others return to the lemniscus. The lateral lemniscal nucleus is a relay station in the auditory pathway associated with the trapezoid nucleus.
The medial lemniscus (see Figs 10.12, 8.32) retains its paramedian position in the ventral pontine tegmentum, where it lies a little lateral to the median raphe and is joined medially by fibres from the principal trigeminal sensory nucleus. The trigeminal lemniscus, lateral spinothalamic tract and lateral lemniscus and its nucleus all lie dorsolaterally.
Cochlear Nuclei
Although the cellular origins are not precisely known, axons of most neuronal types in the cochlear nuclei leave to end at pontine levels in the superior olivary, trapezoid and lateral lemniscal nuclei (see Fig. 10.12). They leave the cochlear nuclei by three routes. The largest group of axons lies ventrally and decussates as the trapezoid body, level with the pontomedullary junction (see Figs 10.12, 10.14). Most of these axons ascend slightly, decussate and relay in the contralateral nuclei. A few do not cross and synapse in the ipsilateral superior olivary nuclei. From both nuclei, the next-order axons ascend in the corresponding lateral lemniscus. Occasional decussating fibres traverse the contralateral superior olive and enter the lateral lemniscus to relay in lemniscal nuclei.
The nucleus of the lateral lemniscus consists of small groups of neurones that lie among the fibres of the lateral lemniscus. Dorsal, ventral and intermediate groups probably receive afferent axons from both cochlear nuclei. Their efferents enter the midbrain along the lateral lemniscus and terminate in the inferior colliculi (see Fig. 10.4). Total neuronal counts of 18,000 to 24,000 have been recorded in human lemniscal nuclei.
Vestibular Nuclei
The vestibular nuclear complex contains medial, lateral, inferior and superior nuclei. The medial vestibular nucleus is the largest subdivision and extends up from the medulla oblongata into the pons. It lies under the vestibular area of the floor of the fourth ventricle and is crossed dorsally by the striae medullares. The inferior vestibular nucleus is lateral to the medial nucleus and extends to a lower medullary level. It lies between the medial nucleus and the inferior cerebellar peduncle. Descending branches of afferent vestibular fibres end among its cells. The lateral nucleus is ventrolateral to the upper part of the medial nucleus and is characterized by its large neurones. Its rostral end is continuous with the caudal end of the superior nucleus, which extends higher into the pons than other subdivisions and occupies the upper part of the vestibular area.
All vestibular nuclei receive fibres from the vestibulocochlear nerve and also from the spinal cord and the reticular formation. Vestibulocerebellar fibres from the nuclei travel via the inferior cerebellar peduncle mainly to the flocculus and nodule. Some afferent fibres bypass the nuclei and reach the flocculus and nodule directly via the inferior cerebellar peduncle. Cerebellovestibular fibres pass to the nuclei in the inferior cerebellar peduncle. They arise mainly in the flocculus and nodule (posterior lobe), but some fibres are derived from the anterior lobe and fastigial nucleus (see Case 3).
In summary, the vestibular nuclear complex is a relay station on an afferent cerebellar path and a distributing station for vestibulocerebellar fibres. Fibres from vestibular nuclei also enter the medial longitudinal fasciculus (see Fig. 10.26) and ascend or descend to motor nuclei of the oculogyric and nuchal muscles. It is suggested that excitatory and inhibitory projections exist, mediating complex and subtle integration between vestibular signals and eye movements. From the vestibular nuclei, and from the lateral nucleus in particular, fibres descend in the ventral funiculus of the spinal cord as the vestibulospinal tracts. Information from the vestibular nuclei also reaches the cerebral cortex by way of the thalamus (probably via posterior parts of the ventroposterior complex and the medial pulvinar). The primary vestibular cortical area is located in the parietal lobe at the junction between the intraparietal and postcentral sulci, which is adjacent to that portion of the postcentral gyrus where the head is represented. This makes sense functionally, because this region of the somatosensory cortex is concerned with conscious appreciation of body position. There may be an additional representation of the vestibular system in the superior temporal gyrus near the auditory cortex. Through its connections, the vestibular system influences movements of the eyes, head and muscles of the trunk and limbs to maintain equilibrium.
Abducens Nucleus
The abducens nucleus occupies a paramedian position in the central grey matter, in line with the trochlear, oculomotor and hypoglossal nuclei, with which it forms a somatic motor column (see Fig. 10.1). It lies ventromedial to the medial longitudinal fasciculus, which is the means by which vestibular, cochlear and other cranial nerve nuclei, especially the oculomotor, connect with the abducens. The abducens nucleus contains large motor neurones and small multipolar interneurones, which are intermixed, although the latter are most heavily concentrated in its lateral and ventral aspects. Axons from the motor neurones cross the midline at the level of the nucleus and ascend in the medial longitudinal fasciculus to all three medial rectus subnuclei of the oculomotor nucleus. The total number of neurones in the nucleus is approximately 6500.
Efferent abducens axons pass ventrally; descend through the reticular formation, trapezoid body and medial lemniscus; and traverse the ventral pons to emerge at its inferior border (see Fig. 10.20 and Case 6).
Facial nucleus
Efferent fibres of the large motor neurones of the facial nucleus form the motor root of the facial nerve. The motor nucleus represents the branchial efferent column, but it lies much more deeply in the pons than might be expected, and its axons have an unusual course (see Fig. 10.20). At first they incline dorsomedially toward the fourth ventricle, below the abducens nucleus, and ascend medial to it, near the medial longitudinal fasciculus. They then curve around the upper pole of the abducens nucleus and descend ventrolaterally through the reticular formation. Finally, they pass between their own nucleus medially and the spinal trigeminal nucleus. They emerge between the olive and the inferior cerebellar peduncle at the cerebellopontine angle (see Fig. 10.3).
The facial nucleus receives corticobulbar fibres for volitional control. Neurones that innervate muscles in the scalp and upper face are believed to receive bilateral corticobulbar fibres, whereas those supplying lower facial musculature receive only a contralateral innervation. Clinically, upper and lower motor neurone lesions of the facial nerve can be differentiated: the former results in paralysis confined to the contralateral lower face, and the latter results in complete ipsilateral paralysis (Bell’s palsy; see Ch. 11, Case 9).
Corneal Reflex
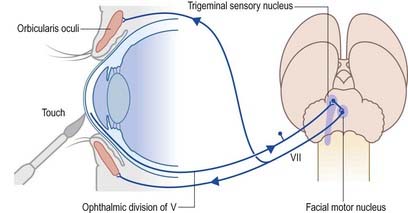
Touching the cornea or shining a bright light into the eye elicits reflex closure of the eye. The former action stimulates nasociliary branches of the ophthalmic nerve, and the latter stimulates the retina and optic pathway. In both cases, afferent impulses enter the central nervous system and spread via interneurones to activate neurones in the facial motor nucleus in the pons (Fig. 10.21). The efferent impulses pass along the facial nerve to activate the palpebral component of orbicularis oculi, which contracts, producing a ‘blink.’ The sweep of the eyelids carries lacrimal secretions across the eye, which helps remove any irritating particles.
Trigeminal Sensory Nucleus
On entering the pons, the fibres of the sensory root of the trigeminal nerve run dorsomedially toward the principal sensory nucleus (see Fig. 10.12). About 50% of the fibres divide into ascending and descending branches; the others ascend or descend without division. The descending fibres form the spinal tract of the trigeminal, which terminates in the subjacent spinal nucleus of the trigeminal nerve. The spinal nucleus was described in detail earlier.
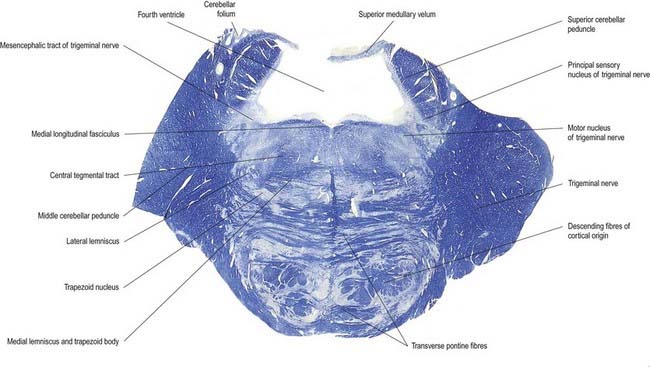
Some ascending trigeminal fibres, many of them heavily myelinated, synapse around the small neurones in the principal sensory nucleus (Fig. 10.22), which lies lateral to the motor nucleus and medial to the middle cerebellar peduncle and is continuous inferiorly with the spinal nucleus. The principal nucleus is thought to be concerned mainly with tactile stimuli.
Jaw-Jerk Reflex
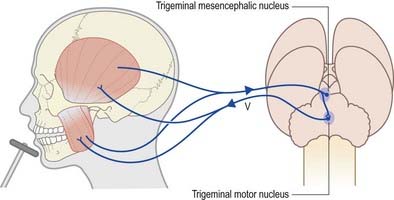
Rapid stretching of the muscles that close the jaw (masseter, temporalis, medial pterygoid) activates muscle spindle afferents, which travel via the mandibular division of the trigeminal nerve to the brain stem (Fig. 10.23). The cell bodies of these primary afferent neurones are located in the mesencephalic nucleus of the trigeminal. Collaterals project monosynaptically to the motor nucleus of the trigeminal nerve in the pons. From there, motor axons of the mandibular nerve innervate the muscles that close the jaw. Clinically, an exaggerated jaw jerk is noted with bilateral lesions in the upper brain stem.
Trigeminal Motor Nucleus
The trigeminal motor nucleus is ovoid in outline and lies in the upper pontine tegmentum, under the lateral part of the floor of the fourth ventricle (see Fig. 10.1). It lies medial to the principal sensory nucleus and is separated from it by fibres of the trigeminal nerve. It occupies the position of the branchial (special visceral) efferent column.
Midbrain
External Features and Relations
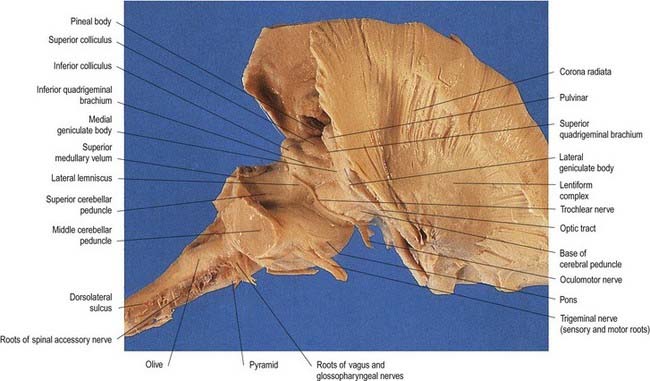
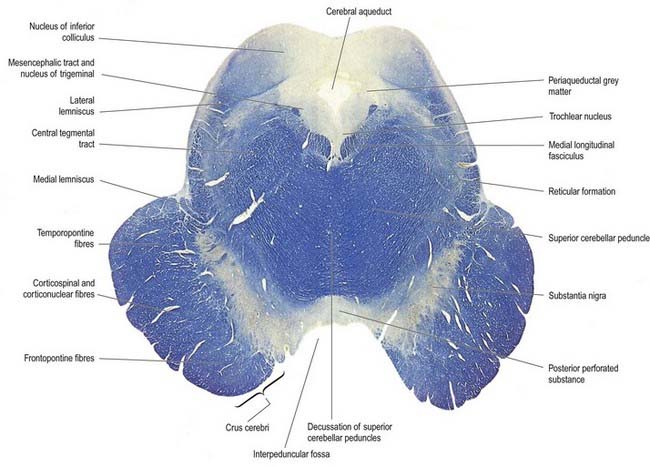
The crura cerebri are superficially corrugated and emerge from the cerebral hemispheres. They converge as they descend and meet as they enter the pons, where they form the caudolateral boundaries of the interpeduncular fossa (Figs 10.24, 10.25). At the level of the tentorial incisure, the basilar artery divides in the interpeduncular fossa into the right and left posterior cerebral arteries. The superior cerebellar arteries branch from the basilar artery immediately distal to this bifurcation. The posterior cerebral and superior cerebellar arteries both run laterally around the ventral (basilar) crural surfaces. The former passes above the tentorium cerebelli, the latter below it. The oculomotor and trochlear nerves lie between the two arteries. The roots of the oculomotor nerve emerge from a medial sulcus on each crus (see Figs 10.3, 10.24, 10.25). The posterior communicating artery joins the posterior cerebral artery on the medial surface of the peduncle in the interpeduncular fossa. The median caudal part of the interpeduncular fossa is a greyish area called the posterior perforated substance, which is pierced by central branches of the posterior cerebral arteries. The optic tract winds dorsolaterally around the crus near the crural entry into the hemispheres. Its lateral surface adjoins the parahippocampal gyrus and is crossed by the trochlear nerve (see Figs 5.11, 10.4). It bears a longitudinal lateral sulcus in which fibres of the lateral lemniscus reach and form a surface elevation. The latter inclines rostrodorsally; part joins the inferior colliculus, while the rest continues into the inferior quadrigeminal brachium.
The colliculi or corpora quadrigemina are two paired eminences (see Figs 5.11, 10.4). They lie rostral to the superior medullary velum, inferior to the pineal gland and caudal to the posterior commissure, the whole sloping ventrally as it ascends. Below the splenium of the corpus callosum, they are partly overlapped on each side by the pulvinar of the dorsal thalamus. The superior and inferior colliculi are separated by a cruciform sulcus. The upper limit of the sulcus expands into a depression for the pineal gland, and a median frenulum veli is prolonged from its caudal end down over the superior medullary velum. The trochlear nerves emerge lateral to the frenulum. They pass ventrally over the lateral aspects of the cerebral peduncles and traverse the interpeduncular cistern to the petrosal end of the cavernous sinus. The superior colliculi, larger and darker than the inferior, are stations for visual responses. The inferior colliculi, smaller but more prominent, are associated with auditory paths. The difference in colour is attributed to the presence of superficial layers of neurones in the superior colliculi.
A brachium ascends ventrolaterally from the lateral aspect of each colliculus (see Figs 5.11, 10.4). The brachium of the superior colliculus (superior quadrigeminal brachium) passes below the pulvinar, partly overlapping the medial geniculate body, and continues partly into the lateral geniculate body and partly into the optic tract. It conveys fibres from the retina and optic radiation to the superior colliculus. The brachium of the inferior colliculus (inferior quadrigeminal brachium) ascends ventrally. It conveys fibres from the lateral lemniscus and inferior colliculus to the medial geniculate body.
Internal Structure
Transverse Sections of the Midbrain
In transverse section, the cerebral peduncles are composed of dorsal and ventral regions separated by the substantia nigra (see Figs 10.24, 10.25). On each side, the dorsal region is the tegmentum and the ventral part is the crus cerebri. The tegmenti are continuous across the midline, but the crura are separated.
Crus Cerebri
Each crus cerebri is semilunar in section. It contains corticospinal, corticonuclear and corticopontine fibres. Corticonuclear and corticospinal fibres occupy the middle two-thirds of the crura and descend via the pons and medulla. Corticonuclear fibres end in the nuclei of the cranial nerves and other brain stem nuclei, whereas corticospinal fibres continue into the medullary pyramid (see Fig. 8.41). Corticopontine fibres arise in the cerebral cortex and form two groups, both of which end in the pontine nuclei. The frontopontine fibres from the frontal lobe, principally areas 6 and 4, traverse the internal capsule and then occupy the medial sixth of the ipsilateral crus cerebri. The temporopontine fibres, which are largely from the posterior region of the temporal lobe, traverse the internal capsule but occupy the lateral sixth of the ipsilateral crus. Parietopontine and occipitopontine fibres are also described in the crus, lying medial to the temporopontine fibres. There are few fibres from the primary sensory cortex in corticopontine projections.
Mesencephalic Tegmentum
The medial longitudinal fasciculus adjoins the somatic efferent column, dorsal to the decussating superior cerebellar peduncles (Fig. 10.26). The medial, trigeminal, lateral and spinal lemnisci form a curved band dorsolateral to the substantia nigra. Fibres in the medial, spinal and trigeminal lemnisci continue a rostral course to synapse with neurones in the lateral and medial ventral posterior nuclei of the thalamus, respectively (see Figs 8.33, 10.22). Some fibres of the lateral lemniscus end in the nucleus of the inferior colliculus, encapsulating it and synapsing with its neurones. The remaining fibres (direct lemniscal) join inferior colliculus–derived fibres and enter the inferior quadrigeminal brachium, which starts at this level and carries the fibres to the medial geniculate body. Some fibres to the inferior colliculus are collaterals of direct lemniscal fibres.
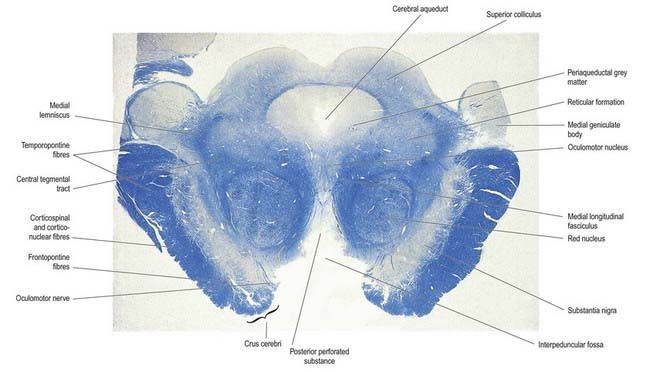
Superiorly, level with the superior colliculus, the tegmentum contains the red nucleus, which extends into the subthalamic region. The ventromedial central grey matter around the aqueduct contains the oculomotor nucleus, which is elongated and is related ventrolaterally to the medial longitudinal fasciculus and caudally reaches the trochlear nucleus. The oculomotor nucleus is divisible into neuronal groups that are partially correlated with the motor distribution of the oculomotor nerve. A group of preganglionic parasympathetic neurones, the accessory oculomotor (Edinger–Westphal) nucleus, which controls the activity of smooth muscle within the eyeball (for pupillary constriction), lies dorsal to the oculomotor nucleus (Ch. 12).
Substantia Nigra
The substantia nigra is semilunar in transverse section, concave dorsally and thicker medially, where it is traversed by oculomotor axons as they stream ventrally to their point of exit in the interpeduncular fossa. Extensions from its convex ventral surface pass between fibres of the crus cerebri. The substantia nigra is subdivided into a dorsal pars compacta and a ventral pars reticulata (reticularis), and the cells of these two parts have different connections. The pars compacta consists of many darkly pigmented neurones that contain neuromelanin granules. Their arrangement is irregular, and they partially penetrate the subjacent pars reticulata. The pigmentation is easily visible in transverse or coronal sections and is related to the aminergic status of the neurones (see Figs 10.24, 10.25). Pigmentation increases with age; it is most abundant in primates, maximal in humans, and is present even in albinos. The pigmented pars compacta neurones synthesize dopamine as their neurotransmitter and project to the corpus striatum of the basal ganglia and other sites.
The pars compacta of the substantia nigra corresponds to the dopaminergic cell group A9 (see Fig. 14.10). Two other dopaminergic cell groups are found in the ventral tegmentum: cell group A10 in the rostromedial region, which constitutes the ventral tegmental area (of Tsai), and cell group A8 in the dorsolateral reticular area, which forms the nucleus parabrachialis pigmentosus. The whole ventral tegmental system of dopaminergic neurones appears to act as an integrative centre for adaptive behaviour. It projects via a number of pathways, mainly through ipsilateral fibres in the medial forebrain bundle. These pathways are a mesodiencephalic system, which terminates in thalamic and hypothalamic nuclei; a mesostriatal projection; a mesolimbic (mesorhombic) pathway to the nucleus accumbens, olfactory tubercle, lateral septum, interstitial nucleus of the stria terminalis, amygdala and entorhinal cortex; and mesocortical fibres to most cortical areas, particularly the prefrontal, orbitofrontal and cingulate cortex.
The pars compacta projects heavily to the caudate nucleus and putamen in a topographically organized fashion (nigrostriatal fibres). Lesser projections end in the globus pallidus and subthalamic nucleus. In Parkinson’s disease, the levels of dopamine in the substantia nigra and striatum decrease dramatically as a result of the degeneration of pars compacta neurones (see Ch. 14, Case 5).
Red Nucleus
The red nucleus is an ovoid mass approximately 5 mm in diameter, with a pink tinge, dorsomedial to the substantia nigra (see Fig. 10.25). The tint appears only in fresh material and is caused by a ferric iron pigment in its multipolar neurones. The latter are of varying size. Their proportions and arrangements vary among species; for example, in primates, the magnocellular element is decreased, and there is a reciprocal increase in the size of the parvocellular component. Small multipolar neurones occur in all parts of the nucleus. In humans, the larger neurones are restricted to the caudal part of the nucleus and have been estimated to be as few as 200 in number. The magnocellular element is considered phylogenetically old, which accords with the parvocellular predominance in primates. Rostrally, the red nucleus is poorly demarcated, and it blends into the reticular formation and caudal pole of the interstitial nucleus. It is traversed and surrounded by fascicles of nerve fibres, including many from the oculomotor nucleus.
Principal afferent connections of the red nucleus travel via corticorubral and cerebellorubral fibres. Uncrossed corticorubral fibres originate from primary somatomotor and somatosensory areas. In animals, the red nucleus receives fibres from the contralateral nucleus interpositus (which corresponds to the human globose and emboliform nuclei) and dentate nucleus, via the superior cerebellar peduncle. It has bilateral, probably reciprocal connections with the superior colliculi. In humans, the rubrospinal tract is small and originates from the caudal magnocellular part of the red nucleus. Few fibres reach the cervical cord. The fibres decussate and then run obliquely laterally in the ventral tegmental decussation, ventral to the tectospinal decussation and dorsal to the medial lemniscus. On reaching the grey matter ventral to the inferior cerebellar peduncle, the tract turns caudally to enter the lateral part of the lateral lemniscus. It continues descending ventral to the tract and nucleus of the trigeminal nerve throughout the medulla and enters the upper part of the cervical cord, intermingled with fibres of the lateral corticospinal tract (Ch. 8). Some efferent axons form a rubrobulbar tract to motor nuclei of the trigeminal, facial, oculomotor, trochlear and abducens nerves.
The largest group of efferents from the red nucleus in humans is found in the massive uncrossed central tegmental tract (fasciculus), which lies in the ventral part of the midbrain. Initially it lies lateral to the medial longitudinal fasciculus and dorsolateral to both the red nucleus and the decussation of the superior cerebellar peduncles (see Figs 10.12–10.14, 10.24). Most fibres arise from the parvocellular part of the red nucleus and join the tract as it traverses the nucleus on its way to the ipsilateral inferior olivary nucleus in the medulla. Some tract fibres terminate in the brain stem reticular nuclei. Ascending and descending axons from the brain stem reticular formation run in the central tegmental tract. Their collaterals and terminals innervate other ‘reticular’ or adjacent ‘specific’ nuclei. These axons include dorsal and ventral ascending noradrenergic bundles, a ventral ascending serotoninergic bundle and some fibres of dorsal and ventral ascending cholinergic bundles.
Lesions of the corticospinal system in humans result in permanent paresis. In monkeys, although the paralysis is initially complete, it eventually disappears, and a good recovery ensues. The explanation for this interprimate variability in recovery from corticospinal lesions could lie in the differential capacity of the rubrospinal system to compensate for the loss of corticospinal drive. Monkeys never fully recover from combined lesions of both the corticospinal and rubrospinal tracts, which suggests that the two systems are functionally interrelated in the control of movement. Both encode force, velocity and direction parameters, but the rubrospinal system primarily directs activity both during the terminal phase of a movement and preceding a movement. There is thus overlap of activity in the two systems for all parameters during the movements of limbs and even of individual digits. The corticospinal system is most active during the learning of new movements, whereas the rubrospinal system is most active during the execution of learned automated movements.
Trochlear Nucleus
The trochlear nucleus lies in the grey matter in the floor of the cerebral aqueduct, level with the upper part of the inferior colliculus (see Figs 10.1, 10.24). It is in line with the ventromedial part of the oculomotor nucleus, in the position of the somatic efferent column. The medial longitudinal fasciculus is ventral and lateral to it. The oculomotor and trochlear nuclei often overlap slightly but can be distinguished by the smaller size of the trochlear neurones.
Medial Longitudinal Fasciculus
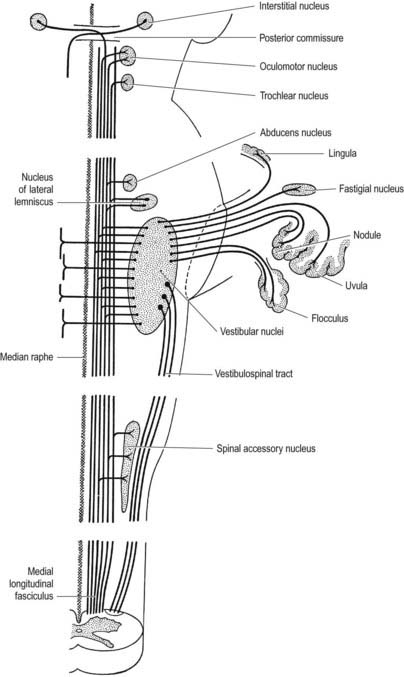
The medial longitudinal fasciculus (see Fig. 10.26) is a heavily myelinated composite tract lying near the midline, ventral to the periaqueductal grey matter. It ascends to the interstitial nucleus (of Cajal), which lies in the lateral wall of the third ventricle, just above the cerebral aqueduct. The fasciculus retains its position relative to the central grey matter through the midbrain, pons and upper medulla, but it is displaced ventrally by successive decussations of the medial lemnisci and lateral corticospinal tracts. At spinal levels, it is synonymous with the medial vestibulospinal tract.
The medial longitudinal fasciculus interconnects the oculomotor, trochlear, abducens, Edinger–Westphal, vestibular, reticular and spinal accessory nuclei, coordinating conjugate eye movements and associated movements of the head and neck. Lesions cause internuclear ophthalmoplegia. All four vestibular nuclei contribute ascending fibres. Those from the superior nucleus remain uncrossed, while the others are partly crossed. Some fibres reach the interstitial and posterior commissural nuclei, and some decussate to the contralateral nuclei. Descending axons, from the medial vestibular nuclei and perhaps the lateral and inferior nuclei, partially decussate and descend in the fasciculus as the medial vestibulospinal tract (see Fig. 8.42). Fibres join from the dorsal trapezoid, lateral lemniscal and posterior commissural nuclei, which means that both the cochlear and vestibular components of the vestibulocochlear nerve may influence movements of the eyes and head via the medial longitudinal fasciculus. Some vestibular fibres may ascend in the medial longitudinal fasciculus as far as the thalamus (see Ch. 12, Case 6).
Tectum
Inferior Colliculus
The inferior colliculus (see Fig. 10.24) has a central, ovoid main nucleus that is continuous with the periaqueductal grey matter. It is surrounded by a lamina of nerve fibres, many from the lateral lemniscus, which terminate in it. The central nucleus has dorsomedial and ventrolateral zones, which are covered by a dorsal cortex. In humans, the cortex has four cytoarchitectonic layers: layer I contains small neurones with flattened radial dendritic fields; layer II, medium-sized neurones with ovoid dendritic fields aligned parallel with the collicular surface; layer III, medium-sized neurones with spherical dendritic fields; and layer IV, large neurones with variably shaped dendritic fields. The central nucleus is laminated. Bands of cells with disc-shaped or stellate dendritic fields orthogonally span the fibre layers in which the terminals of lateral lemniscal fibres ramify. The neurones are sharply tuned to frequency, and the laminae may represent the structural basis of tonal discrimination. Experimental studies have found cells driven by low frequencies in the dorsal laminae, and others driven by high frequencies in the ventral laminae. Neurones are broadly frequency tuned in the dorsal cortex and lateral nucleus.
Brain Stem Reticular Formation
Studies with the Golgi technique show that few brain stem reticular neurones are classic Golgi type II neurones (i.e. with short axons that branch locally). In contrast, they have long dendrites that spread across the long axis of the brain stem in transverse sheets. These radiating dendrites may spread into 50% of the cross-sectional area of their half of the brain stem, and they are intersected by, and may synapse with, a complex of ascending and descending fibres. Many axons of the reticular neurones ascend or descend, or bifurcate to do both. They travel far, perhaps through the whole brain stem and often beyond. As an example, a bifurcating axon from a cell in the magnocellular medullary nucleus may project rostrally into the upper medulla, pons, midbrain tegmentum, subthalamus, hypothalamus, dorsal thalamus, septum, limbic system and neocortex, while its descending branch innervates the reticular core of the lower medulla and may reach the cervical spinal intermediate grey matter (laminae V and VI). Many reticular neurones have unidirectional, shorter axons that synapse with the radiating dendrites of innumerable other neurones en route and give off collaterals, which synapse with cells in ‘specific’ brain stem nuclei or cortical formations, such as the cerebellum. Multitudes of afferent fibres converging on individual neurones and their myriad synapses and destinations provide the structural basis for the polymodal responses elicited by experiments, and also for such terms as ‘diffuse, non-specific polysynaptic systems.’
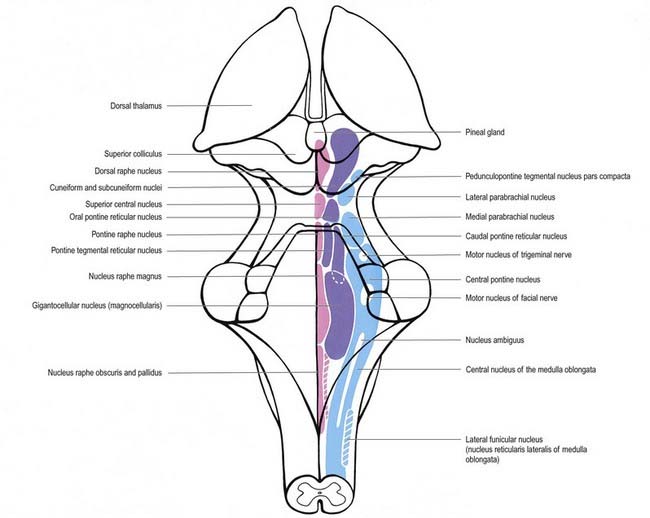
In general terms, the reticular formation is a continuous core that traverses the whole brain stem and is continuous below with the reticular intermediate spinal grey laminae. It is divisible, on the basis of cytoarchitectonic, chemoarchitectonic and functional criteria, into three bilateral longitudinal columns: median; medial, containing mostly large reticular neurones; and lateral, containing mostly small to intermediate neurones (Fig. 10.27).
Median Column of Reticular Nuclei
The median column of reticular nuclei extends throughout the medulla, pons and midbrain and contains neurones that are largely aggregated in bilateral, vertical sheets, blended in the midline and occupying the paramedian zones. Collectively, they are called the nuclei of the raphe, or raphe nuclei (see Fig. 10.27). Many neurones in raphe nuclei are serotoninergic and are grouped into nine clusters, B1 to B9. The raphe pallidus nucleus and associated raphe obscurus nucleus lie in the upper two-thirds of the medulla and cross the pontomedullary junction. The raphe magnus nucleus, corresponding to many B3 neurones, partly overlaps them and ascends into the pons. Above it is the pontine raphe nucleus, which is formed by the cell group B5. Also located in the pons is the central superior raphe nucleus, which contains parts of cell groups B6 and B8. The dorsal (rostral) raphe nucleus, approximating cell group B7, ascends—expanding, then narrowing—through much of the midbrain.
Principally, the mesencephalic serotoninergic raphe system is reciprocally interconnected rostrally with the limbic system, septum, prefrontal cortex and hypothalamus. Efferents ascend and form a large ventral pathway and a diminutive dorsal pathway. Both originate from neurones in the dorsal and central superior raphe nuclei. The raphe magnus nucleus also contributes to the dorsal ascending serotoninergic pathway, which is at first incorporated into the dorsal longitudinal fasciculus (of Schütz). A few fibres terminate in the central mesencephalic grey matter and posterior hypothalamus, but most continue into the medial forebrain bundle and merge with the axons of the ventral pathway, which are distributed to the same targets. The fibres of the ventral ascending serotoninergic pathway exit the ventral aspect of the mesencephalic raphe nuclei and then course rostrally through the ventral tegmentum, where fibres pass to the ventral tegmental area, substantia nigra and interpeduncular nucleus. A large number of fibres then enter the habenulo-interpeduncular tract and run rostrally to innervate the habenular nucleus; intralaminar, midline, anterior, ventral and lateral dorsal thalamic nuclei; and lateral geniculate body. The ventral ascending serotoninergic pathway enters the median forebrain bundle in the lateral hypothalamic area and splits to pass medially and laterally. The fibres in the medial tract terminate in the mammillary body; dorsomedial, ventromedial, infundibular, anterior and lateral hypothalamic nuclei; medial and lateral preoptic nuclei; and suprachiasmatic nuclei. Those in the lateral tract take the ansa peduncularis–ventral amygdalofugal path to the amygdala, striatum and caudal neocortex. The medial forebrain bundle carries the remaining ventral ascending serotoninergic axons into the medullary stria, stria terminalis, fornix, diagonal band, external capsule, cingulate fasciculus and medial olfactory stria, to terminate in all the structures that these systems interconnect.
Medial Column of Reticular Nuclei
The medial column of reticular nuclei is composed predominantly of neurones of medium size, although very large neurones are found in some regions, and most have processes oriented in the transverse plane (see Fig. 10.27). In the lower medulla, the column is indistinct and is perhaps represented by a thin lamina lateral to the raphe nuclei. However, in the upper medulla, it expands into the medullary gigantocellular (magnocellular) nucleus, which lies ventrolateral to the hypoglossal nucleus, ventral to the vagal nuclei and dorsal to the inferior olivary complex. Ascending farther, the column continues as the pontine gigantocellular (magnocellular) nucleus, which lies medially in the tegmentum. Its neurones suddenly diminish in size to form, in rostral order, the almost coextensive caudal and oral pontine tegmental reticular nuclei. It then expands into the cuneiform nucleus and subcuneiform nucleus before fading away in the midbrain tegmentum.
Afferent components to the medial reticular nuclear column include the spinoreticular projection and collaterals of centrally projecting spinal trigeminal, vestibular and cochlear fibres. Spinoreticular fibres arise from neurones in the intermediate grey matter of the spinal cord. They decussate in the ventral white commissure; ascend in the ventrolateral funiculus, usually via several neurones; and terminate not only at all levels of the medial column of reticular nuclei but also in the intralaminar nuclei of the thalamus. Three areas of the medial reticular zone receive particularly high densities of terminations: the combined caudal and rostral ends of the gigantocellular and central nuclei, respectively; the caudal pontine reticular nucleus; and the pontine tegmentum. Retinotectal and tectoreticular fibres relay visual information, and the medial forebrain bundle transmits olfactory impulses.
Lateral Column of Reticular Nuclei
The functions of the locus coeruleus and related tegmental noradrenergic cell groups are poorly understood, largely because the afferent neurones that drive them have yet to be identified. The diversity of their rostral and caudal projections suggests a holistic role in central processing. In animals, firing rates of locus coeruleus neurones peak during wakefulness and decrease during sleep—they cease almost completely during rapid eye movement (REM) sleep. During wakefulness, firing rates are augmented when novel stimuli are presented. The locus coeruleus may therefore function to control the level of attentiveness. Other functions that have been ascribed to the locus coeruleus include control of the wake–sleep cycle, regulation of blood flow and maintenance of synaptic plasticity.
Brain Stem Lesions
Unilateral brain stem lesions may arise as a result of extrinsic compression of the brain stem by space-occupying tumours (e.g. meningioma, acoustic neuroma, metastatic carcinoma) or may be caused by intrinsic disease (e.g. glioma, demyelination, stroke) (Figs 10.28, 10.29). The clinical syndrome is determined by the neuroanatomical site of the lesion. At the segmental level, an ipsilateral cranial nerve palsy occurs. Below the level of the lesion, there is a contralateral loss of power and sensation in the limbs (corresponding to dysfunction of the decussating corticospinal and ascending sensory pathways) and ipsilateral incoordination of the limbs (as a result of the interruption of efferent and afferent cerebellar connections).
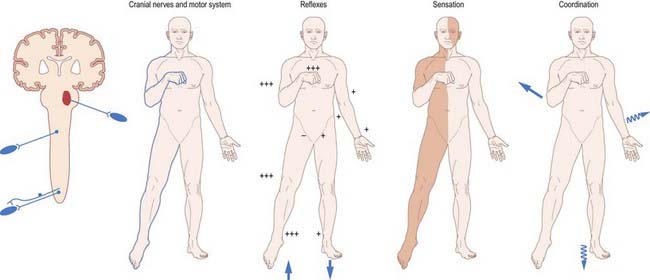
Fig. 10.28 Brain stem lesions.
(By permission from Crossman, A.R., Neary, D., 2000. Neuroanatomy, 2nd ed. Churchill Livingstone, Edinburgh.)
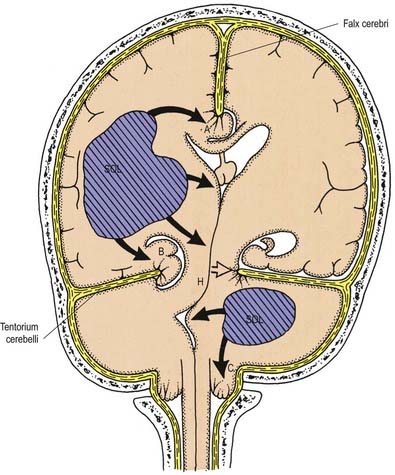
Bilateral destructive lesions of the brain stem are fatal if untreated because of damage to centres in the medulla that control respiration, heart rate and blood pressure. Impairment of the reticular activating system in the core of the brain stem leads to progressive impairment of consciousness, followed by stupor and coma. In this state of ‘brain stem death,’ life can only be supported artificially. This is the fate of all untreated expanding space-occupying lesions in the cranium (e.g. haematoma, abscess or tumour, whether extrinsic or intrinsic to the brain; cerebral oedema). A space-occupying lesion within the unyielding skull raises the intracranial pressure directly as well as indirectly by obstruction of cerebrospinal fluid flow, which causes headache and papilloedema. The brain is distorted and displaced downward (rostrocaudally) within the skull and meningeal framework. The brain stem is vulnerable to compression at two critical sites, which are determined by the neuroanatomical relationship of the meningeal tentorium and foramen magnum to the cerebral hemisphere (supratentorial) and brain stem (infratentorial). Downward displacement of the cerebral hemisphere leads to herniation of the ipsilateral medial temporal lobe (uncus) through the tentorial notch. There may be direct ipsilateral compression of the midbrain and emergent oculomotor and trochlear cranial nerves or contralateral compression of the upper brain stem by the abutting sharp edge of the tentorium. The ipsilateral posterior cerebral artery is vulnerable to compression at this site. Unilateral herniation is heralded by a progressive oculomotor nerve palsy (ophthalmoplegia, pupillary dilatation and ptosis), contralateral limb weakness, falling level of consciousness and, if treatment is long delayed, contralateral homonymous hemianopia. Compression of the contralateral brain stem by the tentorium leads to ipsilateral ‘false localizing’ signs (Kernohan’s syndrome).
Adams R.D., Victor M., Mancall E.L. Central pontine myelinolysis. A hitherto undescribed disease occurring in alcoholic and malnourished patients. Arch. Neurol. Psychiatry. 1959;81:154.
Brodal P., Bjaalie J.G. Organization of the pontine nuclei. Neurosci. Res.. 1992;13:83-118.
Ciriello J. Brainstem projections of aortic baroreceptor afferent fibres in the rat. Neurosci. Lett.. 1983;36:37-42.
Dahlström A., Fuxe K. Evidence for the existence of monamine-containing neurones in the central nervous system. Acta. Physiol. Scand. Suppl.. 1964;232:1-55.
Dahlström A., Fuxe K. Evidence for the existence of monoamine neurones in the central nervous system. II. Experimentally induced changes in the intraneuronal amine levels of bulbospinal neurone systems. Acta. Physiol. Scand. Suppl.. 1965;247:1-36.
Hamilton R.B., Norgren R. Central projections of gustatory nerves in the rat. J. Comp. Neurol.. 1984;222:560-577.
Johnston J.B. The morphology of the forebrain vesicle in vertebrates. J. Comp. Neurol.. 1909;19:458-539.
Kleinschmidt-DeMasters B.K., Rojiani A.M., Filley C.M. Central and extrapontine myelinolysis: then and now. J. Neuropathol. Exp. Neurol.. 2006;65:1-11.
Leigh R.J. Zee DS the Neurology of Eye Movements, second ed. Philadelphia: FA Davis; 1991. p. 462
Millar J., Basbaum A.I. Topography of the projection of the body surface of the cat to cuneate and gracile nuclei. Exp. Neurol.. 1975;49:281-290.
Nathan P.W., Smith M.C. The rubrospinal and central tegmental tracts in man. Brain. 1982;105:223-269.
Nieuwenhuys R., Voogd J., van Huijzen C. The human central nervous system. A synopsis and atlas, third ed. Berlin: Springer Verlag; 1988.
Olszewski J. On the anatomical and functional organization of the spinal trigeminal nucleus. J. Comp. Neurol.. 1950;92:401-409.
Schmeichel A.M., Buchhalter L.C., Low P.A., et al. Mesopontine cholingeric neuron involvement in Lewy body dementia and multiple system atrophy. Neurology. 2008;70:368-373.
Wolf J.K. The classical brain stem syndromes. Springfield: Charles C. Thomas; 1971.