Chapter 35. Assessment of the paediatric patient
The aim of the prehospital assessment is management of the child’s condition rather than specific diagnosis.
The age of a child is usually known but the weight must sometimes be approximated by the formula:
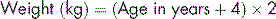
This works well between the ages of 1 year and 10 years.
The average birthweight of a full-term infant is 3.5 kg; this has usually doubled by 5 months of age and tripled by 12 months.
| Age | Weight (kg) |
|---|---|
| 2 months | 5 |
| 6 months | 7.5 |
| 1 year | 10 |
| 3.5 years | 15 |
| 6 years | 20 |
| 10 years | 30 |
| 13 years | 40 |
| 14 years | 50 |
Immediate assessment
The SAFE approach should be used. Children are usually easy to move to a safer place.
Airway
Check for responsiveness. Failure to respond indicates a significantly lowered level of consciousness and therefore an airway at risk. There may be a need for airway opening manoeuvres and action to protect the airway.
Partial upper airway obstruction is suggested by snoring, rattling or gurgling.
Stridor is heard best in inspiration – this differentiates it from wheezing, which is usually loudest in expiration. Stridor suggests obstruction at the level of the larynx and upper trachea and can be caused by a foreign body or by infection (usually associated with fever).
Do not examine the throat with any instrument in children with stridor or suspected partial airway obstruction – doing so may convert the problem to complete obstruction
Drooling, the inability to swallow saliva, suggests blockage at the back of the throat.
Cyanosis and reduced haemoglobin saturation readings on a pulse oximeter are very late signs of airway obstruction
All children will benefit from high-concentration oxygen therapy. Only a small group of infants with congenital heart disease need controlled oxygen therapy.
It is not worth struggling to make an unwilling child wear an oxygen mask
If a child’s airway can be maintained by simple manoeuvres, an oropharyngeal (Guedel) airway is best avoided. This is because retching is easily induced in children and may be followed by laryngospasm or aspiration.
• Oropharyngeal airway size = the distance from the centre of the lips to the angle of the jaw
• Nasopharyngeal airway size = the distance from the tip of the nose to the tragus of the ear Endotracheal tube size:
• 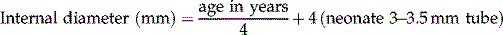
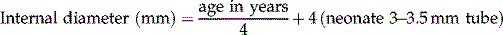
• 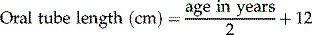
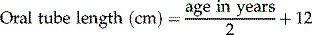
Assess the need for cervical spine protection before any airway intervention
Breathing
Look, listen and feel for breathing. The absence of breath sounds indicates the need to follow procedures for cardiorespiratory arrest.
Look for:
• Difficulty in talking – a child who is unable to speak because of laboured breathing is very unwell
• An abnormal respiratory rate – usually fast, laboured breathing. Very slow respiratory rates may occur just before respiratory arrest or in children poisoned with narcotic drugs
• Recession of the chest wall – the indrawing of the elastic tissues of a child caused by increased respiratory effort
• Wheezing and rattling, grunting and panting
• Nasal flaring and use of the shoulder and neck muscles during breathing
• Unequal or diminished breath sounds.
| Age (years) | Respiratory rate (breaths/min) | Pulse rate (bpm) |
|---|---|---|
| Under 1 | 30–40 | 110–160 |
| 1–5 | 25–30 | 95–140 |
| 6–12 | 20–25 | 80–120 |
Absence of breath sounds means that the movement of air in the lungs is so diminished that it cannot be heard
All the above suggest that the child is struggling to achieve normal respiration. Failure to adequately oxygenate the blood and hence the tissues, is shown by:
• Tachycardia – the hypoxic nervous system is stimulating the heart
• Cyanosis – a late sign
• Irritability, confusion or reduced responsiveness mean that the brain is short of oxygen – this is an extremely worrying sign.
The oxygen saturation shown by the pulse oximeter should be close to 100% in a normal, healthy child
All wheezy children will benefit from nebulised bronchodilators, whether they are known to be asthmatic or not. Agitation, tachycardia and tremor may be signs of salbutamol overdosage. Ventilation is indicated as an emergency procedure for respiratory insufficiency in a child in the same way as in an adult, suggested ventilator settings for children are:
• Tidal volume 10 mL/kg
• Minute volume 100 mL/kg.
Circulation
Check for a central pulse (over 10 seconds). The brachial or femoral pulses should be used in infants rather than the carotid pulse. The absence of a central pulse (or a rate of less than 60 bpm in infants) indicates the need to follow procedures for cardiorespiratory arrest.
In a child with ventricular fibrillation and no obvious precipitating factors, the cause could be poisoning with tricyclic antidepressants
A fast or slow heart rate
The worst cause of bradycardia is severe hypoxia (or hypovolaemia) and, in this case, cardiac arrest is imminent. Occasionally, bradycardia is seen with poisoning and severe head injury.
Abnormal systolic blood pressure
This varies with age.
Estimation of normal blood pressure:
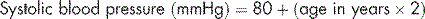
Blood pressure can be difficult to measure in young, restless children and requires a cuff of the correct size. It will not fall until very late in shock.
A raised capillary refill time
It should be less than 2 seconds if the circulation is satisfactory. May be prolonged in a cold patient.
Pallor and coolness of the skin
The body diverts blood away from the skin when there are circulatory problems.
Active bleeding
A child’s blood volume is approximately 80 mL/kg
Inadequate circulation will reduce tissue oxygenation and thus may also cause a raised respiratory rate or altered level of consciousness. The ECG is rarely as helpful in making a diagnosis in children as it is in adults, except for arrhythmias. A cardiac monitor does, however, provide constant information about the heart rate.
The need for venous access and the site should be assessed carefully. Use IO access if necessary.
Give the minimum IV fluids required to achieve improvement, start with small boluses of fluid up to a maximum of 3 × 20 mL/kg in all patients.
Bolus fluid therapy
Excessive fluid therapy runs the risk of causing heart failure and may be counter-productive.
Dehydration is shown by a dry, non-elastic skin or sunken eyes. In infants, a floppy anterior fontanelle is a useful, if late, sign of severe fluid loss. Diarrhoea and vomiting can quickly dehydrate a small child. Wet nappies confirm urine output in young children.
Disability
The AVPU scoring system is as useful for children as for adults:
A – Alert
V – Voice elicits a response
P – Pain elicits a response
U – Unresponsive.
Consider hypoglycaemia as a cause for a reduced level of consciousness
Signs of an intracerebral problem
• Reduced level of consciousness – even sleepy children should be rousable
• Abnormal pupils – dilated, fixed or uneven pupils
• Abnormal posture and limbs movement – never assume an abnormality is congenital
• Airway obstruction
• Respiratory depression
• Bradycardia and hypertension.
Exposure and environment
Look for:
• Cold extremities
• Shivering
• Wet clothing
• Pyrexia and clamminess
• The position in which the child is most comfortable
• The proximity of the mother or other carer.
Because of their large surface area relative to their small body volume children will lose heat much faster than adults. Attention to these details early on can radically change the wellbeing (and demeanour) of a child. A child may well need clothing removed to facilitate assessment. However, children easily become cold and embarrassed.
Fits
Look for:
1. Frank tonic or clonic activity
2. Spasmodic twitching
3. Postictal drowsiness
4. Gurgling, rattling or other signs of airway obstruction
5. Cyanosis – during a fit there is a very high demand for oxygen, coupled with respiratory inadequacy
6. Signs of head injury
7. Signs of other injury caused by a convulsion (e.g. a bitten tongue and intraoral bleeding)
8. Reasons to consider hypoglycaemia.
It is very difficult to assess or manage a fitting child. Hence termination of the convulsion must be an immediate aim.
Glucose
Children use their glucose reserves very quickly. Glucagon will therefore be less consistently effective than in adults.
Look for:
• Restlessness, agitation or other mental change (‘jitteriness’ in a neonate)
• A reduced level of consciousness
• Signs of insulin usage (all diabetic children will be on insulin; oral hypoglycaemic drugs are generally only used in adults. This does not mean, of course, that a child cannot take someone else’s drugs and become hypoglycaemic)
• A low blood glucose level on testing with a reagent strip
• Convulsions – can be caused by hypoglycaemia.
Glucose: 5 mL/kg of 10% dextrose solution
Immediate needs of the child
The relief of suffering is of paramount importance. Assess:
1. The need for analgesia
2. The need for limb splintage
3. The tolerance of cervical and spinal splintage.
The needs of the parents
Parent and carers will need reassurance and sometimes need medical treatment themselves. Parental anxiety should not be dismissed as it may be the only sign of serious illness in a child.
Poisoning
Bizarre symptoms and signs and unexplained combinations of findings suggest poisoning. Younger children may ingest substances accidentally; older children may experiment with drugs. Look for the most common signs:
• Confusion, agitation and drowsiness
• Tachycardia
• Dilated pupils
• Evidence at the scene (which is of enormous help to hospital staff).
Other important findings
• Raised temperature – a hand on the abdomen may reveal an obvious pyrexia. This often accompanies a fit. Febrile convulsions are common between 5 months and 5 years of age. Children with epilepsy are more likely to have a fit during a pyrexia
• Neck stiffness indicates inflammation of the meninges, i.e. meningitis. This is often accompanied by pyrexia, headache and drowsiness; however, the diagnosis can be difficult
• Rashes usually indicate systemic infection, allergy or specific skin disease. Purpura is the most worrying skin sign (suggesting possible meningococcal septicaemia or other cause of vasculitis)
• Drawing up of the knees suggests pain in the abdomen
• Signs of congenital abnormality – children with congenital problems are often prone to fits and chest infections
• The relationship and interaction with the parents and the other family members is always important.
Signs of child abuse
Signs suggestive of non-accidental injury
• Unexplained head, facial, chest or limb injuries – especially in children who are not able to walk and thus fall (few children walk before the age of 11 months)
• Multiple bruising
• Injuries of different ages
• Unusual burns (e.g. those of a ‘glove’ or ‘stocking’ distribution)
• Unusual cuts and bruises – imprints of hands, sticks, cords, shoes, belts and teeth may be present.
For further information, see Ch. 35 in Emergency Care: A Textbook for Paramedics.