CHAPTER 131
Lymphedema
Mabel Caban, MD, MS; Lori Hall, PT, MS, CLT-LANA
Definition
Between 3 and 5 million people in the United States suffer from lymphedema, which in a significant number develops from cancer and its treatment [1]. The incidence of post-mastectomy lymphedema ranges from 6% to 48%, depending on whether the patient received axillary radiation and surgery; if only lumpectomy is performed, the incidence drops to only 6%. This increases to 23% with use of sentinel node biopsy and radiation therapy; but if axillary lymph node dissection and radiation therapy are used, the incidence is even higher at about 35% to 48% [1].
About 80% of lymphedema cases involve the lower limbs and relate to peripheral vascular disease [1]. Cervical cancer, melanoma, and pelvic cancers increase the frequency of secondary lymphedema of the lower extremity. An incidence of 21% to 49% is reported after cervical cancer surgery and radiation therapy. In women with endometrial cancer, 11% developed lower limb lymphedema after surgery and radiation therapy. Around the world, infection in the form of filariasis is the most common cause of lymphedema. An estimated 15 million people present with lower extremity lymphedema in filariasis-endemic regions in the world [2].
Lymphedema is a condition of an abnormal enlargement of part of the body associated with lymphostasis from dysfunction of the lymphatic system (Fig. 131.1). The dysfunction is due to the abnormal morphology of the lymphatic system, high production of lymph, or blockage in drainage [3,4]. The lymphatic system consists of vessels with lymph traveling through lymph nodes. The lymphatic vessels transport fluid, plasma proteins, and other substances from the tissue back into the circulatory system. Lymphedema results from the inability to drain the lymphatic fluid and the accumulation of it in the limb. Chronic edema initiates a cascade of events that cause transformation of the tissue with skin thickening, fibrosis, deposition of fat, and unhealthy skin changes after months to years. A classification of lymphedema includes primary (heritable) and secondary (acquired) causes [5]. Phlebolymphedema pertains to dysfunction of the lymphatic system in association with chronic venous insufficiency [6]. Chronic venous insufficiency is a manifestation of deep venous thrombosis, angiodysplasia, lack of valves in the venous system, or varicosities.
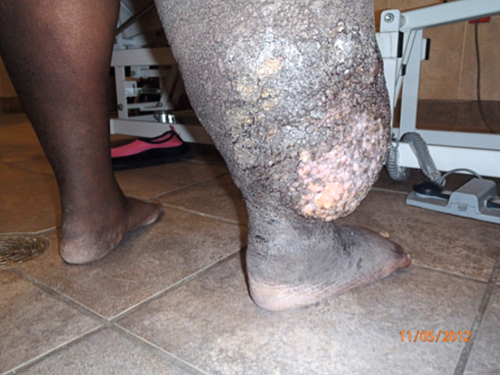
The radical excision of lymph nodes for malignant disease does not always cause lymphedema [7]. Lymphedema could occur as a late complication of surgery for malignant disease because of gradual failure, making the distal lymphatics pump harder through the most proximal damaged ducts over time. The body compensates by regenerating the transected lymphatics to some extent. With irradiation, fibrous scarring forms, increasing the risk of lymphedema. The diagnosis depends on the history and characteristic changes of the skin on clinical examination (Fig. 131.1).
Symptoms
The hallmark of lymphedema is painless swelling. Although many people believe that pain is a major component of lymphedema, this is not typically present, especially in the early stages. One of the first symptoms of lymphedema is tightness of the cutis and subcutis [8]. Chronic indolent swelling of a limb is the most common presentation of lymphedema. Patients may complain that the arm feels heavy or that rings feel tight. Hypertrophy of fatty tissue occurs and eventually fibrosis too. In true lower extremity lymphedema, the feet are involved. The skin condition changes from being soft initially to becoming harder over time. Early or postsurgical lymphedema can spread proximally, an unusual finding after the first year, and lasts about 3 months after surgery [7].
Physical Examination
The patient with limb edema requires a thorough physical examination before the initiation of therapy. Swelling of a limb with or without pain may be the presentation of an infection, deep venous thrombosis, or obstruction caused by a tumor at the level of the lymph nodes. Limb temperature and discoloration should be noted. In early stages, the edema is pitting, but as lymphedema progresses, the edema becomes nonpitting. In the absence of treatment, distal enlargement of the wrist or ankle occurs. A discrepancy of 2 cm in circumference or a difference of 200 mL in volume from side to side has been accepted for the diagnosis of lymphedema. A multitude of skin changes occur over time (Table 131.1) [9]. Signs of lymphedema progression include a cool limb, skin thickening, limited range of motion, increased presence of papillomas, mycosis, and bacterial infection. Infection, such as cellulitis, erysipelas, and lymphangitis, must be recognized to prevent systemic malaise and worsening of the swelling [3].
Staging of the condition helps assess progression and evaluate better treatment options. Stages of lymphedema are as follows:
Stage 0 Preclinical: there is no swelling, and it can lasts months or years.
Stage I Reversible stage: swelling is soft and pitting.
Stage II Spontaneously irreversible stage: increased swelling and change in tissues with fibrosis formed.
Stage III Lymphostatic elephantiasis: limb becomes extremely swollen with thickened skin.
Lymphedema does not cause neurologic deficits, but paresthesias and numbness may occur in the same distribution of the edema. Explanations include coexistence of neurologic damage from node dissection, peripheral nerve injury, plexopathy, and chemotherapy-induced polyneuropathy. The possibility of cancer recurrence must be ruled out with imaging, such as computed tomography or magnetic resonance imaging with contrast enhancement.
Lipedema can occur with lymphedema. This is an abnormality of the deposition of fat involving the lower body, most commonly in women, of symmetric appearance. Swelling starts at the waist and finishes at the ankles without inclusion of the feet as opposed to lymphedema, in which the feet are involved. Lipedema does not respond to dietary intervention or complete decongestive therapy. If underlying hormonal imbalance exists, correction will improve this condition, and although it is controversial, liposuction can improve it in some cases [10,11].
Unilateral or bilateral venous insufficiency may be manifested with varicosities, fibrosis, thickened cutis, and brownish skin discoloration. Superimposed venous ulcers may occur in advanced cases [3,7].
Functional Limitations
Impaired mobility due to the excessive weight of the limb may occur in severe cases (Table 131.2) [4]. Tight clothing, restriction of movement, and loss of body image and self-esteem are frequent complaints leading to psychosocial impairment. Women with breast cancer–related lymphedema report problems with their sexual well-being and social interaction [12]. In the past, avoidance of physical activity was the norm for fear of worsening the edema. This has changed with new evidence supporting the benefits of physical activity and exercise [12]. Wearing of a compression garment during exercise is advised (Fig. 131.2).
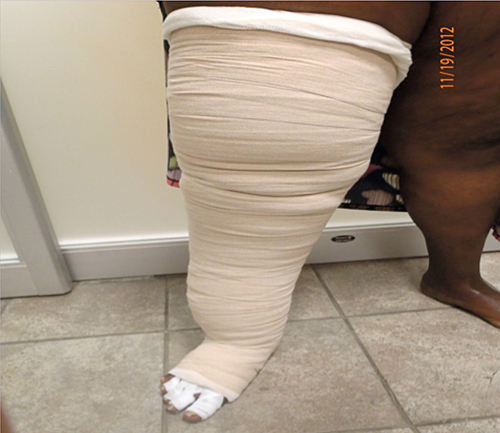
Diagnostic Studies
The diagnosis of lymphedema is based on the history, physical examination, and noninvasive diagnostic procedures. New-onset lymphedema should be a diagnosis of exclusion after deep venous thrombosis and malignant disease (including cancer recurrence) are ruled out. Therefore, most patients with new-onset lymphedema will have a workup for malignant disease as well as a Doppler ultrasound examination to rule out deep venous thrombosis. The diagnosis can be confounded with conditions such as obesity, chronic venous insufficiency, occult trauma, fracture, and repeated infections. Genetic testing may be necessary if gene therapy becomes clinically viable in the future [13]. Currently, research with animal models is targeting the vascular endothelial growth factor receptor 3 (VEGFR-3) and its primary ligands (VEGF-C and VEGF-D), looking for potential molecular treatment strategies.
Treatment
Initial
The risk of lymphedema can be reduced by use of sentinel node biopsy as part of the treatment for malignant neoplasms [14]. Early lymphedema may revert with appropriate compression of the limb and by maintaining an active lifestyle. The goals of the initial treatment include reduction of swelling, arrest of progression, improvement of other related symptoms, avoidance of infection, and optimization of function and quality of life. Treatment includes conservative, surgical, pharmacologic, and alternative methods.
The most commonly used drugs are the diuretics. However, diuretics are believed to worsen other types of lymphedema because they increase urination and produce hemoconcentration of tissue proteins. Because the edema is protein rich, the diuretic prompts protein to remain stagnant in the congested area, leading to fibrosclerosis. Diuretics may be used in the presence of ascites or hydrothorax. A short course of diuretics can help in the presence of malignant lymphedema [4].
Benzopyrones may increase the number of macrophages that hydrolyze tissue proteins to facilitate the removal of protein. Their exact mechanism of action is not well understood, the benefits remain unproven, and the use is limited because of the potential for liver toxicity [3]. Selenium, a free radical scavenger, reportedly has an antiedematous effect that potentiates the effect of complete decongestive therapy and reduces the risk of erysipelas infections in patients with lymphedema [15].
Antiseptic dressings for minor wounds and the early use of antibiotics for infections can prevent long-term complications. Prophylaxis with antibiotics such as phenoxymethylpenicillin (500 mg daily) is recommended for cases with recurrent cellulitis [3].
Rehabilitation
Treatment outcomes are most favorable with diagnosis and treatment early before fibrosis and hardening of the tissue occur. When pitting edema exists, the lymphedema is more responsive to treatment [16]. Complete decongestive therapy, the standard of care for lymphedema, is a multifaceted treatment approach performed by a certified lymphedema therapist that consists of two phases.
Phase one is the reductive phase. During this phase, manual lymphatic drainage, a technique similar to a gentle light touch massage that stimulates the lymphatics and facilitates drainage of congested areas, is used. Compression bandages employ multiple layers of short-stretch bandages and other materials, such as foam padding, to create a bandage with a low resting pressure and a high working pressure in the affected limb. Remedial exercises are movements with light exertion and stretches done while compression bandages or garments are worn. These exercises stimulate the lymph drainage into the thoracic duct [17]. Finally, meticulous skin and nail care requires moisturizing with a low-pH lotion; this prevents skin from drying and cracking and also discourages the growth of bacteria and fungus, which can cause infections and wounds. The initial phase of complete decongestive therapy ends when the maximum volume reduction is achieved and there is no further improvement. Relative contraindications to institution of complete decongestive therapy include acute infections, cardiac edema, peripheral arterial occlusive disease, renal dysfunction, and acute deep venous thrombosis. Recurrent tumor should be treated before the use of massage (manual lymphatic drainage).
During phase two, or the maintenance phase, the patient is fitted with a compression garment to wear during the day and taught how to continue bandaging at night or to apply a nighttime compression device [17]. The patient may also be taught self-drainage of lymph or the use of an intermittent pneumatic compression device. The use of the intermittent pneumatic compression device is controversial, and there are concerns that a high-pressure single chamber may cause damage to superficial structures, edema in the trunk or genitals, and development of a fibrosclerotic ring above the device sleeve. In response to some of the concerns, the latest models have multichambers, with sequential pressure delivery, programmable pressures, and truncal clearance [18]. In this phase, it is important that the patient continue to take care of the skin and perform the home exercise program. Weight reduction has been proved to have a positive impact by reducing limb volume [19].
Studies have shown some success when other modalities are included together with complete decongestive therapy. For example, low-level laser therapy was approved by the Food and Drug Administration in 2006 for professional treatment and self-treatment of lymphedema. Studies have shown moderate to strong evidence for the effectiveness of low-level laser therapy [20]. Kinesio tape is widely used to treat edema and may be an alternative to short-stretch bandaging for breast cancer–related lymphedema when compliance with short-stretch bandaging after 1 month of intervention is poor [21]. Kinesio tape in conjunction with compression may improve results but has yet to be sufficiently studied. Oscillation therapy involves the use of electrostatic impulses to create a kneading effect to promote lymphatic drainage [22].
Surgery
Surgical options can benefit a few patients when the size of the limb interferes with mobility. Surgical procedures are still controversial. These are debulking procedures to remove excess tissue overgrowth; microsurgery to restore lymphatic continuity by use of a lymphatic collector or vein segment, also known as lymphaticovenous anastomosis [23]; and liposuction when lymphedema is nonresponsive to conservative management from the excess fat overgrowth. Patients still need to wear compression garments long term [24].
The standard of care in the past was to excise all of the regional lymph nodes during cancer surgery, but this is no longer the case to prevent morbidity such as lymphedema. For example, in breast cancer patients, sentinel lymph node dissection is associated with lower incidence of lymphedema than axillary lymph node dissection is. Sentinel lymph node dissection facilitates the resection of the sentinel node that combined with frozen-section histologic examination prevents unnecessary secondary surgeries, prevents lymphedema, and improves disease-specific survival [25].
Potential Disease Complications
Recurrent cellulitis and infections with staphylococcal resistant bacteria may occur. Delay in treatment increases the risk of sepsis. If it is untreated, lymphedema may progress to fibrosclerosis of the tissue and elephantiasis. A rare complication is lymphangiosarcoma, a malignant neoplasm in a lymphedematous limb described in post-mastectomy lymphedema and congenital lymphedema [7]. Stewart-Treves syndrome was first described in women who had undergone a radical mastectomy with subsequent lymphedema and lymphangiosarcoma.
Potential Treatment Complications
Potential complications include disease progression, liver complications from the use of benzopyrones, and worsening of lymphedema after liposuction from disruption of the remaining lymphatics.







