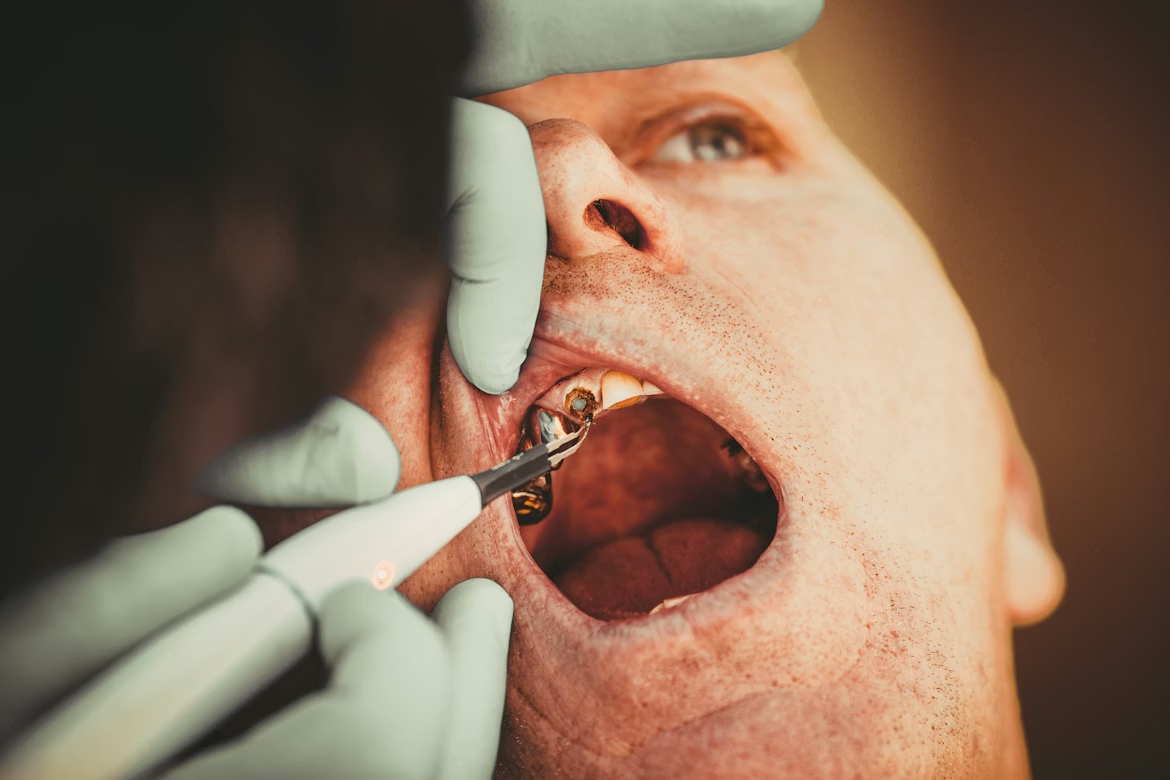
According to the American Dental Association’s 2023 surveillance data, nearly half of all adults over 30 show signs of gum disease, yet most don’t recognize the early symptoms until significant damage has already occurred. In New York City’s fast-paced environment, where stress levels run high and quick meals often replace balanced nutrition, these statistics take on particular urgency. The combination of demanding schedules, environmental factors, and lifestyle pressures creates a perfect storm for periodontal problems that can progress silently for months.
What makes this especially concerning is how gum disease symptoms often masquerade as minor inconveniences — a little bleeding during brushing, occasional bad breath, or gums that feel slightly tender. Most people dismiss these as temporary issues rather than warning signs of a condition that, left untreated, can lead to tooth loss and serious systemic health complications. The gap between symptom onset and professional intervention often determines whether someone needs simple maintenance or extensive restoration.
Understanding what to watch for and when to seek specialized care isn’t just about preserving your smile — it’s about protecting your overall health and avoiding the complex, costly treatments that become necessary when gum disease advances unchecked.
How to Recognize Early and Common Gum Disease Symptoms
The first signs of gum disease often appear so gradually that they blend into daily life, making them easy to overlook until they become impossible to ignore. Bleeding gums during brushing or flossing represents one of the earliest and most reliable indicators, yet many people assume this is normal or caused by brushing too vigorously. Healthy gums don’t bleed with gentle, proper oral hygiene — when they do, it signals inflammation and bacterial infection taking hold.
Persistent bad breath that doesn’t improve with brushing, mouthwash, or breath mints often indicates bacterial overgrowth below the gum line. This halitosis has a distinctly different quality from morning breath or food-related odors — it tends to return quickly after oral hygiene efforts and may carry a metallic or sour undertone. Consider someone who maintains good oral hygiene but notices colleagues stepping back during conversations, or family members commenting on breath odor despite recent brushing.
Swollen, red, or tender gums mark another clear progression from healthy pink tissue to inflamed, puffy areas that may feel sensitive to touch or temperature changes. You might notice your gums appear darker red than usual, particularly around the base of teeth, or feel unusually soft when you run your tongue along them. This inflammation often starts between teeth where cleaning is most challenging.
Gum recession becomes visible as teeth appear longer than before, or you notice increased sensitivity when consuming hot or cold foods and drinks. The gum line gradually pulls away from teeth, exposing root surfaces that were previously protected. Many people first notice this when they realize their smile looks different in photos, or when dental floss reaches deeper between teeth than it used to.
Loose teeth or changes in bite alignment represent more advanced symptoms that require immediate attention. You might notice teeth feeling slightly mobile when you press on them with your tongue, or experience subtle changes in how your upper and lower teeth fit together when chewing. Even minor shifts in tooth position can indicate that the supporting structures around teeth are compromised.
These symptoms rarely appear in isolation — they tend to develop in patterns that reflect the progressive nature of gum disease, making early recognition crucial for preventing more serious complications.
What Makes Gingivitis Different From Periodontitis
Early Signs of Gingivitis Everyone Should Know
Gingivitis represents the mildest and most reversible form of gum disease, characterized by inflammation that affects only the soft tissue around teeth without damaging the underlying bone or connective structures. The hallmark symptoms include mild bleeding during brushing, slight gum swelling, and tissue that appears redder than the normal pink color. What distinguishes gingivitis from more serious forms is that the inflammation remains superficial — your teeth stay firmly anchored, there’s no recession of the gum line, and no permanent damage occurs to the structures holding teeth in place.
Most people with gingivitis experience symptoms that come and go, particularly during times of stress, illness, or when oral hygiene routines become inconsistent. The bleeding might appear for a few days, then disappear, leading many to assume the problem resolved itself. However, this cyclical nature actually indicates that bacterial levels fluctuate but never fully clear, setting the stage for progression if underlying causes aren’t addressed.
The encouraging aspect of gingivitis is its complete reversibility with proper intervention. Unlike more advanced stages, gingivitis responds well to improved home care and professional cleaning, often showing dramatic improvement within two to three weeks of consistent treatment.
How Periodontitis Develops and Its Advanced Symptoms
Periodontitis occurs when gingivitis progresses beyond surface inflammation to affect the deeper structures supporting teeth, including the periodontal ligament and alveolar bone. This transition marks a critical threshold — while gingivitis can be completely reversed, periodontitis causes permanent damage that can only be managed, not cured. The symptoms become more pronounced and persistent, including deep pockets forming between teeth and gums, significant gum recession exposing root surfaces, and gradual loosening of teeth.
Advanced periodontitis presents with symptoms that dramatically impact daily life: teeth shifting position, changes in bite that affect chewing, and spaces developing between teeth that weren’t there before. The bacterial infection creates deeper pockets around teeth, sometimes reaching 6-8 millimeters compared to the healthy 1-3 millimeter depth. These pockets harbor bacteria that regular brushing and flossing cannot reach, creating a cycle of ongoing infection and tissue destruction.
The progression from gingivitis to periodontitis isn’t inevitable, but certain factors — particularly smoking, diabetes, stress, and genetic predisposition — can accelerate the transition. Once periodontal damage occurs, the goal shifts from reversal to prevention of further loss, requiring ongoing periodontal care in NYC to maintain stability and prevent tooth loss.
Risk Factors and Causes Affecting Gum Health in NYC Adults
How Lifestyle and Health Conditions Increase Gum Disease Risk
New York City’s unique lifestyle patterns create a convergence of risk factors that can accelerate gum disease development in otherwise healthy adults. Smoking and tobacco use remain the most significant controllable risk factors, with tobacco users showing three to six times higher rates of periodontal disease compared to non-users. The chemicals in tobacco products restrict blood flow to gum tissue, impair immune response, and create an environment where harmful bacteria thrive while beneficial healing processes struggle.
Stress levels common in NYC’s competitive work environment directly impact gum health through multiple pathways. Chronic stress elevates cortisol levels, which suppresses immune function and makes it harder for the body to fight off bacterial infections in the mouth. Additionally, stress often leads to behaviors that compound the problem — grinding or clenching teeth, neglecting oral hygiene routines, and increased consumption of caffeine, alcohol, or comfort foods that feed harmful bacteria.
Diabetes presents a bidirectional relationship with gum disease that’s particularly relevant for NYC’s diverse adult population. Uncontrolled blood sugar levels make it harder to fight infections anywhere in the body, including the gums, while severe gum disease can make blood sugar more difficult to control. People with diabetes who develop periodontal disease often find their glycemic management becomes more challenging, creating a cycle that affects both conditions.
Genetic predisposition accounts for approximately 30% of gum disease susceptibility, meaning some individuals remain vulnerable despite excellent oral hygiene while others maintain healthy gums with minimal care. Family history of tooth loss, particularly in parents or siblings who lost teeth due to gum problems rather than cavities, suggests inherited risk factors that require more aggressive prevention strategies.
The Role of Diet and Environment in Gum Disease Development
The typical NYC adult diet — characterized by frequent coffee consumption, quick meals, and limited time for proper oral hygiene between meals — creates conditions that promote harmful bacterial growth. Frequent snacking, particularly on processed foods high in simple carbohydrates, provides constant fuel for bacteria that produce acids and toxins harmful to gum tissue. Coffee consumption throughout the day creates an acidic oral environment while often leading to reduced saliva production, which normally helps neutralize acids and wash away food particles.
Environmental factors unique to urban living also contribute to gum disease risk. Air pollution and environmental toxins can increase systemic inflammation, making the body less effective at fighting localized infections like gum disease. The stress of commuting, noise pollution, and reduced exposure to natural environments all contribute to chronic stress responses that impact immune function.
Nutritional deficiencies common in busy lifestyles — particularly inadequate intake of vitamin C, vitamin D, and omega-3 fatty acids — can compromise the body’s ability to maintain healthy gum tissue and respond effectively to bacterial challenges. Many NYC adults rely heavily on convenience foods that provide calories but lack the micronutrients necessary for optimal immune function and tissue healing.
The combination of these dietary and environmental factors creates a cumulative effect that can overwhelm the body’s natural defense mechanisms, making even people with good oral hygiene habits more susceptible to gum disease development and progression.
How Gum Disease Symptoms Connect to Systemic Health Risks
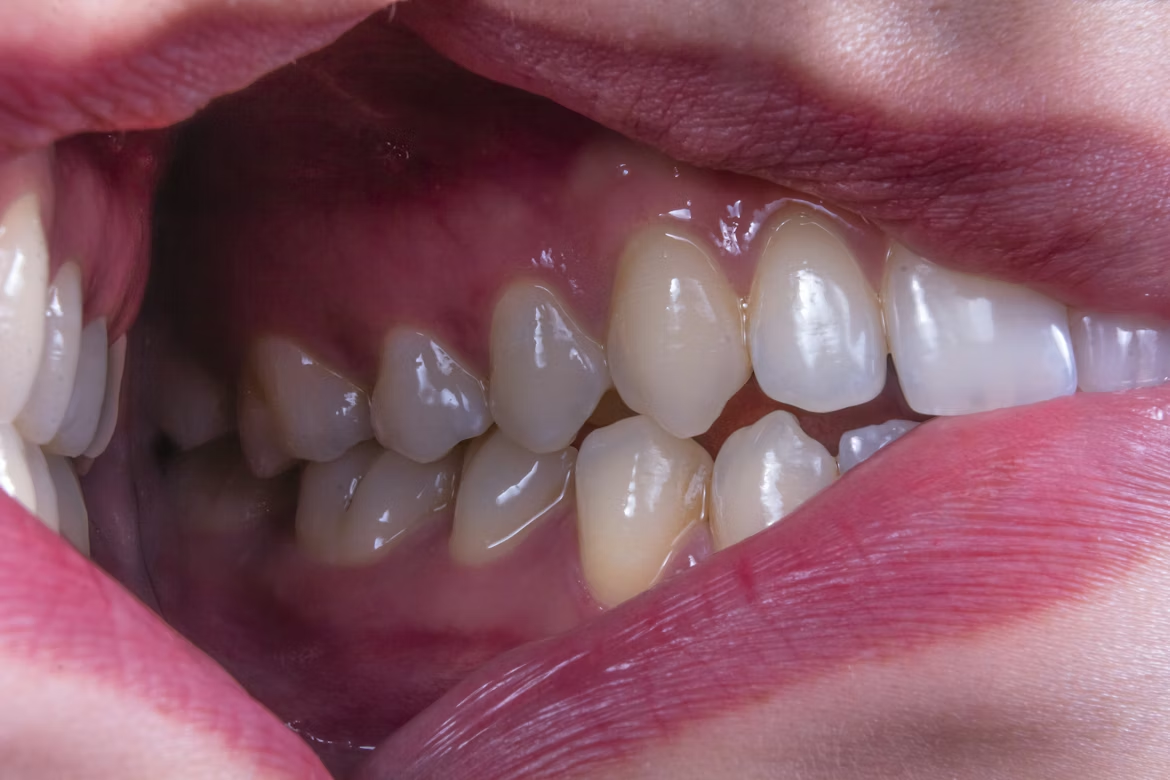
The bacteria causing gum disease don’t remain isolated in the mouth — they enter the bloodstream through inflamed, bleeding gum tissue and can trigger inflammatory responses throughout the body. Research from the American Heart Association shows that people with moderate to severe gum disease face a 20% higher risk of cardiovascular disease, with the chronic inflammation from periodontal bacteria contributing to arterial plaque formation and increased risk of heart attack and stroke.
The connection becomes particularly serious for people managing diabetes, where gum disease creates a vicious cycle that compromises blood sugar control. Severe periodontal infection can increase insulin resistance and make glycemic management more difficult, while poorly controlled diabetes impairs the body’s ability to fight the bacterial infection in the gums. This bidirectional relationship means that addressing gum disease symptoms early becomes crucial for maintaining overall diabetic health management.
Pregnancy outcomes also show strong correlations with gum health, with expectant mothers experiencing moderate to severe gum disease facing increased risks of preterm birth and low birth weight babies. The inflammatory mediators produced during gum disease can trigger early labor, making prenatal periodontal care an important component of comprehensive pregnancy health.
Beyond these well-documented connections, emerging research suggests links between gum disease and respiratory infections, rheumatoid arthritis, and certain cancers. The chronic inflammatory burden from untreated gum disease appears to tax the immune system, potentially reducing its effectiveness in fighting other health challenges. For NYC adults juggling multiple health priorities, recognizing that bleeding gums or persistent bad breath might signal risks extending far beyond dental problems provides crucial motivation for seeking timely professional evaluation.
The systemic health implications transform seemingly minor gum disease symptoms into potential indicators of broader health risks, making early detection and treatment investments in overall wellness rather than merely dental maintenance.
Prevention and Early Interventions for Gum Disease Symptoms
Effective daily oral hygiene requires more precision than most people realize — it’s not just about frequency but technique and timing. Brushing should occur at least twice daily with fluoride toothpaste, using gentle circular motions that focus on the gum line where bacteria accumulate most readily. Flossing daily removes bacterial deposits from areas that toothbrushes cannot reach, particularly between teeth and just below the gum line where early gingivitis typically develops.
Professional dental cleanings every three to six months serve as both prevention and early intervention, removing hardened bacterial deposits (tartar) that home care cannot eliminate. During these appointments, dental professionals can identify early symptoms before they become noticeable to patients, often catching gingivitis when it’s most easily reversible. The frequency of these visits should increase for people with risk factors like diabetes, smoking history, or genetic predisposition to gum disease.
Antimicrobial mouth rinses containing cetylpyridinium chloride or essential oils can provide additional protection by reducing bacterial levels between brushing and flossing sessions. However, these products work best as supplements to, not replacements for, mechanical plaque removal through proper brushing and flossing.
Early intervention becomes crucial when symptoms first appear — even minor bleeding during brushing signals the need for more aggressive home care and professional evaluation. People who address bleeding gums within the first few weeks of onset often see complete resolution, while those who ignore early symptoms may progress to stages requiring more extensive treatment. The window for simple intervention closes relatively quickly, making prompt response to any gum disease symptoms essential for maintaining long-term oral and systemic health.
The most successful prevention strategies combine consistent daily habits with professional monitoring, creating a system that catches problems early while maintaining the oral environment necessary for lifelong gum health.

