Chapter 7
Clinical assessment of the orthopaedicand trauma patient
Rebecca Jester
London South Bank University, London, UK; Dudley Group NHS Foundation Trust, Dudley, West Midlands, UK
Introduction
The aim of this chapter is to provide an evidence-based discussion of assessment of the orthopaedic and trauma patient. The chapter adopts a person centred approach to the subject of assessment as it is important to remember that, although a person’s chief complaint will be a musculoskeletal problem, most are likely to have co-morbidities and psycho/social issues that relate to their problem. Practitioners will be using their assessment skills throughout the patient’s journey from initial presentation in primary care, emergency room or outpatients department to on-going evaluation following intervention or change in medical status. Throughout the chapter, where robust evidence exists, there will be critical application of research to approaches to assessment and examination. However, to date there is very little high level evidence to support many aspects of patient assessment/clinical diagnostics within trauma and orthopaedics affirmed by a dearth of systematic reviews. Therefore the information within this chapter is in the main based upon evidence from the following sources: formal education, symposia, conference presentations, non-research publications, expert opinion and reflections on clinical experience (the author’s and other clinical experts’).
Principles of clinical assessment
Clinical assessment can be defined as gathering both objective and subjective data for the purposes of generating differential diagnoses, evaluating progress following a specific procedure or course of treatment and evaluating the impact of a specific disease process. Examples of objective and subjective data can be found in Table 7.1.
Table 7.1 Types of subjective and objective data
| Subjective data | Objective |
| History – dependent on accuracy of patient and/ or family as historians | Radiographic and other clinical investigations such as blood tests, MRI, CT |
| Patient reported outcome measures (PROMS), patients’ subjective perceptions of their symptoms and the impact on their quality of life and functional ability, mental health status | Measurement of range of movement (ROM) using goniometry Base line observations such as blood pressure, weight, height, body mass index (BMI), temperature, heart rate |
| Pain assessment | Measurements of limb length and muscle strength |
| Physical assessment including muscle, strength, palpation, auscultation and inspection. | |
| Clinician measures such as timed get up and go test. |
There are some important key principles related to assessment including:
- introducing yourself
- confirming the patient’s identity
- explaining what the assessment is going to involve
- gaining the patient’s consent for the assessment
- establishing if the patient wants a family member or carer to be present during the assessment
- good hand hygiene prior to and on completion of assessment/examination.
It is important to establish, either prior to or early in the assessment, if the patient has any degree of cognitive dysfunction. Communicating with patients with impaired cognition requires management of the immediate environment to reduce accessory noise and constant re-orientation to what you are doing and why. It is also important to establish that the patient has the mental capacity to consent to the assessment before proceeding. People with learning disabilities often are not supported well in acute hospitals (MENCAP 2007). Thoughtful communication involves minimising healthcare jargon, use of pictorial aids if appropriate and including a family carer. These can all help to alleviate anxiety during the assessment process. Non-verbal and para-verbal communication play a key role in putting patients with cognitive impairment or learning difficulties at ease during the assessment and enhancing the accuracy and quality of information elicited during the assessment.
It is important to:
- Ensure the patient is comfortable and their privacy and dignity are maintained at all times during the assessment. Patients of either sex should be asked if they would like a chaperone present during any physical examination and unless the patient refuses (this should be documented) a chaperone should always be present during intimate examinations of patients of the opposite sex. The name and signature of any chaperone should be clearly documented.
- Check the patient is not in pain, thirsty, hungry or needing the toilet prior to embarking on the assessment process. Also be mindful not to overtire older or frail patients with prolonged questioning, examination and clinical investigations. Patients may require a break and the assessment process may need to be phased to accommodate their needs.
- When documenting the assessment ensure you record negative as well as positive findings. For example ‘patient reports no locking or giving way of the knee joint’.
Models and frameworks of patient assessment
It is important to adopt a systematic approach to patient assessment to avoid missing valuable information and to minimise repetition. Patient assessment should be inter-professional and a shared assessment document adopted. This approach enables the multidisciplinary team (MDT) to share information and avoid wasting the patient’s time by several health care professionals attempting to collect the same information. Approaches to patient assessment will vary depending upon patient needs; for example, whether the patient is presenting as an emergency with multiple trauma or a non-emergency with a painful joint/s or musculoskeletal dysfunction.
Emergency presentation
The patient presenting in the Emergency Department (ED) with severe or multiple injuries must have an urgent and systematic assessment to identify life threatening issues using Advanced Trauma Life Support (ATLS). In most healthcare organisations these observations will be recorded on a Modified Early Warning Score (MEWS) chart. See Chapter 16 for further detail regarding assessment of the patient following trauma.
Non-emergency, elective or planned presentation
Within orthopaedic care the medical model of assessment has predominated, with the main aim of the assessment being to understand the patient’s chief complaint/problem and arrive at a differential diagnosis. Traditionally, this has been solely within the remit of the medical profession, but in recent years a growing number of specialist and advanced nurse and physiotherapy practitioners have taken on this role. The medical model comprises:
- taking a history to elicit the chief complaint or presenting problem
- observation and inspection
- physical examination using palpation, percussion and auscultation
- assessing movement and strength
- clinical investigations.
The medical model lends itself to the patient who is presenting with a clearly defined orthopaedic problem with minimal co-morbidities or without complex social or psychological issues. However, many patients within the orthopaedic setting have more problems than just a single chief complaint and require a more person-centred rather than disease-centred approach to their assessment. The medical model of assessment tends to focus on the disease process rather than the impact of the disease on an individual and the ideology of holistic health assessment is to review the individual as a whole, with a focus on their overall health needs rather than the disease.
There are several assessment frameworks or models that lend themselves to the person with multiple physical, social and psychological issues and which nurses may find useful to structure their assessment. Assessment is the first part of the nursing process (comprising assessment, planning, implementation and evaluation of care). Nursing models and theories seem to have lost favour in contemporary clinical practice which has become mainly target-orientated, but it remains important that nurses promote a holistic approach to assessment and care. An overview of the assessment component of these nursing or psychological models is presented below.
Roy’s Adaptation Model
This model, developed by Roy (1984), is based upon four modes; physiologic, self-concept (including body image and self-concept), role function and interdependence mode. This model lends itself particularly well to patients who are in the restorative phase following musculoskeletal trauma or spinal cord injury or those suffering with chronic conditions such as back pain and arthritis (see Chapter 6 for further reading on rehabilitation). The model focuses on assessing the patient’s behaviour and stimuli toward adaptation in each of the four modes. The physiologic mode includes:
- oxygenation
- nutrition
- elimination
- activity and rest
- skin integrity
- the senses
- fluid and electrolytes
- neurological function and
- endocrine function.
The role function model includes:
- primary role (age, sex, development level)
- secondary role (relatively permanent positions requiring performance such as spouse, parent, sibling) and
- tertiary role (freely chosen and relatively temporary such as employee, student).
The self-concept mode includes:
- the physical self
- body image
- body sensations
- the personal self – comprising self-ideal and self-expectancy and the
- moral–ethical–spiritual self.
The interdependence mode is about:
- support systems, both intrinsic and extrinsic to the individual, and their receptive/contributive behaviours.
Wellness framework
The wellness framework (Pinnell and de Meneses 1986) can be used to provide a systematic approach to data collection during the assessment process. It focuses on health and wellness rather than disease or ill health and uses the following categories:
- Degree of fitness: exercise patterns, muscle strength, muscle and joint flexibility, body proportions (fat and muscle).
- Level of nutrition: analysis of nutritional intake, patient’s knowledge of healthy nutrition, sociocultural beliefs about diet.
- Risk appraisal/level of life stress: identification of patient’s risk factors to health, identification of sources of stress to the patient, the patient’s perception of stress and their coping patterns.
- Life-style and personal health habits: habits regarding health behaviours, regular health screening, dental checks, alcohol/drug/smoking consumption, sleep and weight management.
The role of the nurse in orthopaedic care must incorporate promotion of healthy life styles and supporting patients to minimise risk such as the link between obesity and joint problems and the wellness framework lends itself well to this aspect of orthopaedic assessment.
Maslow’s hierarchy of needs
Maslow (1954) first developed his theory of motivation and personality. From this seminal work, a hierarchy of needs can be used to structure the assessment process. The needs are arranged in a pyramid based on the premise that until the lowest or most fundamental needs of the individual are addressed they are unable to move to higher levels of functioning. These levels of need are presented below in order (lowest to highest):
- Physiological (survival needs) – Assessment of oxygenation, nutrition status, fluid balance, body temperature, elimination, shelter (home conditions and support) and sex (assessing individual’s concerns about resuming sexual activity following procedures such as spinal fusion or hip arthroplasty).
- Safety and security (need to be safe and comfortable) – Physical safety: assess risk of falls; pressure sores, infection, VTE, pain assessment. Psychological security should be assessed in terms of the patient’s need for information and inclusion in decisions about their care and treatment.
- Love and belonging – Elicit information about the patient’s social and family support.
- Esteem and self- esteem – assess issues around body image and adaptation and coping and eliciting what the patient’s goals are.
- Self-actualisation – assess the extent to which the patient’s full potential is being reached, their levels of autonomy and motivation.
The medical model
History taking
Taking a history has three principal functions:
- Provision of data to inform decision making around differential diagnosis and treatment planning.
- Initiates a medium by which a therapeutic bond is formed between patient and practitioner.
- Creates a forum for education.
The importance of thorough and accurate history taking has been recognised for many years. It is very tempting for busy practitioners to try and steer the patient’s presenting signs and symptoms to fit a particular disease pattern by asking leading questions, but this can lead to an inaccurate diagnosis. Silverman and Hurst (1991) suggest that history alone can provide the correct diagnosis in approximately 80% of patients.
History taking comprises ten stages which should be followed in order:
- Chief complaint – elicit the chief complaint, using an open-ended question such as ‘What brings you here today’?
- History of the chief complaint –
- Provocative or palliative – what makes it worse or better?
- Quantity or quality – how often do you experience the problem?
- Region or radiation – is the problem localised or more diffuse?
- Severity or scale – how would you rate your problem?
- Timing – is there a particular time of the day or night associated with your problem? When was the onset of your problem and has it been constant or intermittent?
- Recapitulation – re-affirm with the patient at this stage that you have understood what their main problem is and the history of that problem as this allows any misconceptions to be resolved before proceeding further with the history.
- Family history – some musculoskeletal conditions have a genetic disposition such as rheumatoid arthritis. A genogram is the most systematic and succinct way to record a family history.
- Past medical history (PMH) – including all major illnesses, surgery and treatments. Patients may often forget significant aspects of their PMH and you may need to triangulate information with accessory information from the patient’s notes, further questioning based on their medication, and findings from inspection such as scarring indicating previous trauma or surgery.
- Psychosocial and occupational history – frequently musculoskeletal problems can be associated with patients’ previous or current occupation, for example often severe osteoarthritis of the knee is related to occupations such as HGV driving, climbing up and down ladders or carpet fitters. Repetitive strain injury of the wrists and hands is often found in people who use computers for long periods of time on a daily basis. A social history will elicit what the patient’s home situation is in terms of living accommodation and support from family and friends. This is very important for discharge planning and ascertaining if any adaptations to the home or work environment are needed to alleviate the patient’s symptoms and increase independence.
- Review of symptoms – although the patient will be presenting with a chief complaint of a musculoskeletal problem/s in certain situations such as preoperative assessment, it is necessary to review all the body systems to rule out any co-morbidities that may present as a risk during surgery/anaesthesia (see Chapter 5 for further detail on pre-operative assessment). The review of systems should also include a review of the individual in terms of rest and sleep patterns, smoking and alcohol habits. Table 7.2 provides guidance on reviewing the body systems. To review the systems in a systematic way it is best to take a head-to-toe approach.
- Allergies – ascertaining if the patient has any known allergies to medications, dressings/adhesive or latex. Historically patients were tested for sensitivity to nickel, cobalt or chromium, but the clinical significance of metal sensitivities following prosthetic replacements is questionable and therefore routine metal allergy testing is no longer recommended. However, it is still important to question patients about metal skin sensitivity, specifically nickel as the patient may have a skin reaction from clips or staples following surgery. The evidence base for the value of routine metal allergy testing is equivocal as a study by Frigerio et al. (2011) concluded that objective determination of metal sensitivity at preoperative assessment should be considered when planning joint arthroplasty, as it would help the surgeon determine the most appropriate prosthesis.
- Medications – including prescribed, over the counter (OTC) and homoeopathic medicines. Patients can often be unsure of the names, doses and function of their medications so it is important to cross-verify with accessory information such as prescription printouts.
- Education – this stage of the history taking process facilitates the opportunity for the patient and/or their family if present to ask questions and also to provide health promotion advice. For example if the patient reports smoking then smoking cessation advice can be provided. Also, if the patient is obese or morbidly obese, information and support for weight reduction can be offered. It is also important to offer the patient and/or family member the opportunity to ask any questions or raise any issues they feel have not been covered during the history taking/assessment.
Table 7.2 Review of Systems
| Body system | Example questions |
| Integmentary | Do you have any skin lesions, sores, unhealed wounds, pressure sores, rashes, fungal infections of nails? |
| Mental health/psychological well-being | Do you currently suffer with anxiety or depression? |
| Neurological | Do you suffer with fits, faints, blackouts, headaches, muscle weakness/wasting or altered or loss of sensation? |
| Respiratory | Do you suffer with shortness of breath either at rest or on exertion or suffer with wheezing, bronchitis, asthma, chest infections or dry or productive cough? |
| Cardiovascular | Do you have any problems with chest pain, circulatory problems, leg ulcers, blood clots or varicose veins? |
| Musculoskeletal (The chief complaint will have been explored earlier in the history, but additional musculoskeletal problems may be present.) |
Do you have any joint pain, swelling, locking or giving way, limitations to movement, fractures or muscle/tendon/ligament injury? |
| Gastrointestinal | Do you have any gastric bleeding, ulcers, abdominal pain, oesophageal reflux, loss of appetite, unintentional weight loss or gain. Ascertain bowel habits and if there has been any recent change. |
| Genitourinary | Do you have any problems passing urine such as urgency, frequency, incontinence, hesitancy, nocturia or urine infection? |
Principles of physical examination
Based on information gained during the history, the practitioner can then focus the physical examination. Which body systems to include in the assessment will depend on both information from the history and the nature of the assessment. For example if the patient is presenting postoperatively with deteriorating vital signs a thorough examination of several systems including cardiovascular, respiratory, neurological and abdominal may be needed. If the patient is presenting in the orthopaedic or primary care clinic with a specific localised musculoskeletal problem then the examination can focus on the joint of concern, bearing in mind that musculoskeletal pain can often be referred and therefore it is important to include examination of joints above the specific site of the problem and to always compare both limbs. The important principle is to have a sound rationale for which systems and specific elements of systems you decide to include and exclude and this should be documented within your assessment.
It is important to use all senses during assessment including sight, smell, hearing and touch. There are several techniques used within physical examination which are observation, inspection, palpation, percussion, auscultation and measurement.
Observation
The first step of assessing a patient is through observation of them. Observation involves the senses of sight, smell and hearing. A good tip is to start observing the patient as you approach them (or them you) to observe:
- How they rise from a chair, transfer from bed to chair etc
- Facial expressions indicating pain/discomfort, anxiety or low mood
- Use of a walking aid and if they are using it correctly
- Gait analysis e.g. Trendelenburg gait indicating a potential hip problem, stiff knee gait or a drop foot
- Crepitus from movement of the joints or wheezing/ rattles from the chest
- Does the patient look flushed, hot, pale, sweaty or jaundiced?
- Does the patient look well cared for or unkempt?
- Smell of acetone from the breath indicating ketosis
- Smell of urine or faeces.
Your initial observations should be recorded within the assessment and explored with the patient during the history.
Inspection
Inspection is much more detailed than general observation and focuses on detecting specific issues in musculoskeletal examination such as the presence or absence of swelling, bruising, scarring, skin discoloration, oedema, muscle wasting, alteration of shape, posture or deformity.
Inspection for swelling/s should note if it is localised or diffuse and confined to the joint or extending beyond the joint. Swelling confined to the joint itself can indicate either effusion due to excessive synovial fluid or non-pyogenic conditions such as rheumatoid or osteoarthritis. Swelling beyond the joint may indicate infection of the limb such as cellulitis, tumours, vascular or lymphatic problems. It is important to be precise in recording the location and extent of any swelling observed and to affirm by further questioning the onset, duration and pattern of swelling e.g. intermittent, fluctuating in severity, relieving or exacerbating factors. There are specific tests to confirm swelling which are discussed under palpation and special tests.
Inspection should also include the identification of any bruising or abrasions suggesting recent trauma and scarring from previous surgery or trauma. Changes to skin colour should also be noted, specifically erythema (redness), which may indicate a localised response to trauma or infection, or pallor possibly indicating compromised vascular function. Any muscle wasting should be noted, usually indicating limited use due to pain or injury or impaired nerve supply (denervation). For example, muscle wasting of the quadriceps can be very common in patients with knee trauma or pathology and wasting of the thenar eminence (of the thumb) in conditions of the hand/wrist such as carpal tunnel syndrome (median nerve compression). Inspection should also be used to detect deformity, altered posture or shortening; these can result from either a congenital abnormality, trauma or destructive joint disease.
Palpation
Palpation should be used to detect changes in temperature of the limbs/joints/spine and detect any tenderness. The back of the hand rather than the practitioner’s palms should be used to detect localised or diffuse changes in temperature. Increased heat over a joint is indicative of inflammatory processes, whereas diffuse heat away from the joint may indicate a tumour or infection such as cellulitis. Coolness of a limb is generally indicative of arterial pathology such as atherosclerosis.
Identifying the exact location of tenderness is important in identifying precisely which underlying structures may be involved. Observing the patient for signs of distress or discomfort during palpation is important; as is documenting precisely the exact location and extent of tenderness and or alteration in skin temperature.
Assessing movement
Many orthopaedic conditions result in loss or restriction of movement. Assessing the range of joint movement requires knowledge of the normal range possible (Chapter 4). Restriction in movement can be due to contraction of joint capsules, tendons and muscles or lodging of loose bodies between the articulations of the joint. A resultant fixed flexion deformity of the joint can occur; most commonly an inability to fully flex the joint. Movement of the joint controlled by the patient is known as active range of movement and passive movement is when the practitioner controls the movement of the joint; the latter being appropriate when the muscles responsible for movement of the joint are paralysed. It is important to observe and listen to the patient when conducting measurement of range of movement, observing for signs of pain and distress. There is an unequivocal evidence base regarding the best method of measuring range of joint movement.
Assessing muscle strength
Assessing strength of muscle contraction is indicative of the strength of each joint movement and therefore should be included within the examination process. A scale developed by the Medical Research Council (MRC 1975) is used to record muscle strength and is shown in Box 7.1
Assessing for shortening of the lower limbs
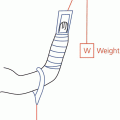
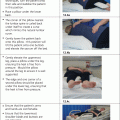
As part of examination of the hip and lower limb it is important to determine the presence or absence of shortening (McRae 2010). True shortening, where the limb is physically shorter, may be caused by a number of pathologies including loss of articular cartilages caused by arthritis, displaced hip fracture, dislocation of the hip, epiphyseal trauma and old fractures of the tibia or femur. In apparent shortening the limb length is not altered but appears shorter because of contracture of the adductor muscles resulting in tilting of the pelvis. To measure for true shortening the first stage is to ask the patient to lie flat on a couch with the pelvis positioned squarely and both legs stretched out as straight as possible with heels flat to the couch. In the normal patient the heels and the anterior iliac spines are level. If a discrepancy is noted by this visual check it is necessary to measure the limbs with a tape measure which should be of material that does not stretch. Measure from the inferior edge of the anterior superior iliac spine to the middle of the medial malleolus and then extend the measurement down to the bottom of the heel with the ankle in the neutral position. Compare both sides and repeat the measurements until accuracy is assured. To measure for apparent shortening, measure between the umbilicus or xiphisternum down to the middle of both medial malleoli.
Gait assessment
There are many causes of abnormal gait patterns, including neurological and musculoskeletal disorders. There are a number of orthopaedic conditions that may produce gait abnormalities including Trendelenburg gait (waddling gait) due to hip pathology, stiff knee gait due to knee pathology and drop foot gait due to damage to the nerves responsible for dorsi-flexion of the foot. Gait analysis is most commonly undertaken by the physiotherapist or orthopaedic surgeon, but nurses working within specialist or advanced roles may carry out gait analysis as part of their assessments.
Special tests
There are a number of specific tests that may be included as part of examination of the patient. Clinical reasoning based upon the patient history and prior aspects of the examination including observation, inspection, palpation and measurement of motion will determine if special tests are required to assist in making a differential diagnosis. The most common of these include testing for valgus instability of the knee joint using the anterior draw test, testing for varus instability using the Lachman test and the Trendelenburg test for weakness of the abductor muscles of the hip. The Trendelenburg test involves the patient standing on one leg and then the tilt of the pelvis on the opposite side is observed – if the pelvis drops below the horizontal plane then the test is said to be positive.
Assessing deep tendon reflexes
Deep tendon reflexes are tested by gently tapping over a tendon using a patellar hammer and observing for movement of the associated muscles. When examining the spine for suspected prolapsed intervertebral disc, both the knee and ankle reflexes should be tested. When testing the knee reflex, the knee should be supported by the clinician’s arm and the infra patellar tendon gently tapped observing for contraction of the quadriceps. A diminished or absent contraction indicates a possible prolapse at the level of L3/L4. The ankle reflex is assessed by positioning the ankle in the mid position, knee bent and hip slightly externally rotated then lightly tapping the Achilles tendon and observing for plantar flexion of the foot. An absent or diminished ankle reflex is indicative of pathology at vertebrae S1/S2. It is important when assessing deep tendon reflexes that there is no muscle contraction in the area being assessed so the patient must be relaxed. Reflexes are recorded as follows:
- 0 = absent
- + = reduced
- ++ = normal
- +++ = increased
- ++++ = increased with clonus
Clinical investigations
Once the history and examination have been completed the practitioner needs to decide what clinical investigations are needed to arrive at a differential diagnosis and/or treatment plan. Clinical investigations including X-Rays, MRI and CT scans or blood investigations have associated costs and risks to the patient e.g. cumulative doses of radiation, and so should be requested only with a clear justification of their need. Nurses working in trauma and orthopaedics should have an understanding of the common investigations to offer support and explanation to the patient. Nurses working in specialist and advanced roles often undertake the requesting and interpretation of clinical tests within their scope of practice. The most common investigations include:
- Radiographic imaging (X-ray) – the most commonly used diagnostic imaging in trauma and orthopaedics. AP and lateral views are the most frequently requested view, but other views include: comparison images, oblique views, localised views and stress films. All clinicians requesting X-Rays must undertake specific radiology safety training and be judicious in requesting X-Rays in relation to the cumulative dose of radiation the patient is receiving.
- Computed tomography (CT scan) – still uses beams of radiation, but provides a more detailed view of tissue slices from different angles and more detailed differentiation of different tissue types.
- Magnetic resonance imaging (MRI) – avoids any exposure to radiation, using high strength magnetic fields and electrical impulses to create detailed images of bone and soft tissue. These are increasingly used in the investigation of spinal problems such as suspected prolapsed intervertebral discs and damaged structures such as meniscal and ligament tears in the knee and shoulder.
- Ultrasound imaging – is regarded as being risk-free and comparatively inexpensive. Its main value is to detect fluid in and around joints and therefore is useful in identifying heamarthrosis or the presence of infected or inflamed tissue.
- Dual energy X-ray absorptiometry (DEXA) – A non-invasive scan to test the density of bones for diagnosis of osteoporosis.
- Common haematological investigations – including full blood count (FBC) (which includes red and white cells and platelets), tests for inflammatory processes include C-reactive protein (CRP), erythrocyte sedimentation rate (ESR) and plasma viscosity (PV). It should be noted that these markers of inflammation can also be present due to infection. Serum uric acid and serum calcium, phosphate and alkaline phosphate may also be requested.
Boxes 7.2 and 7.3 provide examples of the underpinning evidence for two modes of physical assessment.
Assessing the impact of disease on the individual
It is important, as part of the assessment process, to evaluate the impact of a particular disease on the individual to inform the treatment or management plan. There may be little correlation between what clinical investigations and examination reveal and the perception of the individual. Patients with severe osteoarthritic changes on X-Ray may report minimal disruption to their activities of daily living. Conversely patients with minimal radiographic changes may report their symptoms to be intolerable with a dramatic impact on their quality of life and functional ability (Swagerty and Hellinger 2001). This is explored in more detail in Box 7.4.
Self-report outcome measures can be broadly categorised into general health-related quality of life tools (HRQoL) and disease-specific tools. HRQoL measures aim to measure the multifaceted nature of health including physical, social and psychological health and can be used across many different types of diseases and health issues (Jester et al., 2011). Their main limitation is that they lack the sensitivity to detect relatively small changes in health status for a particular disease process (Bowling, 2001) and therefore should be used in conjunction with disease-specific measures. Examples of HRQoL measures include: Sickness Impact Profile, The Nottingham Health Profile and Short Form 36 Health Survey Questionnaire (SF 36). There are many disease-specific self-report measures developed for patients with musculoskeletal conditions including; the Arthritis Impact Measurement Scale, the Oxford Hip and Knee Scores, the WOMAC index and the Harris Hip Score. The practitioner should ensure that any HRQoL or disease-specific measure used as part of the assessment process has undergone rigorous testing to ensure it is valid, reliable, sensitive, specific and patient-friendly.
Assessing cognitive function
A significant number of patients presenting with musculoskeletal problems may have a degree of cognitive dysfunction this may already be noted in the patient’s records. As part of a comprehensive assessment process the nurse should ensure that cognitive dysfunction is detected and its cause investigated and managed. It should never be assumed that because a patient is elderly their confusion is due to dementia. It is vital to ascertain the onset of the patient’s confusion, specifically if it is an established diagnosed problem due to dementia, head injury or stroke or whether there has been a recent onset. Acute confusional states must be thoroughly investigated by taking a history of the onset from the patient if possible, family members or informal carers and then carrying out appropriate clinical investigations and observations to elicit the cause. Acute confusion (delirium) can be caused by many factors including urea and electrolyte (U and E) imbalance, sepsis, hyper- or hypoglycaemia, adverse reaction to prescribed medications, raised intracranial pressure (ICP) and drug/alcohol related. The practitioner should inform the medical team of the onset of acute confusion and commence observations using the MEWS chart and Glasgow Coma Scale (Chapter 16) to determine if any vital signs fall outside of normal parameters. Then the practitioner, in collaboration with the medical team, should begin to collect information to contribute towards determining the cause of confusion including:
- blood tests for U and E, capillary blood sugar (CBS), liver function tests, blood cultures, CRP and ESR
- urinalysis for protein, ketones and glucose and send a MSU if a urine infection is suspected
- oxygen saturation rates
- accurate monitoring of fluid input and output
- review medication with medical and pharmacy team for possible interactions or adverse reactions.
Once delirium has been ruled out based on these investigations then the patient’s cognitive status should be assessed using a valid and reliable tool such as the Abbreviated Mental Test Score (AMTS, Qureshi and Hodkinson 1974) or the Mini Mental State Examination (MMSE, Folstein et al., 1975). The AMTS comprises ten items as detailed in Box 7.4; the best possible score is 10/10 with each correct item scoring 1. The diagnostic cut-off point varies between authors, but generally <6 indicates cognitive dysfunction (Jester et al., 2011). Although widely used in clinical practice and well tested for their psychometric properties, both the MMSE and AMTS have their limitations as they are developed for a specific age and ethnic group. Explain to the patient why you are asking the questions comprising the MMSE and AMTS and ensure privacy and an environment that has minimal background noise and disruption to get the best results.
Assessing risk
An integral part of the assessment process is to assess patient’s risk of harm or injury including risk of: falls, pressure sores, malnutrition and VTE. Specific risk assessment tools are presented and discussed within the related chapters of this text. However, the predictive accuracy of all risk assessment tools must be evaluated to ensure that the practice associated with them is evidence-based. Predictive accuracy is the ability of a tool to be both sensitive and specific; to minimise the number of false positives (over prediction) and false negative (under prediction). A pilot study by Jester et al. (2005) found the predictive accuracy of two falls assessment tools (FRASE and STRATIFY) with older hip fracture patients to be poor, reporting Receiver Operator Characteristic scores to be 0.560 and 0.629 respectively, indicating significant over-prediction when using the tools.
Summary
This chapter has discussed best practice in assessment of orthopaedic and trauma patients. The content has included the traditional medical approach to assessment including physical examination, but has also offered a number of alternative models rooted in nursing and psychology theory. Where available there has been critical application of research and the deficit of high level evidence to underpin clinical assessment has been highlighted. Good assessment skills are fundamental to nursing practice as they generate data from which our care and treatment is planned and implemented.
Recommended further reading
- McRae, R. (2010) Clinical Orthopaedic Examination, 6th edn. Churchill Livingstone Elsevier, Edinburgh.
References
- Bowling, A. (2001) Measuring Disease, 2nd edn. Open University Press, Maidenhead.
- Folstein, M., Folstein, S. and McHugh, P. (1975) ‘Mini-Mental State’ a practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 12, 189–198.
- Frigerio, E., Pigatto, P., Guzzi, G. and Altonare, G. (2011) Metal sensitivity in patients with orthopaedic implants: a prospective study. Contact Dermatitis, 64(5), 273–279.
- Fukui, N., Yamane, S., Ishida, S. et al. (2010) Relationship between radiographic changes and symptoms or physical examination findings in subjects with symptomatic medial knee osteoarthritis: a three-year prospective study. BMC Musculoskeletal Disorders, 11, 269–279.
- Hambly, K., Sibley, R. and Ockendon, M. (2012) Agreement between a novel smartphone application and a long arm goniometer for assessment of knee flexion. International Journal of Physiotherapy and Rehabilitation, 54(October), 4–6.
- Jester, R., Wade, S., and Henderson, K. (2005) A pilot investigation of the efficacy of falls risk assessment tools and prevention strategies in an elderly hip fracture population. Journal of Orthopaedic Nursing, 9(1), 27–34.
- Jester, R., Santy, J. and Rogers, J. (2011) Oxford Handbook of Orthopaedic and Trauma Nursing. Oxford University Press, Oxford.
- Maslow, A. (1954) Motivation and Personality. Harper, New York.
- McRae, R. (2010) Clinical Orthopaedic Examination, 6th edn. Churchill Livingstone Elsevier, Edinburgh.
- Medical Research Council (MRC) (1975) Aids to the Investigation of Peripheral Nerve Injuries. HMSO, London.
- MENCAP (2007) Death by Indifference. MENCAP, London. Available at: http://www.nmc-uk.org/Documents/Safeguarding/England/1/Death%20by%20Indifference.pdf (accessed 21 May 2013).
- Neogi, T., Felson, D., Niu, J. et al. (2009) Association between radiographic features of knee osteoarthritis and pain, results from two cohort studies. British Medical Journal, 339, b2844.
- Pinnell, N. and de Meneses, M. (1986) The Nursing Process: Theory, Application and Related Processes. Appleton-Lange, Norwalk, CT.
- Qureshi, K. and Hodkinson, H. (1974) Evaluation of a 10 question mental test in the institutionalized elderly. Age and Ageing, 3, 152–157.
- Roy, C. (1984) Introduction to Nursing: An Adaptation Model, 2nd edn. Prentice-Hall, New Jersey.
- Swagerty, D. and Hellinger, D. (2001) Radiographic assessment of osteoarthritis. American Family Physician, 64(2), 279–287.
- Watkins, M., Riddle, D., Lamb, R. and Personius, W. (1991) Reliability of goniometric measurements and visual estimates of knee range of motion obtained in a clinical setting. Physical Therapy, 71, 90–96.